Case Report
Pulmonary Arteriovenous Malformations Leads To Embolic Cerebral Infarcts with Haemorrhagic Transformation
Dr. Wai-Hun Cheah*
Department of Radiology and Faculty of Medicine, Universiti Sultan Zainal Abidin, Malaysia
*Corresponding author: Wai-Hun Cheah, Department of Radiology and Faculty of Medicine, Universiti Sultan Zainal Abidin, Gong Badak, 21300, Kuala Terengganu, Terengganu, Malaysia
Published: 05 Jul, 2018
Cite this article as: Cheah W-H. Pulmonary Arteriovenous
Malformations Leads To Embolic
Cerebral Infarcts with Haemorrhagic
Transformation. Ann Clin Case Rep.
2018; 3: 1532.
ISSN: 2474-1655
Abstract
Pulmonary arteriovenous malformations (PAVM's) are rare vascular anomalies involving the
pulmonary vessels. Patients with PAVM are commonly asymptomatic despite the presence of a
right to left shunt. We report aninteresting case of a patient with multiple PAVMs complicated with
recurrent paradoxical brain embolism and leads to cerebral infarction.
Keywords: Pulmonary arteriovenous malformation; Stroke; CT; Embolism
Abbreviations
PAVM: Pulmonary Arteriovenous Malformation; CT: Computed Tomography; GCS: Glasgow Coma Scale
Introduction
Pulmonary arteriovenous malformation (PAVM) is defined as an abnormal communication between the pulmonary arteries and veins. It is a relatively rare finding and patients are commonly asymptomatic despite the presence of a right to left shunt [1,2]. However, it is well recognized as one of the many causes of paradoxical stroke [3]. Brain infarction associated with PAVMs often occur in patients with bigger feeding arteries (> 3mm ) but not in small or tiny vessels [3]. We report a case of a patient with multiple PAVMs leads to paradoxical embolic cerebral infarct.
Case Presentation
An 85 year-old man, underlying rheumatoid arthritis presented with fall prior to hospital
admission. On presentation he was noted to have left sided body weakness (power of both upper
and lower limb 3/5), facial asymmetry and slurred speech. Patient was alert and GCS was full. His
blood pressure was high on admission (170/84 mmHg). Initial CT brain showed an acute infarct
in right centrum semiovale. He was then started on acetylsalicylic acid 100 mg once daily and
admitted to ward for further management. However, in the ward, he developed worsening left sided
body weakness. At day 3 of admission, there was worsening speech and no improvement of the
weakness. GCS remained full. A repeated CT brain demonstrated evolving right basal ganglia with
haemorrhagic transformation and acute infarct of the midbrain and pons (Figure 1). Aspirin was
stopped immediately. Subsequently patient was monitored closely in the ward.
At day 13 of admission, he complained of dyspnea with SpO2 dropped to 90%. CXR showed few
small well circumscribed round opacities at both lower lobes as shown in Figure 2. Immediately the
medical team requested for a CT Pulmonary Artery (CTPA) scan to rule out pulmonary embolism.
The CT scan showed multiple pulmonary arteriovenous malformations as evidenced by serpiginous
feeding and draining vessels from the pulmonary vasculaturesin right upper and bilateral lower
lobes as shown in Figure 3 and Figure 4. There were also airspace consolidations in right middle
and lower lobes. The radiological diagnosis was multiple pulmonary arteriovenous malformations
associated with active lung infection. The earlier CT scans of brain showing cerebral infarcts were
likely due to paradoxical emboli from PAVM. Subsequently he was treated for pneumonia requiring
IV antibiotics and non-invasive oxygen treatment. Patient was offered for diagnostic pulmonary
angiography and embolization under interventional radiological department. However, due to
financial constraint, no further treatment was done. After 2 days, patient was discharged with
Aspirin 100 mg daily and scheduled for follow up in the outpatient clinic.
Figure 1
Figure 1
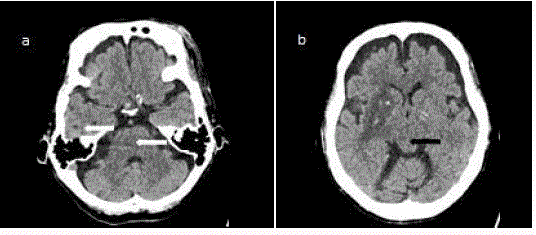
Plain CT brain in axial views showing (a) right temporal lobe,
pontine infarcts (white arrows and (b) midbrain infarct (long black arrows) and
right basal ganglia (short white arrow). Hyperdensities noted within the right
basal ganglia consistent with haemorrhagic transformation (short arrows).
Figure 2
Figure 2
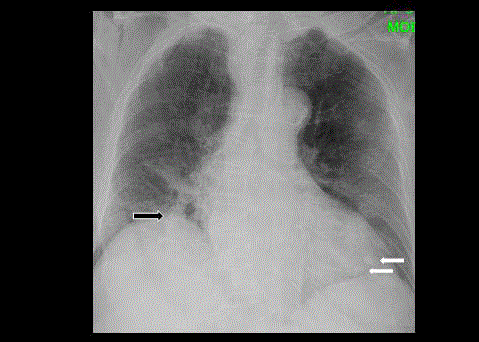
Chest radiograph showing several well defined hyperdense
nodules in the right lower lobe (black arrow) and left lower lobe (white arrow).
Discussion
PAVM (Pulmonary Arteriovenous Malformations) is a vascular
malformation between the pulmonary arteries and veins causing
right-to-left shunt [2]. It is rare and usually detected as an incidental
finding or on autopsies [2]. PAVMs are always associated with
Hereditary Hemorrhagic Telangiectasia (HHT), also known as
Osler–Weber–Rendu syndrome, which is an autosomal dominant
syndrome [1]. Approximately 15%–35% of patients with HHT have
associated with PAVMs and 50%–85% of PAVMs patients were
diagnosed to have HHT [3].
Majority of patients (more than 50%)with PAVM have the
abnormal vessels located in unilateral segments of lower lobe.One
of the most important complications of PAVM is cerebral infarction
where it occurred due to continuous right-to-left shunting [3].
Sometimes stroke is the first presentation of PAVM, in particular
HHT patients with undiagnosed PAVM in [3]. Moussouttas et al. [4]
has concluded that cerebral infarction are likely to occur in PAVM
patients with feeding arteries of more than 3 mm in diameter. This
finding was consistent with the current case scenario whereby the
feeding artery is 3.5 mm in diameter. Therefore, PAVM embolization
therapy was recommended for this patient [4]. However, procedure
was not proceeding due to financial constraint.
Figure 3
Figure 3
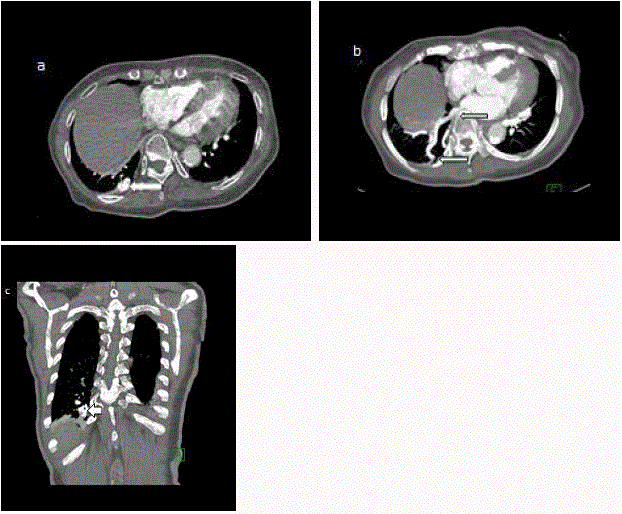
CECT thorax (a,b) in axial views (c) in coronal view showing a
arteriovenous malformation in the right lower lobe near the pleural surface
which appeared to be a serpiginous pulmonary vein (arrows).
Figure 4
Figure 4
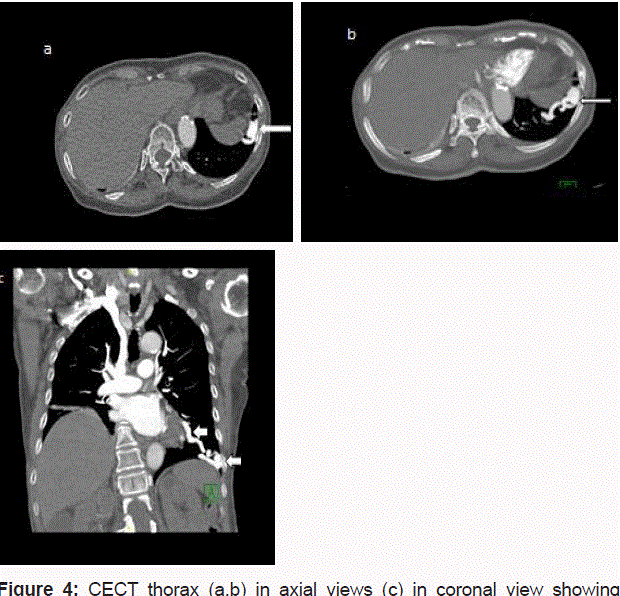
CECT thorax (a,b) in axial views (c) in coronal view showing
another similar dilated tubular vessels (long arrows) in the left lower lobe
which communicated by a feeding artery measuring 4.6mm in diameter
(short arrows).
Conclusion
PAVMs are relatively rare vascular anomaly with a strong association between PAVM and HHT [5]. Chest radiograph can often suggests the diagnosis of PAVM if it is large enough and contrast enhanced CT of the thorax or pulmonary angiography is confirmative [6]. Our case history presents a rare cause of embolic stroke with haemorrhagic transformation likely from PAVMs. In those patients with cerebral infarction secondary to embolism from PAVM, long-term thrombolytic therapy may be an option for stroke prevention [2].
References
- Kareem Abed, Lalith Premachandra, Viren Vankawala, Qi Sun. Intrapulmonary arteriovenous malformation causing recurrent strokes. J Community Hosp Intern Med Perspect. 2015; 5.
- Sabrina Anticoli, Francesca Romana Pezzella, Antonio Siniscalchi, Luca Gallelli, Maria Cristina Bravi. Pulmonary arteriovenous malformation as a cause of embolic stroke: case report and review of the literature. Interv Neurol. 2015; 3: 27-30.
- Kenichi Todo, Hiroshi Moriwaki, Masahiro Higashi, Kohji Kimura, Hiroaki Naritomi. A small pulmonary arteriovenous malformation as a cause of recurrent brain embolism. AJNR Am J Neuroradiol. 2004; 25: 428-430.
- Moussouttas M, Fayad P, Rosenblatt M, Hashimoto M, Pollak J, Henderson K, et al. Pulmonary arteriovenous malformations cerebral ischemia and neurologic manifestations. Neurology; 2000: 55: 959-964.
- Khurshid I, Downie GH. Pulmonary arteriovenous malformation. Postgrad Med J. 2002; 78: 191-197.
- Remy J, Remy-Jardin M, Wattinne L, Deffontaines C. Pulmonary arteriovenous malformations: evaluation with CT of the chest before and after treatment. Radiology, 1992; 182: 809-816.