Case Report
Neurobrucellosis: An Unusual Location of Brucellosis
Rym Abid*, Olfa Smaoui, Imene Oueslati, Souha Hannachi, Riadh Battih and Bessem Louzir
Department of Internal Medicine, Military Hospital of Tunis, Tunisia
*Corresponding author: Rym Abid, Department of Internal Medicine, 1008 Montfleury, Military Hospital of Tunis, Tunisia
Published: 20 Jun 2018
Cite this article as: Abid R, Smaoui O, Oueslati I, Hannachi
S, Battih R, Louzir B. Neurobrucellosis:
An Unusual Location of Brucellosis. Ann
Clin Case Rep. 2018; 3: 1525.
Abstract
Man, 33 years old, a farmer, who had since two months an alteration of the general state and
paresthesia type burn in lower and upper limbs, associated to weakness of the four limbs with
progressive worsening, then appearance of instability to walking. Physical examination was
objectified tetraparesia predominant in distal and posterior cord syndrome as well as static and
kinetic cerebellar syndrome. The lumbar puncture had objectified hyper proteinorachie without
other abnormalities. Cerebro-spinal cord MRI had shown a cerebellar and thalamus impairment.
The serology of brucellosis in blood was positive. The diagnosis of neurological brucellosis had been
retained. The patient was put under a triple therapy of antibiotics associated with corticotherapy
with a good clinical improvement.
Keywords: Neurobrucellosis; Serology; Cerebellitis; Paralysis
Introduction
Brucellosis is an anthropozoonotic infection caused by bacteria of the genus Brucella. Its extension is worldwide with predominance in the Mediterranean basin and the developing countries. The clinical presentations of human brucellosis are polymorphic [1]. Neurological involvement remains rare but serious. The diagnosis of neurobrucellosis is based on the association of general and neurological clinical manifestations, brain imaging, serology of brucellosis and or positive blood cultures and a favorable response under specific treatment [1,2]. The purpose of our work is to recall this localization of brucellosis and to insist on the need for rapid and prolonged therapeutic management.
Case Presentation
He was a 33-year-old man with no particular pathological background. He was a farmer from the
North West of Tunisia. The patient had consulted for neurological signs appeared since 2 months.
He complained of paresthesia type burns with muscle weakness of the four limbs and instability in
walking appeared since two months. The patient had an impairment of general condition with a
weight loss of 30 kg in two months and anorexia, without fever or night sweats.
The patient had not fever, with cardiopulmonary, abdominal and osteoarticular examination
without abnormalities. Neurologically, he was aware and well oriented in time and space. The
cranial nerves were intact. He had muscular atrophy of the four limbs with tetraparesia predominant
in lower limbs. The patellar and ankle reflexes were absent on both sides with an impairment of
the superficial sensitivity predominant in lower limbs. A static and kinetic cerebellar syndrome
was objectified by a Romberg sign, incoordination in the finger-nose test, an ataxic walk with
enlargement of the support polygon and difficulty in walking at a straight line, worsening all when
closing the eyes. The electromyogram confirmed the neurogenic involvement of the four limbs
with a severe axonal sensitivo-motor neuropathy predominant in the lower limbs. A cerebro-spinal
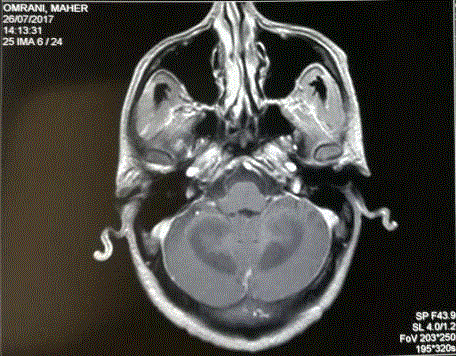
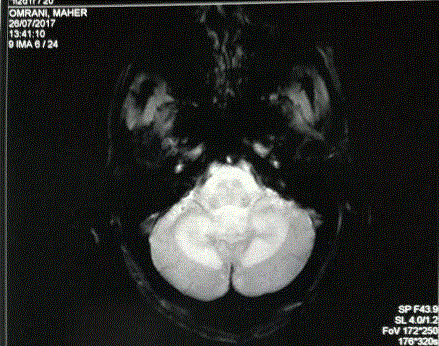
MRI showed diffuses lesions in hyposignal T1 and hyperintense T2 Flair at the posterior fossa and
involvement of the cerebellar white matter with enhancement after gadolinium injection (Figures 1
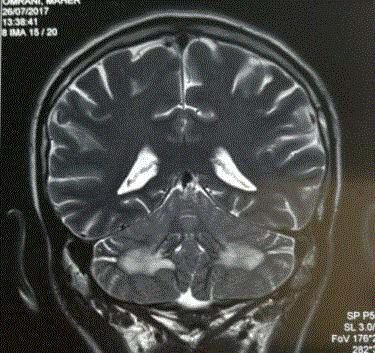
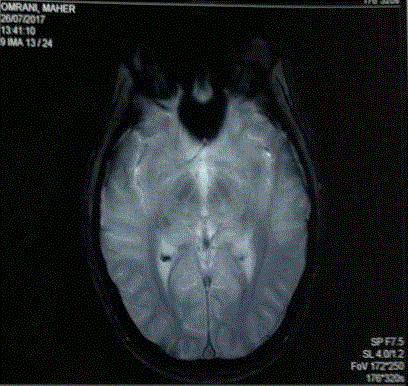
and 2). In the two thalami, a lesion was individualized in hyposignal T1 and hyperintense T2 Flair,
enhancing after gadolinium injection (Figures 3 and 4). The biological assessments were without
abnormalities, in particular no biological inflammatory syndrome and no abnormalities in the
blood count. The study of cerebro-spinal fluid showed a clear appearance with normal cytology
(WBC= 2 / mm3), normal glucorrachia, hyper proteinorachie at 1.29 g/l and negative culture. Given
the epidemiological context, a serology of brucellosis was requested, and was positive: Bengal Rose
Test +++ and Wright serology in blood was positive at 1/360. The blood cultures were negatives. The
diagnosis of neurobrucellosis was retained with polyradiculoneuritis and cerebellitis. The patient
has received a triple antibiotic therapy based on Rifampicin (15 mg/kg/day), Doxycycline 200 mg/ day and Sulfamethoxazole-trimethoprim (40 mg/kg/day), associated
with oral corticosteroid therapy (prednisone) at a dose of 1 mg/kg/
day for two weeks and then at a regressive dose of 10 mg/week. He
has received also Pregabalin for neurogenic pain. The evolution was
marked by progressive clinical improvement with improvement of
walking after two weeks and of cerebellar syndrome after 2 months, as
well as a decrease in Wright's serology rate and a regression of brain
lesions in control imaging. The total duration of treatment was 12
months. The patient had kept memory problems as sequels.
Figure 1
Figure 2
Discussion
Brucellosis is the most common zoonotic infection in the world. Its
incidence varies from one country to another. It is still a public health
problem in the Mediterranean basin [1]|. The mode of transmission
of this infection is generally digestive by the consumption of
unpasteurized dairy products or cutaneo-mucus by contact with the
flock. Brucella melitensis is the species most frequently responsible for
human brucellosis [2,3].
Neurological involvement in brucellosis is rare but serious. It was
first described by Hughes in 1896. The neurological manifestations
can be seen at different stages of the disease: in the acute phase of
brucellosis and in the sub-acute or chronic phase [1]. Physiologically,
the involvement of the nervous system could be related either the
intracellular development of the bacterium or the immune response
mechanisms of the body against infection [4].
The neurological involvement of brucellosis is polymorphic and
can affect both the central and peripheral nervous system. Several
clinical presentations are possible. Meningitis and encephalitis are
the most common sites in brucellosis. However, it may be myelitis,
polyradiculoneuritis or sometimes diffuse involvement. Cerebellitis is
an unusual complication of brucellosis and is poorly described in the
literature [1,5,6]. In our case, it was the combination of a peripheral
polyradiculoneuropathy and a cerebellitis.
Neurobrucellosis must be evoked in association with an orienting
epidemiological context, lesions of the nervous system not explained
by another neurological pathology with confirmation of systemic
progressive brucellosis, either by serology or blood cultures [5,7]. In
fact, blood cultures are positive in 24% of cases of neurobrucellosis [1].
Cerebro-spinal fluid study assists in the diagnosis of neurobrucellosis
if meningitis or meningoencephalitis is suspected. It typically shows
lymphocytic meningitis [5,7]. Cerebrospinal fluid culture is positive
for Brucella in 14% of neurobrucellosis [1].
At radiological explorations, neurobrucellosis can be manifested
essentially by three types of lesions: inflammatory lesions,
abnormalities of the white matter signal and ischemic vascular lesions
[5,8].
The management of neurobrucellosis should be fast and effective
because of the severity of the pathology. Treatment should include
active antibiotics on Brucella and with good neuromeningeal
diffusion for a long period. There is no consensus on the choice of
antibiotic, the dose and the duration of treatment of neurobrucellosis,
but the treatment is usually based on a combination of two or
three antibiotics among doxycyclin, rifampicin, trimethoprimsulfamethoxazole,
streptomycin or ceftriaxone [1,9,10]. The duration
of treatment is variable ranging from 2 to 15 months, but duration
of at least 6 months is recommended [1,5,11]. The indication of
corticosteroids in the therapeutic management of brucellosis in
combination with antibiotics is not well codified. Corticosteroid
therapy is recommended in order to act on inflammatory process.
Some authors indicate corticosteroid therapy systematically in
front of a neurobrucellosis while others prescribe it in case of severe forms: arachnoiditis, cranial nerve damage, myelopathy, intracranial
hyperpressure, optic neuritis or papillary syndrome [4,5,9].
The evolution of neurobrucellosis is variable depending on
the type of injury. Paralysis related to brucellosis usually regress
completely with the administration of antibiotics, while the central
nervous system is associated with permanent neurologic deficits.
However, mortality during neurobrucellosis remains low [11,12].
Figure 3
Figure 4
Conclusion
Neurological manifestations of brucellosis are polymorphic and of varying severity. The neurological involvement must be suspected on clinical and or radiological abnormalities, in an epidemiological context suggestive of brucellosis. Therapeutic management must be rapid but it is not clearly codified.
References
- Hanefi Cem Gul, Hakan Erdem, Semai Bek. Overview of neurobrucellosis: a pooled analysis of 187 cases. Int J Infect Dis. 2009; 13: e339-e343.
- K Skalsky, D Yahav, J Bishara, S Pitlik, L Leibovici, M Paul. Treatment of human brucellosis: systematic review and meta-analysis of randomised controlled trials. BMJ. 2008; 336: 701-704.
- Oueslati, A Berriche, L Ammari, R Abdelmalek, F Kanoun, B Kilani, et. al. Epidemiological and clinical characteristics of neurobrucellosis case patients in Tunisia. Med Mal Infect. 2016; 46: 123-130.
- Akdeniz H, Irmak H, Anlar O, Demiroz AP. Central nervous system brucellosis: presentation, diagnosis and treatment. J Infect. 1998; 36: 297-301.
- Ben Hamouda I, Gouider R, Mrabet A. Neurobrucellose. EMC Neurologie. 2007; 17: 051-B50.
- Shakir RA, Al Din AS, Araj GF, Lulu AR, Moussa AR, Saadah MA. Clinical categories of neurobrucellosis: a report of 19 cases. Brain. 1987; 110: 213-223.
- MA Shaalan, ZA Memish, SA Mahmoud, A Alomari, MY Khan, M Almuneef, et al. Brucellosis in children: Clinical observations in 115 cases. Int J Infect Dis 2006; 6: 182-186.
- Al-Sous MW, Bohlega S, Al-Kawi MZ, Alwatban J, McLean DR. Neurobrucellosis: clinical and neuroimaging correlation. AJNR Am J Neuroradiol. 2004; 25: 395-401.
- Pappas G, Akritidis N, Christou L. Treatment of neurobrucellosis: what is known and what remains to be answered. Expert Rev Anti Infect Ther. 2007; 5: 983-990.
- Koussa S, Tohme A, Ghayad E, Nasnas R, El Kallab K, Chemaly R. Neurobrucellose : étude clinique et thérapeutique de 15 cas. Rev Neurol 2003;159:1148-55.
- Gul HC, Erdem H, Go¨renek L, Ozdag MF, Kalpakci Y, Avci IY, et al. Management of Neurobrucellosis: An Assessment of 11 Cases. Intern Med. 2008; 47: 995-1001.
- Gouider R, Samet S, Triki C, Fredj M, Gargoguri A, el Bahri F, et al. Neurological manifestations indicative of brucellosis. Rev Neurol. 1999; 155: 215-218.