Case Report
Ectopic Pancreatic Tissue of the Proximal Ileum Presented as Acute Appendicitis
Hussain A1*, Obeid N2 and EL-Hasani S2
1Department of General Surgery, Doncaster Royal Infirmary, UK
2Department of General Surgery, Princess Royal University Hospital, UK
*Corresponding author: Abdulzahra Hussain, Department of General Surgery, Doncaster Royal Infirmary, Doncaster, UK
Published: 12 May, 2016
Cite this article as: Hussain A, Obeid N, EL-Hasani S. Ectopic Pancreatic Tissue of the Proximal Ileum Presented as Acute Appendicitis. Ann Clin Case Rep. 2016; 1: 1002.
Abstract
Introduction: The ectopic pancreas of the small bowel is unusual submucosal hamartoma. It may present acutely or as an incidental finding during exploratory laparotomy or diagnostic laparoscopy.
Materials and Methods: This patient presented as acute appendicitis. Gridiron incision was used for exploration and the appendix was normal. Free peritoneal fluid and subserosal mass of about 1.2x1 cm was seen in the proximal ileum. Appendicectomy and exicion of the mass were performed.
Results: The abdominal pain had settled and the patient was discharged 10 days postoperatively. Conclusion: Ectopic pancreatic tissue of gastrointestinal tract is a rare condition and may presents as an acute abdomen.
Keywords: Ectopic pancreas; Gastrointestinal tract; Proximal
Introduction
Ectopic pancreatic (EP) tissue can be defined as normal aciner and ductal pancreatic tissue that has no vascular connection and occupying anatomical site other than the normal pancreas. It is an uncommon submucosal tumour in the gastrointestinal tract (GIT), but histologically similar to normal pancreatic tissue [1]. The presentation may be acute one as in our case, with signs and symptoms of clinical acute appendicitis, while incidental finding during surgery reports vary between 0.17% and 0.83% [2]. It is unlikely to cause acute symptoms but of course, diseases of normal pancreatic tissue such as acute pancreatitis can develop in the ectopic tissues [3]. Most occurrences of heterotopic pancreas are located in the stomach wall, duodenum, and small intestine or anywhere in the gastrointestinal tract [4]. The most common localization was in the prepyloric area and in the duodenal wall, and can be detected in all cases by routine histopathological examination of surgical specimens [5]. Some other rare locations were reported in literature such as anterior mediastinum [6].
Case Presentation
A 26 years old man was admitted through the accident and emergency unit with 5 days history
of vague abdominal pain that shifted to the right iliac fossa and associated with nausea but no
vomiting or fever. The patient has also described an episode of such pain two weeks before his
admission. Review of the other systems was unremarkable. He has no significant medical or surgical
history. On examination his pulse rate was 92/minute, has normal temperature and blood pressure.
No abnormality was reported on chest examination. Abdominal examination revealed right iliac
fossa tenderness with rebound tenderness but no guarding or rigidity. White cell count was 13000/
cmm, Amylase was 61. Liver function, and other blood tests result including C reacting protein was
within normal range.
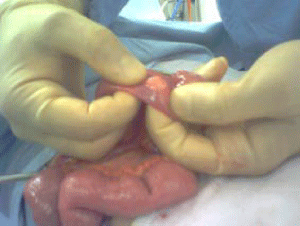
During exploration, there was reactionary peritoneal fluid and the appendix was macroscopically
normal. Examination of the rest of the bowel, surprisingly, showed a subserosal mass of 1.2x1 cm
at the antimesenteric border of the proximal ileum (Figure 1). Excisional biopsy of this lesion was
performed carefully and serosa was closed with vicryl suture. Appendicectomy was performed
as well. The histopathology examination of the lesion reported as non-inflamed hamartomatous
ectopic pancreatic tissue and the microscopical examination of the appendix was normal.
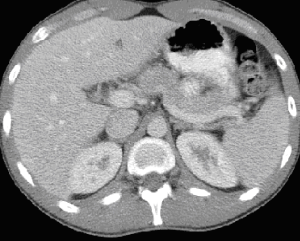
The patient had rough postoperative recovery. Post operative abdominal computed tomography
(CT) scan(Figure 2) and diagnostic laparoscopy showed no abnormality. He was settled and discharged after 10 days. Postoperative follow up in the clinic was unremarkable.
Figure 1
Figure 2
Discussion
The operative confirmation of clinical diagnosis of acute abdomen
is crucial, however it is not possible in every case and negative
exploration or missed pathology are the possibilities. Sometimes a
surprising pathology is found incidentally during exploration. One
of these rare pathologies is the EP that may presents clinically as
acute appendicitis and therefore normal looking appendix during
operation will require surgeons to find a cause for the patient
symptoms and signs. EP is extremely difficult to be diagnosed on
clinical or cross sectional imaging; in fact, most of the cases of EP
are an incidental finding, although in retrospective review, symptoms
from EP are reported in up to 50% of the cases [7]. EP tissue should
be considered in the differential diagnosis of GIT mass and the most
common sites are in the stomach wall, duodenum, small intestine
and can cause inflammation and transmural perforation [2]. EP
tissue was reported in literature in young and elderly patients and
was capable of producing symptoms, depending on its location, size,
and involvement of the overlying mucosa [8].
In general, the acute presentation is either abdominal pain, or
luminal bleeding such as malena [9]. Camunas Mohinelo et al. [10] described 10 cases presented as GIT bleeding, chronic gastro duodenal
ulcers, pancreaticobiliary disease, and suprarenal abnormalities. EP
of the duodenum may presents with symptoms and radiological
findings mimicking superior mesenteric artery syndrome [11].
Magnetic Resonance Cholangio pancreatography MRCP is
helpful in the detection of symptomatic ectopic pancreatitis in the
small-bowel mesentery [12]. CT-enteroclysis was a proved to be
a good method for diagnosis of small bowel EP. This technique,
combining helical CT and small bowel opacification through a nasojejunal
tube, allows detection of small tumours [13]. The enhancement
pattern of EP after intravenous iodine contrast administration is the
same as that of leiomyoma or carcinoid [14]. In cases of GIT bleeding
due to EP, a technetium-99m-labeled RBC scan can show massive
radioactivity in loops of small bowel due to active bleeding and
superior mesenteric angiography may reveal a hypervascular stained
mass supplied by proximal jejunal branch [9].
The possibility of acute pancreatitis was not confirmed in the
histology of excised EP in our patient, although this may be the case,
because he had abdominal pain two weeks before admission, he
might be in the resolving period with normal amylase during that
admission. We found no cause to account for his symptoms. We
performed excision of the lesion and closure of the serosa as excision
of the EP is the treatment of choice in all cases [9,10,14].
Conclusion
Ectopic pancreatic tissue of gastrointestinal tract is a rare condition and may presents as an acute abdomen. Excisional biopsy is treatment of choice and it is feasible without segmental bowel resection, especially for small lesion.
References
- Chen HL, Lin SC, Chang WH, Yang TL, Chen YJ. Identification of ectopic pancreas in the ileum by capsule endoscopy. J Formos Med Assoc. 2007; 106: 240-243.
- Petersen CD, Skarbye M. Small-intestine tumor with ectopic pancreas tissue and acute pancreatitis. Ugeskr Laeger. 2005; 167: 3601-3602.
- Mulholland KC, Wallace WD, Epanomeritakis E, Hall SR. Pseudocyst formation in gastric ectopic pancreas. JOP. 2004; 5: 498-501.
- Zinkiewicz K, Juśkiewicz W, Zgodziński W, Szumiło J, Cwik G, Furtak J, et al. Ectopic pancreas: endoscopic, ultrasound and radiological features. Folia Morphol (Warsz). 2003; 62: 205-209
- Mocny G, Krzeszowiak J, Kedra B. Ectopic pancreas in the surgical practice. PrzeglLek. 2003; 60: 640-641.
- Tamura Y, Takahama M, Kushibe K, Taniguchi S. Ectopic pancreas in the anterior mediastinum. Jpn J Thorac Cardiovasc Surg. 2005; 53: 498-501.
- Maggi G, Navarra L, Cianca G, Vittorini V, Ciccarelli O, Pietroletti R, et al. Ectopic pancreas in Meckel's diverticulitis: a description of a new clinical case. Ann Ital Chir. 2002; 73: 647-649.
- Joo YE, Kim HS, Choi SK, Rew JS, Park CS, Kim YJ, et al. Massive gastrointestinal bleeding caused by ectopic pancreas mimicking jejunal tumor. Digestion. 2001; 64: 133-136.
- Nakamura H, Motegi S, Nishizaki Y, Muramatsu C, Kobayashi F, Itakura M, et al. A case of ileal heterotopic pancreas causing melena. Nihon Shokakibyo Gakkai Zasshi. 2001; 98: 549-552.
- Camuñas Mohinelo FA, Estrada Caballero JL, Trigueros Mateos M, Carrión Tomás A, Coloma Lidón JV, Cañellas Sierra G. Ectopic pancreas. Rev Esp Enferm Dig. 1996; 88: 672-676.
- Verma R, Abraham DT, Joseph P, Nayak S, Agarwal S. Ectopic pancreas mimicking superior mesenteric artery syndrome. Indian J Gastroenterol. 2003; 22: 105-106.
- Silva AC, Charles JC, Kimery BD, Wood JP, Liu PT. MR Cholangiopancreatography in the detection of symptomatic ectopic pancreatitis in the small-bowel mesentery. AJR Am J Roentgenol. 2006; 187: W195-197.
- Ménard Y, Martins A, Crombé A, Fouque P, Orjollet C, Henry L, et al. [Ectopic pancreas located in the small bowel: CT-endoscopic appearance. Apropos of two cases]. J Radiol. 1999; 80: 943-944.
- Wang C, Kuo Y, Yeung K, Wu C, Liu G. CT appearance of ectopic pancreas: a case report. Abdom Imaging. 1998; 23: 332-333.