Case Report
Obsessive-Compulsive Disorder Possibly Secondary to Dilated Perivascular Space in Left Lentiform Nucleus: A Case Report
Zhao Zhenru1, Leow Hong Foo2 and Ng Beng Yeong2*
1Department of Psychiatry, National Health Group, Singapore
2Department of Psychiatry, Singapore General Hospital, Singapore
*Corresponding author: Ng Beng Yeong, Department of Psychiatry, Singapore General Hospital, 20 Academia Road, Singapore
Published: 31 May, 2016
Cite this article as: Zhenru Z, Foo LH, Yeong NB.
Obsessive-Compulsive Disorder
Possibly Secondary to Dilated
Perivascular Space in Left Lentiform
Nucleus: A Case Report. Ann Clin Case
Rep. 2016; 1: 1016.
Abstract
This case report presents symptoms of obsessive-compulsive disorder (OCD) in a previously healthy 66 year-old man, who was found to have a dilated perivascular space in the left lentiform nucleus. This report is consistent with recent imaging studies implicating the basal ganglia in the pathogenesis of obsessive-compulsive disorder and adds the experience of treating a patient with OCD induced by structural damage of lentiform nucleus.
Keywords: Obsessive-compulsive disorder; Dilated perivascular space; Lentiform nucleus
Introduction
Obsessive-compulsive disorder (OCD) is a common mental illness which usually starts in
the second decade of life. Onset after age of 50 is relatively rare and may be more likely to have
an organic aetiology [1-3]. Late-onset OCD can be associated with a number of cerebral lesions
including traumatic brain injury, tumours, haemorrhages and infarcts [4] in certain brain areas
such as the frontal lobes and basal ganglia [5]. Here we report a case of a 66-year-old gentleman
presenting with OCD symptoms after structural change of left lentiform nucleus. He responded
partially to pharmacological treatment.
Case Report
Mr M is a 66-year-old right handed Malay gentleman who first presented to a medical ward in
our hospital in Jan 2016, displaying repetitive, intrusive and distressing thoughts that 'God is evil'
in the preceding two months. He could recognize that these were his own thoughts. He tried to stop
the thoughts by excessively praying or talking to him, but he could not resist them. No depressive or
psychotic symptoms were elicited.
He does not have any past psychiatric history or family history of mental illness; He has never
taken any psychiatric medications before and he does not abuse alcohol or illicit drugs. A systemic
review showed he had been diagnosed with hypertension and diabetes. His pre-morbid character was
described as out-going and cheerful. He had high-school education and worked as a bank executive.
He is married and has four children and a stable and content family
life. He is a religious person, believes in Islam and prays 5 times a
day. He has sought help from his religious teachers before seeking
treatment from doctors.
Physical and neurological examinations were unremarkable.
A brain computed tomography (CT) scan revealed a non-specific
hypodense focus in left lentiform nucleus, and the configuration
suggested dilated perivascular space and chronic in nature (Figure 1).
He was diagnosed with OCD according to DSM-V criteria.
He was treated with fluoxetine and the medication was titrated up
to 80 mg a day. He was calmer and less distressed by the obsessive
thoughts, suggesting a partial remission of his OCD symptoms had
been achieved after 3 months of treatment. Because of his religious
belief, it is hard to involve him in psychological treatments as he finds
it distressing even to elaborate on his obsessive thoughts; it is a great
religious taboo to talk about negative things in relation to his religion.
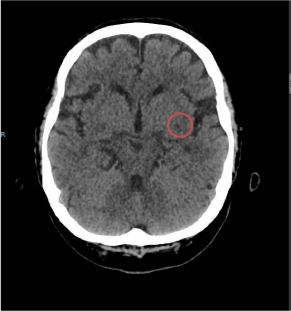
Figure 1
Figure 1
A non-specific hypodense focus in left lentiform nucleus, and the configuration suggested dilated
perivascular space.
Discussion
In this case report we describe a patient, who developed
OCD symptoms that could be due to structural change of left
lentiform nucleus. There is no focal neurological deficit and only
partial remission of his OCD symptoms has been achieved with
pharmacotherapy.
Because OCD is an illness that usually presents in the second or
third decade of life, onset after age 50 should alert the physician to
possible "organic" causes of OCD symptomatology [6,7]. For this
patient, the location of dilated perivascular space in left lentiform
nucleus is in agreement with current theories that basal ganglia
dysfunction in the pathogenesis of OCD[8].
The treatment with high dose of fluoxetine reduced the frequency
and intensity of the symptoms. Permanent neuroanatomical lesions
may partially explain the resistance to treatment with psychotropic
medication [9]. The patient's religious faith also plays a part in his
OCD condition and treatment; research has shown theoretical
linkages supporting both positive and negative religious effects on
mental health including OCD [10]. In the future, involving religious
teachers in his care may be helpful in managing his condition.
In summary, this report adds to a body of evidence
suggesting organic brain lesions can induce obsessive-compulsive
symptomatology and shares our experience in managing such a case.
However, more large scale research is needed to study the pathology
and treatment of brain lesion induced OCD.
References
- Barahona-Corrêa JB, Camacho M, Castro-Rodrigues P, Costa R, Oliveira-Maia AJ. From Thought to Action: How the Interplay Between Neuroscience and Phenomenology Changed Our Understanding of Obsessive-Compulsive Disorder. Front Psychol. 2015; 6: 1798.
- Weiss AP, Jenike MA. Late-Onset Obsessive-Compulsive Disorder: A Case Series. J Neuropsychiatry Clin Neurosci. 2000; 12: 265-268.
- Tonna M, Ottoni R, Ossola P, De Panfilis C, Marchesi C. Late-onset obsessive-compulsive disorder associated with left cerebellar lesion. Cerebellum. 2014; 13: 531-535.
- Etcharry B, Dubas F. Obsessive-compulsive disorders associated with focal brain lesions. In: Behaviours and Mood disorders in Focal brain Lesions. Cambridge. UK. Cambridge University Press. 2000; 304-326.
- Göttlich M, Krämer UM, Kordon A, Hohagen F, Zurowski B. Decreased limbic and increased fronto-parietal connectivity in unmedicated patients with obsessive-compulsive disorder. Hum Brain Mapp. 2014; 35: 5617- 5632.
- Diamond A, Ondo WG. Resolution of severe obsessive--compulsive disorder after a small unilateral nondominant frontoparietal infarct. Int J Neurosci. 2011; 121: 405-407.
- Katz BS, Flemming KD. Obsessive compulsive disorder due to a cavernous malformation hemorrhage in the dominant caudate head. J Clin Neurosci. 2015; 22: 398-399.
- Gunaydin LA, Kreitzer AC. Cortico-Basal Ganglia Circuit Function in Psychiatric Disease. Annu Rev Physiol. 2016; 78: 327-350.
- Fineberg NA, Reghunandanan S, Simpson HB, Phillips KA, Richter MA, Matthews K, et al. Obsessive-compulsive disorder (OCD): Practical strategies for pharmacological and somatic treatment in adults. Psychiatry Res. 2015; 227: 114-125.
- Himle JA, Chatters LM, Taylor RJ, Nguyen A. The relationship between obsessive-compulsive disorder and religious faith: Clinical characteristics and implications for treatment. Ann Psychology of Religion and Spirituality. 2011; 3: 241-258.