Case Report
Diagnosis of Spontaneous Vertebral Artery Dissection in a Healthy Teenager
Anders Messersmith*, Robert Ikerd, Sergio Barksdale and Andrew Muck
Department of Emergency Medicine, University of Texas Health Science Center, USA
*Corresponding author: Anders Messersmith, Department of Emergency Medicine, University of Texas Health Science Center, MC7736, 7703 Floyd Curl Drive, San Antonio
Published: 18 Jun, 2018
Cite this article as: Messersmith A, Ikerd R, Barksdale S,
Muck A. Diagnosis of Spontaneous
Vertebral Artery Dissection in a Healthy
Teenager. Ann Clin Case Rep. 2018;
3: 1521.
Abstract
Spontaneous Vertebral Artery Dissection (SVAD) is a rare condition typically characterized by headache, neck pain, and tinnitus with most dissections occurring in middle-aged adults. Spontaneous dissections cause approximately 2% of all strokes, but account for significant morbidity for pediatric patients. We present a case of SVAD in a healthy teenager with atypical symptoms.
Introduction
Spontaneous vertebral artery dissection in the general population is rare occurring with an
annual incidence between 2.5 to 3 cases/100,000 [1]. Most dissections occur during the fifth decade
of life. Spontaneous dissections cause approximately 2% of all strokes, but account for significant
morbidity for pediatric patients.
Three studies conducted in the 1990’s by Schievnik et al. [2-5] attempted to determine the
underlying etiology of SVAD. Autosomal polycystic kidney disease, Marfan syndrome, and Ehlers-
Danlos type IV are associated with a 1%-5% increased risk for SVAD. Family history of SVAD was a
minor risk factor. In 1999, Grau et al. [6] reported that recent respiratory infections are a risk factor.
Although these risk factors are known, due to the overall low incidence of VAD, it is difficult to
apply them as predictors of disease.
According to a 2013 study by Von Babo et al. [7,8], individuals with SVAD typically present with:
cerebral ischemia (84.4%), headache (70.4%), neck pain (65.8%), subarachnoid hemorrhage (6%),
and tinnitus (3.4%). In this report, we present a case in which SVAD was initially misdiagnosed due
to both the lack of risk factors and common symptoms.
Case Presentation
A healthy 16-year-old Caucasian male presented with vertigo, nausea, vomiting, blurred vision,
and left sided extremity weakness. He denied smoking, alcohol, drug use, or family history of
significant disease. Symptoms were present upon waking six days prior. He had been lifting weights
the day before symptoms began, but denied injury. He had been evaluated at an outside hospital
with a normal non-contrast head CT, given a diagnosis of benign positional vertigo, and discharged
home. Despite symptomatic therapy, his symptoms worsened.
The pertinent physical findings on presentation to our emergency department: blood pressure
148/91, heart rate 57, with normal temperature, pulse oximetry, and respiratory rate. The right pupil
was 3 mm in diameter with minimal response to light and accommodation. Cranial nerves were
otherwise intact. There was 4/5 strength in the left upper and lower extremity versus 5/5 on the right
side. A decrease in sensation was noted to light touch and temperature in his left arm and leg. A mild
left dysmetria was observed. The patient was unable to stand due to loss of balance.
Blood work showed a normal CBC, chemistry, and INR. A Computer Topography (CT)
angiogram of the neck was performed and revealed an occlusion of the distal segment of the
right vertebral artery (Figure 1). Magnetic Resonance (MR) imaging of the brain showed acute
right posterior inferior cerebellar artery territory infarctions located at the inferior cerebellum
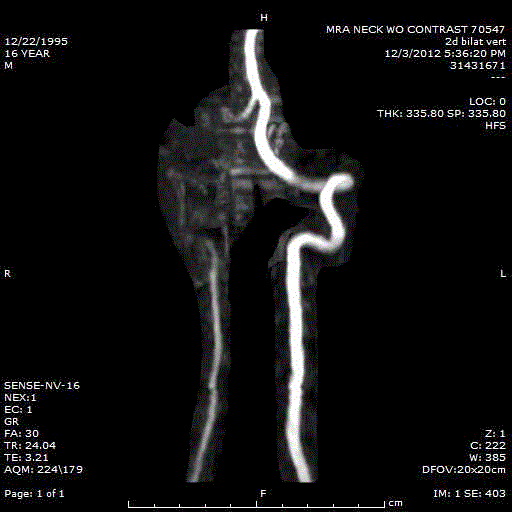
and posterior medulla (Figure 2). A MR angiogram of the neck revealed a right vertebral artery
dissection (Figure 3).
He was admitted to the hospital and oral aspirin therapy was initiated for treatment of the VAD.
No invasive intervention or further anti-coagulation was deemed necessary by the neurosurgery
team [9,10]. The patient had an uneventful hospital course. He was discharged five days after
admission on aspirin therapy with three months abstinence from weight lifting and contact sports.
At three month follow up he was doing well with resolution of his
symptoms.
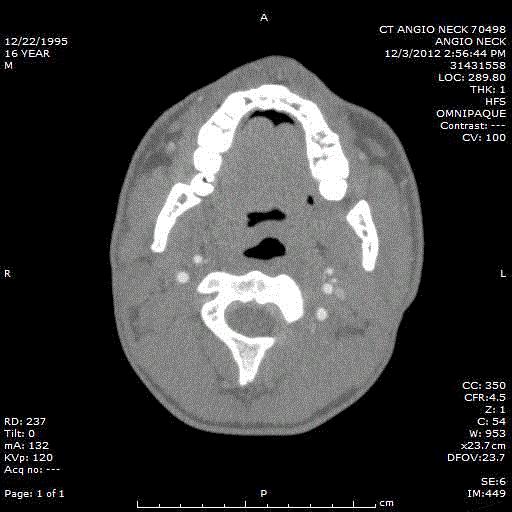
Figure 1
Figure 1
A Computer Topography (CT) angiogram of the neck was performed
and revealed an occlusion of the distal segment of the right vertebral artery.
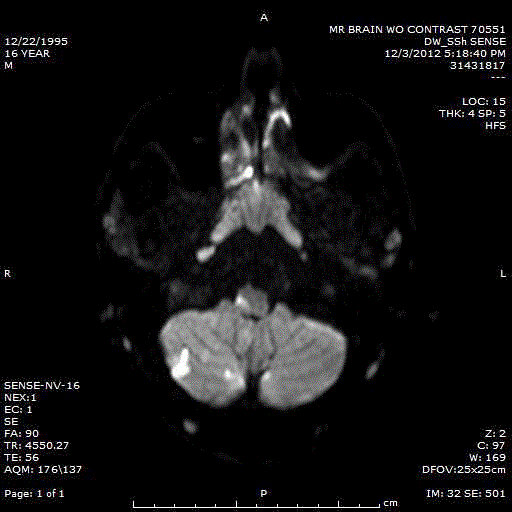
Figure 2
Figure 2
Magnetic Resonance (MR) imaging of the brain showed acute right
posterior inferior cerebellar artery territory infarctions located at the inferior
cerebellum and posterior medulla.
Discussion
Of 134 patients retrospectively studied with spontaneous vertebral
artery dissection, the most common presenting symptoms were head
and/or neck pain, and pulsatile tinnitus with 13 (8%) asymptomatic
[8]. Many other diagnoses can present with vertigo, nausea and
vomiting such as benign positional vertigo, alcohol intoxication, and
post concussion syndrome. Spontaneous vertebral artery dissection is
such an uncommon entity that in this case it is not unexpected that
this patient’s initial evaluation did not lead to the correct diagnosis.
A concerning aspect of this teenager’s physical examination
was the unilateral extremity weakness with vision complaints. Any
posterior circulation symptoms and extremity weakness should raise
a red flag and prompt further investigation to include neuroimaging.
Conclusion
Spontaneous vertebral artery dissection is a rarely encountered clinical problem. In this case report, we describe a healthy 16-year- old Caucasian male with vertigo, nausea, vomiting, blurred vision, and left sided extremity weakness. Diagnostic imaging should be considered in a young patient with an unexplained focal neurologic deficit due to the higher association of ischemic stroke and vertebral artery dissection in this population.
Figure 3
Acknowledgment
The authors acknowledge the University of Texas Health Science Center at San Antonio Departments of Radiology and Neurosurgery.
References
- Redekop G. Extracranial carotid and vertebral artery dissection: A review. Can J Neurol Sci. 2008; 35:146-152.
- Schievink WI. The treatment of spontaneous carotid and vertebral artery dissections. Curr Opin Cardiol. 2000; 15: 316-321
- Schievink WI, Mokri B, Whisnant JP. Internal carotid artery dissection in a community: Rochester, Minnesota, 1987-1992. Stroke. 1993; 24: 1678- 1680.
- Schievink WI, Mokri B, O'Fallon WM. Recurrent spontaneous cervical artery dissection. N Eng J Med. 1994; 330: 393-397.
- Bassetti C, Carruzzo A, Sturzenegger M, Tuncdogan E. Recurrence of cervical artery dissection: a prospective study of 81 patients. Stroke. 1996; 27: 1804-1807.
- Grau AJ, Brandt T, Buggle F, Orberk E, Mytilineos J, Werle E, et al. Association of cervical artery dissection with recent infection. Arch Neur. 1999; 56: 851-856.
- Michelle von Babo, Gian Marco De Marchis, Hakan Sarikaya, Christian Stapf, Fréderique Buffon, Urs Fischer, et al. Differences and similarities between spontaneous dissections of the internal carotid artery and the vertebral artery. Stroke. 2013; 44: 1537-1542.
- Arnold M, Bousser MG, Fahrni G, Fischer U, Georgiadis D, Gandjour J, et al. Vertebral artery dissection: presenting findings and predictors of outcome. Stroke. 2006; 37: 2499-2503.
- Shea K, Stahmer S. Carotid and vertebral arterial dissections in the emergency department. Emerg Med Pract. 2012; 14: 1-23.
- Chandra A. Spontaneous Dissection of the Carotid and Vertebral Arteries: the 10-year UCSD experience. Ann of Vasc Surg. 2007; 21: 178-185.