Case Report
Ruptured Intracranial Dermoid Cyst: A Rare Cause of Post-Partum Seizures
William B Welte*, Daniel R Calnan and Harman S. Gill
Department of Emergency Medicine and Critical Care, Dartmouth-Hitchcock Emergency Medicine, USA
*Corresponding author: William B Welte, Department of Emergency Medicine and Critical Care, Dartmouth-Hitchcock Emergency Medicine, 1 Medical Center Dr, Lebanon, NH 03766, USA
Published: 05 Mar,2018
Cite this article as: Welte WB, Calnan DR, Gill HS.
Ruptured Intracranial Dermoid Cyst: A
Rare Cause of Post-Partum Seizures.
Ann Clin Case Rep. 2018; 3: 1507.
Abstract
In this case report we will discuss a 34-year-old female who presented six months post-partum with headaches, auras and burning in her arm. Progressive weakness ultimately lead to confusion and generalized tonic-clonic seizure on arrival to the emergency department. After stabilization, she was found to have a ruptured, intracranial dermoid cyst which had spread sebum throughout her central nervous system. She developed chemical meningitis as a result, and had a myriad of neurological symptoms including word finding difficulties, decreased sensation and seizures. Her cyst was resected and she has been doing well. In a post-partum patient, ruptured intracranial dermoid cyst is an abnormal cause of headaches and seizures. Going unrecognized, severe neurological outcomes are probable. In this case report we will discuss her presentation, identification of her mass and therapeutic measures undertaken.
Case Presentation
A 34-year-old female was brought to the Emergency Department (ED) for right sided
hemiparesis, expressive aphasia and confusion. She was six months post-partum and had a history
of depression, GERD, chronic urinary tract infections and pyelonephritis. For the past three months
she began to have daily headaches characterized as dull and worse in the afternoon without associated
nausea/vomiting or visual changes/auras. Over the past week she had been having difficulty holding
her baby due to sensations of extreme heat in her right arm with associated weakness. The day she
presented she was found by her neighbors banging her hand against a wall and confused.
Upon arrival to an outlying ED, she experienced two episodes of generalized tonic-clonic
seizures with rightward gaze preference, each lasting approximately four minutes. Her seizures were
treated with diazepam and a loading dose of Levetiracetam. Head CT demonstrated a 4.4cm extraaxial
mass extending from the suprasellar region with mass effect on right basal ganglia, right lateral
and third ventricles (Figure 1). There was also the presence of sebum in the subarachnoid space and
ventricles.
Upon arrival in our ED at the tertiary care referral center, her symptoms and mental status had
improved. She was able to provide further history given above and initial vitals were as follows:
T 37C (98.6F), HR 81, Resp 19, BP 118/81, SpO2 98% on room air. Exam was remarkable for 5/5
strength in all extremities, but scattered areas of decreased sensation on the dorsum of the right
hand, arm and foot. Her cranial nerves were intact, her speech was remarkable for subtle word
finding difficulties though she remained alert and oriented to person, time and place. She went for MRI with findings likely representing ruptured dermoid cyst
with significant FLAIR signal abnormalities within the left cerebral
hemisphere (Figure 2).
She was admitted to the neurosurgical service for a planned
resection. Over the course of her hospitalization she developed
SIADH which was successfully treated with salt tablets. Her cyst was
resected without incident and she was discharged on post-op day 6.
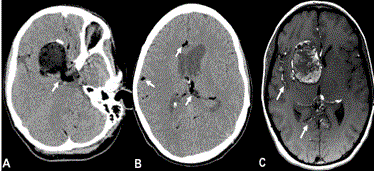
Figure 1
Figure 1
Non-contrast head CT revealed a large right sided cystic mass, ipsilatreral to her symptoms (A) with
hyoidense foci throughout the subarachnoid space (A and B, Arrows). MRI imaging of the brain revealed T1
hyperintensity throughout the subarachnoid space (C, Arrows).
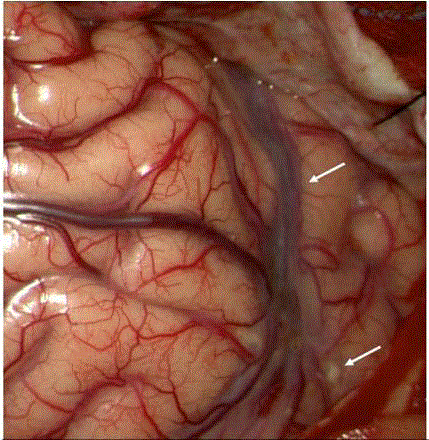
Figure 2
Discussion
Intracranial dermoid cysts are benign growths most commonly
found in the supra/parasellar, or posterior fossa regions. They
characterize only 0.04% to 0.6% of all intracranial neoplasms [1-4].
They are most commonly discovered during the third to fifth decades
of life and usually incidentally, after spontaneous or traumatic
rupture or when symptoms present from mass-effect. Average sizes
tend to be 4 cm to 4.5cm and they grow overtime from the secretion
of sebaceous material into the cyst, along with sloughing of epidermal
cells [1,5]. The clinical signs of rupture include headaches, seizures,
sensory or motor hemiparesis and chemical meningitis which
may have sequelae of cerebral ischemia and possibly death [3,4].
While this case reports a 34-year-old female presenting with classic
features of headache, altered mental status, seizures and hemisensory
deficits after spontaneous rupture of intracranial dermoid cyst; the
existence of these symptoms in a post-partum female and the clinical
correlation of neurologic exam findings in relation to neuroimaging
findings made this case unique.
Dermoid cysts have characteristic CT and MRI findings. On CT
(Figure 1) they have well-demarcated and hypodense appearances
sometimes seen with calcified borders [2,6]. On T1-weighted MRI
sequencing they reveal a hyperintense cyst which is secondary to the
high cholesterol content of the cyst [1,6]. They will typically appear
heterogeneous on T2-weighted images (Figure 1). The fat intensity
signal witnessed on MRI is secondary to sebaceous secretions and
cholesterol [1,4,6].When a dermoid tumor ruptures, fat dropletsappearing
hypodense on CT or hyperintense on T1 MRI-may be
seen scattered and floating within the nondependent portions of
the ventricular system and/or subarachnoid space. Recognition
of rupture makes the availability of a dedicated neuroradiologist
invaluable as this is a rare phenomenon - 5 out of 2707, or 0.18% of
all new CNS tumors operated on during a 12-year period at a major
tertiary care center [8]. Furthermore, rupture can have grave clinical
consequence due to associated aseptic chemical meningitis that
produces irritative effects from the disseminated cholesterol debris
[9] (Figure 2). Chemical meningitis can also lead to cerebral ischemia
due to vasospasm with resultant infarction and death [10,11]. Our
patient had evidence of all of the classic findings associated with a
ruptured intracranial dermoid cyst.
Clinically in a patient with no history of epilepsy, post-partum
seizures are generally eclampsia until proven otherwise. Despite the
common misconception that delivery is the ‘cure’ for preeclampsia
and eclampsia, there have been reported seizures from eclampsia up
to 5 weeks post-partum [7]. This patient was 6 months post-partum
however and given the patient’s blood pressure and CT/MRI findings
usual etiologies such as eclampsia, cavernous sinus thrombosis and
CNS infections became unlikely diagnoses in her case.
After her seizures the patient in the ED only had subtle right
arm sensory deficits and expressive aphasia. In a report by El-Bahy
et al. [12] symptoms seen after cyst rupture are typically - headache
(32.6%), seizures (26.5%), cerebral ischemia with sensory and/or
motor hemisyndrome (16.3%) and aseptic meningitis (8.2%).Yet, the
inconsistency observed clinically was that her sensory deficits were
ipsilateral to her cortical lesion seen on imaging. Pathophysiologically
this could only be explained by three main mechanisms - mass effect
on neural structures, subarachnoid spread from sebum and cerebral
edema from cyst content or the effect of hydrocephalus. The mass
effect seen on imaging is actually on the R sided cortical tracts and
if affected these fibers would decussate in the medulla and affect
structures on the L side and thus not likely. Though obvious mass
effect was seen on imaging the slow growth of this lesion most likely
allowed structures to shift appropriately without clinical effect.
This slow growth is also the likely reason why there is no associated
hydrocephalus and thus an unlikely explanation of R sided symptoms.
Figure 3 shows clear edema in the contralateral L cerebral hemisphere
with provides a plausible explanation for R sided sensory deficits,
subtle expressive aphasia appreciated on exam alongside a potential
nidus for the initiation of generalized tonic clonic seizure. Postictal
Todd’s paralysis is also plausible but the MRI findings make localized
cerebral edema a more likely culprit. In conclusion, an emergent
MRI in this patient really helped settle the discrepancy between the
clinical and imaging findings and reveal the etiology of symptoms not
apparent on CT imaging.
The timing of her symptoms made her post-partum state
clinically intriguing. Her headaches first started approximately three months ago, followed by heat sensations in her arm all the
way to her acute worsening of headache associated with seizures
that led to her eventual presentation. The exact pathophysiology of
dermoid cyst rupture remains poorly understood. Hypotheses have
included glandular secretions due to age dependent hormones [13],
trauma as well as head movements and brain pulsations [14]. To the
best of these authors knowledge, pregnancy and the well described
post-partum hormonal changes have not been well described as a
possible etiology for spontaneous intracranial dermoid cyst rupture.
Furthermore the literature reports that symptom onset from time
of rupture can vary anywhere from three months to 6.5 years since
the irritative effects of leaked contents require time to develop [15].
It is hypothetically possible that the known post-partum hormonal
changes and specifically their known impact on neuro-hormonal
balance may have led to the rupture of this cyst and/or accelerated
the manifestations of cyst rupture such as headache, aseptic/chemical
meningitis, seizures and cerebral edema.
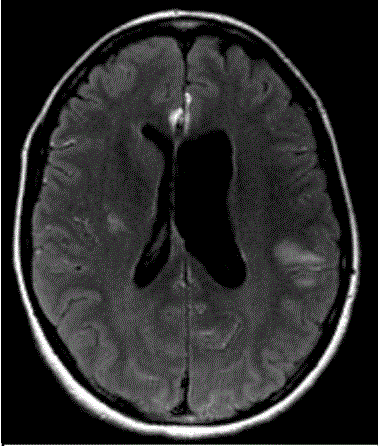
Figure 3
Figure 3
FLAIR hyperintensity of MRI within the left (contralateral) cerebral
hemisphere (D, *) suggesting subarachnoid spread of sebum and cerebral
edema as an etiology for her symptoms.
Conclusion
Intracranial dermoid cyst rupture is a rare etiology of headache, seizures, aseptic/chemical meningitis and neurological deficits. Due to its rare incidence, a multi-disciplinary approach including acute seizure and headache management in the ED, prompt diagnosis on advanced neuroimaging such as MRI by seasoned neuroradiologists and definitive management via resection from an experienced neurosurgery team is of paramount importance. Pregnancy may or may not play a role in the pathophysiologic mechanism of cyst rupture and the rate of manifestations of its associated symptoms.
References
- DG Johnson, SJ Stemper, TK Withers. Ruptured “giant” supratentorial dermoid cyst. J Clin Neurosci. 2005;12: 198-201.
- Ruediger Stendel, Terttu Aulikki Pietilä, Kerstin Lehmann, Ralf Kurth, Olaf Suess, Mario Brock. Ruptured intracranial dermoid cysts. Surgical Neurology. 2002;57:391-398.
- Berhouma Moncef. "Oiled Brain and Status Epilepticus: Intraventricular and Subarachnoid Rupture of a Temporal Dermoid Cyst." Journal of Medical Cases. 2010;1:94-97.
- M Jordan Ray, David W Barnett, George J Snipes , Kennith F Layton , Michael J Opatowsky .Ruptured Intracranial Dermoid Cyst. Proceedings (Baylor University. Medical Center). 2012;25:23-25.
- Fenstermaker RA, Ganz E, Roessmann U. Giant invasive intracerebral dermoid tumour with subependymoma-like reaction: case report. Neurosurgery. 1989;25:646-648.
- Osborn AG, Preece MT. Intracranial cysts: radiologic-pathologic correlation and imaging approach. Radiology. 2006;239:650-664.
- Lakshmi R, Upreti D, Agrawal A, Raina A. Late postpartum eclampsia at five weeks post-delivery. Singapore Med J. 2007;48:946-947.
- Liu JK, Gottfried ON, Salzman KL, Schmidt RH, Couldwell WT. Ruptured intracranial dermoid cysts: clinical, radiographic, and surgical features. Neurosurgery. 2008;62:377-384.
- Venkatesh SK, Phadke RV, Trivedi P, Bannerji D. Asymptomatic spontaneous rupture of suprasellar dermoid cyst: a case report. Neurol India. 2002;50:480-483.
- Smirniotopoulos JG, Chiechi MV. Teratomas, dermoids, and epidermoids of the head and neck. Radiographics. 1995;15:1437-1455.
- Das CJ, Tahir M, Debnath J, Pangtey GS. Neurological picture. Ruptured intracranial dermoid. J Neurol Neurosurg Psychiatry. 2007;78:624-625.
- Cohen JE, Abdallah JA, Garrote M. Massive rupture of suprasellar dermoid cyst into ventricles. Case illustration. J Neurosurg.1997;87: 963.
- Stendel R, Pietila TA, Lehmann K, Kurth R, Suess O, Brock M. Ruptured intracranial dermoid cysts. Surg Neurol. 2002;57:391-398.
- Lunardi P, Missori P. Supratentorial dermoid cysts. J Neurosurg. 1991;75:262-266.
- Venkatesh SK, Phadke RV, Trivedi P, Bannerji D. Asymptomatic spontaneous rupture of suprasellar dermoid cyst: a case report. Neurol India. 2002;50:480-483.