Case Report
Mastoid Mucocele: An Uncommon Alert of Fibrous Dysplasia Onset: Case Report and Literature Review
Davide Brotto1*, Ezio Caserta1, Elisa Lovo1, Renzo Manara2, Sara Ghiselli1, Patrizia Trevisi1, Alessandro Martini1 and Roberto Bovo1
1ENT Unit, Neurosciences Department, Università degli Studi di Padova, Via Giustiniani 2, 35128, Padova, Italy
2Neuroradiology, Università degli Studi di Salerno, Via S. Allende 1, 89081, Salerno, Italy
*Corresponding author: Brotto Davide, ENT unit, Neurosciences Department, Università degli Studi di Padova, Via Giustiniani n. 2, 35128, Padova, Italy
Published: 24 Apr, 2017
Cite this article as: Brotto D, Caserta E, Lovo E, Manara
R, Ghiselli S, Trevisi P, et al. Mastoid
Mucocele: An Uncommon Alert of
Fibrous Dysplasia Onset: Case Report
and Literature Review. Ann Clin Case
Rep. 2017; 2: 1486.
Abstract
The Problem: Fibrous dysplasia affects bone metabolism determining nonmalignant osseous change. Craniofacial skeleton is usually affected and temporal bone involvement is uncommon.
Furthermore, when a concomitant rare mastoid mucocele is already affecting the same region, the
related diagnosis can be even more challenging.
The Methodology: Here we report a radiological and surgical case, with CT, MRI and surgical
imaging of a patient affected by a mastoid mucocele to be considered as a first sign of fibrous
dysplasia onset.
Conclusions: Mastoid mucocele is a rare finding. To date, in medical literature only three cases are
depicted. Etiology is still unknown even if multiple have been the hypothesis put forward. Although
fibrous dysplasia temporal bone localization is well known, to our knowledge, this is the very first
case in medical literature of a mastoid mucocele as an alert of fibrous dysplasia onset.
Keywords: Mucocele; Mastoid; Temporal bone; Head CT; MRI
Introduction
Mucocele is an expansile collection of sterile mucus which, lined by epithelium or covered by
granulation tissue, could be frequently found in oral mucosa. Though only sporadically observable
in the air bones cavities, among them paranasal sinuses are the most predominately involved areas
while temporal bone is hardly affected. Pathology uncommon in adults and rare in childhood,
mucocele is supposed to arise from the obstruction of the normal drainage of mucus in normal
air cells [1]. As a matter of fact, mucosal thickening, bone overgrowth or fibrosis might lead to
progressive inspissation of mucus and bone remodeling with local inflammation, thus determining
the compression of the neighboring structures [2].
Clinical diagnosis, mostly relied on neuroradiological imaging (especially CT and MRI), can
be challenging. Surgery is the gold standard for treatment whilst pathologic confirmation could
be needed in atypical cases. Nowadays, medical literature provides for five cases of temporal bone
mucoceles. Among them only three refer to the mastoid region [2-5].
Craniofacial localization of fibrous dysplasia, especially concerning paranasal sinuses and
midface involvement, is well documented in medical literature as these regions are the most
frequently affected. A recent article by Frisch has extensively presented which the clinical features of
the fibrous dysplasia are and how temporal bone affection can be managed as the pathology is less
common in this bone [6].
Also in consideration of the shortage of articles referring to temporal bone mucoceles available
in medical literature, a case study of a mastoid mucocele to be considered an alert of fibrous dysplasia
onset in a young patient treated with surgical drainage will follow.
Case Report
An 8-years-old boy, with medical history of right purulent otitis media occurred 3 years before, presented with subtle pain and swelling behind the right ear. For diagnostic reasons the patient underwent head CT and head MRI. Consequently a mastoidectomy was performed in order to drain the cyst. After the surgery the patient underwent a follow up head CT.
Figure 1
Figure 1
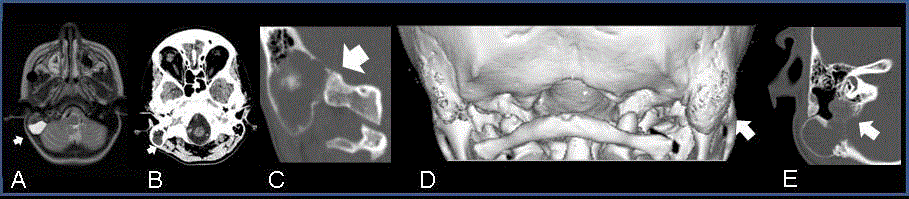
Neuroimaging of mastoid mucocele.
A) Brain MRI, axial T2 image showing a hyperintense mass in the right mastoid (arrow) dislocating the sigmoid sinus, consistent with a mastoid mucocele. B) Head
CT axial image showing isodense tissue and loss of bone septa in the right mastoid (arrow). C) Head CT coronal image showing a loculated cavity (arrow) in the
inferior right mastoid clearly divided by the healthy aerated mastoid. D) Head CT 3D reconstruction showing the enlargement of the right mastoid (arrow) compared
to the contralateral one due to bone remodeling. E) Head CT coronal image showing a new cystic cavity (arrow) posterior to the middle ear.
Figure 2
Figure 2
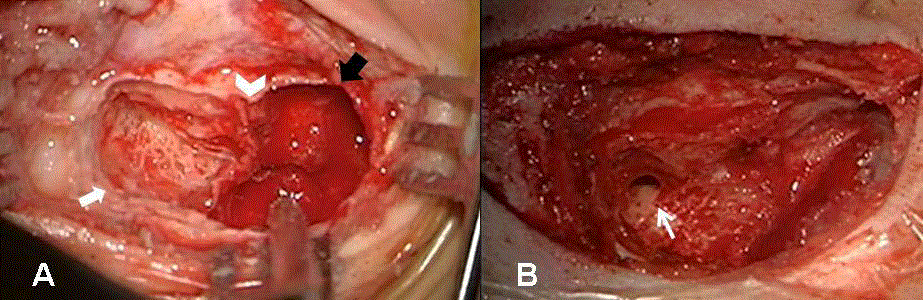
Surgical images during right mastoidectomy for mucocele.
A) The open right mastoid shows the healthy bone (white arrow), the cavity of the mucocele (black arrow) with a highly vascularized wall and a bone septum
dividing the two regions (arrowhead). B) The surgical field after the exposure and drainage of the mucocele with decompression of the sigmoid sinus. The wide
aditus ad antrum (small white arrow) provides a proper aeration of the cavity.
Results
After the clinical evaluation, the patient underwent head CT that
showed a cyst-like lesion (Figure 1B) clearly divided from the healthy
aerated mastoid cells by a bone septum (Figure 1C); the mastoid
proved to be enlarged (Figure 1D). At MRI, the lesion appeared
hyperintense on T2 (Figure 1A) and iso-hypointense on T1 and
diffusion weighted imaging revealed an intense peripheral contrast
enhancement (not shown in figure). The surgical inspection disclosed
a mucus collection with a highly vascularized cyst wall (Figures 2A
and B).
After surgery the patient underwent a follow up CT (Figure 1E),
which show a growing cystic lesion, similar to the one that drove to
mastoidectomy in a more anterior area, in the posterior part of the
middle ear.
Discussion
Fibrous dysplasia is a rare idiopathic, progressive bone remodeling
disorder. Etiology is still unknown. Craniofacial involvement is
frequent, particularly with regards to membranous bones such as
maxilla, mandible, frontal ethmoid, and sphenoidal. Temporal bone
affection is reported to range from 25% to 70% of the cases [6]. The
bone remodeling pattern can be monostotic, affecting a single cranial
bone (70% of cases), or polyostotic thus involving multiple cranial
bones (30% of cases) [7]. Typically, first symptoms debut during the
first or the second decade of life, males are less frequently affected
and clinical features depend on both the site and growth of the lesion.
Prepubertal adolescents can show rampant bone remodeling slowing
down in adulthood [8].
Whenever mastoid is involved, recurrent mastoiditis and conductive hearing loss can be symptomatic indicators.
To our knowledge, no case report in medical literature even
suggests that fibrous dysplasia might appear concomitantly to a
mastoid mucocele.
Only five cases of temporal bone mucoceles are covered by
medical literature [2-5], the latter one reporting lesions found three
times in the mastoid [2-5] and only once in the middle ear [5] or in
the petrous apex [3].
.
Although surgical intervention can be delayed in case of
asymptomatic lesion, in light of the fact that mastoid mucocele,
likewise paranasal sinuses mucocele, is expansile [5], drainage of the
cyst must be performed whenever adjacent structures are involved
[2,9]. For such a purpose, mastoidectomy should be considered a valid
approach to drain the lesion and provide for an adequate aeration.
Conclusion
The etiology of temporal bone mucocele is still unknown
although some authors reported history of chronic otitis media in
patients affected by a temporal bone mucocele [4,5,10], noteworthy, our patient suffered of right purulent otitis media 3 years before
the exordium of the retroauricular swelling. The very same authors
suggest that recurrent local inflammation is supposed to potentially
determine mucosal or bone thickening affecting the ostium of a
normal air cell thus causing a local mucus collection.
In our specific patient, bone remodeling typical of the fibrous
dysplasia might have been started proximal to a mastoid cell ostium,
therefore determining its occlusion causing the collection of mucus
and such atypical bone remodeling.
Postsurgical neuroradiological CT examination showed typical
fibrous dysplasia cystic bone remodeling. Tissue samples are currently
under genetic evaluation to exclude McCune-Albright syndrome.
References
- Huang KL, Huang CC, Lee TJ, Huang CC. An isolated intracranial mucocoele herniated from the frontal sinus. B-ENT. 2015;11:245-247.
- Hwang PH, Jackler RK. Facial nerve dysfunction associated with cystic lesions of the mastoid. Otolaryngol Head Neck Surg. 1998;119:668-672.
- DeLozier HL, Parkins CW, Gacek RR. Mucocele of the petrous apex. J Laryngol Otol. 1979;93:177-180.
- Weichselbaumer W, Kotscher E. Pseudomucocele of the mastoid in chronic otitis media. HNO. 1964 ;12:289-292.
- Karandikar A, Goh J, Loke SC, Yeo SB, Tan TY. Mucous retention cyst of temporal bone: a mimic of cholesteatoma on DW-MRI. Am J Otolaryngol. 2013;34:753-754.
- Frisch CD, Carlson ML, Kahue CN, Pelosi S, Haynes DS, Lane JI, et al. Fibrous dysplasia of the temporal bone: a review of 66 cases. Laryngoscope. 2015;125:1438-1443.
- Albright F, Butler AM, Hampton A, Smith P. Syndrome characterised by osteitis fibrosa disseminata, areas of pigmentation and endocrine dysfunction, with precocious puberty in females. N Engl J Med 1937;216:727-746.
- Megerian CA, Sofferman RA, McKenna MJ, Eavey RD, Nadol JB Jr. Fibrous dysplasia of the temporal bone: ten new cases demonstrating the spectrum of otologic sequelae. Am J Otol 1995;16:408-419.
- Cavazza S, Bocciolini C, Laudadio P, Tassinari G, Dall'Olio D. Two anomalous localizations of mucocele: clinical presentation and retrospective review. Acta Otorhinolaryngol Ital. 2007;27:208-211.
- De Carlo D, Zotto LD, Carollo C, Porzionato A, D'Avella D, Pomerri F, et al. Spontaneous involution of diffuse fibrous dysplasia of paranasal sinuses. J Child Neurol. 2015;30:767-771.