Case Report
Lobular Capillary Hemangioma Presenting as Bleeding Nasal Mass during Pregnancy
Abhijeet Singh1*, Amit Kumar1, Jaimanti Bakshi1 and Gurwinder Kaur2
1Department of Otolaryngology Head and Neck Surgery, Post Graduate Institute of Medical Education and
Research, Chandigarh, India
2Department of Histopathology, Post Graduate Institute of Medical Education and Research, Chandigarh, India
*Corresponding author: Abhijeet Singh, Department of Otolaryngology Head and Neck Surgery, Post Graduate Institute of Medical Education and Research, Chandigarh, India
Published: 30 Aug, 2017
Cite this article as: Singh A, Kumar A, Bakshi J, Kaur
G. Lobular Capillary Hemangioma
Presenting as Bleeding Nasal Mass
during Pregnancy. Ann Clin Case Rep.
2017; 2: 1428.
Abstract
Epistaxis during pregnancy presents a difficult situation and its management can be complex depending on the pregnancy status and severity of symptoms. “Pregnancy Tumor” or “pyogenic granuloma” also called, as Lobular capillary hemangioma (LCH) is a benign, fibrovascular bleeding tumor, which may originate in vascular tissues of skin, muscle, glands, mucosa and bone. These are rapidly growing lesion with extensive endothelial proliferation, of unknown etiology that originate mainly from the nasal septum (65%), lateral nasal wall (18%) and nasal vestibule (16%). Pyogenic granuloma gravidarum (incidence 2% to 5%) may have similar presentation, occurring as small oral or nasal mass, which normally involutes spontaneously after childbirth.
Introduction
We present here a case of pregnant female who presented to us in 2nd trimester with epistaxis and was managed conservatively till the completion of pregnancy and then endoscopic excision was planned electively [1-4].
Case Presentation
A 25-year-old pregnant female (16 weeks) presented to our outpatient department with chief complaints of occasional bleeding from right nasal cavity and right nasal obstruction since last 1 month. The symptoms were insidious in onset and gradually progressive and associated with few episodes of heavy bleed that resolved with conservative treatment and medication not requiring nasal packing. There was no other traumatic or allergic history. The pregnancy was otherwise uneventful and past medical history was unremarkable. She took a medical consultation outside where an anterior rhinoscopy revealed pinkish mass in right nasal cavity and was advised diagnostic nasal endoscopy (DNE) for which she was referred to our center. DNE revealed a reddish polypoidal mass lesion in right nasal cavity with attachments to septum medially, middle turbinate posterosuperiorly and lateral nasal wall infero-laterally (Figure 1). A Magnetic Resonance Imaging (MRI) of nasal cavity and paranasal sinuses was done that revealed T-2WI, STIR hyperintense and T-1WI isointense lobulated soft tissue (26*19*43 mm) in right nasal cavity predominantly located in right middle meatus and extending to inferior meatus obstructing right osteomeatal complex (Figure 2). A provisional diagnosis of an angiomatous polyp was made and a plan for biopsy was deferred. The patient was kept on conservative management (saline nasal drops) and follow-up till completion of pregnancy. The delivery went uneventful without any further episodes of epistaxis. Two months post-delivery patient was planned for endoscopic surgical excision (Figure 3) under general anesthesia. Intraoperative, 4 * 3 centimeter pinkish polypoidal mass lesion filling right middle meatus & nasal cavity and attached medially to septum, laterally lateral nasal wall and superiorly to middle turbinate. All the attachment was cauterized using bipolar cautery and mass was delivered in toto (Figure 4). Post excision the attachments sites were debrided and single merocoel packing was done which was removed after 48 hours. The patient was subsequently discharged on day 3 on oral medications. The histopathological examination report confirmed features of lobular capillary hemangioma (Figure 5) and follow-up nasal endoscopy revealed well healing cavity.
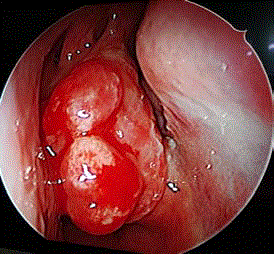
Figure 1
Figure 1
Diagnostic nasal endoscopy showing reddish polypoidal mass
lesion in right nasal cavity with attachments to septum medially, middle
turbinate postero-superiorly and lateral nasal wall infero-laterally.
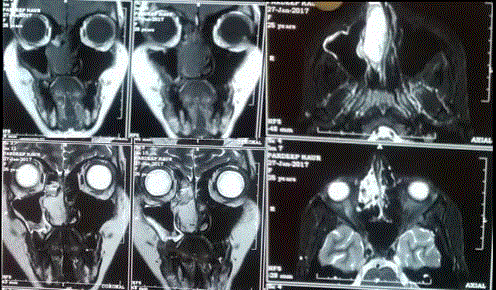
Figure 2
Figure 2
Magnetic resonance images showing T-2WI/STIR hyperintense
and T-1WI isointense lobulated soft tissue in right nasal cavity.
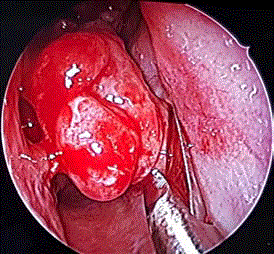
Figure 3
Figure 4
Figure 5
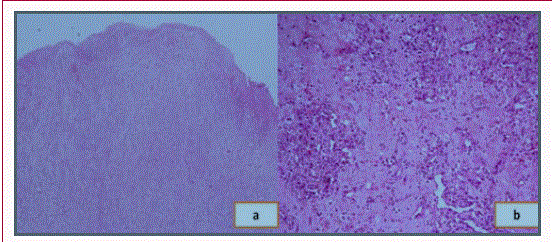
Figure 5
Photomicrograph of the lobular capillary hemangioma showing
a) a polypoidal lesion lined by respiratory lining epithelium with focal
ulceration and squamous metaplasia (Hematoxylin and Eosin; 40x);
b) many lobules of well-formed and uncanalized and abortive capillaries
lined by plump endothelial cells in a fibrocollagenous stroma admixed with
moderate inflammatory infiltrate comprising of lymphocytes and plasma
cells (Hematoxylin and Eosin; 200x).
Discussion
Pyogenic granuloma term was first used in 1904, however it was in 1940 that the first case of
pyogenic granuloma was described [5]. The Term Pyogenic granuloma is a misnomer because the
tumor has well described histological characteristics and is neither pyogenic nor granulomatous.
It was in 1980 when Stacey mills coined the term lobular capillary
hemangioma (LCH) as the tumor mostly presents as skin lesion in
males and mucosal lesion in females having characteristic lobular
arrangement of capillaries in a network of fibrovascular tissue at base
[6]. Other terminologies include pregnancy granuloma, granuloma
gravidarum, granuloma pyogenicum, pregnancy tumor, and
telangiectatic polyp [7].
The disease may present at any age, however the incidence
is greatest in the 3rd decade, with a slight female predominance
mainly during last two trimesters of pregnancy [8]. The clinical
characteristic suggests it being a hormone sensitive inflammatory
overgrowth associated with use of oral contraceptive drugs rather
than true neoplasm. The exact etiology being unknown the other
proposed mechanisms include trauma, viral infection, arterio-venous
malformation and increased production of angiogenic growth factor [7,8].
The increased levels of estrogen and progesterone during
pregnancy cause hypervascularity of the lesion due to increased
endothelial proliferation. Although studies have suggested similar
numbers of estrogen and progesterone receptors in tissue samples
of LCH from male, female or pregnant women, it's the level of
pregnancy associated circulating hormone that is more important
in the pathogenesis [1,4,6]. Nose picking and nasal packing during
pregnancy leads to local irritation that gets exacerbated because
of proinflammatory state, causing rapid increase in size of lesion
(maximum 2 cm) which regresses over months to become a fibroma
[7].
The medical treatment modality includes corticosteroids and
propranolol [9]. The mainstay of treatment, if the lesion is not selfregressed
post-delivery remains surgical excision with desiccation
of base. This decreases chances of recurrence however there have
been upcoming treatment modality in forms of laser therapy and
sclerosing agents.
Conclusion
LCH can be mistaken for malignancy at times and may divert the treatment modality as in young boys and pregnant women. Surgery with or without embolization remains the primary treatment modality if lesion isn’t self-regressing.
References
- Jones JE, Nguyen A, Tabaee A. Pyogenic granuloma (pregnancy tumor) of the nasal cavity. A case report. J Reprod Med. 2000; 45: 749-53.
- Takeda K, Takenaka Y, Hashimoto M. Intraosseous heman- gioma of the inferior turbinate. Case Report Med 2010; 409429.
- Kapella M, Panosetti E, Rombaux P, Delos M, Weynand B. Lobular capillary haemangioma of the nasal cavity: observation of three specific cases. Acta Otorhinolaryngol Belg 2001;55: 241–6
- Choudhary S, MacKinnon CA, Morrissey GP, Tan ST. A case of giant nasal pyogenic granuloma gravidarum. J Craniofac Surg. 2005; 16: 319-321.
- Frank I, Blahd M. Pyogenic granuloma of the nasal fossa. Arch Otolaryngol 1940; 31: 919–924.
- Nichols GE, Gaffey MJ, Mills SE, Weiss LM. Lobular capillary hemangioma. An immunohistochemical study including steroid hormone receptor status. Am J Clin Pathol 1992; 97: 770–775.
- Zarrinneshan AA, Zapanta PE, Wall SJ. Nasal pyogenic granuloma. Otolaryngol Head Neck Surg. 2007; 136: 130-131.
- Puxeddu R, Berlucchi M, Ledda GP, Parodo G, Farina D, Nicolai P. Lobular capillary hemangioma of the nasal cavity: A retrospective study on 40 patients. Am J Rhinol. 2006; 20 :480-484.
- Simic R, Vlahovic A, Subarevic V. Treatment of nasal hemangiomas. Int J Pediatr Otorhinolaryngol. 2009; 73: 1402-1406.