Clinical Image
Severe Desquamation in Kawasaki Disease: Is it Somehow Protective?
Jubran Theeb Alqanatish* and Amir Babiker
Department of Paediatric Rheumatology, King Abdullah Specialized Children’s Hospital, King Abdulaziz Medical
City, National Guard Health Affairs & King Saud Bin Abdulaziz University, Saudi Arabia
*Corresponding author: Jubran Theeb Alqanatish, Department of Paediatric Rheumatology, King Abdullah Specialized Children’s Hospital, King Abdulaziz Medical City, National Guard Health Affairs & King Saud Bin Abdulaziz University, PO Box 22490/MC 1940, Riyadh 11426, Saudi Arabia
Published: 26 Aug, 2017
Cite this article as: Alqanatish JT, Babiker A. Severe
Desquamation in Kawasaki Disease: Is
it Somehow Protective?. Ann Clin Case
Rep. 2017; 2: 1424.
Clinical Image
A previously healthy 12-year-old boy was first treated in the primary care for a possible
pharyngitis because of fever, conjunctivitis and a non-desquamating skin rash. The fever continued
for 10 days then remitted, while other symptoms resolved. Two weeks later, he started to have
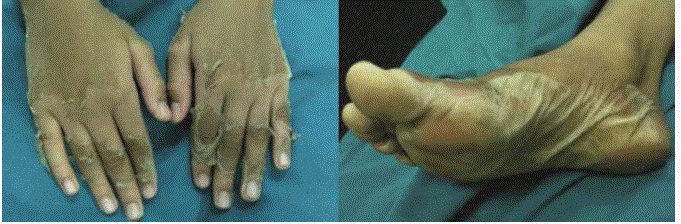
desquamation, which rapidly progressed to a full thickness, over his palms and soles when he
presented to our center (Figure 1). His blood tests revealed: Platelets 804 x 109/L (reference: 150-450
x109 /L), Erythrocyte sedimentation rate (ESR) 61 mm/h (reference: 0-10 mm/h), C-reactive protein
(CRP) 7.09 mg/L (reference: <3.5 mg/L) and Lactate Dehydrogenase (LDH) 281 g/L (reference:
125-220 U/L). Urinalysis, Throat culture, and Anti-streptolysin-O titer were unremarkable. An
echocardiogram was normal. He was started on oral Aspirin 81 mg daily and was followed in clinic
when he developed onycholysis over all fingernails. A repeat blood test in 6 weeks was normal. The
echocardiogram was repeated 3 times and showed no coronary abnormality; hence, Aspirin was
discontinued.
Desquamation is very common in Kawasaki disease (KD). In the original report on KD from
Japan, 49 out of 50 had desquamation and was also above 90% in two different series from the United
States, [1-4]. Although a lower rate was reported in Chinese (83%), [5]. Full-thickness epidermal
peeling is a hallmark of KD and often prompts the diagnosis in missed cases. The sensitivity and
specificity of desquamation in KD is unknown. However, patients who did not peel were more likely
to develop aneurysms interestingly suggesting somehow a protective role of skin peeling [4].
Figure 1
References
- Kawasaki T. [Acute febrile mucocutaneous syndrome with lymphoid involvement with specific desquamation of the fingers and toes in children]. Arerugi. 1967; 16: 178-222.
- Ichida F, Fatica NS, O'Loughlin JE, Klein AA, Snyder MS, Levin AR, et al. Epidemiologic aspects of Kawasaki disease in a Manhattan hospital. Pediatrics. 1989; 84: 235-241.
- Morens DM, Anderson LJ, Hurwitz ES. National surveillance of Kawasaki disease. Pediatrics. 1980; 65: 21-25.
- Wang S, Best BM, Burns JC. Periungual desquamation in patients with Kawasaki disease. Pediatr Infect Dis J. 2009; 28: 538-539.
- Huang GY, Ma XJ, Huang M, Chen SB, Huang MR, Gui YH, et al. Epidemiologic pictures of Kawasaki disease in Shanghai from 1998 through 2002. J Epidemiol. 2006; 16: 9-14.