Case Report
Lingual Actinomycosis, an Uncommon Diagnosis of Tongue Lesions: A Case Report and Review of Literature
Prem Singh Jat, Antony Abraham Paulose and Sunita Agarwal*
Department of ENT, SMS Medical College and Hospital, Jaipur (Rajasthan), India
*Corresponding author: Sunita Agarwal, Department of ENT, SMS Medical College and Hospital, 3/1, Heera Bagh Flats, Sawai Ram Singh Road, Jaipur (Rajasthan), India
Published: 19 Jun, 2017
Cite this article as: Jat PS, Paulose AA, Agarwal S.
Lingual Actinomycosis, an Uncommon
Diagnosis of Tongue Lesions: A Case
Report and Review of Literature. Ann
Clin Case Rep. 2017; 2: 1381.
Abstract
Actinomycosis is a chronic suppurative infection caused by Actinomyces israelii. Actinomycotic infections of the cervicofacial region are the most common sites involved followed by abdominal and thoracic. However, actinomycosis of the tongue is rare. Actinomycetes may become pathologic due to poor oral hygiene, dental/periodontal problems, trauma and following oral surgical procedures. Our report describes a patient with an unusual actinomycotic nodular lesion that was limited to the tongue. Diagnosis was based on histopathological examination. The patient recovered completely after surgical excision, and three weeks of doxycycline.
Keywords: Actinomycosis; Tongue; Cervicofacial
Introduction
Actinomycosis is a chronic suppurative infection mainly caused by Actinomyces israelii, a Gram-positive anaerobic bacterium that is fastidious, a commensal saprophyte often found in the oral mucosa, teeth cavites and the tonsillar crypts, especially in cases of poor oral hygiene, and also in the respiratory and digestive tract. Actinomycetes may become pathologic due to poor oral hygiene, dental/periodontal problems, trauma and following oral surgical procedures. A mass that may mimic both benign and malignant lesions can be seen at clinical presentation and may be misdiagnosed [1,2]. Human actinomycosis was first described in the medical literature in 1857. In 1877, Bollinger and Harz [3] named the genus Actinomyces when they described the etiologic agent of bovine actinomycosis (“lumpy jaw”) and called it Actinomyces bovis [4]. In 1878, Israel discovered granules in human autopsy material and described actinomycosis in humans in 1885 [5,6]. Actinomycosis can rightly be called the "masquerader" of the head and neck as the symptoms are often vague and non-specific. The diagnosis can be delayed until a vital organ becomes eroded or obstructed [7].
Case Presentation
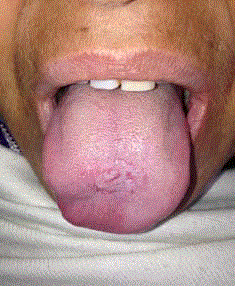
A 44-year-old woman presented to the Department of ENT with complaints of a nodular mass on the dorsum of her tongue without symptoms. The patient was referred to our institute from primary health centre for poor response with oral antibiotics and for suspicion of malignancy. Oral examination revealed an elevated, non-ulcerated and non-tender mass covered with a normal appearing mucosa over the dorsum of tongue adjacent to midline (Figure 1). The patient had poor oral hygiene and dental caries. On clinical examination, a mass was present over the dorsum of tongue measuring 15 mm x 15 mm x 10 mm in diameter, well-demarcated, and firm in consistency. Tongue movements were normal. There was no cervical lymphadenopathy. Patient underwent routine telelaryngoscopy to rule out synchronous lesions. The patient had no history of previous trauma, previous dental procedures or risk of immunodeficiency and was immunocompetent. Under local anaesthesia, excisional biopsy of the mass was done and was subjected to histopathological examination. Histopathological report revealed a granulomatous inflammatory lesion with underlying matted colony of actinomyces and sulphur granules surrounded by large collections of polymorphonuclear leukocytes. The patient was referred for a dental opinion for caries and poor oral hygiene, where the patient was advised dental scaling. Patient was treated with oral doxycycline 100 mg twice a day for a period of three weeks. The patient was instructed to keep a better oral hygiene with 0.2% chlorhexidine gluconate irrigation as per dental opinion for 1 week and was advised to return for follow-ups. The case was followed up for a period three months at regular intervals and no evidence of recurrence was noted.
Figure 1
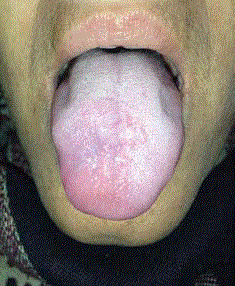
Figure 2
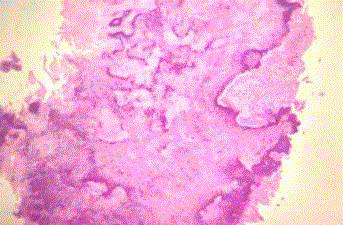
Figure 3
Figure 3
Histopathological section of specimen showing polymorphonuclear
leukocytic infiltration and dark staining bacterial colonies.
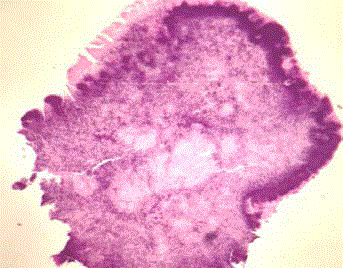
Figure 4
Figure 4
Histopathological section of specimen showing chronic
granulomatous lesion with surrounding polymorphonuclear leukocytes and
dark staining bacterial colonies (arrow) on H & E Stain.
Discussion
Head and neck cancers constitute the commonest cancer in Indian men and third most common cancer in women. The high incidence of head and neck cancer in India is attributed to widespread use of tobacco in multiple forms [8]. In such disease burdened clinical setting, it is essential to come at timely diagnosis of malignancy as well as rule out diseases that mimics malignancy with best utilization of resources. Actinomycosis is known to masquerade as head and neck malignancy [7]. Actinomyces species are ubiquitous and fastidious to cultivate. The species that causes human disease are Actinomyces Israeli, A. gerencseriae, A. turicensis, A. radingae, A. europaeus [9]. Actinomyces is a common oral commensal often found in the oral mucosa, teeth cavites and the tonsillar crypts, especially in cases of poor oral hygiene, and also in the respiratory and digestive tract. Actinomyces may also become pathologic due to trauma, dental and periodontal pathologies, following oral surgical procedures and immunodeficiency [10]. Clinical presentation of the disease is that of a submucosal swelling following a breach in overlying mucosa or epithelium with multiple abscess formation when untreated. Tongue actinomycosis is generally located on the anterior two thirds, lateral to the median sulcus, and presents as a moderately painful nodule and poorly mobile on the adjacent planes [11]. A massive fibrotic reaction surrounding necrotic centre which on palpation feels like a solid swelling is characteristic [12]. Because clinical symptoms are nonspecific, actinomycosis can be misdiagnosed as a tumor. However, the history can guide the clinician to define the lesion’s inflammatory origin and differentiate it from neoplasm [13]. In the present case, there was no history of trauma but the patient had dental caries and poor oral hygiene. A nodular mass over the dorsum of tongue that may mimic both benign and malignant lesions can be seen at clinical presentation and may be misdiagnosed. This could have been due to the inadequate treatment received before being referred to our institute. Surgery plays an important role in diagnosis of Actinomycosis for local control of disease and preventing further tissue destruction. Inadequate short term antibiotic therapy can result in the relapse of infection after apparent cure. To prevent the chance of relapse of the disease, prolonged antibiotic therapy is necessary [14]. High dose penicillin over prolonged duration (6 months to 1 year) is the cornerstone of management of actinomycosis. Penicillin G is the drug of choice for treating infections caused by Actinomycetes. Success with shorter courses of therapy (< 6 mo) has been reported, especially in cervicofacial actinomycosis. Other drugs that are commonly used are doxycycline, clindamycin, amoxicillinclavulanate, ceftriaxone and imipenem/cilastin [15]. Our patient had already taken a course of penicillin and hence oral doxycycline was preferred for better compliance to treatment. Sakallioglu et al [17]. proposed administration of doxycycline for oral Actinomycosis and oral irrigation of 0.2% Chlorhexidine [16,17]. This case report emphasizes the rarity of actinomycosis of the tongue, diagnostic and treatment challenge it poses in a clinical scenario with high incidences with head and neck malignancies and short course treatment of surgical debridement combined with doxycycline and chlorhexidine irrigation over a prolonged parenteral pencillin treatment.
Conclusion
The treatment of choice for cervicofacial actinomycosis, once confirmed is parenteral penicillin for 6 months to 1 year. Actinomycosis due to its rarity and its nature to mimic malignancy are often misdiagnosed and mismanaged by the time a diagnosis is made. Due to the local destructive nature of the actinomycotic infection, early diagnosis should be made especially in the oral cavity to prevent the hazardous spread of the disease. Hence, actinomycosis should be included in the differential diagnosis of neoplasm and chronic granulomatous lesions of tongue. Surgical debridement of the lesion and oral antibiotic course with doxycycline can help in better compliance by decreasing treatment duration of actinomycosis to three weeks.
References
- Atespare A, Keskin G, Erçin C, Keskin S, Camcioglu A. Actinomycosis of the tongue: a diagnostic dilemma. J Laryngol Otol. 2006; 120: 681-683.
- Ficarra G, Di Lollo S, Pierleoni F, Panzoni E. Actinomycosis of the tongue: a diagnostic challenge. Head Neck. 1993; 15: 53-55.
- Richtsmeier WJ, Johns ME. Actinomycosis of the head and neck. CRC Crit Rev Clin Lab Sci. 1979; 11: 175-202.
- Bollinger O. Ueber eine neue Pilzkrankheit beim Rinde. Zentralblatt Medizinische Wissenschaft. 1877; 15: 481–90.
- Israel J. Neue Beobachtungen auf dem Gebiete der Mykosen des Menschen. Archiv Pathologische Anatomie. 1878; 74: 15–53.
- Wolff M, Israel J. Ueber Reincultur des Actinomyces und seine Uebertragbarkeit auf Thiere. Archiv f. pathol Anat. 1891; 126: 11–59.
- Rankow RM, Abraham DM. Actinomycosis: masquerader in the head and neck. Ann Otol Rhinol Laryngol. 1978; 87: 230-237.
- Asthana S, Patil RS, Labani S. Tobacco-related cancers in India: A review of incidence reported from population- based cancer registries. Indian J Med Pediaric Oncol. 2016; 37: 152-157.
- Pulverer G, Schutt-Gerowitt H, Schall KP. Human cervicofacial Actinomycoses: microbiological data for 1997 cases. Clin Infect Dis. 2003; 37: 490-497.
- Habibi A, Salehinejad J, Saghafi S, Mellati E, Habibi M. Actinomycosis of the tongue. Arch Iran Med. 2008; 11: 566-568.
- Gerbino G, Bernardi M, Secco F, Sapino A, Pacchioni D. [Actinomycosis of the tongue. Report of two cases and review of the literature]. Minerva Stomatol. 1998; 47: 95-101.
- Palonta F, Preti G, Vione N, Cavalot AL. Actinomycosis of the masseter muscle: report of a case and review of the literature. J Craniofac Surg. 2003; 14: 915-918.
- Ngow HA, Wan Khairina WM. Cutaneous actinomycosis: the great mimicker. J Clin Pathol. 2009; 62: 766.
- Ellis IE, Hupp JR, Tucker MR. Contemporary Oral and Maxillofacial Surgery. St. Louis: Mosby. 1998.
- Sudhakar SS, Ross JJ. Short-term treatment of actinomycosis: two cases and a review. Clin Infect Dis. 2004; 38: 444-447.
- Bennhoff DF. Actinomycosis: diagnostic and therapeutic considerations and a review of 32 cases. Laryngoscope. 1984; 94: 1198-1217.
- Sakallioğlu U, Açikgöz G, Kirtiloğlu T, Karagöz F. Rare lesions of the oral cavity: case report of an actinomycotic lesion limited to the gingiva. J Oral Sci. 2003; 45: 39-42.