Case Report
Large Biopsy-Related Renal Allograft Pseudoaneurym: Evident Sonographically but Indistinct Angiographically
Ilario C, Sentissi O* and Coste C
Department of Mental Health and Psychiatry, University Hospital of Geneva, Switzerland
*Corresponding author: Othman Sentissi, Department of Mental Health and Psychiatry, University Hospital of Geneva, Clinic Belle Idée: Chemin du Petit-Bel-Air 2, 1225 Chêne-Bourg, Switzerland
Published: 09 Jun, 2017
Cite this article as: Ilario C, Sentissi O, Coste C.
Neuroleptic Malignant Syndrome
without Hyperthermia Induced by
Aripiprazole Extended-Release
Injection. Ann Clin Case Rep. 2017; 2:
1372.
Abstract
Neuroleptic malignant syndrome may be considered an idiosyncratic neurological condition with potentially lethal consequences associated with the assumption of all antipsychotics, first described in the early sixties in association with the antipsychotic haloperidol. Recently, several cases of the syndrome have been reported in literature as a complication of typical and atypical antipsychotic drugs. Moreover, a widespread use of antipsychotics in numerous neuropsychiatric disorders has lead to the analysis of the risks and consequences of neuroleptic malignant syndromes. This case report describes the occurrence of a neuroleptic malignant syndrome in a 55-year-old woman with intellectual disability presenting with organic delusional disorder, following administration of aripiprazole extended-release injection. Although cases of neuroleptic malignant syndrome induced by aripiprazole or by atypical antipsychotics extended-release have been published in literature, this is the first case report regarding a neuroleptic malignant syndrome induced by aripiprazole extended-release injection.
Keywords: Neuroleptic malignant syndrome (NMS); Aripiprazole extended-release injection; Antipsychotic drugs
Introduction
Neuroleptic Malignant Syndrome (NMS) is a rare, idiosyncratic and unpredictable adverse
reaction associated to antipsychotic use with life-threatening [1] consequences. All antipsychotics may be associated with the development of a neuroleptic malignant syndrome, especially the first
generation antipsychotics (Table 1). The incidence rate of NMS in subjects treated with antipsychotic drugs is actually approximately 0.02%, compared to a rate of 3% recorded 50 years ago [2]. The syndrome occurs in all age groups (including children), but young adults are more affected [3], and the male/female ratio is 2:1 with a high mortality rate in 10-20% of cases. However, lower mortality rates have recently been observed most probably related to early detection of NMS and improved
management [2]. The key risk factors for neuroleptic malignant syndrome are demographic
(male gender), environmental (restraint, dehydration) and pharmacological (polypharmacy, oral
haloperidol, aripiprazole, long-acting flupentixol), because of their pharmacodynamics mechanism.
Concurrent medical conditions are also relevant (delirium, confusion) [4]. Authors reported a correlation between a higher proportion of antipsychotics, the pharmacokinetic properties and the
severity of the syndrome [5].
The pathogenesis is still unknown [1], but investigations have revealed involvement of two
main mechanisms: an abnormal reaction of skeletal muscle with a central D2 receptor blockade [6] and the removal of tonic inhibition from the sympathetic nervous system, with sympathoadrenal
hyperactivity and dysfunction leading to autonomic dysfunction [7]. The clinical features are often heterogeneous in onset, presentation and progression. Most patients develop mental status change
with delusion, mutism and catatonia, then muscular lead pipe rigidity with tremor, hyperthermia
(above 38°C) and autonomic instability [1,8]. Leukocytosis and Creatine Kinase (CK) elevation are commonly observed. The largest systematic review of literature comparing the characteristics
and differences of the neuroleptic malignant syndrome induced by first and second generation
antipsychotic has reported a lower incidence and severity of symptoms with second-generation
antipsychotics with fewer extrapyramidal symptoms and less rigidity [8].
In neuroleptic malignant syndrome subsequent to administration of aripiprazole, rigidity and
autonomic symptoms are present in all cases reported [9], with a lower frequency of hyperthermia, diaphoresis and tachypnea than in neuroleptic malignant syndromes induced by other secondgeneration
antipsychotics [1]. However, literature reports three cases of neuroleptic malignant syndrome induced by aripiprazole in which pyrexia was absent [10-12]. On average, neuroleptic malignant syndrome develops 14 days
following the initial administration of aripiprazole with a mean
prescribed dosage of 5 to 30 mg/day [9], in some clinical illustrations,
in association with other psychotropic drugs, such as selective
serotonin reuptake inhibitors (fluoxetine and escitalopram) [9].
Selective serotonin reuptake inhibitors (SSRIs) may contribute to the
development of neuroleptic malignant syndrome with an increase in
serotonin which inhibits dopamine release in the ventral tegmentum
area and the substantia nigra [13] and thereby may worsen a
hypodopaminergic state induced by antipsychotics. NMS has been
reported also in association with escitalopram and citalopram,
antidepressants that are not known to inhibit the cytochrome P450
system (the Cyt P450 system is not relevant for NMS-development)
[13,14]. Twenty-nine cases of neuroleptic malignant syndrome in
association with a second-generation antipsychotic and serotonergic
antidepressants have been published in literature, but only one
case involved oral aripripazole and escitalopram, with symptoms
appearing after one week of treatment [13,15]. The different types
and presentations of NMS could be explained by: different risk
factors in populations; possible association of NMS with other lethal
syndromes; incidence of NMS in patients treated by neuroleptic
agents, which is still unclear (from 0.7% to 2.2%) [6].
In our knowledge, this is the first case report concerning a
neuroleptic malignant syndrome induced by aripiprazole extendedrelease
injection, medication, which is increasingly being prescribed
by clinicians.
Case Presentation
Mrs F, a 55-year-old Caucasian single woman presented a medical
history of intellectual disability caused by traumatic brain injury
at the age of 17, and organic delusional disorder with supposedly
related temporal lobe epilepsy. She was monitored in outpatient
psychiatric basis and received treatment with quetiapine 300 mg
twice daily, lorazepam 1 mg three times daily and amlodipine 5 mg
daily. However, the patient experienced an episode of aggressiveness consistent with delusional phenomena and recurrences due to poor treatment compliance. She was admitted to our psychiatric
crisis unit for the fourth time in 2016, accompanied by her mother
following an acute exacerbation of auto and hetero-aggressiveness
and delirious speech. In a patient with organic encephalopathy, using
atypical antipsychotics is “off-label”, but in this clinical situation of
chronic psychosis and behaviour disorder such as aggressiveness, this
treatment remains one of the few options available. On admission,
Mrs F presented an abrupt change from baseline mental status
with severe anxiety and inappropriate affect. On examination, no
abnormalities were detected. Urine and blood tests were within
normal limits. Following consultation with the patient and her family,
we decided to switch to aripiprazole extended-release injection (400
mg), in favour of its adequate safety profile, few metabolic side effects
and its powerful/ solid anti-impulsive and antipsychotic effects.
Subsequently, we prescribed oral aripiprazole 15 mg/day with a
reduction of quetiapine at 300 mg/day for a week, then discontinued.
The first injection of aripiprazole extended-release (400 mg) was
administered fourteen days after oral administration (Figure 1).
No side effects were observed. The level of aripripazole the day
after the injection was at 507 nmol/l (330-1115 nmol/l), and active
metabolite (dehydroaripiprazole) at 287 nmol/l. Ten days after the
treatment, the level of aripiprazole was at 332 nmol/l and the level of
dehydroaripiprazole at 225 nmol/l. Eight day after the injection, the
patient experienced mood worsening with feelings of worthlessness
and escitalopram 5 mg/day was introduced. Eleven days after the first
injection of aripiprazole extended-release, the patient complained of
muscular rigidity and intermittent mutism. The examination showed
a mild rigidity, slight decrease in deep tendon reflexes with walking
abnormalities and asymmetric upper limb tremor. The hematologic
parameters and ionogram were within normal limits. The day after, the
patient was transferred to the emergency department with suspected
neuroleptic malignant syndrome due to a sudden deterioration of the
clinical symptoms (dilated pupils, heavy sweating and diarrhea were
absent). The patient was aggressive and presented fluctuating level of
conscientiousness, limbs and axial extrapyramidal symptoms (such as severe rigidity, hypokinesia, dysphagia and asymmetric upper limb tremor), poverty of speech, intermittent mutism. Mild hyperreflexia,
no dystonia and no posturing. Mrs F’s temperature was 37.5°C, blood
pressure 155/93 mmHg, pulse 106 beats per minute, respiratory rate
20 per minute (baseline for the subject: 140/80 mmHg, 70 beats per
minute). Laboratory data showed leukocytosis (13,000 cells/mm3),
increased creatine phosphokinase (CK: 8,511 IU/L) and acute renal
failure (serum creatinine: 89 μmol/L; glomerular filtration flow:
63 mL/min/1.73m²), other blood test values, complete metabolic
panel and ionogram levels were all within normal limits. Immediate
electroencephalographic (EEG) examination showed global slow
activity without argument for comitiality or metabolic disorder. The
magnetic resonance imaging showed damage to the left temporal lobe
caused by brain injury (at the age of 17).
On Sachdev rating scale for NMS [16], Mrs F’s rating is 16 on
36. When NMS is suspected, a score superior to 8 is in favour of the
diagnosis. On Naranjo Scale, Mrs F’s rating is 9 on 13, a score superior
to 9 is in favour of the diagnosis of adverse drug reaction.
Some drugs, like bromocriptine mesylate (a dopamine agonist),
could be used to treat NMS. However, the supportive and symptomatic
therapy is the most common treatment, because the safety of other
therapies is still unclear. So, the supportive treatement was started.
Oral aripiprazole and escitalopram were discontinued abruptly
(the most important intervention), lorazepam 0.5 mg 4 times a day
was administred with nursing care, close clinical and paraclinical
monitoring. The patient overall showed slow but progressive
improvement in motor and cognitive functions. However, during the
two months of treatment in a somatic unit, she developed a number
of complications: acute renal failure due to rhabdomyolysis for which
a intravenous hydratation has been helpful; acute urinary retention
that required the instalment of a probe; acute aspiration pneumonia
due to swallowing impairment, treated with clindamycin (injection
600 mg 1x/8h, 1800 mg daily). The patient recovered gradually
and benefit from progressive administration of clozapine, before
returning to our unit. After four months of inpatient care, Mrs F
finally went back home.
Figure 1
Figure 1
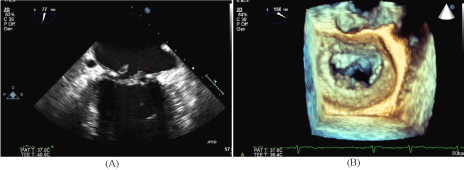
Trans-esophageal echocardiogram following stroke.
(A) 2-chamber view of the mitral valve in systole with vegetations attached to
the mitral annuloplasty ring.
(B) 3D TEE image of the mitral valve in diastole with multiple small vegetations
attached to the mitral annuloplasty ring.
Table 1
Discussion
We report a case of a patient with neuroleptic malignant syndrome
induced by Aripiprazole Extended-Release Injection. We carried out
an exhaustive literature review and we found eighteen published
case reports with similar characteristics following administration of
aripiprazole [1,9-12] (Table 1), not related to an “off-label” use.
In this clinical situation, rigidity and autonomic characteristics
were observed, in line with all cases of neuroleptic malignant
syndrome caused by aripiprazole reported. These symptoms are more
common compared to cases of patients using clozapine, olanzapine
and quetiapine [9]. Furthermore, other extrapyramidal signs detected
in our patient such as tremor and hypokinesia, are predominantly
related to aripiprazole compared to both traditional [17] and atypical
antipsychotic drugs [9].
The atypical clinical presentation of NMS following aripiprazole
administration could be related to its peculiar pharmacodynamic
profile [1]. In fact, aripiprazole possesses a partial agonist activity
at D2 and 5-HT1A receptors and antagonistic activity at 5-HT2A
receptors, with an affinity 20-fold lower than haloperidol affinity
for D2 [10]. This unique characteristic may be related to the lower
severity rate and duration in contrast to neuroleptic malignant
syndrome induced by other atypical antipsychotics.
Neuroleptic malignant syndrome may be deceptive in
presentation. The most important differential diagnosis is serotonin
syndrome, which can have similitudes in clinical presentation [2].
Hyperthermia, tremor and alteration of mental status can occur in
both, but muscular rigidity, hypertonia and bradykinesia are specific
in NMS. Moreover, symptoms are progressive in NMS whereas in
serotonin syndrome they develop faster. In some cases an overlap of
neuroleptic malignant syndrome and serotonin syndrome may occur
[18].
In this case, the progressive installation of extrapyramidal
symptoms (tremor, hypokinesia and severe rigidity), mutism and
dysphagia associated with CPK elevation and leucocytosis is in favour
of a NMS. However in our case report a typical feature of serotonin syndrome, hyperreflexia, was present on diagnosis, most likely related to the use of therapeutic doses of escitalopram.
Neuroleptic malignant syndrome is a life-threatening neurologic
emergency, and the risk of a recurrent episode after restarting on
neuroleptic agents is relatively high but difficult to quantify. An
apparent decrease in severity is, however, suggested by the lower
mortality rate reported in the last decade [10]. This may relate to
early detection of neuroleptic malignant syndrome as well as to
improvements in management of the condition or lower severity
with atypical antipsychotics [6]. Subsequent to neuroleptic malignant
syndrome, over 30% of patients develop major complications during
the first weeks, together with potential persistent long-term sequelae
[19]. Considering the impact of genetic polymorphisms on the
elimination of aripiprazole, a genotype / phenotype test of CYP2D6
may also be proposed. Allelic variants altering CYP2D6-mediated
metabolism may be associated with an increased risk of NMS [13].
Case reports of neuroleptic malignant syndrome induced by
aripiprazole or by second-generation antipsychotics extended-release
have been published in literature, but we report herein the first case of
a neuroleptic malignant syndrome induced by a different formulation
of aripiprazole, the extended-release injection never been described
in the literature. In conclusion, this original case report may be
considered important contribution for clinicians in their daily practice
in order to appropriately investigate and address to the serious side
effects of extended-release injection of aripiprazole, causing a more
prolonged course of NMS. The atypical clinical presentation of
NMS following aripiprazole administration could be related to its
peculiar pharmacodynamic profile, which represents a modern and
innovative therapeutic tool in the treatment of major psychiatric
disorders [20]. However, this case report cannot give information on
incidences or prevalence and further research is required to increase
our knowledge of the consequences and efficacy of treatments and to
better understand neuroleptic malignant syndrome, especially in the
extended release formulation.
Acknowledgments
We would like to thank Mrs Giuseppina Caraglia for the English editing.
References
- Belvederi Murri M, Guaglianone A, Bugliani M, Calcagno P, Respino M, Serafini G, et al. Second-generation antipsychotics and neuroleptic malignant syndrome: systematic review and case report analysis. Drugs R D. 2015; 15: 45-62.
- Strawn JR, Keck PE Jr, Caroff SN. Neuroleptic malignant syndrome. Am J Psychiatry. 2007; 164: 870-876.
- Sarkar P, Natarajan C, Gode N. Prevalence of neuroleptic malignant syndrome in 672 consecutive male in-patients. Indian J Psychiatry. 2009; 51: 202-225.
- Su YP, Chang CK, Hayes RD, Harrison S, Lee W, Broadbent M, et al. Retrospective chart review on exposure to psychotropic medications associated with neuroleptic malignant syndrome. Acta Psychiatr Scand. 2014; 130: 52-60.
- Tse L, Barr AM, Scarapicchia V, Vila-Rodriguez F. Neuroleptic Malignant Syndrome: A Review from a Clinically Oriented Perspective. Curr Neuropharmacol. 2015; 13: 395-406.
- Adnet P, Lestavel P, Krivosic-Horber R. Neuroleptic malignant syndrome. Br J Anaesth. 2000; 85: 129-135.
- Gurrera RJ, Caroff SN, Cohen A, Carroll BT, DeRoos F, Francis A, et al. An international consensus study of neuroleptic malignant syndrome diagnostic criteria using the Delphi method. J Clin Psychiatry. 2011; 72: 1222-1228.
- Trollor JN, Chen X, Chitty K, Sachdev PS. Comparison of neuroleptic malignant syndrome induced by first- and second-generation antipsychotics. Br J Psychiatry. 2012; 201: 52-56.
- Trollor JN, Chen X, Sachdev PS. Neuroleptic malignant syndrome associated with atypical antipsychotic drugs. CNS Drugs. 2009; 23: 477-492.
- Molina D, Tingle LE, Lu X. Aripiprazole as the causative agent of neuroleptic malignant syndrome: a case report. Prim Care Companion J Clin Psychiatry. 2007; 9: 148-150.
- Chakraborty N, Johnston T. Aripiprazole and neuroleptic malignant syndrome. Int Clin Psychopharmacol. 2004; 19: 351-353.
- Spalding S, Alessi NE, Radwan K. Aripiprazole and atypical neuroleptic malignant syndrome. J Am Acad Child Adolesc Psychiatry. 2004; 43: 1457-1458.
- Stevens DL. Association between selective serotonin-reuptake inhibitors, second-generation antipsychotics, and neuroleptic malignant syndrome. Ann Pharmacother. 2008; 42: 1290-1297.
- Tanaka E. Clinically significant pharmacokinetic drug interactions with benzodiazepines. J Clin Pharm Ther. 1999; 24: 347-355.
- Rodriguez OP, Dowell MS. A case report of neuroleptic malignant syndrome without fever in a patient given aripiprazole. J Okla State Med Assoc. 2006; 99: 435-438.
- Sachdev PS. A rating scale for neuroleptic malignant syndrome. Psychiatry Res. 2005; 135: 249-256.
- Addonizio G, Susman VL, Roth SD. Neuroleptic malignant syndrome: review and analysis of 115 cases. Biol Psychiatry. 1987; 22: 1004-1020.
- Mazhar F, Akram S, Haider N, Ahmed R. Overlapping of Serotonin Syndrome with Neuroleptic Malignant Syndrome due to Linezolid-Fluoxetine and Olanzapine-Metoclopramide Interactions: A Case Report of Two Serious Adverse Drug Effects Caused by Medication Reconciliation Failure on Hospital Admission. Case Rep Med. 2016; 2016: 7128909.
- Adityanjee, Sajatovic M, Munshi KR. Neuropsychiatric sequelae of neuroleptic malignant syndrome. Clin Neuropharmacol. 2005; 28: 197-204.
- Gründer G, Kungel M, Ebrecht M, Göröcs T, Modell S. Aripiprazole: pharmacodynamics of a dopamine partial agonist for the treatment of schizophrenia. Pharmacopsychiatry. 2006; 39 Suppl 1:S21-S25.