Case Report
Delayed Tracheal Perforation after Hemithyroidectomy
Melina Benson, Vaninder Dhillon and Ralph Tufano*
Department of Otolaryngology and Head and Neck Surgery, The Johns Hopkins University, Maryland, USA
*Corresponding author: Ralph Tufano, Department of Otolaryngology and Head and Neck Surgery, The Johns Hopkins University, Maryland, 601 North Caroline St, 6th Floor, Baltimore, MD 21287, USA
Published: 06 May, 2017
Cite this article as: Benson M, Dhillon V, Tufano R. Delayed Tracheal Perforation after Hemithyroidectomy. Ann Clin Case Rep. 2017; 2: 1355.
Abstract
Background: Hemithyroidectomy is a low-risk, outpatient procedure commonly performed for benign and some small, differentiated thyroid malignancies. Delayed tracheal perforation is
exceedingly rare and has previously only been reported after total thyroidectomy.
Case Report: We describe a 25-year-old patient who underwent an unremarkable right
hemithyroidectomy to remove a 4 centimeter FNAB cytologically indeterminate thyroid nodule,
who presented four weeks later with acute anterior neck swelling and subcutaneous emphysema
after strenuous exercise. Computed tomography showed pockets of air tracking along a right lateral
tracheal wall irregularity on the operative side. Flexible tracheobronchoscopy identified a pinholesized
defect. A bedside neck evacuation of the air was performed with drain placement. The patient
was restricted to limited activity for 4 weeks.
Results: The patient recovered uneventfully.
Conclusion: Surgeons who perform thyroid surgery must be aware of the possibility of delayed
tracheal perforation after hemithyroidectomy. Conservative management may be appropriate for
the stable patient.
Keywords: Endocrine; Thyroid cancer; Hemithyroidectomy; Late complication; Tracheal injury
Case Presentation
A 25-year-old man presented with a 4 cm right thyroid nodule. Fine needle aspiration was
consistent with atypia of undetermined significance and molecular testing positive for NRAS
mutation. The left thyroid lobe was unremarkable on ultrasound. An uncomplicated right thyroid
lobectomy and is thmusectomy were performed under general endotracheal anesthesia, with a
6 NIMS Trivantage endotracheal tube for recurrent laryngeal nerve monitoring. Valsalva was
performed, without air escape, and no intra-operative tracheal injury was identified to visual
inspection. Estimated blood loss was minimal. The patient was discharged on the day of surgery.
Pathology returned a 30 gm thyroid lobe with a 4 centimeter papillary carcinoma, classical variant,
as well as an 8 mm papillary thyroid microcarcinoma. Post-operative instructions included no
lifting over 10 pounds for two weeks.
The patient was seen in clinic on post-operative day 21 for routine follow up. At that time, the
patient’s incision was healing well and there was no crepitus or peri-incisional swelling on exam.
The patient did not complain of swelling upon Valsalva, and voice, swallow and breathing were
normal. The patient reported compliance with the activity restrictions, and was advised to ease back
into activity as tolerated.
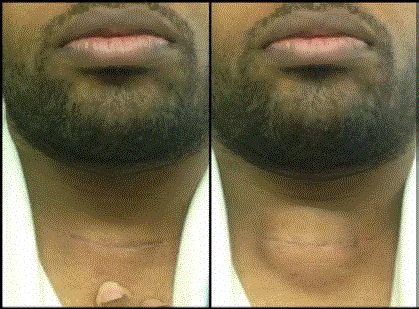
On post-operative day 27, the patient reported a golf-ball sized collection beneath his incision
that occurred immediately after performing pull-ups. He was otherwise asymptomatic. The patient
observed that the collection diminished in size over time but re-accumulated to its original size
each time he bore down (Figure 1). He was evaluated at an outside hospital emergency department, where he was determined to be stable and discharged.
He was seen inclinic on post-operative day 29, where needle aspiration of the 4 centimeter by
4 centimeter ballotable pocket did not yield air or fluid. A pressure dressing was placed on his
anterior neck with instructions to apply manual pressure to the area with cough or strain, and he
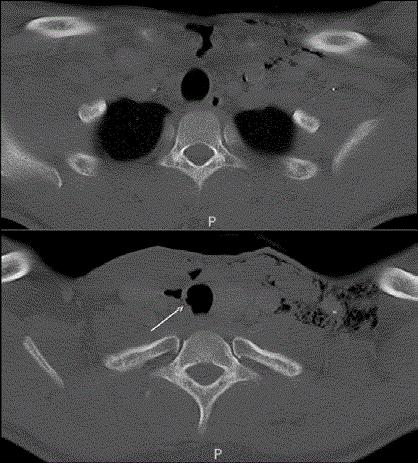
was admitted to the hospital. A computed tomography neck with intravenous contrast was obtained
revealing extensive subcutaneous air tracking to the surgical bed, with irregularity of the right lateral
trachea at the level of the first and second tracheal ring (Figure 2).
A bedside laryngobronchoscopy after trans-tracheal injection of 4% lidocaine topical anesthestic
was performed which identified a 1 millimeter mucosal irregularity along the lateral right tracheal wall below the cricoid, with overlying scant granulation tissue that
was not obstructive. Bedside neck exploration was then performed
for evacuation of the air pocket, with successful air egress. A penrose
drain was placed beneath the strap muscles at the level of the tracheal
injury. The skin site was closed, and an overlying pressure dressing
applied. His crepitus resolved by the following hospital day, and he
was discharged to home with instructions for minimal activity for
four weeks. The patient was seen in clinic four days after discharge for
drain removal and wound closure. He has since had no recurrence of
crepitus or subcutaneous air.
Figure 1
Figure 2
Figure 2
Axial computed tomography revealing subcutaneous air pocket
tracking to the right thyroid lobectomy surgical bed (top), and right lateral
tracheal irregularity closely associated with collection of air in the soft tissues
(bottom). Subcutaneous air is also noted in the left neck.
Discussion
Hemithyroidectomy is a safe procedure performed for
benign as well as some small, differentiated thyroid malignancies.
Complication rates from hemithyroidectomy are lower than that of
total thyroidectomy, and include hypocalcemia (7.1%), hematoma
(1.24%), respiratory complications (0.84%), vocal cord paralysis
(0.59%), and bleeding (0.15%) [1]. Tracheal injury during total
thyroidectomy is rare. A 2005 review of 11,917 thyroidectomies
reported 2 cases of tracheal perforation identified intra-operatively
during partial thyroidectomy (0.02%). Existing literature identifies
trends in cases of tracheal injury in thyroidectomy. Most injuries
are noted intra-operatively, occur posterolaterally in the relatively
less vascular region of the ligament of Berry, and generally follow
suture ligation of vessels or use of diathermy to dissect the thyroid
off of the trachea. These are generally repaired at the time of
injury with little morbidity [2]. Delayed tracheal perforation has
previously only been reported after total thyroidectomy. We have
identified seven previous cases of delayed tracheal perforation after
total thyroidectomies without neck dissection, all presenting with
subcutaneous emphysema [3-9]. The range of post-operative day
of presentation is 4-21 days, with a mean of 11 days. Two previous
reported injuries were managed conservatively with success [4,6]. The
remainder of delayed perforations described were surgically explored
and closed primarily with absorbable suture or with muscle flaps.
Rotational muscle flaps were used in three cases, to close two larger
lacerations, and one rupture complicated by infection, respectively.
One of these repairs included circumferential tracheal resection and
primary anastomosis to repair tracheal necrosis involving multiple
tracheal rings [7].
Previous reports have attributed delayed injury in total
thyroidectomy to bilateral devascularization of the trachea causing
necrosis. The trachea is supplied by lateral pedicles drawing vessels from the inferior thyroid, subclavian, supreme intercostal, internal
thoracic, innominate and superior and middle bronchial arteries.
These longitudinal anastomoses arborize with the contralateral
side via transverse vessels that course in the soft tissue between the
cartilages [10]. In partial thyroidectomy, perhaps injury is less likely
because of the contralateral blood supply, and because the remaining
lobe of the gland confers protection to the tracheal tissue during
diathermy.
The case presented here is the first reported delayed tracheal injury
following partial thyroidectomy. In the opinion of the surgeons, the
injury appeared on bedside tracheobronchoscopy to be secondary to
thermal energy transmitted by bipolar cautery. The tracheal mucosal
lesion was located in the less vascular region of Berry’s ligament. It
is possible that the transverse vessels were cauterized, or the area
of injury was water shed. In our case, devascularization with or
without direct thermal injury most likely weakened an area in the
fibrocartilaginous tracheal wall, making it susceptible to yielding to
air pressure during episodes of increased intra-thoracic pressure.
Additional potential contributing factors in this case include
the etiology of the thyroid disease, as total lobe resection is more
important for clear margins in an operation to extirpate a possible
cancer. In addition, the patient underwent is thmusectomy as well,
adding to the amount of dissection necessary for operative success.
Finally, the patient was a young, healthy male who returned to his
intensive workout regimen at the end of the two week activity
restriction period that our institution implements, leading to the acute
elevations of intra-thoracic pressure that unmasked the weakness in
the tracheal wall.
Strict activity restrictions are of paramount importance in the
post-operative period. Restrictions include lifting no more than 10
pounds, abstaining from strenuous activity, and returning to the
preoperative level of activity slowly by adding activities of daily living
back over the course of two weeks. Delayed injury from coughing and
sneezing are reported in the total thyroidectomy literature; here, the intra-thoracic pressure resulted from a pull-up. Our case occurred
27 days post-operatively. However, given the rarity of this event and
the median post-operative day of subcutaneous emphysema in total
thyroidectomy cases of 11, we do not plan on changing our postoperative
activity restrictions.
Management of delayed tracheal perforation depends largely on
the stability of the patient presenting with subcutaneous emphysema.
Large pneumothorax, cardiorespiratory distress, enlarging
subcutaneous air, and tracheal deviation are among indications for
urgent surgical exploration. In the patient with a stable air pocket
without acute distress, however, conservative management is a
reasonable option without the added morbidity of an emergent neck
exploration under general anesthesia. Two previous reported cases
cite conservative management of pretracheal swelling and imagingconfirmed
subcutaneous air without any intervention. We elected to
open the incision bedside, insert a penrose to achieve complete air
egress and place a compressive dressing with one inpatient night of
monitoring. Our patient had no re-accumulation of air after drain and
dressing removal, suggesting that conservative therapy is appropriate
in select patients.
Surgeons who perform thyroidectomies should be aware of
the possibility of delayed tracheal perforation even one month
post-operatively. Contributing factors include use of diathermy,
and episodes of increased intra-thoracic pressure. Care should be
taken when using diathermy to dissect the thyroid off the trachea,
especially in the less vascular region of the ligament of Berry. Activity
restrictions and monitoring for postoperative peri-incisional swelling
with a high index of suspicion for tracheal violation are paramount.
Conservative therapy may be appropriate for the stable patient.
References
- Hauch A, Al-Qurayshi Z, Randolph G, Kandil E. Total Thyroidectomy is Associated with Increased Risk of Complications for Low- and High-Volume Surgeons. Ann Surg Oncol. 2014;21:3844-52.
- Gosnell JE, Campbell P, Sidhu S, Sywak M, Reeve TS, Delbridge LW. Inadvertent tracheal perforation during thyroidectomy. Brit J Surg. 2006;93:55-6.
- Bertolaccini L, Lauro C, Priotto R, Terzi A. It sometimes happens: Late tracheal rupture after total thyroidectomy. Interact Cardiovasc Thorac Surg. 2012;14(4):500-1.
- Conzo G, Fiorelli A, Palazzo A, Stanzione F, Pietra C Della, Santini M. An unpredicted case of tracheal necrosis following thyroidectomy. Ann Ital Chir. 2012;83(1):55-8.
- Damrose EJ, Damrose JF. Delayed tracheal rupture following thyroidectomy. Auris Nasus Larynx. 2009;36(1):113-5.
- Davies P, Alhamarneh O, Campbel J. Conservative Treatment of Delayed Tracheal Perforation Following Thyroidectomy. Case Rep. 2013;6(2):119-21.
- Jacqmin S, Lentschener C, Demirev M, Gueroult S, Herman P, Ozier Y. Postoperative necrosis of the anterior part of the cervical trachea following thyroidectomy. J Anesth. 2005;19(4):347-8.
- Mazeh H, Suwanabol PA, Schneider DF, Sippel RS. Late manifestation of tracheal rupture after thyroidectomy: case report and literature review. Endocrine practice? Official journal of the American College of Endocrinology and the American Association of Clinical Endocrinologists. 2012;18(4):e73-6.
- Sanna S, Monteverde M, Taurchini M, Mengozzi M, Genestreti G, Grossi W, et al. It could suddenly happen: delayed rupture of the trachea after total thyroidectomy: A case report. G Chir. 2014;35(3-4):65–8.
- Salassa JR, Pearson BW, Payne WS. Gross and microscopical blood supply of the trachea. Ann Thorac Surg. 1977;24(2):100-7.