Case Report
Capillary and Cavernous Hemangiomas of the Maxilla: Case Report of Two Patients and A Review of the Literature
Parveen A Lone1, Tahir Ahmad2*, Sandeep Kaur3, Farhat Raza4
1Professor and Head Department of Oral and Maxillofacial Surgery, Indira Gandhi Government Dental College and Hospital Jammu, India
2House Surgeon, Department of Oral and Maxillofacial Surgery Indira Gandhi Government Dental College Jammu, India
3Registrar, Indira Gandhi Government Dental College Jammu
4Post Graduate Scholar, Himachal Dental College, Sundarnagar, India
*Corresponding author: Tahir Ahmad, Department of Oral and Maxilo Facial Surgery, Indira Gandhi Government Dental College, Jammu -180001, India
Published: 27 Mar, 2017
Cite this article as: Lone PA, Ahmad T, Kaur S, Raza F.
Capillary and Cavernous Hemangiomas
of the Maxilla: Case Report of Two
Patients and A Review of the Literature.
Ann Clin Case Rep. 2017; 2: 1316.
Abstract
Hemangiomas are the most common benign vascular lesions of the head and neck region. However, their occurrence in the oral cavity is relatively rare, especially in oral soft tissue. Hemangiomas are endothelial cell proliferations, followed by gradual involution tumors with unique biologic characteristics that they grow rapidly regress slowly and have very less recurrence. This case report present a case of central hemangioma in a female patient in the maxillary canine-premolar region of unusual size, which is uncommon and a case of cavernous hemangioma in buccal and palatal area of male patient. Even though the lesion has benign growth yet,detailed description, clinical and histopathological features along with new treatment modalities are hugely important for a dental profession.
Introduction
The term hemangioma has traditionally been used to describe a variety of developmental
vascular anomalies. Hemangiomas are benign, enlarged, vascular hamartomas that may be seen in
any soft tissue or bony intra-oral location. They occur early in life and somewhat more commonly in
women than in men [1,2]. Soft tissue hemangiomas occur commonly in the dorsum of the tongue,
gingiva and buccal mucosa. Vascular lesions of the face are not very common. These lesions are a
perplexing group of problems that over the years have generated a significant debate and confusion
as regards their terminology and classification. Descriptive anatomic, pathologic and embriologic
classification scheme have been devised however generally have not offered the clinician significant
guidance for treatment. The classification developed by Mulliken and Glowacki in 1982 is based on
the cellular kinetics of anomalous vessels, providing a diagnostic and therapeutic approach based
on the biologic behaviour of the lesion. In this classification, two entities exist: 1) hemangiomas
and 2) vascular malformations [1,2]. The International Society for the Study of Vascular Anomalies
(ISSVA), in 1996, approved a classification system modified from the one proposed by Mulliken,
Glowacki (1982) [3]. The diseases were subdivided into (a) tumors: hemangioma (HEM), pyogenic
granuloma, rapidly involuting congenital hemangioma, noninvoluting congenital hemangioma,
hemangiopericytoma, tufted angioma and kaposiform hemangioendothelioma; and (b) vascular
malformation (VM) [4].
Wassef “et al.” [5] updated official ISSVA classification of vascular anomalies in 2015. The
General biological scheme of the classification is retained. The section on tumors has been expanded
and lists the main recognized vascular tumors, classified as Benign, locally aggressive or borderline,
and malignant. A list of well-defined diseases has been included under each generic heading in the
“Simple Vascular Malformations” section. Two new sections were created: one dealing with the
malformations of individually named vessels (previously referred to as “truncular” malformations);
the second groups lesions of uncertain or debated nature (tumor versus malformation) [5].
Hemangiomas are considered to be benign tumors and has a predilection towards of infancy that
are characterized by a rapid growth phase with endothelial cell. It presents as a red macula, papule
or nodule, depending on the congestion degree and on how deep it is in the tissue. Although HEM
is a benign lesion, in some cases, it may lead to compression of surrounding structures, formation of
fissures, ulcers or hemorrhages, and functional and aesthetic problems [6,7]. Oral HEM can be found
in the lips, tongue or buccal mucosa. It is more common in white female, in twins and in premature infants. On the other hand, vascular malformations are structural
anomalies of blood vessels without endothelial proliferation [1-3].
Clinically, they are similar to HEM; however, they are always present
at birth and grow as the patient physically develops [3]. It does not
spontaneously regress, remaining stable throughout life. Frequently,
bone involvement is present as a radiolucent, multilocular and wellcircumscribed
image [6]. The few studies on benign oral vascular
lesions frequently do not distinguish between oral HEM and VM, or
regard oral VM as a histological type of HEM, known as arteriovenous
hemangiomas [8].
Vascular Malformations may be single vessel forms (capillary,
arterial, lymphatic, or venous) or a combination. They are designated
according to the predominant channel type as capillary malformations,
lymphatic malformations, venous malformations, arteriovenous
malformations, and complex forms such as capillary lymphatico
capillary lymphatico- venous malformation. Malformations with an
arterial component are rheologically fast flow, while the remainder
are slow-flow. Hemangiomas are classified on the basis of their
histological appearance as capillary, cavernous or mixed. Capillary
hemangiomas are composed of many small capillaries lined with
a single layer of endothelial cells supported in connective tissue
stroma of varying density. Cavernous hemangiomas are formed by
large, thin-walled vessels or sinusoids that are lined with a single
layer of endothelium and are separated by thin septa of connective
tissue. Mixed hemangiomas consist of both capillary and cavernous
components [8].
Figure 1
Case Presentation
Case 1
A female patient of 35 years age reported to the Department of
Oral medicine and radiology of Government Dental College and
hospital Jammu with the chief complaint of swelling in the upper
gingival area for the past 2 months which was slowly progressive
nature. There were no relevant contributory history to our case
report. Patient was a Housewife, Vegetarian and had no history of
any tobacco usage of any form. On clinical examination no significant
extra-oral finding and no visible facial asymmetry was noted.Lymph
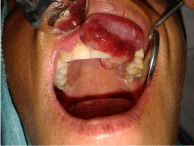
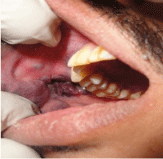
nodes were non palpable. Intra-orally a well defined erythematous
growth with distinct borders, arising from the gingival aspect of the
Maxillary Second Quadrant’s Central incisor to second pre molar
region was seen. The same lesion of 2.5 cm x 1.5 cm in size extended to
palatal aspect of the maxillary Premolar area (Figure 2). On palpation
the growth was firm in consistency with blanching and bleeding on
provocation was seen. Non tender,no ulceration and no pulsation or
bruit was noted (Figure 1 and 2).
Radiographical investigation: Intra-oral periapical (IOPA)
X-ray revealed the presence of an ill-defined radiolucency involving
the periapices of 23–25 with slight displacement of regional teeth.
There was no significant bone destruction (Figure 3). Based on
the clinical and radiological findings, a provisional diagnosis of
pyogenic granuloma was made. The differential diagnosis for this
intra oral lesion was peripheral ossifying fibroma and peripheral
giant cell granuloma. Incisional biopsy of both the soft tissue mass
and underlying bone was performed under local anesthesia. The
tissue was preserved in 10% formalin and sent for histopathological
examination.
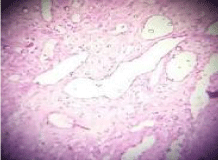
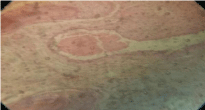
Histopathologically: The excised specimen showed few large
endothelial cells lined blood vessels and numerous proliferating
endothelial cell lined capillaries. Containing RBC’s in a lobular
pattern segregated by fibrous septa in the connective tissue stroma.
Chronic inflammatory infiltrate composed predominantly of Plasma
cells and Lymphocytes and few extravasated RBC’s were also present.
Thus, this was suggestive of capillary hemangioma (Figure 4).
Case 2
A male patient of 45 years age reported to the Department of Oral
Medicine and Radiology of Government Dental College and Hospital
Jammu with the chief complaint of swelling present over the right
side of his mouth since 2 months. There was no significant medical,
dental and family history given by the patient. The patient was a
businessman by profession, non vegetarian and had no history of any
tobacco usage of any form. Clinical examination of patient reveals no
extra oral swelling, no facial asymmetry and no palpable lymph nodes.
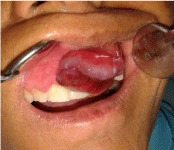
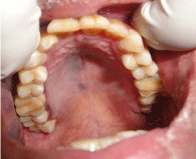
Intra oral examination revealed Multilobulated swelling present over
the right buccal mucosa area (Figure 5). There is irregularity in shape,
extending from retro-commercial area upto retromolar area, Around
4 cm x 3 cm, 2 cm x 3 cm & 2 cm x 2 cm in size respectively. Overlying
mucosa was reddish blue in color. (mention picture reference). A
growth was seen on buccal mucosa with burrowing on the buccal
vestibule Irregular in shape , overlying mucosa is deep red in color.
On palpation: Soft non - tender, easily bleeds on provocation.
A flat macular lesion is present near the palatal region on the right
side, blue in color around 2 cm x 2 cm in size diffuse in shape (Figure
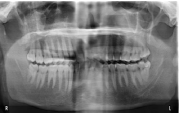
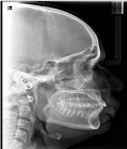
6). Radiographs were advised to rule out any bony lesion suggestive
of central variety of hemangioma, or any malignancy or to identify a
foreign body that should need to be removed with the lesion, however
in our case the orthopantomogram as well as the lateral cephalogram.
Didn’t reveal any significant changes (Figure 7).
Histopathpologically: The excised specimen showed stratified
squamous keratinized epithelium with the connective. Tissue stroma
showing large dilation of endothelial lined vascular spaces. Along
with engorged Red blood cells. Deeper connective tissue layers
showed chronic inflammatory cell infiltrates along with adipose and
muscle cells, all this suggested of vascular malformations (Figure 8).
Figure 2
Figure 3
Figure 4
Figure 5
Figure 6
Figure 7
Figure 8
Floaw Chart
Discussion
The history of hemangioma dates back to 1843 when Liston first
described the case of hemangiomas [9]. Later on cases of vertebral
hemangioma (Virchow, 1867) [9] cutaneous hemangiomas (Kasabach
and Merrit, 1940) were documented [10]. In 1973 Sznajder “et al.” [11]
described hemangiomas under the term ‘‘Hemorrhagichemangioma’’.
However, there have been many conflicting reports over the
nomenclature. Bormann first used the term hemangioendothelioma
in 1899 [12]. In 1908, Mallory used the term malignant vascular
tumor for this lesion [13]. Stout described the histological features
of hemangiomas in 1944 [14]. Hemangiomas are the most common
soft tissue tumor of childhood [15–17] and head and neck region is
the most common site for hemangiomas development (about 60% of
cases) [17]. Hemangiomas are the most common benign tumours of
the head and neck in children, but their occurrence on the palatal
mucosa is extremely rare [18]. In 80% of cases, hemangiomas occur as
single lesions [19]. Moreover, capillary hemangiomas have a 3:1 femalemale
ratio and occur more frequently among Caucasians than other
racial groups [19,20]. Also it has been documented that Hemangiomas
are the most common tumors of infancy, occurring in 5% to 10% of
1-year-old children. They are much more common in females than
males. The most common location is the head and neck region,
which accounts for 60% of all cases. Eighty percent of hemangiomas
occur as single lesions, but 20% of affected patients will have multiple
tumors. Hemangiomas of the oral mucosa may be flat or raised, often
multinodular, and distinctly reddish, blue, or purple [20,21]. Most oral
hemangiomas are located on the tongue, where they are multinodular
and bluish red. The multinodularity is racemose and diffuse. Tongue
angiomas frequently extend deeply between the intrinsic muscles of
the tongue. The lip mucosa is another common site for hemangiomas
in children; these tumors are usually localized, blue, and raised. The
aforementioned port-wine stain involves the facial skin and is flat and magenta in color. Histopathologically, hemangiomas are classified as
cavernous or capillary type according to their
Vascular network. Early hemangioma is characterized by the
presence of plump endothelial cells and indistinct vascular lumen and
is often known as turbine or cellular hemangiomas [23]. Thickened
multi laminated endothelial basement membrane with the ready
incorporation of tritiated. Thymidine in endothelial cells and the
presence of a large number of mast cells are noted in the Proliferating
phase of hemangiomas [24]. As it matures, the endothelial cells become
flattened and tiny capillary sized vascular spaces become prominent
[24]. When the lesion involutes,the vascular. As spaces become more
dilated (cavernous) and widely spaced [24]. There is little or no
incorporation of tritiated thymidine in endothelial cells and normal
count of mast cells are noted in the involuting phase [24]. Capillary
hemangiomas are usually present at birth, while most cavernous
hemangiomas occur in adulthood. Cavernous hemangiomas are less
common than capillary hemangiomas in all other areas of the body
except in the oral cavity. Almost all intraosseous hemangiomas of the
facial skeleton are to be cavernous type [24].
The diagnosis of hemangioma is based on clinical history and
physical examination. Imaging studies may be necessary to clarify and
confirm the diagnosis, and in order to analyze the extent of the lesions
by permitting an evaluation of their non-visible component as well
as the affection of neighboring structures. The imaging techniques
employed for hemangiomas include MRI, CT, CT with contrast
media, ultrasonography and angiographic techniques (arteriography,
phlebography) [25-32].
Syndromes associated with cavernous hemangiomas are Sturge
Weber syndrome, Kasabach Merritt syndrome, PHACE (posterior
fossa brain malformations, haemangioma of the face, arterial
cerebrovascular anomalies, cardiovascular anomalies, eye anomalies,
and sterna defects or supraumbilical raphe) syndrome [33].
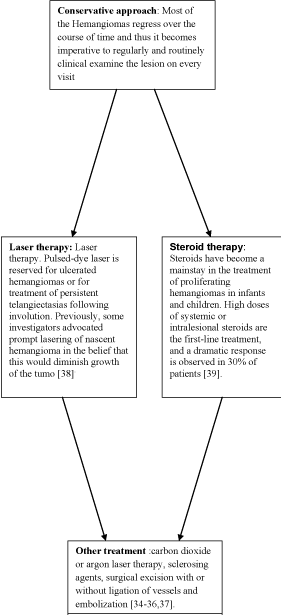
The management of hemangiomas of the oral mucosa varies
according to the age of the patient, the size of the lesion, the site of
involvement and the clinical nature of the hemangioma. The range
of treatment includes steroid therapy, carbon dioxide or argon laser
therapy, sclerosing agents, surgical excision with or without ligation
of vessels and embolization [34-36,37]. Larger lesions that extend
into muscles are more difficult to eradicate surgically, and sclerosing
agents such as 1% sodium tetradecyl sulfate may be administered by
intralesional injection. These agents result in postoperative pain, and
the patient must be managed with a moderate-level analgesic such as
oxycodone or aspirin with codeine. Cutaneous port-wine stains can
be treated by subcutaneous tattooing or by argon laser. However in
our case 1, after all lab investigations and histo pathological reports
were done, surgical excision of the lesion was performed under local
anesthesia under all aseptic conditions. Because the lesion was localized
and had no underlying pathology. There is been no recurrence of the
lesion at 1-month, 6-month, or 1-year follow-ups as patient has been
reviewed periodically. In our 2nd case intralesional triamcinolone
acetonide (4 mg/mL) was started weekly upto 6 months. Patient had
a definite response and showed great improvement. The patient has
been on review (Flow Chart).
Conclusion
Haemangiomas are common benign vascular growth , but their occurrence in the oral cavity has been rare, thus it becomes imperative for dental professional to evaluate them clinically,histopathologically and undertake all necessary investigation. Dental professionals should be well versed with all the clinical and treatment modalities that are associated with hemangiomas and all necessary precautions should be taken before attempting surgical excision as the tissues may bleed profusely and unexpectedly.
References
- Patel SB, Desai A, Desai S, Vyas RR, Soni HC. Case Report:Vascular lesions of face. Ind J Radiol Imag. 2003;13(3):257-260.
- Regezi JA, Sciubba JJ, Jordan RCK editors: Oral pathology: Clinical pathologic correlations. 4th ed. St Louis: W.B. Saunders, 2003; pp111-112.
- Mulliken JB, Glowacki J. Hemangiomas and vascular malformations in infants and children: a classification based on endothelial characteristics. Plast Reconstr Surg. 1982;69(3):412-22.
- BEAN WB. The changing incidence of certain vascular lesions of the skin with aging. Geriatrics. 1956;11(3):97-102.
- Wassef M, Hunt SJ, Santa Cruz DJ, Barnhill RL. Vascular tumors and vascular malformations. In: Barnhill RL, Crowson AN, Magro CM, Piepkorn MW, eds. Dermatopathology. 3rd ed. New York, NY: McGraw- Hill; 2010:802–856
- Donnelly LF, Adams DM, Bisset GS 3rd. Vascular malformations and hemangiomas: a practical approach in a multidisciplinary clinic. AJR Am J Roentgenol. 2000;174(3):597-608.
- Jackson IT, Carreño R, Potparic Z, Hussain K. Hemangiomas, vascular malformations, and lymphovenous malformations: classification and methods of treatment. Plast Reconstr Surg. 1993;91(7):1216-30.
- Barrett AW, Speight PM. Superficial arteriovenous hemangioma of the oral cavity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90(6):731-8.
- Nandaprasad S, Sharada P, Vidya M, Karkera B, Hemanth M, Kage C. Hemangioma - a review. Internet J Hematol 2008;l6(2).
- Capillary hemangioma with extensive purpura: report of a case, .Am J Dis Child 1940;59:1063–70.
- Sznajder N, Dominguez FV, Carraro JJ, Lis G. Hemorrhagic hemangioma of gingiva: report of a case. J Periodontol. 1973;44(9):579-82.
- Borrmann R. Metastaserbildung bis histologisch gutartigin Geschuulsten (fall metastasierendem Anjoun). Beitr z Path Anat 1907; 40: 372.
- Mallory FB. The results of the application of special histological methods to the study of tumors. J Exp Med. 1908;10(5):575-93.
- Stout AP. Hemangio-Endothelioma: A tumor of Blood Vessels Featuring Vascular Endothelial Cells. Ann Surg 1943; 118(3): 445-64 Oral cavernous haemangioma with phleboliths
- Kutluhan A1, Bozdemir K, Ugras S. The treatment of tongue haemangioma by plasma knife surgery. Singapore Med J. 2008;49(11):e312-4.
- Eivazi B1, Ardelean M, Bäumler W, Berlien HP, Cremer H, Elluru R, et al. Update on hemangiomas and vascular malformations of the head and neck. Eur Arch Otorhinolaryngol. 2009;266(2):187-97.
- Werner JA, Dünne AA, Folz BJ, Rochels R, Bien S, Ramaswamy A, et al. Current concepts in the classification, diagnosis and treatment of hemangiomas and vascular malformations of the head and neck. Eur Arch Otorhinolaryngol. 2001;258(3):141-9.
- Lale AM, Jani P, Coleman N, Ellis PD. A palatal haemangioma in a child. J Laryngol Otol. 1998;112(7):677-8.
- Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. 2nd ed. Saunders Philadelphia, p:390-2, 2002.
- Braun IF, Levy S, Hoffman JC Jr. The use of transarterial microembolization in the management of hemangiomas of the perioral region. J Oral Maxillofac Surg. 1985;43(4):239-48.
- Neville BW, Damm DD, Allen CM, Bouquot JE (ed): Oral & maxillofacial pathology, 2nd edn. Philadelphia: W.B. Saunders, 2002, pp 467-468.
- Olsen KI, Stacy GS, Montag A. Soft-tissue cavernous hemangioma. Radiographics. 2004;24(3):849-54.
- Neville BW, Damm DD, Allen CM, Bouquot JE. Oral &maxillofacial pathology. 2nd ed. Philadelphia: Saunders; 2002, p. 390–2.
- Shafer’s textbook of oral pathology, . 7th ed. Elsevier; 2012, p. 144–8.
- Martínez de la Cuesta A1. [Imaging studies in the diagnosis of haemangiomas and vascular malformations]. An Sist Sanit Navar. 2004;27 Suppl 1:71-80.
- Kakimoto N, Tanimoto K, Nishiyama H, Murakami S, Furukawa S, Kreiborg S. CT and MR imaging features of oral and maxillofacial hemangioma and vascular malformation. Eur J Radiol. 2005;55(1):108-12.
- Yonetsu K, Nakayama E, Miwa K, Tanaka T, Araki K, Kanda S, et al. Magnetic resonance imaging of oral and maxillofacial angiomas. Oral Surg Oral Med Oral Pathol. 1993;76(6):783-9.
- Kaplan PA, Williams SM. Mucocutaneous and peripheral soft-tissue hemangiomas: MR imaging. Radiology. 1987;163(1):163-6.
- Levine E, Wetzel LH, Neff JR. MR imaging and CT of extrahepatic cavernous hemangiomas. AJR Am J Roentgenol. 1986;147(6):1299-304.
- Paltiel HJ, Burrows PE, Kozakewich HP, Zurakowski D, Mulliken JB. Soft-tissue vascular anomalies: utility of US for diagnosis. Radiology. 2000;214(3):747-54.
- Fontes A, Campos MS, de Sousa SC, Martins MT, Nunes FD. Diagnostic implications of oral intravascular papillary endothelial hyperplasia. Odontology. 2011;99(1):92-7.
- Cohen A, Maly A, Azaz B. Intravascular papillary endothelial hyperplasia of the lower lip: surgical approach and review of the literature. Gerodontology 2009; 26:305-308.
- Shafer, Hine, Levy. Shafer’s Textbook of Oral Pathology. 6thed.Noida (India): Elsevier; 2009.197-202
- Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. 2nd ed. Saunders Philadelphia, p: 390-2, 2002.
- Dilley DC, Siegel MA, Budnick S. Diagnosing and treating common oral pathologies. Pediatr Clin North Am. 1991;38(5):1227-64.
- Chin DC. Treatment of maxillary hemangioma with a sclerosing agent. Oral Surg Oral Med Oral Pathol. 1983;55(3):247-9.
- Braun IF, Levy S, Hoffman JC Jr. The use of transarterial microembolization in the management of hemangiomas of the perioral region. J Oral Maxillofac Surg. 1985;43(4):239-48.
- Garden JM, Bakus AD, Paller AS. Treatment of cutaneous hemangiomas by the flashlamp-pumped pulsed dye laser: prospective analysis. J Pediatr 1992; 120:555– 60.
- Mulliken JB, Boon LM, Takahashi K, et al. Pharmacologic therapy for endangering hemangiomas. Curr Opin Dermatol. 1995;109-113.