Case Report
Surgical Treatment of Extensive Hemangiomas of the Neck among Children
Baymakhanov BB, Muradov MI*, Bayguzeva АА, Mukhamedkerim KB, Kazantaev KE and Koshkarbaev DZh
Department of Reconstructive, Plastic and Aesthetic Microsurgery A. Syzganov's National Scientific Center of
Surgery, Republic of Kazakhstan
*Corresponding author: Muradov MI, Department of Reconstructive, Plastic and Aesthetic Microsurgery, A. Syzganov's National Scientific Center of Surgery, Zheltoksan 62, Almaty, 05004, Republic of Kazakhstan
Published: 20 Mar, 2017
Cite this article as: Baymakhanov BB, Muradov MI,
Bayguzeva АА, Mukhamedkerim
KB, Kazantaev KE, Koshkarbaev
DZh. Surgical Treatment of Extensive
Hemangiomas of the Neck among
Children. Ann Clin Case Rep. 2017; 2:
1310.
ISSN: 2474-1655.
Abstract
Background: Treatment of hemangiomas still remains one of the urgent problems of modern
medicine. The main problems of Hemangiomas are characterized by a rapid, progressive growth.
Growing, they destroy surrounding tissue and cause significant functional and cosmetic damage to
the patient.
Case Presentation: In this paper, for example of 14 patients with hemangiomas of the neck had been
shown that the optimal treatment of hemangiomas are stage endovascular embolization followed by
surgical removal of formation. In the absence of conditions for endovascular embolization and with
contraindications for using of propranolol is recommended operative treatment using microsurgical
techniques and bloodless technologies.
Conclusions: In control of the ultrasound examination after 1 year was performed, no recidive
growth of formation. All patients were examined at various time intervals after surgery recidive
growth of formation is not revealed. In the absence of conditions for endovascular embolization, if
exist contraindications for the use of propranolol we prefer operative treatment using microsurgical
techniques and bloodless technologies.
Keywords: Hemangiomas–reconstructive; Plastic and aesthetic microsurgery–children
Introduction
Treatment of hemangiomas still remains one of the urgent problems of modern medicine. The
main problems of Hemangiomas are characterized by a rapid, progressive growth. Growing, they
destroy surrounding tissue and cause significant functional and cosmetic damage to the patient [1].
Currently there are more than 50 methods of treatment of hemangiomas with different
mechanisms of action [2–5]. This is due to the different localization of formations, multiple forms
of their manifestations and search for optimal treatment. At the same time, the surgical method
in the treatment of hemangiomas is still one of the main. In reconstructive, plastic and aesthetic
microsurgery department of National Scientific Center of Surgery named after A.N. Syzganov for
2 years were operated 14 patients with hemangiomas of the neck. The age of patients ranged from
1 to 10 years. In anamnesis in 8 of them on tumors previously held several of interventions in the
department of endovascular surgery (cryo, laser destruction, excision, embolization, conservative
treatment by propranolol etc). 6 patients came primary diagnosis of the presence of formations was
not difficult. Accompanying relatives of patients complained of the presence of large formations on
the neck, changing color depending on the position of the child. 3 patients had significant limitation
of movement of the head, deviation of the neck, 4 patients had pain syndrome, due to compression
of the primary trunks of the brachial plexus. In all patients, the presence of hemangioma was
determined during the first month of life. On examination revealed localization, prevalence and
functional impairment determined by palpation symptoms "squeezing and filling". Soreness
occurred in 4 patients. Pulsation determined on 5 formations. All formations were soft consistency,
immobile performing imaging studies was limited. Age of children was not always allowed to
perform certain research. At the same time, ultrasound, angiography, and magnetic resonance
imaging were performed in all children.
Ultrasound examinations of hemangiomas were performed using high-resolution linear
encoder 8 MHz. To rate blood flow was applied pulse Doppler and color mapping of the flow. With
the help of electronic meters measured linear sizes of hemangiomas, and using a ruler stroke a path and calculates the area of hemangiomas. Carrying out ultrasound
investigation in 14 patients with hemangiomas, allowed us to set the
depth of lesion, clarify the localization of hemangioma, anatomic
topographical relationship of the tumor to the surrounding tissues,
degree of interest of main vessels and blood flow speed in the formation
and in parenchyma. In our observations sizes of hemangiomas ranged
from 5.0 cm x 4.0 cm to 17.0 cm x 9.0 cm. Formation had irregular
shapes, deckle-edged. Sonographic signs of capsule were detected
only in 3 cases and corresponded to cavernous forms. During Doppler
ultrasound in 9 patients with cavernous and mixed hemangiomas in
formations identified blood flow. It was characterized by "mosaic"
view due to multiple un-and hypoechogenic areas of irregular shape
with a diameter- 0.1-0.2 cm, representing the vessel lumen. With
angiography identified the sources and variations of blood supply in
the affected area, localization, sizes and character of vascular changes.
In 4 patients formation sprouted into the surrounding tissues and
had a relationship with a major vascular system, studied blood flow
speed, and also 2 patients conduct differential diagnostics of complex
of hemangiomas with different forms angiodysplasias. Magnetic
resonance imaging performed on the MRI's magnetic field of 1.5
tesla. Scanning was planned in three mutually perpendicular planesaxial,
sagittal, coronal, mode T1-T2-weighted images. On magnetic
resonance imaging in all patients indicated the presence of soft tissue
formation, inhomogeneous structure with hyper intense areas.
Surgery was performed under general anesthesia with the
use of microsurgical techniques, increase (microsurgical loupe),
microsurgical instruments and hyperfine suture material.
13 patients were performed stage endovascular embolization (up
to 4-5 times) followed by excision of formation under magnification to
5 times. In these operations no technical difficulties were encountered,
as hemangiomas were sclerosed. Blood loss was minimal. Difficulties
were raised in the allocation of the anatomical structures of the neck from sclerosed tissue.
Figure 1
Figure 2
Case Presentation
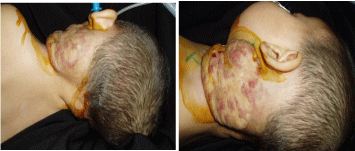
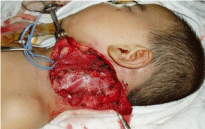
Patient "K" 1 year 4 months has been hospitalized with the
diagnosis: "Tumor formation left to neck with compression of the
nerve trunks of cervical and brachial plexus". Complained on the
presence of a painful neck tumor formation, labored breathing,
movement disorders of the head and left upper extremity, sleep
disorder.
From the words of her mother she has the formation from birth.
The formation still is increasing. Over the last month pain appeared
in the field of formation, labored breathing, movement disorders of
the head and left upper extremity, sleep disorder. Over the entire
period formation has changed color from flesh to cyanotic-purple.
locally: on the left side of the neck with the transition to the front
and back surfaces has a tumor formation, rounded shape, sizes 16.0
cm x 9.0 cm, holding ½ of the perimeter surface of the neck, purple
colored, moderately painful, soft-elastic consistency, immobile,
pulsing. During Valsalva probe has been a sharp expansion of the
internal jugular vein. Active and passive movements of the left upper
extremity are painful (Figure 1 and 2).
Besides general clinical examination conducted instrumental
methods of research. Doppler ultrasound: cavernous hemangioma
of the neck on the left. Common carotid artery and internal jugular
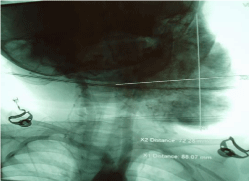
vein are passable. Thoracic aortography: Angiographic picture
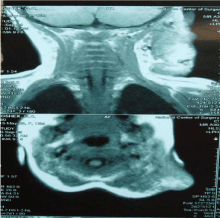
volumetric formation of the left half of the neck (Figure 3). Magnetic
resonance imaging of soft tissues of the neck: soft-tissue formation
in the projection of the soft tissues of the neck on the left (Figure
4). Magnetic resonance imaging of the brain: residual signs of encephalopathy with unexpressed ventriculomegalia. The formation
of cervical region on the left ECG result: sinus bradycardia.
Patient was examined by oncologist, cardiologist, maxillofacial
surgeon, pediatrician, vessel surgeon. Consilium recommended
phasing endovascular embolization followed by excision of formation.
Patient underwent unsuccessful attempt of endovascular
destruction in relation with the throw back of a contrasting substance
into the internal jugular vein which could worsen the condition
of the child. Considering to growth of labored breathing, pain
syndrome, clinic of compression the nerve trunks of the brachial and
cervical plexus, been decided not to perform the second attempt of
embolization and remove the formation.
Under general anesthesia using a 2.5-fold increase was performed
operation: excision of tumor formation of the neck. Operation
stages: after appropriate processing of the surgical field, to reduce the
amount of blood loss as possible, performed finger "pushed out" of
formation, while formation became flesh colored. At the base of the
tumor imposed mild intestinal clamps. The skin over the bloodless
formation dissected in obliquely - longitudinal direction. At revision:
the formation is a cellular structure without a capsule, intimately
soldered with sub clavian vein, common carotid artery to the
bifurcation level, grows into the neck muscles, intimately soldered to
the nerve trunks of the cervical and brachial plexus, thyroid cartilage.
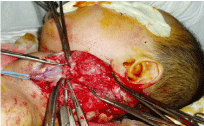
Tumor nourishment was carried out of the pool of the common
carotid artery, branch of the thyroid-cervical trunk. Outflow of blood
is carried by the supraclavicular vein (Figure 5). It was performed
removal of formation with excision of superficial neck muscles, partial
excision of the sternocleidomastoid, scalenes muscles. Alloying of the
nourishment vessels of formation with excision of supraclavicular
vein (Figure 6). Blood loss was 50 ml the resulting defect of covering
tissues was removed by plastic with local tissues (Figure 7). Active
wound drainage. Pathology-histological conclusion: Juvenile capillary
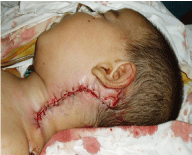
hemangioma of the neck. Postoperatively, the patient received anti-bacterial, anti-inflammatory therapy. The general condition has
stabilized. Sutures are removed on the 11th day. Child had been
discharged in satisfactory condition with the recommendations.
Figure 3
Figure 4
Figure 5
Figure 6
Figure 7
Figure 8
Conclusion
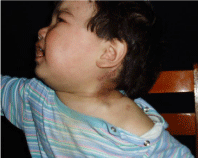
In control of the ultrasound examination after 1 year was performed, no recidive growth of formation (Figure 8). All patients were examined at various time intervals after surgery recidive growth of formation is not revealed. Thus, the optimal treatment of hemangiomas is a stage endovascular embolization followed by surgical removal of formation. In the absence of conditions for endovascular embolization, if exist contraindications for the use of propranolol we prefer operative treatment using microsurgical techniques and bloodless technologies.
References
- Greco A, D'Erme AM, Zamma Gallarati B, Caputo R, de Martino M. A further experience for severe infantile hemangiomas of the face: an observational study. Dermatol Ther. 2014;27(4):198-202.
- Semkova K, Kazandjieva J, Tsankov NK. What's new in infantile hemangiomas: current insights and future perspectives. Skinmed. 2013;11(6):341-9.
- Yilmaz S, Kozakewich HP, Alomari AI, Fishman SJ, Mulliken JB, Chaudry G. Intramuscular capillary-type hemangioma: radiologic-pathologic correlation. Pediatr Radiol. 2014;44(5).
- Ji Y, Chen S, Li K, Li L, Xu C, Xiang B. Signaling pathways in the development of infantile hemangioma. J Hematol Oncol. 2014;7:13.
- Funk T, Prok L, Brown LD, Bruckner AL. Multifocal vascular tumors and fetal hydrops. J Pediatr. 2014;164(5):1214-8.