Clinical Image
Atypical Trigeminal Trophic Syndrome: A New Cause of Facial Ulceration?
Maria-Angeliki Gkini1*, Taylor R2 and Bewley AP1
1Department of Dermatology, Royal London Hospital, UK
2Department of Liaison Psychiatry, Royal London Hospital, UK
*Corresponding author: Maria-Angeliki Gkini, Department of Dermatology, Royal London Hospital, Whitechapel Road, Whitechapel, E1 1BZ, London, UK
Published: 08 Mar, 2017
Cite this article as: Gkini M-A, Taylor R, Bewley AP.
Atypical Trigeminal Trophic Syndrome:
A New Cause of Facial Ulceration?. Ann
Clin Case Rep. 2017; 2: 1292.
Clinical Image
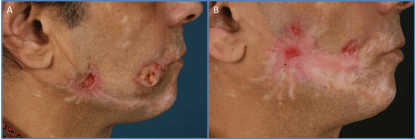
We present a case of a 56-year-old Caucasian male patient, who presented to our specialist
psychodermatology clinic, complaining about severe chronic facial pain, bilateral ulceration and
scarring, following the mandibular nerve distribution. All this condition started 6 years ago. The
affected areas included left and right cheeks, left post-auricular area and chin. The triggering factor
appeared to be an episode of shingles. Before his referral at our clinic, his skin lesions were attributed
either to dermatitis artefacta or acne excoriee. He was previously treated with antipsychotic
medication and psychotherapy, with no significant improvement in his condition.
Differential diagnosis of facial ulcers included malignancy, infection, vasculitis, pyoderma
gangrenosum and psychodermatologicaldisorders (dermatitisartefacta, trigeminal trophic
syndrome, atypical trigeminal trophic syndrome and acne excoriée).
Swabs from active ulcers were taken and were negative for pathogens, excluding infection.
Blood results revealed microcytic anaemia, with no underlying cause. Biochemical check for
pruritus, including liver function, urea and electrolytes, thyroid function, syphilis serology, was
negative. Vasculitis serology was negative. A skin biopsy was performed showing only scarring of
the epidermis, excluding malignancy and pyoderma gangrenosum. Magnetic resonance craniofacial
imaging was also performed showing mild chronic inflammation of the facial sinuses. Finally,
neurophysiology, including electromyelogram, revealed bilateral trigeminal nerve dysfunction on
both trigeminal nerves, which was in favour of atypical trigeminal trophic syndrome.
After previous treatment with antipsychotics and psychotherapy with limited efficacy, the
patient had a lengthy consultation with pain services in association with our multidisciplinary
team and he was started on aripiprazole 5 mg daily, morphine sulphate (MST) 40mg twice daily,
pregabalin 300 mg twice daily, duloxetine 60 mg twice daily, oxcarbazepine 150 mg twice daily and
topical lidocaine patches.
Trigeminal Tropic Syndrome (TTS) is a rare but important cause of facial ulceration
characterised by ulceration, anaesthesia and paraesthesia following the distribution of trigeminal
syndrome [1,2]. Injury to the trigeminal nerve, central or peripheral, is the main causative agent.
The resulting intractable dysasthesia leads to self-mutilating behaviour resulting in ulcers [1-3]. Diagnosis is made clinically1and neurophysiological studies can be helpful in evaluating function of
the trigeminal nerve [4] TTS is a unilateral condition, typically responding well to antidepressants or antipsychotics [1,2].
Nevertheless, our patient presented with an atypical, bilateral condition that was highly
refractory to established treatments. We believe this patient has a clinically new entity, named as atypical trigeminal trophic syndrome (ATTS) [5], which we
are seeing in an increasing number of patients in our tertiary
psychodermatology clinic. In ATTS, present with bilateral disease
and this is confirmed by nerve conduction studies. Skin involvement
is extensive and may fluctuate in severity. ATTS is highly refractory
to treatment and an obsessive-compulsive element often develops,
which is much less a feature of TTS. We also believe that patients
with ATTS are particularly difficult to treat even with agents that
are typically efficacious in TTS. Clinicians should be aware of this
condition in order to ensure that patients are appropriately referred
to an experienced, multidisciplinary team to manage this mutilating
disorder (Figure 1A and B).
Figure
References
- Kurien AM, Damian DL, Moloney FJ. Trigeminal trophic syndrome treated with thermoplastic occlusion. Australas J Dermatol. 2011; 52: 1-4.
- Setyadi HG, Cohen PR, Schulze KE, Mason SH, Martinelli PT, Alford EL, et al. Trigeminal trophic syndrome. South Med J. 2007; 100: 43-48.
- Sawada T, Asai J, Nomiyama T, Masuda K, Takenaka H, Katoh N. Trigeminal trophic syndrome: report of a case and review of the published work. J Dermatol. 2014; 41: 525-528.
- Bewley A, Taylor R, Reichenberg, J, Magrid M. Practical Psychodermatology. London, UK: Wiley Blackwall, 2014.
- Rashid RM, Khachemoune A. Trigeminal trophic syndrome. J Eur Acad Dermatol Venereol. 2007; 21: 725-731.