Case Report
A Case of Pharynx Syphilis at Secondary Stage
XU Wen, YU Shaoqing* and JIN Ling
Department of Otolaryngology, Tongji Hospital, Tongji University
*Corresponding author: Yu Shaoqing, Department of Otolaryngology, Tongji Hospital, 389 Xincun road, Putuo District, Shanghai city 200065, China
Published: 03 Mar, 2017
Cite this article as: Wen X, Shaoqing Y, Ling J. A Case of
Pharynx Syphilis at Secondary Stage.
Ann Clin Case Rep. 2017; 2: 1287.
Abstract
A 48-year-old female patient had throat discomfort and slightly pain for three month. Her symptom was getting aggravated and repetitive after being misdiagnosed with acute tonsillitis. Later, we found patient’s mucous membrane of double tonsil, palatoglossus arch, palatopharyngeus arch, palatine uvula was covered by white pseudo-membrane. It was suspected as syphilis of the pharynx. Rapid Plasma Reagin (RPR) and Treponema Pallidum Hemagglutination Assay (TPHA) tests confirmed the pharynx syphilis. After the patient went through the anti-syphilitic remedy, her symptoms and signs completely disappeared. During the 24-month routinely follow-up, no relapse was observed and the pharynx lesion disappear accompany with negative RPR tests results.
Keywords: Pharynx; Syphilis; Secondary syphilis
Introduction
Syphilis is a sexually transmitted disease caused by the spirochete Treponema pallidum. Syphilis
could affect any human organs and tissues and trigger various manifestations. The incubation
period of Treponema pallidum is between 15 and 90 days. Recently, the incidence of syphilis is
increased rapidly in China, and it is ranked number three among infectious diseases in China,
only preceded by tuberculosis and hepatitis. China economy development, imbalance of male and
female population, emergence of numerous migrant workers from rural area, the social acceptance
of sexual services, and the growth in number of male homosexuality are the major attributions to
the increase in incidence rate of syphilis [1]. Such incidence rate grew from 6.43 percent of every one
hundred thousand population in 2000 to 32.86 percent in 2013 [2].
The typical site infected by syphilis is genital. About 85 percent of patients with primary syphilis
have genital chancre, and only 4 percent of them have oropharynx be affected [3]. The typical site are
the genital area but 5% of all chancres are extra genital and the mouth is the most frequent location
especially in man who have sex with men. The primary chancre can also occur on anus, fingers,
nipples [4]. The manifestations of syphilis is more complicated nowadays and it is more easily to
get missed and misdiagnosed by physicians [5]. Therefore, pharynx syphilis report is currently quite
rare.
Case Presentation
A 48-year-old female patient had no fever but throat discomfort, mild sore throat, cough, and voice hoarseness three months ago. Her symptom was getting aggravated, and she personally started taking anti-infective medicine as treatment. However, it did not ease her symptoms, so she visit Tongji Hospital’s otolaryngology department and she was preliminarily diagnose with acute tonsillitis. The doctor in Tongji Hospital treated this female patient by using penicillin and metronidazole intravenous dose, and her manifestations were mitigated. However, once the patient’s treatment was discontinued for several days, her manifestations would relapse. On May 20, 2011, this female patient had first visit of my department for another opinion, and I found that she had throat congestion and lymphadenopathy. In addition, mucous membrane of double tonsil, palatoglossus arch, palatopharyngeus arch, palatine uvula was covered by white pseudomembrane, which did not bleed but was hard to be erased and became painful once it was touched (Figure 1). Three tests were performed: rapid plasma regain circle card test (PRP) had titer of 1:64; Treponema Pallidum Hemagglutination test (TPHA) yield positive reaction; HIV screening test show negative result. Later, dermatology department was also invited for consultation. The female patient denied having any unclean sexual intercourse history after being further inquired of her medical history. The husband of this female patient was advised to see the doctor. It was found that he had genital syphilis and he admitted that he had unclean sexual intercourse history. Based on the test results, this female patient was diagnosed with secondary syphilis. To cure the syphilis, a single dose of 2.4 million unit’s benzathine penicillin G was delivered intramuscularly to this female patient once a week for three weeks. The method was very effective and the patient’s manifestations were completely gone during the second week of treatment. Her throat congestion was eased and the white pseudo-membranous gradually subsided (Figure 2). Additionally, the RPR serum antibody titers dropped to 1:4 significantly two weeks later, and disappeared after four weeks of treatment During the 24-month routinely follow-up, the recurrence of clinical symptoms was not observed and throat lesions disappeared. Moreover, the female patient received serum RPR testing once every three months during the follow-up period, and the testing results were negative reactions.
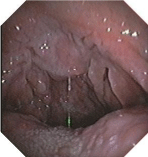
Figure 1
Figure 1
Fiber optic laryngoscopy view before pharynx syphilis treatment:
tonsil, palatoglossus arch, palatopharyngeus arch, palatine uvula was
covered by white pseudomembrane.
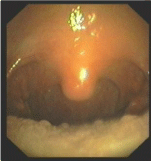
Figure 2
Figure 2
Fiber optic laryngoscopy view after pharynx syphilis treatment:
damaged pharynx mucous membrane recovered.
Discussion
Syphilis has four stages, and it may be so inconspicuous as to go
unnoticed. It is highly infectious in this stage owing to the prosperity
of the spirochetes in the site of primary lesion [6]. The early stages
of syphilis include primary and secondary stage. Besides genital,
pharynx is another common site for lesion. In addition to the impact
on pharynx, most patients with secondary stage of pharynx syphilis
may have their genitals and/or other parts of the body been infected
simultaneously. Other manifestations may include skin and mucous
membrane rashes, cervical lymphadenopathy, pathological changes
on eyes, etc. Primary stage of pharynx syphilis will manifest by
painless chancre developed at the site of infection (usually at tonsil) 2
to 4 weeks following the exposure.
Patients with secondary stage of pharynx syphilis may manifest by
infected mucous membrane. Mucosal plaques are the most common
oral manifestation in the secondary stage [7].
Damages on mucous membrane of pharynx mainly reflect
from two aspects: First, mucosa patches are the most common oral
manifestation during the secondary stage. Second is flat wart. Patients
may or may not have obvious symptom. But, they may experience
mild sore throat and sensation of foreign body. Generally, the lesion
sites of pharynx syphilis are palatine uvula, soft palate, double tonsil,
etc [8]. Laryngeal syphilis is quite rare.
With the increase in incidence rate of syphilis, more and
more patients with infected mucous membrane in pharynx as
initial manifestation have their first diagnosis at departments of
otolaryngology. But, they may be missed or misdiagnosed by relatively
in experience physicians. Therefore, patients who have infected
mucous membrane as initial manifestation should be distinguished
from patients with catarrhal pharyngitis and suppurative tonsillitis.
Manifestations and pathology changes of both types of patients
may has an acute onset, but patients with catarrhal pharyngitis and
suppurative tonsillitis may have fever and other symptom. If those
patients (especially those facing high risk of sexually transmitted
infections) whose pharynx lesions could not be confirmed, physicians
should inquire into patients’ case history for more details and consider
the possibility of pharynx syphilis. In this case, the female patient had
no fever but throat discomfort and progressive mild sore throat. At
first, she was misdiagnosed with acute tonsillitis by another hospital.
Later, she visited my hospital, and her mucous membrane of double
tonsil, palatoglossus arch, palatopharyngeus arch, palatine uvula was
covered by white pseudomembrane. It was suspected as syphilis of
the pharynx. RPR and TPHA tests confirmed the pharynx syphilis.
Currently, diagnosis of syphilis is mainly based on medical history of
patients, the form of infected mucous membrane, and serologic tests
in which TPHA and RPR tests are the key standard for the diagnosis.
Conclusion
Pharynx syphilis of some patients may be alleviated by certain inappropriate treatment, but it may not completely kill treponema pallidum because it is not antisyphilitic treatment. Thus, inappropriate treatments for syphilis will lead to recurrence of symptoms, and it is highly contagious. Early diagnosis of syphilis is a fundamental precondition to prevent the syphilis from spreading.
References
- Tucker JD, Cohen MS. China's syphilis epidemic: epidemiology, proximate determinants of spread, and control responses. Curr Opin Infect Dis. 2011; 24: 50-55.
- Gong XD, Yue XI, Teng F, Jiang N, Men PX. Syphilis in China from 2000 to 2013:epidemiological trends and characteristics. Chin J Dermatol. 2014; 47: 310-315.
- Viñals-Iglesias H, Chimenos-Küstner E. The reappearance of a forgotten disease in the oral cavity:syphilis. Med Oral Patol Oral Cir Bucal. 2009; 14: e416-420.
- Drago F, Ciccarese G, Cogorno L, Tomasini CF, Cozzani EC, Riva SF, at al. Primary syphilis of the oropharynx: an unusual location of a chancre. Int J STD AIDS. 2015; 26: 679-681.
- Drago F, Agnoletti AF, Ciccarese G, Cozzani E, Parodi A. Two cases of oligosymptomatic neurosyphilis in immunocompetent patients: Atypical neurosyphilis presentation. Int J STD AIDS. 2016; 27: 155-156.
- Lahav G, Lahav Y, Ciobotaro P, Ziv N, Halperin D. Laryngeal syphilis: a case report. Arch Otolaryngol Head Neck Surg. 2011; 137: 294-297.
- Ficarra G, Carlos R. Syphilis: the renaissance of an old disease with oral implications. Head Neck Pathol. 2009; 3: 195-206.
- Ikenberg K, Springer E, Bräuninger W, Kerl K, Mihic D, Schmid S, at al. Oropharyngeal lesions and cervical lymphadenopathy: syphilis is a differential diagnosis that is still relevant. J Clin Pathol. 2010; 63: 731-736.