Case Report
Intramural Duodenal Hematoma after Upper Gastrointestinal Endoscopic Biopsy in Children: Two Case Reports and Literature Review
Kestutis Trainavicius* and Ruta Vilija Dagilyte
Children's Hospital, Affiliate of Vilnius University Hospital Santariskiu Klinikos, Lithuania
*Corresponding author: Kestutis Trainavicius, Children's Hospital, Affiliate of Vilnius University Hospital Santariskiu Klinikos, Vilnius University, Vilnius, Lithuania
Published: 09 Feb, 2017
Cite this article as: Trainavicius K, Dagilyte RV. Intramural
Duodenal Hematoma after Upper
Gastrointestinal Endoscopic Biopsy
in Children: Two Case Reports and
Literature Review. Ann Clin Case Rep.
2017; 2: 1265.
Abstract
Intramural duodenal haematoma is an uncommon lesion, usually a complication of blunt abdominal trauma in children and young adults. We present two clinical cases of intramural duodenal haematoma following endoscopic biopsy, which caused partial duodenal obstruction and pancreatitis and resolved with conservative management.
Keywords: Intramural duodenal haematoma; Endoscopic biopsy complication; Conservative management
Introduction
Endoscopic biopsies are a widely used diagnostic tool for celiac disease, gastric ulcers and graft versus host disease. An intramural duodenal hematoma (IDH) is a rare complication of endoscopic biopsy. To our knowledge, there have been 30 other reported cases in literature of this complication and 21 (70%) [1,2] of them presented in patients 18 years old and younger. Most IDHs require conservative management, however it is also associated with pancreatitis, duodenal perforation and biliary obstruction, and, therefore, it is a complication that all pediatric endoscopist should be aware and cautious. We present two clinical cases here of post-endoscopic biopsy IDHs and review literature regarding diagnosis and management of IDH. The first case is of a boy with no previous risk factors, while the second case is in a patient with long history of immunosuppression and a previous bone marrow transplant.
Case Presentation
Case 1
A 12 year old boy underwent an upper endoscopy because of complaints of poor appetite,
inconstant feces and abdominal pain. He had no history of bleeding or failure to thrive. The
endoscopy was performed with “Olympus” video gastroduodenoscope (8.8 mm diameter). Multiple
lesions in the antrum area were observed and biopsies of the esophagus, stomach and duodenum
were obtained using “Olympus” forceps. Histological examination showed mild inflammation of
the esophagus and a pathological diagnosis of reflux esophagitis was concluded. After the procedure
the patient was stable and was discharged home with no present complaints. Two hours after
the discharge, he was re-admitted with abdominal pain (VAS-10) and frequent vomiting. On
physical examination diffuse abdominal tenderness and bloated abdomen were observed, arterial
blood pressure- 106/75 mmHg, pulse- 86 b/min. Blood tests showed leukocytosis (14.00 x 109/l),
hemoglobin of 125g/l, and hematocrit 32.8%, and alkalosis (pH 7.49, pCO221.3 mmHg, pO2 82.5
mmHg, HCO3 16.4 mmol/L, SBE -6.3 mmol/L). His INR (1.4) was slightly prolonged. During the
next few days his hemoglobin dropped to 109g/l, while the metabolic disorder and INR stabilized.
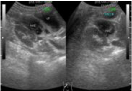
On admission an abdominal ultrasound (Figure 1) showed a solid mass, similar to a hematoma,
compressing the liver and associated to the duodenum. In fear of a perforated duodenum, a contrast
computer tomography (CT) was administered. Because of frequent vomiting, only intravenous
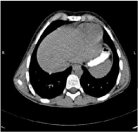
contrast was used. The CT (Figure 2) confirmed a nonhomogeneous, well circumcised oval
mass, filled with fluid, in the second part of the duodenum and local compression of the biliary
tract- consistent with the signs of an IDH. Since no signs of a perforation were observed during
the CT, conservative treatment, consisting of total parental nutrition, painkillers, proton pump
inhibitors and nasogastric suction, was chosen. Repeated abdominal ultrasounds, a CT and video endogastroduodenoscopy were used for the control of the hematoma.
Though there were signs of bowel obstruction, non operative
management was continued and the patient was discharged home
after 21days from the endoscopic biopsy.
Case 2
A 13 year old boy with history of graft versus host disease after
a bone marrow transplant due to meylodisplastic syndrome was
examined because of weight loss. Upper gastrointestinal endoscopy
was performed to determine the presence of chronic graft versus
host disease. Before the procedure the patient had slight anemia
(Hemoglobin- 115g/L) and thrombocytopenia (Platelet count-
58x109/L). The gastroduodenoscopy revealed erosive esophagitis,
varicosis of the esophageal veins, gastropathy and duodenogastric
reflux. Histological examination confirmed low activity graft versus
host disease of the gut.
Immediately after the procedure the patient presented with intense
abdominal pain and frequent vomiting. On physical examination the
patient had a compulsory position, diffuse abdominal tenderness. The
hemoglobin level had decreased to 92g/L, while amylase levels were
increased (3783.4 U/L).
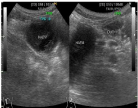
Suspecting acute pancreatitis an abdominal ultrasound was
ordered. It revealed a 70 by 50mm mass, resembling a hematoma by
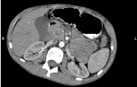
the duodenum with no oedema signs of the pancreas (Figure 3). A CT
(Figure 4) and upper endoscopy confirmed an intramural hematoma
in the second part of the duodenum.
Conservative management, consisting of intravenous fluids,
parenteral nutrition, antibiotics and painkillers, was chosen. After 13
days a resolution of the hematoma was observed and the patient was
transferred to the oncohematology ward for further treatment.
Figure 1
Figure 2
Figure 2
Abdominal CT revealing a nonhomogeneous, oval mass, filled with
fluid, in the second part of the duodenum- signs of an IDH.
Figure 3
Figure 4
Figure 5
Abdominal CT of the second patient revealing a hyperdense mass
by the second part of the duodenum.
Discussion
Even though the first case of IDH was reported in 1838, the
incidence of it is still unknown. IDH is usually a consequence of a
blunt abdominal trauma and predominant in children as mentioned
before. Guzman reports that endoscopic complications in children
present only in 2% of cases, and most are associated with the
anesthesia or bleeding and perforation [3]. The only 2 patients that
developed an IDH post endoscopy in our hospital are described here.
One of the mechanisms, thought to contribute to the development of
an IDH is the duodenum’s fixed retroperitoneal position and the rich
submucosal vascular plexus, which is prompt to bleeding [1,4]. Though
there are no proven risk factors for IDH after an endoscopic biopsy,
previously reported cases have been associated with malnuritment,
anticoagulant therapy [5], and post transplant patients. Some authors
report an IDH in patients with no previous medical history [6,7] such
as in our first clinical case. Our second case portrays the reported
association of an IDH in transplant patients [6,3]. J Ramakrishna et
al. [8] reports that IDH after endoscopic biopsy is usually the result
of thrombocytopenia and levels of over 50x109/L should be sustained
at least for 48 hours after the procedure. It should also be noted that
a study of 24 bone marrow transplants with suspicion of graft versus
host disease, showed that gastric antrum biopsies were more sensitive
for the diagnostics than biopsies from the duodenum or rectum [9].
In consideration this and of the risk factors of a developing IDH
for such patients, duodenal biopsies may not be necessary for the
diagnosis of graft versus host disease and should be performed only
with strong indications.
Because of its’ retroperitoneal position, any trauma to the
duodenum can present itself with unspecific symptoms. The most
common are reported to be abdominal pain and vomiting or
hematemesis usually within 48 hours of the trauma mechanism,
diffuse abdominal tenderness [1,2,6,7]. Laboratory findings are also
unspecific and are associated with such complications of an IDH as
pancreatitis and cholestasis. In our first case, the admission findings
showed only metabolic alkalosis, which was most likely due to the
patients vomiting. Later on, hemoglobin level fell slightly, but did not
require any blood transfusions. And as the obstruction of the biliary
tree by the hematoma progressed, total bilirubin levels elevated. The
second patient had decreased platelets and hemoglobin due to his
primary disease, after the biopsy he first presented with high amylase
levels, followed by increased pancytopenia and anemia.
Imaging techniques such as ultrasound, CT or magnetic
resonance imaging (MRI) [10,11] are used for diagnosing IDH. In
our first case, an upper gastrointestinal endoscopy was also used as
a diagnostic tool. Though not standardized, each one of the imaging
techniques has its own place in the diagnostics of an IDH. Ultrasound
is usually one of the first to be performed for a child presenting with
abdominal pain. D Antoniou et al. [10] reports that a nonperistaltic
hypoechogenic mass associated to the duodenum should give a big
suspicion of an IDH. However, it is hard to distinguish the hematoma
from a pancreas pseudocyst or abscess and ultrasound should not be
used as the only diagnostic test. Due to its low cost and safety for
the patient, it should be considered as one of the main tools for the
control of the hematoma during the course of treatment.
Computer tomography is one of the primary diagnostic tools of
a duodenal trauma [12], which can help differentiate an IDH from
a perforated duodenum and, thus, help determine the treatment
of choice. In a retrospective study, done by Jeffrey R et al. [11],
pneumoperitoneum and extravasation of contrast were found to be
associated with a duodenal perforation. However, KM Kassai et al
reported that in 5 children with a duodenal perforation, none showed
extravasation of contrast on their CT scans, while of the 14 with an
IDH no specific signs on a CT were seen at all, and they were diagnosed
either using an ultrasound or video endogastroduodenoscopy [13].
Literature indicates that conservative management should be of
choice for IDH. 16 of the 21 previously reported cases of and IDH in
pediatrics were treated in this manner. Nonoperative management
consists of nasogastric suction, no oral feeding, intravenous fluids,
and parenteral nutrition [1,7,12]. The resolution of a hematoma is
usually observed within 2-3 weeks.
Surgical treatment is to be preferred in the case of duodenal
perforation or no clinical improvement with conservative
management after 7-14days [1]. Percutaneous drainage of the
hematoma guided by CT [14] or ultrasound [15] can also be of
choice. J Y Lee et al. [16] described endoscopic decompression of
an IDH after unsuccessful conservative treatment. The patient, first
presented here, had total duodenal obstruction and, if conservative
management would not have been successful, endoscopic drainage of
the hematoma could have been considered as the treatment of choice.
Conclusion
There have been only a few cases as of yet of IDH after upper intestinal endoscopy biopsy. Though it is a rare complication, without appropriate treatment it can have lethal results, whereas a timely diagnosis can often lead to successful conservative management. That is why every patient, especially one with medical history of anticoagulation or immunosuppression, presenting with abdominal pain and vomiting after a video gastrointestinal endoscopic biopsy should be examined for an IDH. Ultrasound and CT are both adequate choices for the diagnostics of IDH, however CT is preferred for the primary diagnosis, where as ultrasound can be used as a safe technique to monitor the resolution of the hematoma. Nonoperative management should be preferred for stable patients with surgical treatment reserved for unstable patients and unsuccessful conservative treatment cases.
References
- Grasshof C, Wolf A, Neuwirth F, Posovszky C. Intramural duodenal haematoma after endoscopic biopsy: case report and review of the literature. Case Rep Gastroenterol. 2012; 6: 5-14.
- Ozcelik T, Hindilerden F, Hasbal B, Akyildiz M, Dayangac M, Killi R, et al. Intramural Duodenal Haematoma After Upper Gastrointestinal Endoscopic Biopsy in a Bone Marrow Transplant Recipient. Biology of Blood and Marrow Transplantation. 2013; 19: 302.
- Guzman C, Bousvaros A, Bounomo C, Nurko S. Intraduodenal hematoma complicating intestinal biopsy: case reports and review of the literature. Am J Gastroenterol. 1998; 93: 2547-2550.
- Diniz-Santos DR, de Andrade Cairo RC, Braga H, Araújo-Neto C, Paes IP, Silva LR. Duodenal hematoma following endoscopic duodenal biopsy: A case report and review of the literature. Can J Gastroenterol. 2006; 20: 39-42.
- Wang JY, Ma CJ, Tsai HL, Wu DC, Chen CY, Huang TJ, et al. Intramural duodenal hematoma and hemoperitoneum in anticoagulant therapy following upper gastrointestinal endoscopy. Med Princ Pract. 2006; 15: 453-455.
- Dunkin D, Benkov KJ, Rosenberg HK. Duodenal and rectal hematomas complicating endoscopic biopsies. J Ultrasound Med. 2009; 28: 1575-1580.
- Hoenisch K, Prommegger R, Schwaighofer H, Freund M, Schocke M, Vogel W, et al. Intramural duodenum hematoma after upper gastrointestinal endoscopy. Wien Med Wochenschr. 2011; 161: 441-444.
- Ramakrishna J, Treem WR. Duodenal hematoma as a complication of endoscopic biopsy in pediatric bone marrow transplant recpients. J Pediatr Gastroenterol Nutr. 1997; 25: 426-429.
- Cox GJ, Matsui SM, Lo RS, Hinds M, Bowden RA, Hackman RC, et al. Etiology and outcome of diarrhea after marrow transplantation: a prospective study. Gastroenterology. 1994; 107: 1398-1407.
- Antoniou D, Zarifi M, Gentimi F, Christopoulos-Geroulanos G. Sonographic diagnosis and monitoring of an intramural duodenal hematoma following upper endoscopic biopsy in a child. J Clin Ultrasound. 2009; 37: 534-538.
- Kunin JR, Korobkin M, Ellis JH, Francis IR, Kane NM, Siegel SE. Duodenal injuries caused by blukt abdominal trauma: value of CT in differentiating perforation from hematoma. Am J Roentgenol. 1993; 160: 1221–1223.
- AK Mansoor, J Garner, C Kelty. Management of duodenal injuries. Trauma. 2011; 14: 1-3.
- Desai KM, Dorward IG, Minkes RK, Dillon PA. Blunt duodenal injuries in children. J Trauma. 2003; 54: 640-645.
- Gullotto C, Paulson EK. CT-Guided Percutaneous Drainage of a Duodenal Hematoma. AJR Am J Roentgenol. 2005; 184: 231-233.
- Lloyd GM, Sutton CD, Marshall LJ, Jameson JS. Case of duodenal haematoma treated with ultrasound guided drainage. ANZ J Surg. 2004; 74: 500-501.
- Lee JY, Chung JS, Kim TH. Successful endoscopic decompression for intramural duodenal hematoma with gastric outlet obstruction complicating acute pancreatitis. Clin Endosc. 2012; 45: 202-204.