Case Report
Neonatal Mastitis and Breast Abscess due to Meticilin Resistant Staphylococcus Aureus
Juan Jesús Pérez-Guerrero1, Carlos Alberto Sánchez-Salguero2* and Branislava Grujic3
1Hospital Quirónsalud Campo de Gibraltar, Spain
2University Hospital of Puerto Real, Spain
3University Hospital Puerta del Mar, Spain
*Corresponding author: Carlos Alberto Sánchez-Salguero, University Hospital of Puerto Real, Carretera nacional IV, km 665, 11510, Puerto Real, Cádiz, Spain
Published: 31 Jan, 2017
Cite this article as: Pérez-Guerrero JJ, Sánchez-Salguero
CA, Grujic B. Neonatal Mastitis and
Breast Abscess due to Meticilin
Resistant Staphylococcus Aureus. Ann
Clin Case Rep. 2017; 2: 1253.
Abstract
Infection of breast tissue (mastitis) rarely occurs during neonatal period. It is mostly caused by
bacteria that colonize the skin: Staphylococcus Aureus is the most common identified cause of
mastitis.
Diagnosis is based on the medical history and physical examination. Its most frequent complication
is an abscess formation that may even require surgical intervention. There is no universal consensus
for the treatment, although all authors agree on the need for intravenous antibiotherapy.
We present the first published case of mastitis with breast abscess caused by Methicillin Resistant
Staphylococcus Aureus in a 15 day-old baby
Case Presentation
Female newborn of 15 days of age comes to emergency room presenting inflammation and
erythema of the right breast. Obstetric history: she was born at 40+3 gestational weeks by normal
birth. There was no history of risk for infection. APGAR was 9 and 10 at 1 and 5 minutes respectively.
Birth weight was 3190 grams. She was on exclusive brest-feeds and she presented good weight gain
with the actual weight of 3500 grams.
The mother describes 4 day history of inflammation and erythema of the right breast, which has
gotten worse even though she was applying cold packs locally. In the last 24h she started with the
white secretion through the nipple. Overall, she presented good well-being, she was afebrile and she
presented no irritability or lethargy. She maintained good appetite.
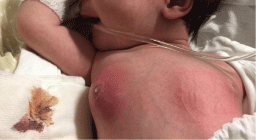
Physical exploration reveals inflamed right breast with local erythema, hot and firm, with no
central suppuration. On palpation there was 2 by 2 cm node that was inmovil and nonfluctuating
(Figure 1). The rest of the exploration was normal.
The complete blood work showed hemoglobin levels at 13 g/dl with hematocrit of 34%. White
blood count was 20700 (59.8% of neutrophils). Procalcitonin levels were 0.14 ng/ml and CRP was
5.4 mg/l. The rest of the complete blood work was normal. We solicited blood culture and culture
of the mammary excretion.
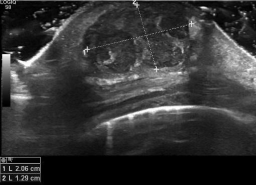
Echography was preformed that showed heterogeneous collection made primarely of
hipoecogenic area mixed with anecoic and other hiperecoic areas. Overall it was 1.4cm on
anterioposterior plane by 2cm on axial plane. It suggested edematous glandular tissue with abscessed
collection in its interior (Figure 2).
The pediatric surgeon was involved and decided to drain the abscess. Afterwards, the lesion was
covered with topic antibiotic and sterile dressing that was to be changed every 8 hours. Systemic
antibiotic therapy was suggested.
Evolution
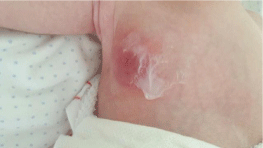
The patient was admitted and i.v. Amoxicilin with clavulonic acid was started. The dressing was changed every 8 hours with local application of Mupirocin. The culture came possitive to Meticilin Resistant Staphylococcus Aureus (MRSA) that was sensitive to Clindamycin. With this result the antibiotic was changed to Clindamycin. The baby presented good evolution and 48h after the change of antibiotic therapy the lesion was resolved, the local erythema and induration disappeared and local temperature was back to normal (Figure 3). There was no need for posterior drainage. There was no systemic affection at no time. She was sent home 72 h after admittance to continue with oral antibiotic therapy at home.
Figure 1
Figure 2
Figure 3
Discussion
Breast hypertrophy is a common finding in newborns (70%),
and it is due to maternal hormones. It is self-limited and at times
there can even appear milk with no pathological implication [1].
On occasion it can be complicated with infection of glandular tissue
(mastitis), usually provoked by Staphylococcus Aureus, although
several cases of infection with Streptococcus type B, enterococcus and
anaerobic Gram negative bacteria were described [1-6]. Up to our
best knowledge there are no infections caused by MRSA described
in pediatric population, although it was hypothesized as one of the
possible culprits [4]. It primarily occurs in female newborns 15 days
after birth (ratio female: male = 2:1) [1,3-7].
In the most of the cases there is only local infection and systemic
manifestation of the disease (poor appetite, fever, irritability etc.) are
rare [4-6]. Other systemic manifestations described are: osteomyelitis
[8], cerebral abscess [9] and necrotizing fasciitis [10]. Even though
our patient didn't have any systemic manifestations, the local
complication was suspected and later confirmed by echography. In
most of the cases, the in hospital care is suggested with iv antibiotic
therapy and previous blood culture as well as culture of the secretion
should be preformed [1-7]. If possible Gram staining should be
preformed [5] and echography to help differentiate the lesion. There
are no evidence about optimal antibiotic treatment [5,6] although
intravenous antibiotic therapy to cover Streptococcus Aureus is
recommended [1-4,7] with association of aminoglycoside antibiotic
if there is systemic affection [2-5]. The normal course of antibiotic
therapy is 10 to 14 days with oral therapy as soon as clinical findings
permits [1-4,6]. If there is poor evolution abscess should be suspected
and drained [3,4,7].
It is our firm belief that proper intravenous therapy along with
previous abscess drainage was the key to fast clinical improvement. It
is therefore important to look for the causing bacteria in the culture
while starting with empiric antibiotic therapy covering the usual
bacteria. Surgical drainage in cases of abscess is another important
part of the overall good medical treatment in the cases of abscessed
neonatal mastitis.
References
- Talat Masoodi, Gowhar Nazir Mufti, Javeed Iqbal Bhat, Rubina Lone, Syed Arshi, Syed Khurshid Ahmad. Neonatal Mastitis: A clinico- Microbiological study. J Neonatal Surg. 2014; 3: 2.
- Walsh M, McIntosh K. Neonatal mastitis. ClinPediatr (Phila).1986; 25: 395-399.
- Efrat M, Mogilner JG, Iujtman M, Eldemberg D, Kunin J, Eldar S. Neonatal mastitis-diagnosis and treatment. Isr J Med Sci. 1995; 31: 559-560.
- Stricker T, Navratil F, Sennhauser FH. Mastitis in early infancy. ActaPaediatr. 2005; 94: 166-169.
- Brett A, Goncalves S, Luz A, Martins D, Oliveira H, Januario L, et al. Neonatal mastitis: 12 years of experience [Article in Portuguese]. Acta Med Port. 2012; 25: 207-212.
- Nahar AL Ruwaili, Dennis Scolnik. Neonatal Mastitis: Controversies in Management. J Clin Neonatol. 2012; 1: 207-210.
- Stauffer WM, Kamat D. Neonatal mastitis. Pediatr Emerg Care. 2003; 19: 165-166.
- Michael IM, Howard FH. Osteomyelitis due to penicillin-resistant staphylococci in infancy following suppurative mastitis. J Trop Pediatr. 1960; 6: 19-21.
- Manzar S. Brain abscess following mastitis in a 3-month-old infant. J Trop Pediatr. 2001; 47: 248-249.
- Hsieh WS, Yang PH, Chao HC and Lai JY. Neonatal necrotizing fasciitis: a report of three cases and review of the literature. Pediatrics. 1999; 103: e53.