Clinical Image
Virtual Amputation in Diabetic Foot Infection with Osteomyelitis
Mohd Yazid Bajuri*
Department of Orthopedics, Universiti Kebangsaan Malaysia, Malaysia
*Corresponding author: Mohd Yazid Bajuri, Department of Orthopedics, Universiti Kebangsaan Malaysia, Kuala Lumpur, Malaysia
Published: 30 Jan, 2017
Cite this article as: Bajuri MY. Virtual Amputation
in Diabetic Foot Infection with
Osteomyelitis. Ann Clin Case Rep.
2017; 2: 1249.
Clinical Image
Osteomyelitis is a common complication and present in approximately 20% of diabetic foot
ulcer cases, and was reported as high as 79% in some other case series [1-3]. It is responsible for most
of the non-traumatic amputation of the lower limb [4].
Amputation of a digit in the foot causes a change in the biomechanics of the amputated limb.
This potentially creates higher pressure areas and new bony deformities that leads to another ulcer
and subsequently leads to amputation, especially with first ray amputation [5,6]. A study by Izumi
and associates found that there is an increased risk of reamputation of the same limb within 6
months after the initial amputation [7].
Diabetic foot infections have a spectrum of clinical presentation, varying in severity and this
present a great challenge in the management. There is difficulty in identifying the optimal treatment
for specific patient with different clinical presentation. The debates focus around the roles of
antibiotic therapy only, combined antibiotic therapy with limited debridement or a more radical
surgery such as amputation.
Aragón-Sánchez classified osteomyelitis in diabetic foot ulcer in order to guide the optimal
method of treatment [8]. His system comprised 4 classes of osteomyelitis that assess the presence of
ischemia and soft tissue involvement (Figure 1).
He observed 82.2% of total 94 patients who presented with infected diabetic foot ulcer, had
osteomyelitis. There was no amputation performed in class 1. However, 37.5% of class 2 (n=16), 82%
of class 3 (n=17), and all 23 patient in class 4 had amputation (Table 1). This confirmed the positive
correlation between presence of soft tissue involvement and ischemia with higher rate of amputation.
The findings also support the notion that presence of osteomyelitis does not necessitate amputation.
However, the weakness of this classification is that the presence of soft tissue involvement can only
be confirmed intraoperatively.
Virtual amputation falls under the category of conservative surgery. It is defined as any procedure
in which bone and non-viable soft tissue are removed without amputation of any part of the foot
is undertaken [2,8]. The procedure is aimed at preserving the physical appearance of foot while removing the infection load (Figure 2). This is coupled with antibiotic
therapy to achieve remission in infection. The antibiotic duration
should be tailored according to wound condition and culture with
infective markers as guidance to predict remission of acute infection
(Figure 3).
The end result is minimal disruption in the biomechanics of
the foot, therefore avoiding the creation of another high-pressure
point within the same foot, which in turn creates another ulcer.
Furthermore, the psychological effect on patient is greater in a positive
way as patient is able to keep the normal appearance of the foot.
Proper wound care and bandaging while waiting for the wound
to heal in a normal axis following the other toes. A proper “guided
healing” of the virtually amputated toe should be in line of the
management plan to maximize the benefit of this procedure.
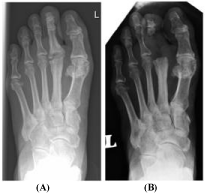
Figure 1
Figure 1
Radiograph of the left foot – evidence of osteomyelitis of proximal phalanx second toe and distal end
of the second metatarsal bone.
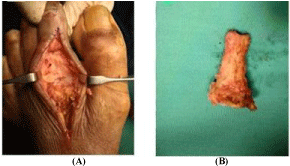
Figure 2
Figure 2
(A) The wound bed after removal of proximal phalanx and head of
second metatarsal bone. (B) proximal phalanx of the toe.
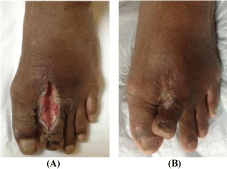
Figure 3
References
- Iannuzzi MC, Rybicki BA, Teirstein AS. Sarcoidosis. N Engl J Med. 2007; 357: 2153-2165.
- Kruger S, Buck AK, Mottaghy FM, Pauls S, Schelzig H, Hombach V, et al. Use of integrated FDG-PET/CT in sarcoidosis. Clin Imaging. 2008; 32: 269-273.
- Aksoy SY, Ozdemir E, Senturk A, Seyda Türkölmez. A case of sarcoidosis diagnosed by positron emission tomography/computed tomography. Indian J Nucl Med. 2016; 31: 198-200.
- Teirstein AS, Machac J, Almeida O, Lu P, Padilla ML, Iannuzzi MC. Results of 188 whole-body fluorodeoxyglucose positron emission tomography scans in 137 patients with sarcoidosis. Chest. 2007; 132: 1949-1953.
- Nishiyama Y, Yamamoto Y, Fukunaga K, Takinami H, Iwado Y, Satoh K, et al. Comparative evaluation of 18F-FDG PET and 67Ga scintigraphy in patients with sarcoidosis. J Nucl Med. 2006; 47: 1571-1576.
- Sulavik SB, Spencer RP, Weed DA, Shapiro HR, Shiue ST, Castriotta RJ. Recognition of distinctive patterns of gallium-67 distribution in sarcoidosis. J Nucl Med. 1990; 31: 1909-1914.
- Statement on sarcoidosis. Joint Statement of the American Thoracic Society (ATS), the European Respiratory Society (ERS) and the World Association of Sarcoidosis and Other Granulomatous Disorders (WASOG) adopted by the ATS Board of Directors and by the ERS Executive Committee, February 1999. Am J Respir Crit Care Med. 1999; 160: 736-755.
- Oksuz MO, Werner MK, Aschoff P, Pfannenberg C. 18F-FDG PET/CT for the diagnosis of sarcoidosis in a patient with bilateral inflammatory involvement of the parotid and lacrimal glands (panda sign) and bilateral hilar and mediastinal lymphadenopathy (lambda sign). Eur J Nucl Med Mol Imaging. 2011; 38: 603.
- Braun JJ, Kessler R, Constantinesco A, Imperiale A. 18F-FDG PET/CT in sarcoidosis management: review and report of 20 cases. Eur J Nucl Med Mol Imaging. 2008; 35: 1537-1543.
- Treglia G, Annunziata S, Sobic-Saranovic D, Bertagna F, Caldarella C, Giovanella L, et al. The role of 18F-FDG-PET and PET/CT in patients with sarcoidosis: an updated evidence-based review. Acad Radiol. 2014; 21: 675-684.