Clinical Image
Are we Missing Hypothyroidism in Sickle Cell Disease?
Likhona S Masika, Mathew Hsieh, Zhen Zhao, Xiaolin Yu and Steven J Soldin*
Department of Laboratory Medicine, National Institutes of Health Clinical Center, USA
*Corresponding author: Steven J Soldin, Department of Laboratory Medicine, Clinical Center, NIH, Bethesda MD, USA
Published: 27 Jan, 2017
Cite this article as: Masika LS, Hsieh M, Zhao Z,
Yu X, Soldin SJ. Are we Missing
Hypothyroidism in Sickle Cell Disease?.
Ann Clin Case Rep. 2017; 2: 1246.
Clinical Image
Sickle Cell Disease (SCD) is a group of inherited hemoglobin disorders caused by a structurally
abnormal variant of hemoglobin that is related to abnormal β-globulin genes [1,2]. This disorder
affects about 1 out of every 600 African Americans and up to 3% of births in sub-Saharan Africa.
Phillips et al. [1] described three cases of hypothyroidism in patients with SCD. The etiology of
hypothyroidism in SCD is not clear but may be related to iron overload from multiple blood
transfusions.
The prevalence of hypothyroidism in SCD is also unknown. The aim of our study was to evaluate
the prevalence of hypothyroidism in SCD and determine how its diagnosis may be missed due to
unreliable immunoassay (IA) methods for the measurement for thyroid hormones.
Van Deventer et al. [3] and Jonklaas et al. [4] have demonstrated how poorly IA methods for
thyroid hormone measurement correlate with TSH. Moreover, Masika et al. [5] have shown that the
measurement of total T3 (TT3) by IA at low concentrations is unreliable and may miss about 50%
of patients with elevated TSH’s and low TT3’s.
We assessed 73 randomly selected patients with SCD, 17 of them (prevalence of 23.3%)
having elevated TSH’s (>4.20 uIU/mL with a mean and median of 8.88 uIU/mL and 5.25 uIU/mL
respectively. Our reference interval for TSH is 0.27 – 4.20 uIU/mL). Previously the prevalence of
hypothyroidism in SCD was never documented.
Reliable laboratory evaluation of thyroid in SCD becomes even more important as in these
patients the symptoms of hypothyroidism may not be obvious. For example in the case of cold
intolerance it is of interest to note that most SCD patients avoid cold temperatures because this can
precipitate a crisis. With constipation, another symptom of hypothyroidism we have discovered
that many SCD patients take stool softeners as they are on narcotics. Depression another symptom
is again hidden as many SCD patients take anti-depressants for pain control reasons. The clinical
laboratory therefore plays a central role in diagnosis by measuring thyroid hormones accurately and
precisely by isotope dilution LC-MS/MS.
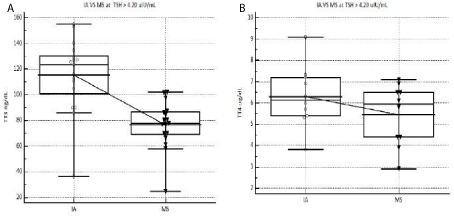
Our results showed that in SCD patients with significantly elevated TSH’s 10% of IA vs. 70%
of LC-MS/MS TT3’s were below the 2.5th percentile (Figure 1A). For total T4 (TT4) measurements
14.3% of IA’s and 43% of LCMSMS results were below the 2.5th percentile (Figure 1B). It is worth
emphasizing that it is T3 that binds avidly to the nuclear receptor and not T4 [5]. Using TT3 and/
or TT4, IA concurred with the elevated TSH’s 11% of the time while MS concurred 72% of the time.
This emphasizes how unreliable IA is in thyroid diagnosis in SCD
and how it may cause physicians to miss patients with low thyroid
hormones. The lack of correlation of the IA’s for TT3 and TT4with
TSH may explain why historically very few cases of hypothyroidism
have been recognized in patients with SCD.
This is a preliminary study and needs to be confirmed in a larger
cohort of patients. Furthermore there is a future need to study the
pathogenesis of hypothyroidism in SCD. Clearly LC-MS/MS will
play an important role in highlighting the true prevalence and
pathogenesis of hypothyroidism in the SCD population.
In conclusion we recommend that SCD patients with elevated
TSH’s have their thyroid hormone measurements performed with
reliable methods such as LC-MS/MS, thereby allowing physicians to
evaluate whether thyroid hormone replacement therapy needs to be
implemented.
Figure 1
Figure 1
(A) IA vs. MS on TT3 at high TSH’s, (B) IA vs. MS on TT4 at high TSH’s. The grey dotted lines show
the lower cutoffs. RI = Reference Interval.
References
- Phillips G Jr, Becker B, Keller VA, Hartman J. Hypothyroidism in Adults with Sickle Cell Anemia. Am J Med. 1992; 92: 567-570.
- Cecchini J, Fartoukh M. Sickle cell disease in ICU. Curr Opin Crit Care. 2015; 21: 569-575.
- Van Deventer HE, Soldin SJ. The expanding role of tandem mass spectrometry in optimizing diagnosis and treatment of thyroid disease. Adv Clin Chem. 2013; 61: 127-152.
- Jonklaas J, Davidson B, Bhagat S, Soldin SJ. Triiodothyronine levels in athyreotic individuals during levothyroxine therapy. JAMA. 2008; 299: 769-777.
- Masika LS, Zhao Z, Soldin SJ. Is measurement of TT3 by immunoassay reliable at low concentrations? A comparison of the Roche Cobas 6000 vs. LC-MSMS. Clin Biochem. 2016; 49: 846-849.