Case Report
Primary Chest Wall Hydatid Cyst, Case Report & Review of Literature
Fitsum Argaw, Engida Abebe* and Ayelign Tsehay
Department of Surgery, SPHMMC, Ethiopia
*Corresponding author: Engida Abebe, Department of Surgery, SPHMMC, Addis Ababa, Ethiopia
Published: 27 Jan, 2017
Cite this article as: Argaw F, Abebe E, Tsehay A. Primary
Chest Wall Hydatid Cyst, Case Report
& Review of Literature. Ann Clin Case
Rep. 2017; 2: 1245.
Abstract
Chest wall cysts in general are uncommon. Among the pathologic processes that may involve the chest wall includes congenital/developmental, post-traumatic, post-treatment (surgery, radiotherapy etc.), infectious/inflammatory (e.g. tuberculosis) and neoplastic. The Chest wall is an unusual location for primary Echinococcus disease. We report a case of primary chest wall Hydatid Cyst (HC) in a 36-year-old woman who presented with left chest wall mass.
Keywords: H. cyst; Chest wall; E. granulosus
Introduction
Hydatid disease has been a well-known entity since the era of Hippocrates. There are more than
six species but three species of the tapeworm are of clinical importance in human hydatid disease;
Echinococcus granulosus, Echinococcus multilocularis and Echinococcus vogeli. The most common
causative organism for hydatid disease and the only one that cause HC is E. granulosus [1-3].
E. granulosus is distributed throughout the world. The infestation is common in sheep-farming
areas of Greece, Turkey, the Middle East, Australasia, Sub-Saharan Africa, parts of America, and India
[1-3]. The disease is also endemic in Ethiopia. Studies conducted at west & east part of the country
showed high overall prevalence of hydatidosis in Ethiopia which indicates that HC is among most
common infestations in the country [6-8]. Dog is the primary host while sheep is an intermediate
host. Humans are only accidental hosts and do not play part in the life cycle of the parasite. Humans
may contract the infection either by direct contact with a dog or by ingestion of foods or fluids
contaminated by the eggs, which are contained in the feces of the dog. After ingestion, the eggs are
freed from their coating and larva penetrate the mucosa of the jejunum reaching through the venous
and lymphatic channels to every region of the body where they transform into small cysts which
gradually enlarge [9].
HC can affect any age group and in any part of the body, except the hair and nails [10]. HC
mostly affects the liver (75%) and lung (15%). It occurs in only 10% cases in other regions of the
body. Skeletal muscle or subcutaneous tissue involvement by primary HC is uncommon and
represents 0.5-4% of patients [1-3,9]. Primary chest wall hydatidosis is very rare, even in countries
where echinococcosis is endemic & its diagnosis is easily missed because of its unusual presentation
unless be kept in mind. We report a case of primary chest wall HC that was misdiagnosed as benign
chest wall mass.
Case Presentation
A 36-years old housewife from rural part of Ethiopia presented to our hospital with the
compliant of left anterior upper chest wall swelling of 2years duration. The swelling was slowly
progressing with associated dragging pain. She had contact with dogs and cats at home. She had
no history of similar illness in the past. She had no cough or chest pain. Physical exam revealed an
eight by six centimeter cystic, non-tender mass over the left infraclavicular area which is mobile (not
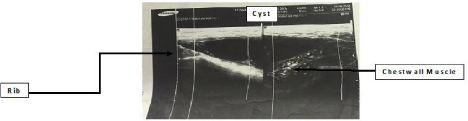
fixed to the skin or underlying structure). She was investigated with Ultrasound of the left chest wall
which showed left anterior chest infraclavicular subcutaneous hypoechoic mass & concluded as left
anterior chest subcutaneous cystic mass (Figure 1). Fine Needle Aspiration(FNA) diagnosis index
was left upper chest wall lymphangioma. Complete blood count was normal excisional biopsy was decided with the diagnosis of benign chest wall mass and patient was
prepared. Under general anesthesia the mass was explored through transverse incision following
the skin crease & cystic mass was found subcutaneously which was excised completely & there was no leak. After completion, the cyst was opened & revealed multiple
daughter cysts with the characteristic germinal layers and ectocyst.
With a clinical diagnosis of subcutaneous chest wall HC specimen was
sent for histopathology and confirmed the diagnosis (Figure 2). In the
post op period she was worked up for possible other site involvement
with abdominal US and chest x-ray which were non revealing.
Patient’s postoperative course was uneventful. She was started
on Albendazole & discharged on the firsts post op day. In the next 6
months She was seen 3 times on follow up and had smooth course &
showed no signs of recurrence.
Figure 1
Figure 2
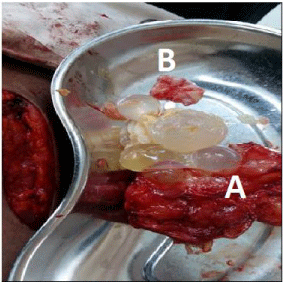
Figure 2
The operation site with opened cyst which revealed the daughter
cysts (arrow) with their characteristic pericyst (A) & germinal layers (B).
Discussion
HC is caused by larval cestodes of the tapeworm E. Granulosus
which results from haematogenic or lymphatic invasion of the body.
The final localization of Echinococcus depends on anatomical and
physiological characteristics of the host, as well as the species and
strain of parasite. Ribs, sternum, or soft tissues of the thoracic wall
may become a locus. Only a few cases of chest wall HC are reported
in literature [1,2,5,8].
Two possible mechanism of primary hydatid cyst of the chest
wall are mentioned on literatures. The first one is when the embryo
passes through the duodenal wall into either the portal vein or the
periduedonal and perigastric lymphatics which connect with the
thoraco-mediastinal lymphatic and the thoracic duct and the second
one when an intrathoracic extrapulmonary hydatid cyst lies in a
neighborhood of bone structures it may result in bone destruction
and chest wall involvement [10-12]. The former mechanism may
explain the development of primary chest wall hydatid disease in our
patient because of the absence of pulmonary or hepatic cysts.
Radiologic diagnostic techniques, dermal test, complementary
fixation test and indirect hemagglutination test can be used for
diagnostic purposes. The most reliable of these techniques is the
radiologic diagnostic tests [4,5,9]. In our patient, US was done
though it was not diagnostic because HC was not considered in the
differentials. FNA is a controversial area in patients suspected to have
HC due to the potential risk of anaphylactic shock [6,10]. In our
patient FNA was done because HC was not considered, unfortunately
the result was inconclusive. Definitive diagnosis in the presented
patient was not possible based on preoperative clinical examination
and radiological investigations. We confirmed diagnosis only by
surgical exploration and histopathology examination.
This case and other case reports are good evidences to consider
hydatid cyst in the differential diagnosis of any cystic mass in any part
of the body especially in the endemic areas [1,3,6,10].
A 7.4% incidence of Intrathoracic extrapulmonary localization of
thoracic cysts was reported. Among these, 14% were in the chest wall.
Primary HC can be seen in the musculoskeletal system in 1–4% cases
& chest wall involvement constitutes only 6% of them [1,2,9].
Kavukcu et al. [3] reported 7 chest wall HC in 1,032 patients
who were operated for pulmonary hydatid disease. There is only one
chest wall involvement in the report of 842 hydatid cysts in the series
of Qian. What makes our patient different is there was no evidence
of pulmonary or intrathoracic HC. The cyst was completely in the
subcutaneous tissue with no rib involvement.
The gold standard in the therapy of this disease is the radical
resection of cyst and involved ribs [6,8,10]. In our patient we
removed all parts of the cyst but no rib was involved. It has been
suggested that better results would be achieved by combining
surgery and chemotherapy (Albendazole) for pre and postoperative
prophylaxis. Large doses of Albendazole over a long period of time
(3-6months) would be a good clinical approach and may reduce
the incidence of relapse whether the cyst is completely removed
or not because of the possibilities of micro perforations [1,2,6-11].
Albendazole and mebendazole are the only antihelminthic drugs that
are effective against cystic echinococcosis. Albendazole is the drug
of choice against HC because its degree of systemic absorption and
penetration into the cysts is superior to that of mebendazole. In our
case the diagnosis was made intraoperatively & we put our patient on
albendazole 800 mg/day for 3 months as postoperative prophylaxis
and she has no sign of recurrence.
Conclusion
HC should be considered in the work up of all patients presented with chest wall cystic mass especially in endemic areas.
References
- Alper F, Dalokay K, Tuba C, Ahmet H. Primary Hydatid Disease of the Chest Wall. Ann Thorac Cardiovasc Surg. 2007; 13: 203-205.
- Oguzkaya F, Akcali A, Kahraman C, Emiroğullari N, Bilgin M, Sahin A. Unusually located hydatid cysts: intrathoracic but extrapulmonary. Ann Thorac Surg. 1997; 64: 334-337.
- Kavukcu S, Kilic D, Tokat AO, Kutlay H, Cangir AK, Enon S, et al. Parenchyma preserving surgery in the management of pulmonary hydatid cysts. J Invest Surg. 2006; 19: 61-68.
- Ozcelik C, Inci I, Toprak M, Eren N, Ozgen G, Yasar T. Surgical treatment of pulmonary hydatidosis in children: experience in 92 patients. J Pediatr Surg. 1994; 29: 392-395.
- Ayuso LA, Peralta GT, Lazaro RB, Stein AJ, Sanchez JA, Aymerich DF. Surgical treatment of pulmonary hydatidosis. J Thorac Cardiovasc Surg. 1981; 82: 569-575.
- Engida A, Ayelign T. Hydatid Cyst Disease in The Left Lateral Neck: An Uncommon Presentation. Ethiop Med J. 2016; 54: 3.
- Nebyou M, Adugna D. Prevalence, cyst variability, organ distributions and financial losses due to hydatidosis in cattle slaughtered at Nekemte abattoir in western Ethiopia. J Vet Med Anim Health. 2014; 6: 280-288.
- Miheret M, Biruk M, Habtamu T, Ashwani. Bovine Hydatidosis in Eastern Part of Ethiopia. MEJS.2013; 5: 107-114.
- Aghajanzadeh M, Alavi CE, Asgary MR, Rimaz S, Massahnia S. Primary Hydatid Cyst of the Rib: Present as a Chest Wall Mass. MOJ Surg. 2016.
- Qassim F, Munther I. Surgical considerations in hydatid disease: Clinical Surgery a practical guide. 2009; 376-389.
- Karaoglanoglu N, Gorguner M, Eroglu A. Hydatid disease of the rib. Ann Thorac Surg. 2001; 71: 372-373.
- Di Gesu G, Massaro M, Picone A, La Bianca A. Fiasconaro G Bone echinococcosis. Minerva Medica.1987; 78: 921-931.