Case Report
Transient Osteoporosis of the Hip in a Non-Pregnant Woman: Rapid Recovery after the Treatment with Intravenous Biphosphonates
Axel Finckh1* and Charna Dibner2
1Department of Specialties of Medicine, University Hospital of Geneva, Switzerland
2Department of Cellular Physiology and Metabolism, University of Geneva, Switzerland
*Corresponding author: Axel Finckh, Department of Specialties of Medicine, University Hospital of Geneva, 26 Ave Beau-Sejour, 1211 Geneva 14, Switzerland
Published: 13 Jan, 2017
Cite this article as: Finckh A, Dibner C. Transient
Osteoporosis of the Hip in a Non-
Pregnant Woman: Rapid Recovery
after the Treatment with Intravenous
Biphosphonates. Ann Clin Case Rep.
2017; 2: 1233.
Abstract
Transient osteoporosis of the hip is an infrequent, self-limiting condition presenting as gradually increasing hip pain, leading to walking disability. The disease mostly affects middle-aged men and women in their late pregnancy. We report a case of a 45-year-old woman diagnosed with transient osteoporosis of the hip (TOH), without any commonly reported risk factors such as pregnancy, chronic diseases, or traumatic events. Administration of a single infusion of a last generation of bisphosphonates (zoledronic acid), along with limited weight bearing and daily exercises, resulted in a complete clinical recovery within 3 months. Neither anti-inflammatory medication nor physiotherapy was needed. We conclude that intravenous bisphosphonates may be effective in TOH and potentially useful in the rare occurrence of this condition in non-pregnant women.
Keywords: Biphosphonates; Transient osteoporosis of the hip
Introduction
Transient osteoporosis of the hip (TOH) is a rare idiopathic disorder characterized by acute onset of hip pain leading to walking impairment [1]. Initial characterization of the disease dates back to 1959, first observed in pregnant women [2]. While the disease is more common in middle-aged men, in women TOH has been mostly commonly diagnosed during the last trimester of pregnancy or immediately following delivery [3]. The most common location is the hip joint, although occasional cases have also been described in the knee, the ankle or the foot bones. Magnetic resonance imaging (MRI) currently represents the most sensitive test for the initial diagnosis and for monitoring the evolution [1,4]. The disease is generally self-limited, with complete disappearance of symptoms occurring typically within 6-18 months after onset [5,6]. The etiology of the disease is currently largely unknown, but hypotheses suggest a potential role of pelvic nerve compression during late pregnancy or neuro-inflammatory mechanisms [6,7].
Case Presentation
A middle aged (45-years-old) non-pregnant female patient complained of gradually increasing mild to very severe pain in the left inguinal area over a period of 3 weeks, which led to nearly complete walking disability at her first consultation. No particular injury or other event preceded the development of her symptoms. An articular ultrasound and a hip radiography were normal, as were extensive blood tests. In particular, no inflammation, no auto-antibodies and no abnormality in phospho-calcic metabolism were found. A MRI scan was performed because of the severity of her symptoms, which revealed increased signal intensity on T2 and STIR weighted images, and a decreased intensity on T1 weighted images. The diffuse bone marrow oedema pattern signal in the absence of osteonecrosis or fractures was strongly suggestive of transient osteoporosis of the hip (Figure 1A). A single iv infusion of zoledronic acid (5 mg) was administered, associated with weight discharge of her left lower limb and daily exercises to prevent muscle wasting. Neither nonsteroidal anti-inflammatory drugs, nor physiotherapy were required during follow-up. Relatively rapid clinical recovery was observed, with a complete disappearance of the hip pain at three months and a complete resuming of her usual physical activities. At six months, the patient fully recovered the normal range of motion of the left hip. In agreement with the clinical examination, a control MRI confirmed the disappearance of any pathological signs in the left hip (Figure 1B). The patient remained symptom-free at a 12 months’ follow-up visit, with a normal control MRI (Figure 1C).
Figure 1
Figure 1
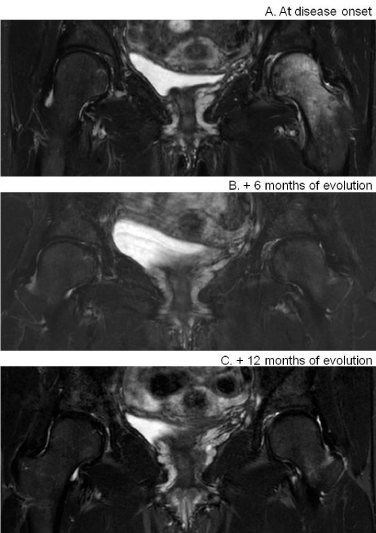
MRI images of both hips (A) at the disease onset, (B) at 6 months
and (C) at one year Images in coronal plane, Gadolinium injected, T2-
STIR sequence of both hips. (A) Signal abnormality of the left femur, with
hyper-intense signals observed at the disease onset. (B)Disappearance of
the signal abnormality at 6 months following the onset (C) confirmed at 12
months.
Discussion
TOH in non-pregnant women
TOH is a self-limiting disease with usually a complete recovery
after 6-18 months, according to the available literature. Although
the overall prognosis is good in vast majority of the cases, it has a
considerable impact on patient’s quality of life during the initial phase
due to functional disability and fear of fracture [3,8,9]. The majority
of TOH cases have been described in healthy middle-aged (40-70
y.o.) men. The remaining case reports (approximately one-third of
the cases) are reported in pregnant women, in their third trimester of
pregnancy or immediately after delivery [3,6,10]. Only two cases of
TOH in non-pregnant women have been described in the literature,
to the best of our knowledge [11,12]. Here we report an additional
case of TOH diagnosis in a 45-year old non-pregnant woman,
supporting the observation that while this disease is undoubtedly
associated with late pregnancy and postpartum in women, it is not
limited to pregnancies. It is thus important to consider the possibility
of incident TOH in non-pregnant women, when confronted with
acute hip symptoms, even though the incidence of TOH appears to be
low in non-pregnant women. The differential diagnosis of TOH are
the early stages of a vascular necrosis of the hip (AVN), which is also
characterized by bone marrow edema, and primary and metastatic
malignancies [1,13], which are however usually associated with other
concomitant symptoms and distinct risk factors.
The etiology of TOH development remains unclear so far. Neuroinflammatory
mechanisms along with type IV hyperlipidemia have
been postulated to play a role [7]. In the case of late pregnancy and postpartum, the disease might be related to the compression of the
obturator and pelvic nerves and vessels. Parathyroid hormone-related
protein has also been proposed to play a role in TOH development
during pregnancy [6]. With respect to TOH in non-pregnant women,
further elucidation of possible diseases mechanisms, unrelated to
pregnancy, are warranted.
Successful treatment with single injection of
bisphosphonates as compared to repetitive injections
Proposed management of TOH comprises weight discharge,
non-steroidal anti-inflammatory drugs and calcitonin. During the
last decade intravenous bisphosphonate treatment have been applied
and suggested to be successful in a number of reports ([14] and
references therein). Authors have proposed multiple injections of 300
mg of clodronate during 10 days, along with calcium and vitamin D
supplements, followed by second course of 5 injections of clodronate,
with considerable clinical improvement within two months. Dr. Seok
and colleagues report one successful use of intravenous zoledronate
[15]. Hereby we report rapid improvement of symptoms (pain relief
and ability to walk) and complete recovery within three months
following single intravenous infusion of zoledronate (5 mg), without
requiring other analgesic therapies or NSAIDs.
Conclusion
A treatment with a single-dose of the iv bisphosphonates (zoledronate) appeared to be effective in reducing the time to recovery in this unusual case of TOH in a non-pregnant female, in association with conservative measures. We conclude that zoledronic acid might be a safe alternative for the treatment of TOH in nonpregnant patients.
Acknowledgements
The authors thank Dr. Nodar Buchukuri (Department of Orthopedic and Trauma Surgery, Thüringen Klinik “Georgius Agricola”, Saalfeld, Germany) and Dr. David Tchernin (Department of Radiology, La Tour Hospital, Geneva, Switzerland) for the help with the diagnosis, and Prof. Christian Jorgensen (Director of IRMB Institute de Recherche de Médecine Régénératrice et de Biothérapies, INSERM, Montpellier, France) for advice on possible treatment strategies.
References
- Gallucci GL, Pacher N, Boretto JG, De Carli P. Bilateral rupture of the extensor pollicis longus tendon. A case report. Chir Main. 2013; 32: 186- 188.
- Anwar I, Owers KL, Eckersley R. Spontaneous rupture of the extensor pollicis longus tendon. J Hand Surg Br. 2006; 31: 457-458.
- Mills SP, Charalambous CP, Hayton MJ. Bilateral rupture of the extensor pollicis longus tendon in a professional goalkeeper following steroid injections for extensor tenosynovitis. Hand Surg. 2009; 14: 135-137.
- Roth KM, Blazar PE, Earp BE, Han R, Leung A. Incidence of extensor pollicis longus tendon rupture after nondisplaced distal radius fractures. J Hand Surg. 2012; 37: 942-947.
- Haher JN, Haher TR, Devlin VJ, Armenti V. Bilateral rupture of extensor pollicis longus. A case report. Orthopedics. 1987; 10: 1577-1580.
- Payne AJ, Harris NJ, Kehoe NJ. Bilateral delayed extensor pollicis longus rupture following bilateral undisplaced distal radial fractures. Orthopedics. 2000; 23: 163.
- Jung SW, Kim CK, Ahn BW, Kim DH, Kang SH, Kang SS. Standard versus over- tensioning in the transfer of extensor indicis proprius to extensor pollicis longus for chronic rupture of the thumb extensor. J Plast Reconstr Aesthet Surg. 2014; 67: 979-985.
- Schaller P, Baer W, Carl HD. Extensor indicis transfer compared with palmaris longus transplantation in reconstruction of extensor pollicis longus tendon: a retrospective study. Scand J Plast Reconstr Surg Hand Surg. 2007; 41: 33-35.
- Shah MA, Buford WL, Vieges SF. Effects of extensor pollicis longus transposition and extensor indicis proprius transfer to extensor pollicis longus on thumb mechanics. J Hand Surg. 2003; 28: 661-668.
- Germann G, Wagner H, Blome-Eberwein S, Karle B, Wittemann M. Early dynamic motion versus postoperative immobilization in patients with extensor indicis proprius transfer to restore thumb extension: a prospective randomized study. J Hand Surg Am. 2001; 26: 1111-1115.