Case Report
Scrotal Melanoma with Brain and Lung Metastasis
Rodrigo Beserra Sousa*, Marcos Francisco Dall’Oglio, Gabriel Barbosa Franco, Mikael Vieira
da Silva, Hermano Covre Argolo, Cassius Martins e Silva and Luiz Jorge Budib
Department of Urology, Santa Marcelina Hospital, Brazil
*Corresponding author: Rodrigo Beserra Sousa, Department of Urology, Rua Santa Marcelina, 177, Itaquera, São Paulo/SP, Brasil, 2º Andar (Chefia da Urologia) CEP 08270-070, Brazil
Published: 06 Jan, 2017
Cite this article as: Sousa RB, Dall’Oglio MF, Franco GB,
da Silva MV, Argolo HC, e Silva CM,
et al. Scrotal Melanoma with Brain and
Lung Metastasis. Ann Clin Case Rep.
2017; 2: 1229.
Abstract
We describe a case of a patient diagnosed with melanoma complications due to cerebral metastatic lesion and at a later investigation diagnosed primary lesion in the scrotum.
Keywords: Scrotalmelanoma; Metastatic melanoma; Orchiectomy; Scrotum; Scrotectomy
Introduction
Primary melanoma of the genitourinary system occurs in less than 1% of all cases, with the
scrotal location having only 17 cases described in the literature. Cases diagnosed in the initial phase
of the disease presented a more favourable prognosis [1].
In a revision study upon penile and urethral melanoma, 57 cases of penile melanoma and 26
of urethral location were revised [2]. In another case series, the files of 16 men with a diagnosis of
melanoma were revised, with 9 cases in the penile location, one in the urethra and 6 in the scrotum;
half of these last were diagnosed incidentally after a local trauma and one was related to a pigmented
scrotal lesion which had been perceptible for the previous 5 months [3].
Taking into account the rarity of the primary scrotal melanoma, the object of this case study is
to show the aggressive and rapid evolution of a melanoma in the scrotum, diagnosed at advanced
stage.
Case Presentation
Male, 76 years old, with history of systemic arterial hypertension, chronic angina and alcohol
consumption, complaining of left hemiplegia and sudden loss of consciousness. A secondary,
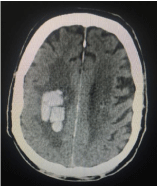
haemorrhagic, cephalic, vascular accident was diagnosed, together with a parietal tumour on right
side (Figure 1). The patient was submitted to drainage of the haematoma with biopsy of the lesion,
which was suggestive of malignant melanoma after immunohistochemical analysis.
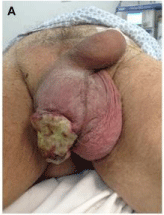
There was a lesion in the right scrotal sack which had begun 2 years previously, with no medical
attendance during this period (Figure 2). Upon physical examination, an ulcerated lesion of around
6 cm was found in the right scrotum with apparent infiltration of the testicle as well as two palpable
nodules in the right, ipsilateral, inguinal region.
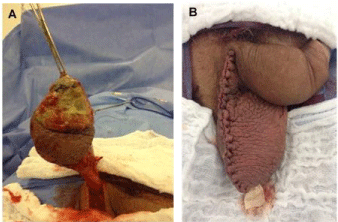
He was submitted to a right orchiectomy with partial resection of the scrotum (Figure 3). The
result of this under anathomo pathological analysis, with immunohistochemical profile of markers Melan-A, HMB-45 and diffuse S-100 protein positives, together with
KI-67 in 80% of the cells, was compatible with scrotal melanoma.
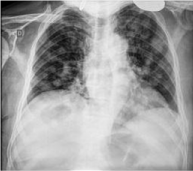
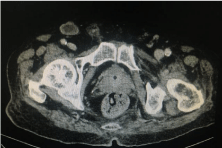
Staging tests with computerized tomography of the thorax,
abdomen and pelvis showed multiple nodular pulmonary lesions,
without apparent metastases into abdominal regions, but inguinal
lymph node enlargement (Figures 4 and 5).
Palliative radiotherapy was indicated for the cerebral tumour
nodule, effected with 2000 Gy, but total intended dose was not
completed due to deterioration of general clinical condition. In this
same month, there was a new episode of intracranial haemorrhage due
to growth of the tumour, with re-admittance, evolving to intracranial
hypertension and obit.
Figure 1
Figure 2
Figure 3
Figure 3
Hemi-scrotectomy and right radical Orchiectomy surgery
with primary reconstruction of testicular sac.
Figure 4
Figure 4
Radiograph in a stillborn infant. Showing extremely short femora
and humeri with flares and cupped metaphyses. (a) frontal view (b) lateral
view.
Figure 5
Discussion
Genitourinary melanoma is rare and scrotal melanoma is the
rarest reported. Penile lesions of old, well defined aspect and single
colour are less suspect for melanoma, but should be examined with
frequency and any suspicious alteration must be correctly biopsied
and monitored [4].
Currently available information reveals that, although the
genitourinary melanoma is an aggressive disease, it is potentially
curable if the pathological characteristics and clinical presentation
are favourable [5]. Within a series of 11 cases of scrotal melanoma,
it was observed that patients submitted to ascrotum resection alone
presented an effective local control, but were at higher risk for
locoregional recurrence [3].
The handling and treatment of the inguinal region in cases of
genitourinary melanoma without palpable lymph nodes is debatable
[6]. In these cases, the indication for inguinal, surgical staging
is based on the site of the tumour and pathological, prognostic
factors such as the thickness of Breslow, Clark level and presence
of tumour ulceration [7]. When lymph nodes are clinically absent,
the recommendation for prophylactic, inguinal lymphadenectomy
would be for melanomas with an invasive depth of 1 mm or over,
Clark IV or V and presence of ulceration [8]. Another possibility
would be the biopsy of dynamic, sentinel lymph node [9]. In cases of
clinically palpable inguinal lymph nodes or when they are shown in
imagery exams (stage III AJCC), the lymphadenectomy is indicated
bilaterally for melanomas of the penis, urethra and scrotum [6,7,10].
The use of adjuvant therapy, either systemic chemotherapy or
radiotherapy, lacks evidence and protocols for use. Even in the studies
with the highest rates of scrotal melanoma, patients submitted to one
modality or another followed distinct schemes with unfavourable
outcomes [1,3].
More important than the management of scrotal melanoma,
this report demonstrates the importance of the evaluation of genitourinary
lesions, taking into account the anatomopathological
result that, as described, may show rare lesions and with a different
management than usual.
References
- Nguyen AT, Kavolius JP, Russo P, Grimaldi G, Katz J, Brady MS. Primary genitourinary melanoma. Urology. 2001; 57: 633-638.
- Manivel JC, Fraley EE. Malignant melanoma of the penis and male urethra: 4 case reports and literature review. J Urol. 1988; 139: 813-816.
- Sánchez-Ortiz R, Huang SF, Tamboli P, Prieto VG, Hester G, Pettaway CA. Melanoma of the penis, scrotum and male urethra: a 40-year single institution experience. J Urol. 2005; 173:1958-1965.
- Milton GW, Shaw HM. Rare variants of malignant melanoma. World J Surg. 1992; 16: 173-178.
- Clark WH, From L, Bernardino EA, Mihm MC. The histogenesis and biologic behavior of primary human malignant melanomas of the skin. Cancer Res. 1969; 29: 705-727.
- Bevan-Thomas R, Slaton JW, Pettaway CA. Contemporary morbidity from lymphadenectomy for penile squamous cell carcinoma: the M.D. Anderson Cancer Center Experience. J Urol. 2002; 167: 1638-1642.
- Kroon BK, Horenblas S, Estourgie SH, Lont AP, Valdés Olmos RA, Nieweg OE. How to avoid false-negative dynamic sentinel node procedures in penile carcinoma. J Urol. 2004; 171: 2191-2194.
- Sim FH, Taylor WF, Ivins JC, Pritchard DJ, Soule EH. A prospective randomized study of the efficacy of routine elective lymphadenectomy in management of malignant melanoma. Preliminary results. Cancer. 1978; 41: 948-956.
- Han KR, Brogle BN, Goydos J, Perrotti M, Cummings KB, Weiss RE. Lymphatic mapping and intra operative lymphoscintigraphy for identifying the sentinel node in penile tumors. Urology. 2000; 55: 582-585.
- Vasudeva P, Agrawal D, Goel A. Malignant melanoma of the scrotum. Urology. 2008; 71: 1053-1054.