Case Report
Rapidly Expanding Erosions in an Elderly Patient
Shaily P Bhatnagar* and Amy W Fox
Department of Dermatology, University of North Carolina, USA
*Corresponding author: Shaily Pandey Bhatnagar, Department of Dermatology, University of North Carolina – Chapel Hill, 410 Market Street, Suite 400, Chapel Hill, NC 27517, USA
Published: 26 Dec, 2016
Cite this article as: Bhatnagar SP, Fox AW. Rapidly
Expanding Erosions in an Elderly
Patient. Ann Clin Case Rep. 2016; 1:
1222.
Abstract
An 85-year old male with diabetes and dementia presented with a two-week history of rapidly growing erosions spanning multiple dermatomes on the left side of the face. Biopsy of the lesion was non-specific; however, a VZV PCR swab was positive, leading to the diagnosis of herpes zoster oticus. The patient was treated with valacyclovir and his rash ultimately healed. This case illustrates a unique presentation of herpes zoster. It typically arises as grouped vesicles in a single dermatomal distribution. Representing reactivation of the varicella zoster virus that lies dormant in the dorsal root ganglion, herpes zoster commonly affects the elderly and the immunosuppressed. Complications include Ramsay Hunt syndrome, which manifests as facial nerve paralysis secondary to herpes zoster oticus. Guanosine analogs are the mainstay of treatment for herpes zoster and recent studies demonstrate their efficacy even after the first 72 hours of symptoms. In the case of Ramsay Hunt Syndrome, corticosteroids should also be administered to avoid permanent paralysis. Ultimately, vaccination is the most effective way to prevent this illness and its long-term effects.
Keywords: Herpes zoster; Shingles; Infection; Ramsay-hunt
Case Presentation
An 85-year-old male nursing home resident with a history of diabetes and dementia presented
with rapidly growing erosions involving the left side of the head and neck. The initial lesion, a papule
on the left posterior scalp was noted 2 weeks prior to presentation; however, the erosions appeared
only a few days before the visit. The patient persistently manipulated the area, but did not complain
of burning or tingling sensations. No one else at the nursing home was affected.
Two weeks prior, the patient was hospitalized for a fall leading to examination of this rash.
The patient was started on antibiotics after an aerobic culture was positive for Acinetobacter and
Enterococcus. A biopsy, Varicella Zoster (VZV) and herpes zoster swab were pending at the time of
dermatology evaluation five days after discharge. Physical examination revealed erosions extending
from the left external ear to the left parietal scalp and involving the left cheek and chin (Figures A and B). At the visit, punch biopsy, aerobic culture, herpes simplex and varicella zoster PCR were
performed.
Clinical Course
The patient was empirically started on valacyclovir 1 gm TID. Same day review of external
medical records revealed a positive VZV PCR during his hospitalization and repeat testing
performed at the visit was also positive, confirming the diagnosis of herpes zoster oticus.
Histopathologic examination was non-specific, showing lichen simplex chronicus superimposed on
chronic eczematous dermatitis. Repeat sections did not reveal viral inclusions suggestive of herpes.
A week later, the patient returned and the lesions appeared to be crusting and healing. The
patient persistently touched his ear, but continued to deny any hearing changes, numbness or
tingling of the area. Given no facial nerve paralysis and no evidence of Ramsay Hunt Syndrome,
physicians deferred corticosteroid use but recommended treatment for post-herpetic neuralgia.
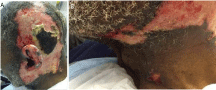
Figure A and B
Figure A and B
Significant erosions on the left head and neck not crossing
the midline and extending from the occipital to parietal scalp, involving the
entirety of the left ear and downward to the left chin.
Discussion
Herpes zoster is a dermatologic and neural disease arising from reactivation of dormant varicella
zoster virus residing in the dorsal root ganglia after initial infection. The virus then travels through
myelinated nerve fibers to the area of skin it innervates leading to cutaneous disease [1]. It presents
unilaterally with macules and papules evolving to vesicles occasionally spanning dermatomes
with pain as the most common symptom. Reactivation usually occurs only once in a life time and
more commonly in elderly or immunosuppressed populations [2]. Herpes zoster affects 20% of
the population with up to 1 million cases in the US annually [3]. The most prevalent sites affected include thoracic and cervical dermatomes, with concern for facial
paralysis and blindness when cranial dermatomes are involved. The
diagnosis is made clinically, but supplemented with Tzanck smears
and viral PCR.
Herpes zoster treatment includes a 7 days course of antiviral
therapy with nucleoside analogs such as acyclovir and valacyclovir.
The initial trial examining acyclovir to treat herpes zoster saw greatest
reduction in time to last lesion formation if treatment began within
48 hours [4]. Guidelines recommend starting treatment within 72
hours; however, as seen in this case, often patients do not present
until days later. Recent studies illustrate no statistically significant
difference in median time to pain cessation or duration of pain if
patients take antiviral therapy before or after 72 hours of rash onset
[5]. In our patient with herpes zoster oticus, development of Ramsay
Hunt Syndrome was of greatest concern. Ramsay Hunt Syndrome
represents a combination of herpes zoster oticus and facial nerve
paralysis involving paralysis of cranial nerves VII and VIII. The most
common cause of acute facial nerve paralysis, its incidence is 5 in
100,000. 80% of patients affected are over 50 years old and exhibit
symptoms such as hearing loss, vertigo, and muscle weakness of
the facial muscles [6]. Without treatment, spontaneous recovery of
facial nerves occurs in 20% of cases. Corticosteroids and antiviral in
combination show the greatest efficacy in regaining motor function
in Ramsay Hunt Syndrome [7].
Post herpetic neuralgia remains the most common long-term
consequence of disease, defined as persistent pain 90 days after
initial rash heals. A direct consequence of virus related damage to
the peripheral nerves during the flare, post-herpetic neuralgia causes
50% of untreated patient residual pain after the rash resolves. Risk
factors include older age, comorbid conditions such as diabetes and
increasing severity of the acute shingles attack [8]. When following
patients for a year after onset of shingles, no difference in residual pain
scores or percentage of patients achieving complete pain resolution is
seen if patients are treated before or after 72 hours of rash onset [9].
Herpes zoster can be a crippling disease with long lasting
complications affecting quality of life. The varicella zoster vaccine proves to be extremely effective in reducing the incidence of shingles.
In Phase III Trials, the vaccine reduces the risk of zoster from 72.4%
to 51% and decreased the burden of illness by 61.1% [10]. While
treatments such as antiviral therapy and corticosteroids help control
its sequel, the only way of truly averting the debilitating consequences
of herpes zoster is by vaccination.
In summary, this case of herpes zoster oticus demonstrates an
unusual presentation of erosions instead of blisters crossing multiple
dermatomes. Confirmatory testing with VZV PCR is recommended
in ambiguous cases, as often the biopsy is non-specific. Treatment
entails administering nucleoside analogs ideally within 72 hours,
yet they still remain efficacious after this time period. Ramsay Hunt
Syndrome and post-herpetic neuralgia is two long-term sequel of
the disease and ultimately, only by adequate vaccination can they be
prevented.
References
- De SK, Hart JC, Breuer J. Herpes simplex virus and varicella zoster virus: recent advances in therapy. CurrOpin Infect Dis. 2015; 28: 589-595.
- Whitley RJ, Weiss H, Gnann JW Jr, Tyring S, Mertz GJ, Pappas PG, et al. Acyclovir with and without prednisone for the treatment of herpes zoster. A randomized, placebo-controlled trial. The National Institute of Allergy and Infectious Diseases Collaborative Antiviral Study Group. Ann Intern Med. 1996; 125: 376-383.
- Yun H, Yang S, Chen L, Xie F, Winthrop K, Baddley JW, et al. Risk of Herpes Zoster in Auto-immune and Inflammatory diseases: Implications for Vaccination. Arthritis Rheumatol. 2016; 68: 2328-2337.
- McKendrick MW, McGill JI, White JE, Wood MJ. Oral acyclovir in acute herpes zoster. Br Med J (Clin Res Ed). 1986; 293: 1529-1532.
- Decroix J, Partsch H, Gonzalez R, Mobacken H, Goh CL, Walsh L, et al. Factors influencing pain outcome in herpes zoster: an observational study with valaciclovir. Valaciclovir International Zoster Assessment Group (VIZA). J Eur Acad DermatolVenereol. 2000; 14: 23-33.
- Uscategui T, Dorée C, Chamberlain IJ, Burton MJ. Antiviral therapy for Ramsay Hunt syndrome (herpes zoster oticus with facial palsy) in adults. Cochrane Database Syst Rev. 2008; 4: CD006851.
- deRu JA, van Benthem PP. Combination therapy is preferable for patients with Ramsay Hunt syndrome. OtolNeurotol. 2011; 32: 852-855.
- Chen N, Li Q, Yang J, Zhou M, Zhou D, He L, et al. Antiviral treatment for preventing postherpetic neuralgia. Cochrane Database Syst Rev. 2009; 2: CD006866.
- Rasi A, Heshmatzade Behzadi A, Rabet M, Hassanloo J, Honarbakhsh Y, Dehghan N, et al. The efficacy of time-based short-course acyclovir therapy in treatment of post-herpetic pain. J Infect Dev Ctries. 2010; 4: 754-760.
- Cook SJ, Flaherty DK. Review of the Persistence of Herpes Zoster Vaccine Efficacy in Clinical Trials. ClinTher. 2015; 37: 2388-2397.