Case Report
Bilateral Choanal Stenosis Requıred Surgical Intervention in a Premature Infant Secondary to Nasal Cpap
Sevim Unal1*, Deniz Gönülal1, Fatih Alper Akcan2 and Didem Aliefendioğlu3
1Department of Neonatology, Ankara Children’s Hematology Oncology Research Hospital, Turkey
2Department of Otorhinolaryngology-Head and Neck Surgery, Ankara Children’s Hematology Oncology Research Hospital, Turkey
3Department of Pediatrics, Kirikkale University School of Medicine, Turkey
*Corresponding author: Sevim Unal, Ankara Children’s Hematology Oncology Research Hospital, İrfan Bastug Cd, Kurtdereli Sk, Altındağ / Ankara / Turkey
Published: 03 Nov, 2016
Cite this article as: Unal S, Gönülal D, Akcan FA,
Aliefendioğlu D. Bilateral Choanal
Stenosis Requıred Surgical Intervention
in a Premature Infant Secondary to
Nasal Cpap. Ann Clin Case Rep. 2016;
1: 1179.
Abstract
Continuous positive airway pressure (CPAP) is defined as "The least harmful way to keep the alveoli open and provide adequate gas exchange" in the neonatal intensive care unit (NICU), thus there has been increased use of CPAP. However, the use of prolonged nasal CPAP (nCPAP), in the premature and especially extremely low birth weight (ELBW) infants might cause serious nasal trauma such as columella and nasal septum necrosis. Herein, we presented an ELBW infant developed bilateral choanal stenosis secondary to prolonged implementation of nCPAP and required surgical intervention.
Introduction
Most of the premature infants require mechanical ventilatory support within the early days of
life. For many years, endotracheal intubation and invasive mechanical ventilation has been the main
modality for this purpose. However, technologic improvements related to mechanical ventilation
have given rise to the development of noninvasive ventilation to meet the newborn infant’s needs.
Noninvasive methods are preferred in the neonatal intensive care unit (NICU) due to the severe side
effects caused by mechanical ventilation (hemodynamic effects, barotrauma, lung injury, oxygen
toxicity, ventilator-associated pneumonia, patient discomfort, ventilator mismatch, requirement
of excessive sedation, tube obstruction, vocal cord injury, tube problems including hemorrhage,
etc.), especially in the preterm infants. Owing to the advantages, non-invasive ventilation should be
applied primarily for respiratory failure in the neonates, if there is no contraindication [1,2].
Continuous positive airway pressure (CPAP) should be defined as "The least harmful known
way to keep the alveoli open and provide adequate gas exchange". CPAP with nasal devices is widely
used in the respiratory management of newborns. Nasal CPAP (nCPAP) prevents alveolar collapse
and prevents pulmonary shunts by protecting functional residual capacity. It prevents obstructive
apnea attacks by the stabilization of large and small airways and reduces the work of breathing,
besides prevents destruction of the surfactant [3]. nCPAP can improve oxygenation, maintain lung volume, lower upper airway resistance, reduce obstructive apnea, and most importantly eliminate
tube/ventilator and the associated risks. As nCPAP is well-documented non-invasive respiratory
support since Gregory [4] first reported the efficacy for respiratory distress syndrome (RDS) in 1971, it is widely used in the NICUs all over the world [5,6]. However, long-term application of nCPAP via nasal devices can cause nasal trauma, such as nasal septum necrosis, especially in the extremely
low birth weight (ELBW) premature infants [6-8]. Herein, we presented an ELBW premature infant
developed bilateral choanal stenosis due to prolonged implementation of nCPAP and required surgical intervention.
Case Presentation
A female ELBW premature infant was referred to our NICU at 4 months old postnatally because
of bilateral choanal stenosis. She was one of the twins born at 28 weeks of gestation by cesarean
section and weighed 990 grams at birth. She was applied surfactant therapy with the diagnosis of RDS
and nCPAP for supplemental oxygen support following birth. As she could not tolerate extubation,
prolonged nCPAP and short period of mechanical ventilation were applied. She was given steroid
therapy with the diagnosis of bronchopulmonary dysplasia (BPD), and antibiotic therapies on
different periods. On admission, her physical examination revealed 2720 gr in weight, 32 cm in head sircumference, deformed nose, tachypnea, subcostal retractions,
acrocyanosis and respiratory failure. Nasogastric catheter could not
be advanced through the both nostrils. Laboratory analysis were
normal except hypoxemia, her cranial ultrasonography was normal,
echocardiography revealed secundum atrial septal defect. Advanced
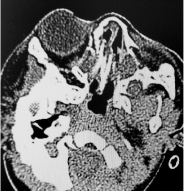
stage of retinopathy was not determined. The patient showed bilateral
choanal stenosis on paranasal computed tomography (Figure 1).
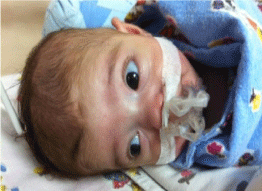
Endoscopic dilation of bilateral choanal stenosis was performed
by the ear-nose-throat department and polyethylene tubes were
placed within the both nostrils for the prevention of restenosis.
Polyethylene tubes were removed after 3 weeks following surgical
intervention (Figure 2).
She was extubated after surgery and additional oxygen support
was discontinued at 5.5 months old postnatally. Her oxygen
saturation level was normal at 6 months of old and discharged to
home on room-air to continue follow-up at outpatient clinic.
Discussion
CPAP is a well-established noninvasive method of respiratory
support for all weight groups of neonates. It is often preferred and
widely used in the respiratory management of the neonates with RDS,
apnea and weaning from the ventilator. Early nCPAP is harmless,
recommended as the first choice, because it is less invasive, costeffective
and easy to apply. It causes 50% reduction in the need for
intubation and surfactant requirement, decreases mortality, and
provides a falling trend in the BPD. Early nCPAP and surfactant
therapy reduce mechanical ventilation requirements, side effects
associated with intubation/ventilation and related risks [2,3,5]. In
this report, our case has been applied early nCPAP and surfactant
therapy, but could not be weaned from the ventilator, developed BPD
and bilateral choanal stenosis secondary to prolonged use of nCPAP.
Although, there are various devices to deliver CPAP such as
nasopharyngeal tube, different prong systems and mask, bi-nasal
prongs have been most widely used in the respiratory management of
newborns. On the other hand, positioning the tip of the tube, prong
or cannula through the nose might be difficult [9]. There were reports
describing systemic and local complications related to nCPAP
delivery methods. Gastric distention, air leaks, nasal congestion, skin
and mucosa hyperemia, local erosion, bleeding, necrosis, septum
breakdown, columella and septal ulcerations are complications
of the nCPAP [5-10]. Nasal injury is the most common form of
complication due to nCPAP, but long-term cosmetic sequelae are very rare. The true incidences of these complications are uncertain.
To our knowledge, this case with severe choanal stenosis developed
secondary to nCPAP is the second one reported in the literature.
Previously Moloney et al. [11] have been reported severe choanal
stenosis due to the implementation of nasopharyngeal CPAP. This
case also required surgical intervention because of choanal stenosis
caused by prolonged nCPAP.
The increased pressure around nostrils decreases the blood flow
to local tissues, impairs perfusion and causes ischemia and skin
breakdown during nCPAP implementaton [9,10]. Nasal injuries
caused by prongs were classified in three stages: mild, moderate
and severe [10,12]. The mild stage described as redness or nasal
hyperemia; the moderate referred bleeding injury and the severe
stage referred necrosis [12]. The pressure of delivery systems and
the duration of nCPAP are important factors causing nasal injury.
Prongs with inappropriate size and fixed into the newborn’s nostrils
very tight defined as harmful. Prolonged duration of CPAP defined
as a major risk factor for the development of nasal injury and trauma
[6,9,12]. We thought that the main risk factor causing nasal injury
was prolonged nCPAP implementation in this case. Nascimento et
al. [13] supposed that the longer the device had used, the more severe
the lesion. They found that CPAP more than 2 days had been risk
factor nasal damage. To avoid nasal trauma, protection of nostrils by
adhesive tapes, such as common patches, hypoallergenic tapes, silicon
gel and hydrocolloid dressings were recommended [9,10,14-16].
The nasal tissue injury caused by the tube, cannula or prongs
placed in the nose is easy to occur and more common in premature
infants on nCPAP. Because, nasal tissue is more vulnareble to
damage, and also muscle tone is looser in preterm infants. nCPAP
may progress to severe nasal ulceration or septal perforation
especially in the preterm and/or very low birth weight infants [5-11].
The physicians are recommended to have a command of indications
and contraindications to nCPAP. Besides close observation of the
baby in terms of disadvantages and complications of nCPAP is a
necessity. The topical protective measures, the implementation of
strict monitoring and scoring systems for the patients on nCPAP have
been reported to decrease the ratios of complications. The accordion
tube system easy to shape, matching prongs to nostril properly, and
a good hat should be used in order to prevent nasal complications
[5-11]. The proper position of the head, using pillows to support the
position, frequent moistening of the nostrils, careful and frequent
airway control are recommended [15,16].
Figure 1
Figure 2
Conclusion
In conclusion, prolonged use of nCPAP in especially premature neonates can cause serious complications, and each NICU administering nCPAP should monitor the babies for complications, develop appropriate protocols and proper care methods. We wanted to underline the preventive treatments, appropriate position of the nose and head, frequent monitoring of the patient might be beneficial on the prevention of nasal damage.
References
- Claure N, Bancalari E. Non-invasive ventilation in premature infants. Arch Dis Child Fetal Neonatal Ed. 2015; 100: 2-3.
- Geary C, Caskey M, Fonseca R, Malloy M. Decreased incidence of bronchopulmonary dysplasia after early management changes, including surfactant and nasal continuous positive airway pressure treatment at delivery, lowered oxygen saturation goals, and early amino acid administration: a historical cohort study. Pediatrics. 2008; 121: 89-96.
- Diblasi RM. Nasal continuous positive airway pressure (CPAP) for the respiratory care of the newborn infant. Respir Care. 2009; 54: 1209–1235.
- Gregory GA, Kitterman JA, Phibbs RH, Tooley WH, Hamilton WK. Treatment of the idiopathic respiratory-distress syndrome with continuous positive airway pressure. N Engl J Med. 1971; 284: 1333–1340.
- Fischer C, Bertelle V, Hohlfeld J, Forcada-Guex M, Stadelmann-Diaw C, Tolsa JF. Nasal trauma due to continuous positive airway pressure in neonates. Arch Dis Child Fetal Neonatal Ed. 2010; 95: 447–451.
- Yong S, Chen S, Boo N. Incidence of Nasal trauma associated with nasal prong versus nasal mask during continuous positive airway pressure treatment in very low birth infants. Arch Dis Child Fetal Neonatal Ed. 2005; 90: 480-483.
- Loftus BC, Ahn J, Haddad J. Neonatal nasal deformities secondary to nasal continuous positive airway pressure. Laryngoscope. 1994; 104: 1019-1022.
- Shanmugananda K, Rawal J. Nasal trauma due to nasal continuous positive airway pressure in newborns. Arch Dis Child Fetal Neonatal Ed. 2007; 92: 18.
- Xie LH. Hydrocolloid dressing in preventing nasal trauma secondary to nasal continuouspositive airway pressure in preterm infants. World J Emerg Med. 2014; 5: 218-222.
- Günlemez A, Isken T, Gökalp AS, Türker G, Arisoy EA. Effect of silicon gel sheeting in nasal injury associated with nasal CPAP in preterm infants. Ind Pediatr. 2010; 47: 265–267.
- Moloney G, Tudehope DI. Severe choanal stenosis complicating nasopharyngeal CPAP. J Paediatr Child Health. 1993; 29: 72.
- Buettiker V, Hug MI, Baenziger O, Meyer C, Frey B. Advantages and disadvantages of different nasal cpap systems in newborns. Intensive Care Med. 2004; 30: 926-930.
- do Nascimento RM, Ferreira AL, Coutinho AL, Santos Verissimo RC. The frequency of nasal injury in newborns due to the use of continuous positive airway pressure with prongs. Rev Lat Am Enfermagem. 2009; 17: 489-494.
- Robertson NJ, McCarthy LS, Hamilton PA, Moss ALH. Nasal deformities resulting flow driver continuous positive airway pressure. Arch Dis Child Fetal Neonat. 1996; 75: 209-212.
- Squires AJ, Hyndman M. Prevention of nasal injuries secondary to nCPAP application in the ELBW infant. Neonatal Netw. 2009; 28: 13-27.
- McCoskey L. Nursing Care Guidelines for prevention of nasal breakdown in neonates receiving nasal CPAP. Adv Neonatal Care. 2008; 8: 116-124.