Case Presentation
Late Metastatic Pontine Melanoma Presenting as Ataxia
Jeremy Hornibrook1*, Scott Wells2, Nicholas Finnis3 and David Gibbs4
1Department of Otolaryngology-Head and Neck Surgery, Christchurch Hospital, New Zealand
2Department of Radiology, Christchurch Hospital, New Zealand
3Department of Neurosurgery, Christchurch Hospital, New Zealand
4Department of Oncology, Christchurch Hospital, New Zealand
*Corresponding author: Jeremy Hornibrook, Department of Otolaryngology-Head and Neck Surgery, Christchurch Hospital, 2 Riccarton Avenue, Christchurch 8410 8410 New Zealand
Published: 01 Nov, 2016
Cite this article as: Hornibrook J, Wells S, Finnis N, Gibbs
D. Late Metastatic Pontine Melanoma
Presenting as Ataxia. Ann Clin Case
Rep. 2016; 1: 1171.
Abstract
Ataxia was the only presenting symptom of a large pontine melanoma secondary in a 63 year-old male after five years of follow-up. Although the brain is a common site for melanoma metastasis, brainstem involvement is uncommon and its presentation with ataxia and no cranial nerve palsies is unusual.
Case Presentation
A 63 year-old man presented with a 2 month history of insecure gait. There were no localising
symptoms in regard to hearing, no headache, and he had not had vertigo. On examination he was
fully alert and orientated. Audiometry showed a symmetrical noise-induced hearing loss. Eye
examination with Frenzel glasses revealed no spontaneous nystagmus. Vestibulo-ocular(VOR)
reflexes ,VOR suppression and a provocative positional tests were normal. Facial nerve function,
facial sensation and tongue movements were normal. The Romberg test was normal. Tandem
walking was performed with difficulty.
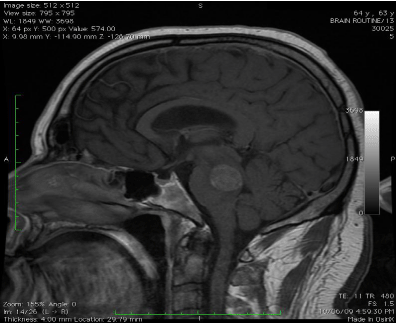
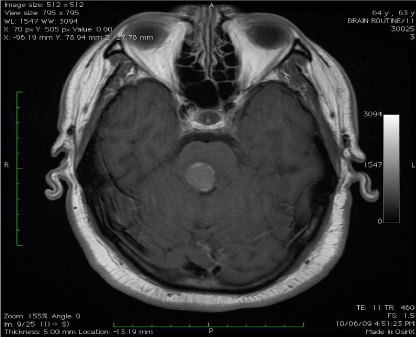
MRI scanning (Figure 1 and 2) revealed an enhancing mass (20 x 19 x 16 mm) to the right of the
midline in the superior pons with surrounding oedema extending into the right cerebral peduncle,
right middle cerebellar peduncle and dorsal pons, with distortion of the fourth ventricle.
Previous history and clinical course
Five years previously histology on a small forearm skin nodule (removed as an ellipse) showed
a malignant melanoma in the mid reticular dermis extending to the sub dermis and one transverse
margin. One year prior a skin lesion was treated by cryotherapy. Staging CT scanning showed no
metastases. Wide local excision with grafting and sentinel node removal was carried out. At annual
oncology follow-ups for 5 years no recurrence could be detected. Further scanning showed small
cerebral, lung and liver metastases. Due to increasing ataxia and slurred speech he was admitted for
high dose dexamethasone and whole brain radiotherapy, but died 8 weeks after initial presentation.
Discussion
Brain metastases are the most common cerebral tumours. The most common primary tumour sources are lung and breast [1-3]. Five to ten percent are from cutaneous melanoma [4]. The distribution of metastases closely follows the volume of the affected in the order cerebrum, cerebellum and brainstem [2] (approximately 10% [3]). In a large series of brain stem metastases [3] 9% were from melanoma. The most common symptoms were hemiparesis and cranial nerve palsies, with ataxia being uncommon. Ataxia is more likely to be a presentation of cerebellar metastases, but in this patient resulted from involvement of cerebellar connections.
Figure 1
Figure 2
References
- Lassman AB, De Angelis LM. Brain metastases. Neurol Clin N A. 2003; 21: 1-23.
- Posner JB, Chernik NL. Intracranial metastases from systemic cancer. Adv Neuro. 1978; 19: 579- 592.
- Hunter KMF, Rewcastle NB. Metastatic neoplasms of the brainstem. Can Med Ass J. 1968; 98: 1- 7.
- Ginaldi S, Wallace S, Shalen P, Luna M, Handel S. Cranial computed tomography of malignant melanoma. AJR Am J Roentgenol. 1981; 136: 145-149.