Clinical Image
Focal Fibrocartilaginous Dysplasia (FFCD)
Zied Jlalia* and Mahmoud Smida
Department of pediatric orthopedics, Kassab institute, Kasar Said 2010 La Manouba, Faculty of Medicine, Tunis El
Manar University, Tunis, Tunisia
*Corresponding author: Zied Jlalia, Department of pediatric orthopedics, Kassab institute, Kasar Said 2010 La Manouba, Faculty of Medicine, Tunis El Manar University, Tunis, Tunisia
Published: 24 Oct, 2016
Cite this article as: Jlalia Z, Smida M. Focal
Fibrocartilaginous Dysplasia (FFCD).
Ann Clin Case Rep. 2016; 1: 1160.
Clinical Image
Although many skeletal disorders may result in bilateral angular deformity of the lower extremity, only a few cause unilateral deformity. Most children who have bilateral angular deformities of the lower extremities also have benign physiological conditions in which the deformities correct with growth [1]. This report is a description our case who had an angular deformity of the distal end of the femur associated with an unusual fibrous tether that resulted in a valgus deformity of the distal end of the femur. A two and one half year old boy was seen for an obvious deformity (genu valgum) of the right lower limb, which had first been noticed by the mother. The deformity was painless, and there was no history of injury or infection. Roentgenograms had shown an unusual ill defined linear defect in the femoral metaphysis and a valgus deformity of the distal end of the femur (Figure 1). The child’s condition was followed regularly. The shortening of the femur increased and there was a slight increase in the valgus angulation of the leg. Surgical correction was performed with external opening osteotomy using hydroxyapatite bone substitute (Figure 2). FFCD is a dysplastic disorder of long bones that was first described by Bell et al. in 1985 [2]. It is a rare cause of unilateral bone deformities in children which usually affects the medial aspect of the tibial metaphysis. The differential diagnosis can be a neurofibromatosis, Ollier disease and growth disturbance resulting from physeal injury or infection. There is a spectrum of histopathologic features that ranges from purely fibrous lesions to those containing hyaline and fibrocartilage. The fibrous band can be break-up as a result of growth and correction of the deformity is spontaneously [3]. Surgery is required when the deformation is greater than 20°.
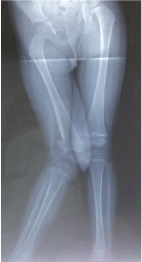
Figure 1
Figure 1
Linear defect in the femoral metaphysis and a valgus deformity of the distal end of the femur.
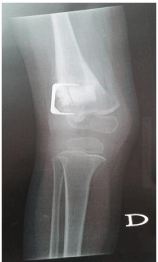
Figure 2
Figure 2
Surgical correction was performed with external opening osteotomy using hydroxyapatite bone
substitute.
Discussion
It is important to understand that suspected Monteggia fractures
should be urgently referred to orthopaedics. Most of the common
complications can be avoided with early intervention. Treatment
following delayed diagnosis is more complex and can lead to poor
outcome [4].
The commonest complication is injury to peripheral nerves,
mainly to the radial nerve or the posterior interosseous nerve. These
are usually affected in type I and II fractures. It usually presents as
a neuropraxia where the nerve function usually returns within 9-10
week. It is very important on the first consultation itself peripheral
nerve examination is thoroughly assed and documented, to avoid
litigation issues.
Periosteal calcification occurs in about 3% of the cases, usually
associated with high energy injuries, fractures involving the radial
head and following multiple attempts at manipulations. It can involve
the annular ligament or around the radial head affecting the ROM if
the elbow.
There are several ways of treating Montaggia fractures. Closed
reduction with manipulation is usually successful in children with
type I and II fractures [5,6]. ORIF of ulna shaft is required in open
or unstable fractures, comminuted fractures and most Montaggia
fractures in adults. If it involves a fracture of the radial head, which is not stable once ulna shaft is fixed, open reduction of the radial head is
also required. Transverse and oblique fractures will inevitably require
IM nailing.
If the patient is discharged post operatively, ideally they should
followed up 7 days post reduction with imaging, then at 2 weeks with
x-ray, 3 weeks to review cast and plaster and then at 6 weeks to assess
healing with imaging. At 6 weeks if mobility if the elbow and wrist
are preserved with satisfactory healing, they can be discharged to the
community with advice to see their GP if there is any deterioration.
Contact sport should also be avoided for the next 2-3 months to
ensure full recovery.
Conclusion
Prompt diagnosis which requires high index of suspicion and following basic principles of managing fracture i.e. examining and radiologically investigating the joint above and below the fracture yield in favourable outcome and good results.
References
- Bado JL. The Monteggia lesion. Clin Orthop Relat Res. 1967; 50: 71-86.
- Wiley JJ, Galey JP. Monteggia injuries in children. J Bone Joint Surg Br. 1985; 67: 728-731.
- http://www.orthobullets.com/trauma/1024/monteggia-fractures.
- http://emedicine.medscape.com/article/1231438-overview#a4.
- http://gait.aidi.udel.edu/educate/montegfxhttp://gait.aidi.udel.edu/ educate/montegfx.
- http://www.rch.org.au/clinicalguide/guideline_index/fractures/ Monteggia_fracturedislocations_Emergency_Department setting/.