Case Report
Montaggia Type 4 Fracture -A Case Report of an Unusual Presentation of a Rare Injury
M Sajjad Athar*, Neil Ashwood, Vijesh Rao and Ilias Galanapoulos
Burton Hospitals NHS Foundation Trust, UK
*Corresponding author: M Sajjad Athar, Burton Hospitals NHS Foundation Trust, Belvedere Road, Burton on Trent, UK
Published: 19 Oct, 2016
Cite this article as: Sajjad Athar M, Ashwood N, Rao V,
Galanapoulos I. Montaggia Type 4
Fracture -A Case Report of an Unusual
Presentation of a Rare Injury. Ann Clin
Case Rep. 2016; 1: 1158.
Abstract
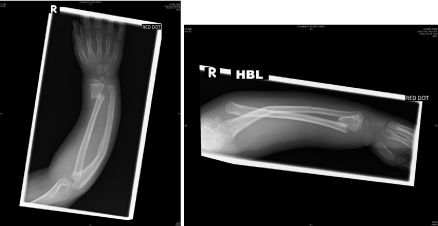
5 year old girl presented to A&E following a fall from the swing. On examination there was tenderness along her right arm, with visible gross deformity. X-rays confirmed that she has a Montaggia type 4 fracture showing multiple fractures along the ulna and radius with dislocation at the proximal radius and dorsal radial displacement. The prompt diagnosis and management of the injury resulted in a favourable outcome.
Introduction
Monteggia fracture is described as a dislocation of the proximal radio-ulnar joint involving
fractures along the forearm. It accounts to less than 5% of forearm fractures.
The ulna fracture is usually clinically and radiographically visible; however the associating radial
head dislocation may be missed. Therefore it is important to obtain x-rays in both AP and true
lateral views including the elbow and the wrist. The posterior border of the ulna should be carefully
assessed, especially if it’s a greenstick fracture of the ulna which is not obvious. If the border is
‘bowed’ it is most probably a greenstick fracture [1,2].
If Monteggia fractures are left untreated it can have dire complications such as malunion and
peripheral inflammatory neuropathy. Bado classification is commonly used to describe Monteggia
fractures (Table 1) [3].
Case Presentation
5 year old girl presented to Accidents and Emergency unit with visible gross deformity, swelling
of right arm. Resulting from an unwitnessed fall while playing on the swing in padded play area.
The child explained that she fell on a step landing on her extended right arm. There after she found
it difficult to mobilise her arm. She had no significant past medical history, no history of recurrent
fractures. Development milestones were appropriate for her age.
On Physical examination there was swelling extending from the elbow to the wrist, mostly
at the mid shaft area, and increased curvature along the forearm. Neurovascular status was not
compromised. She was able to move her fingers and shoulder. Movements along the elbow and wrist
were affected in all directions (Figure 1).
Treatment
Patient was taken to theatre the following morning. Manipulation under anaesthesia was
done initially to reduce the ulna and distal radius fracture, radial head reduced spontaneously.
Unfortunately the reduction remained unstable. Therefore intrameduallary fixation of ulna was
done through an incision over the proximal ulna. 2.5 mm drill hole was made; titanium wire was
passed through the ulna.
Distal radial fracture was stabilised with 1.6 mm K wire, which
was bent and cut, wound closed with 3’0 vicryl
Outcome and follow-up
Uneventful post operatively, discharged home day 5 post op.
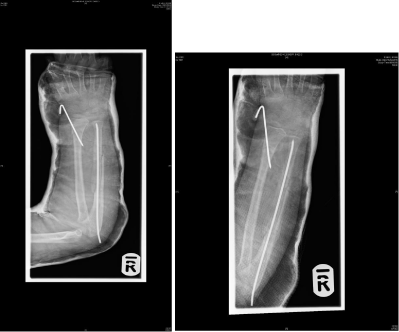
Seen at fracture clinic 10 days post op. X-rays on 10th post op day was
satisfactory (Figure 2). No complications noted.
She was seen in the fracture clinic regularly and the pins were
removed on 08/03/2016. She was sent home with a broad sling.
Further follow up is planned for the following week.
Table 1
Figure 1
Figure 2
Discussion
It is important to understand that suspected Monteggia fractures
should be urgently referred to orthopaedics. Most of the common
complications can be avoided with early intervention. Treatment
following delayed diagnosis is more complex and can lead to poor
outcome [4].
The commonest complication is injury to peripheral nerves,
mainly to the radial nerve or the posterior interosseous nerve. These
are usually affected in type I and II fractures. It usually presents as
a neuropraxia where the nerve function usually returns within 9-10
week. It is very important on the first consultation itself peripheral
nerve examination is thoroughly assed and documented, to avoid
litigation issues.
There are several ways of treating Montaggia fractures. Closed
reduction with manipulation is usually successful in children with
type I and II fractures [5,6]. ORIF of ulna shaft is required in open
or unstable fractures, comminuted fractures and most Montaggia
fractures in adults. If it involves a fracture of the radial head, which is not stable once ulna shaft is fixed, open reduction of the radial head is
also required. Transverse and oblique fractures will inevitably require
IM nailing.
If the patient is discharged post operatively, ideally they should
followed up 7 days post reduction with imaging, then at 2 weeks with
x-ray, 3 weeks to review cast and plaster and then at 6 weeks to assess
healing with imaging. At 6 weeks if mobility if the elbow and wrist
are preserved with satisfactory healing, they can be discharged to the
community with advice to see their GP if there is any deterioration.
Contact sport should also be avoided for the next 2-3 months to
ensure full recovery.
Conclusion
Prompt diagnosis which requires high index of suspicion and following basic principles of managing fracture i.e. examining and radiologically investigating the joint above and below the fracture yield in favourable outcome and good results.
References
- Bado JL. The Monteggia lesion. Clin Orthop Relat Res. 1967; 50: 71-86.
- Wiley JJ, Galey JP. Monteggia injuries in children. J Bone Joint Surg Br. 1985; 67: 728-731.
- http://www.orthobullets.com/trauma/1024/monteggia-fractures.
- http://emedicine.medscape.com/article/1231438-overview#a4.
- http://gait.aidi.udel.edu/educate/montegfxhttp://gait.aidi.udel.edu/ educate/montegfx.
- http://www.rch.org.au/clinicalguide/guideline_index/fractures/ Monteggia_fracturedislocations_Emergency_Department setting/.