Case Report
Extensively Disseminated Tuberculosis in an Immuno Competent Young Women Presenting as Isolated Optic Neuritis
Priya Sivakumarm*, Nirmala Devy and Rengaraj Vengatesh
DNB Ophthalmology, Aravind Eye Care, India
*Corresponding author: Priya Sivakumarm, Aravind Eye Care, Thavalakuppam Pondicherry, 605007, India
Published: 03 Oct, 2016
Cite this article as: Sivakumarm P, Devy N, Vengatesh R.
Extensively Disseminated Tuberculosis
in an Immuno Competent Young
Women Presenting as Isolated Optic
Neuritis. Ann Clin Case Rep. 2016; 1:
1153.
Abstract
Tuberculosis (TB) is the first infectious disease declared by the World Health Organization as a
global health emergency. It remains the leading cause of death among infectious diseases causing
more deaths worldwide than human immunodeficiency virus (HIV). The following case report
highlights the occult and non specific presentations of the disease which makes it a diagnostic
challenge.
We report a case of extensively disseminated tuberculosis in an immunocompetant young
woman presenting as isolated optic neuritis. Extra pulmonary tuberculosis is commoner among
immunocompromised patients .Co-existence of military and intracranial tuberculosis in an
immunocompetent person is extremely rare.
Case Presentation
A 28 years old female patient presented with complaints of defective vision in her right eye for
ten days which was sudden in onset, progressive and painful. Her best corrected visual acuity was
6/60 and 6/6 in right and left eyes respectively. Right eye showed a grade 3 relative afferent pupillary
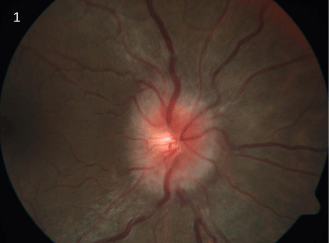
defect, painful extra ocular movements, disc edema with hyperemia (Figure 1), defective colour
vision tested using pseudo isochromatic Ishihara chart and markedly depressed visual field. Left
eye was normal except for poor consensual reflex. Intra ocular pressures were normal. Systemic and
other cranial nerves examinations were normal. She was afebrile with no palpable lymph nodes.
Hemoglobin, blood counts, blood sugar and erythrocytes sedimentation rate were within
normal limits. Her mantoux was negative.
In spite of being chest asymptomatic, with normal blood investigations, negative mantoux
reaction and clinical features pointing towards demyelinating optic neuritis which is a clinical
diagnosis not requiring neuroimaging for confirmation, neuroimaging was planned based on her
history of worsening of vision beyond ten days. To our surprise, Magnetic resonance imaging (MRI)
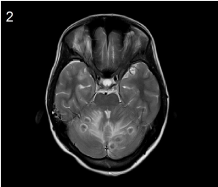
of brain showed multiple granulomatous lesions with ring enhancement in cerebral and cerebellar
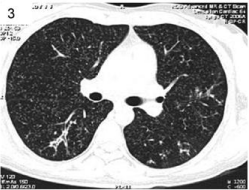
hemispheres (Figure 2). Following which computerized tomography (CT) of chest showed military
mottling (Figure 3), thus confirming the diagnosis of disseminated tuberculosis. She tested negative for HIV.
Figure 1
Figure 1
Right eye fundus picture showing disc edema with hyperemia and normal macula, suggestive of
papillitis form of optic neuritis.
Figure 2
Figure 2
MRI brain showing multiple, well defined, cystic, ring enhancing
lesions of varying sizes with surrounding vasogenic edema suggestive of
tuberculomas.
Discussion
Optic neuritis defined as inflammation of optic nerve, is commonly
due to demyelination associated with multiple sclerosis. It usually
occurs in women less than 40 years and is characterized by acute
unilateral visual loss, eye pain that worsens on movements, optic disc
appearing either normal (64.7%) or swollen (35.3%) and spontaneous
recovery starting within 2 to 3 weeks [1]. High dose corticosteroids
fasten recovery [1]. In rare instances like our patient, occult infection
can mimic demyelinating optic neuritis. If misdiagnosed, patient will
either be observed for spontaneous recovery or administered high
doses of systemic steroids, both of which can be disastrous.
Neuroimaging in optic neuritis is done only to predict
the possibility of multiple sclerosis. In an Asian country like
India where multiple sclerosis is not very prevalent, and due
to poor affordability of patients, neuroimaging is not routinely
done. Potentially life threatening complications of intravenous
steroids in an underlying unaddressed infection like tuberculosis
was avoided with the help of judicious use of neuroimaging.
Although rare, TB should be considered in the differential diagnosis
of apparently isolated papillitis or neuroretinitis [2]. Optic
nerve involvement may be due to hematogenous dissemination,
direct infection, and contiguous spread from choroid or from
hypersensitivity to the infectious agent [3].
Intracranial TB usually presents with seizures, focal neurological
deficits or mass effects [4]. Our patient did not have any neurological
deficit other than unilateral defective vision. Negative mantoux
reaction could be due to tuberculin anergy reported in miliary TB [5].
Latent miliary and intracranial tuberculosis in an
immunocompetent young person presenting as isolated optic
neuritis has not been reported earlier. This report highlights the rare
associations of a common deadly infectious disease thus emphasizing
the importance of a high index of clinical suspicion in our present era
of globalization.
Figure 3
Figure 3
CT chest showing innumerable, small, wide spread pulmonary
nodules suggestive of disseminated tuberculosis.
References
- Beck RW, Gal RL. Treatment of acute optic neuritis: A summary of findings from the optic neuritis treatment trial. Arch Ophthalmol. 2008; 126: 994‑995.
- Gupta V, Gupta A, Rao NA. Intraocular tuberculosis – an update. Surv Ophthalmol. 2007; 52: 561-587.
- Davis EJ, Rathinam SR, Okada AA, Tow SL, Petrushkin H, Graham EM et al. Clinical spectrum of tuberculous optic neuropathy. J Ophthalmic Inflamm Infect. 2012; 2:183-189.
- Togha M, Sahraian MA, Hosseini SJ, Haddadi A. Brain tuberculoma: Report of a case presented with prolonged nonspecific symptoms and multiple brain tuberculoma. Iran J Neurol. 2012; 11: 34-35.
- Surendra k, Mohan A, Sharma A. Challenges in the diagnosis and treatment of military tuberculosis. Indian J Med Res. 2012; 135: 703-730.