Case Report
IVR for SMA Thrombosis of Elder Male
Megumi Nakamura* and Hajime Kitagaki
Department of Radiology, Shimane University, Japan
*Corresponding author: Megumi Nakamura, Department of Medicine, Shimane University, Izumo, Enya 89-1, Shimane, Japan
Published: 12 Sep, 2016
Cite this article as: Nakamura M, Kitagaki H. IVR for SMA
Thrombosis of Elder Male. Ann Clin
Case Rep. 2016; 1: 1123.
Abstract
Recently, mortality rates for super mesenteric artery (SMA) thrombosis have been on the rise. Several papers on interventional radiology (IVR) for SMA thrombosis have been written. When a quick diagnosis is made relative to the time of on set, flow recovery is expected following IVR for SMA thrombosis without intestinal resection. This case involved IVR used for thrombo-aspiration and thrombolysis of a male, 100 years of age, who had SMA thrombosis with almost completely obstructed blood flow. First, by using thrombo-aspiration for the occluded artery, blood flow was somewhat recovered. Second, continuous thrombolysis was performed for three days. The patient reported that he was having stomach pains after SMA flow recovered. After aspiration of the thrombus, a dose of urokinase (240,000U/10cc) was administered. During arterial infusion, urokinase (240,000U) was administered for between two to three days. The sheath was withdrawn on the fourth day. Anti-coagulation was maintained for 160 seconds during arterial infusion therapy. The patient was discharged after 24 days.
Keywords: SMA thrombosis; Thrombolysis; Thrombo-aspiration
Case Presentation
100 years-old male 148cm 42.9kg
Past history: rt. renal tumor (renal cell carcinoma) T2N1M0 thyroid cancer post operation
Family history: not particular
Present illness: nausea, vomiting, stomach pain after lunch
Emergency department visit
BT 36.5oC BP 150/57mmHgpulse67/mins at O2 97% (room air)
Abdominal findings: flat+elastic hard slightly tenderness on whole abdomen; rebound
tenderness (-)
Technical Tips
It is important that the guiding sheath is placed at the origin of the super mesenteric artery.
Many reports have indicated that thrombo-aspiration is a useful
technique for SMA thrombosis. Use of a guiding sheath protects the
SMA from damage during repeated aspiration. It is important that
peripheral flow of the SMA is secured. Use PTA (percutaneous transluminal
angioplasty) as a last resort, because the width of the catheter used during the PTA procedure will push thrombosis to peripheral
vessels, thus preventing the possibility of thrombolysis. With early
detection of thrombosis, blood flow will recover under continuous
thrombolysis.
Table 1
Table 1
Blood laboratory data.
ECG supra ventricular premature contraction ventricular premature contraction flat T waves (V4.5.6).
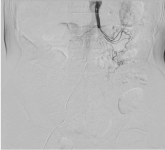
Figure 1
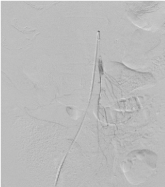
Figure 2
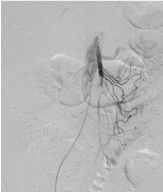
Figure 3
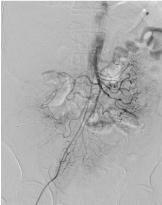
Figure 4
Discussion
Several important features in this case indicated the use of IVR for SMA thrombosis. First, the time from pathogenesis to the start of IVR was brief, and IVR was begun as soon as possible. It cannot be stated that SMA flow was recovered if time from diagnosis to the start of IVR is taken into consideration, because intestinal resection was done. In this case, we decided to use IVR for SMA thrombosis. Given the patient’s age, the option of no treatment was also considered. Second point was included for IVR treatment. In my experiences, SMA flow had recovered using continuous arterial infusion under slight peripheral flow when recovered; flow was obtained faster. For this reason, if SMA thrombosis involves complete obstruction, peripheral artery flow is maintained from other arterial flow. In the case of the 100-year-old male, after removing the thrombosis from SMA center, slight flow from the center to the peripheral artery was obtained. Continuous arterial infusion of urokinase would be promising for SMA flow recovery. In this case, it was confirmed that the peripheral flowed from the other artery.
References
- Lassman AB, De Angelis LM. Brain metastases. Neurol Clin N A. 2003; 21: 1-23.
- Posner JB, Chernik NL. Intracranial metastases from systemic cancer. Adv Neuro. 1978; 19: 579- 592.
- Hunter KMF, Rewcastle NB. Metastatic neoplasms of the brainstem. Can Med Ass J. 1968; 98: 1- 7.
- Ginaldi S, Wallace S, Shalen P, Luna M, Handel S. Cranial computed tomography of malignant melanoma. AJR Am J Roentgenol. 1981; 136: 145-149.