Case Report
Prostate Abscess: Prompt Definitive Treatment by Transurethral Unroofing
Michael T Grant*, Seth K Bechis and Michael L Blute
Department of Urology, Massachusetts General Hospital, USA
*Corresponding author: Michael T Grant, Department of Urology, Massachusetts General Hospital, 55 Fruit Street, GRB 1102, Boston, MA 02114, USA
Published: 05 Sep, 2016
Cite this article as: Grant MT, Bechis SK, Blute ML.
Prostate Abscess: Prompt Definitive
Treatment by Transurethral Unroofing.
Ann Clin Case Rep. 2016; 1: 1121.
Abstract
A 50-year-old man undergoing repeat induction chemotherapy for refractory AML had his course complicated by febrile neutropenia. He was diagnosed with a disseminated pseudomonas infection involving the lung and skin. Due to persistent fevers despite antibiotic treatment, computed tomography (CT) imaging was performed which demonstrated a 2cm prostate abscess. This was managed by transurethral unroofing of the abscess in order to eradicate his infection in the most timely manner. The patient recovered well and resumed his chemotherapy regimen two weeks following treatment.
Case Presentation
A 50-year-old man with a history of alcoholism, asthma, was diagnosed with Acute Myeloid
Leukemia (AML) in October 2015. He underwent induction chemotherapy with cytarabine and
daunorubicin, however post-treatment bone biopsy in November 2015 showed refractory disease.
He underwent re-induction with high dose cytarabine and received 7 of 12 planned doses. He
also received dexamethasone at that time and was being evaluated for a stem-cell transplant. He
subsequently developed a high fever (105ºF) with associated hypotension requiring vasopressors.
Labs demonstrated severe neutropenia (WBC 0.02 K/μL). He was immediately started on broad
spectrum antimicrobial coverage.
Upon initial workup of his high fever, he was found to have pulmonary lesions concerning
for organizing pneumonia as well as skin nodules. Induced sputum cultures grew pseudomonas
and mycobacterial alveolar complex. Blood cultures showed pseudomonas bacteremia and biopsies
of cutaneous lesions confirmed disseminated pseudomonas infection. Despite broad antimicrobial
coverage, the patient continued to have high fevers. A CT of the chest, abdomen, and pelvis was
performed to assess the extent of systemic involvement, which revealed a 2cm right sided prostatic
abscess (Figure 1).
At baseline, the patient denied any urinary symptoms, but reported increased frequency,
urgency, and a sensation of incomplete voiding over the past few weeks.
Urology was consulted for definitive management of the prostatic abscess as soon as possible
because the patient could not complete his chemotherapy course or be considered for stem cell
transplant until the systemic infection was eradicated.
The patient was taken to the OR by urology two days later for a transurethral resection of the
prostatic abscess. Digital rectal exam was notable for a smooth, indurated prostate with no bogginess
but tender to palpation. An intra-operative trans-rectal ultrasound (TRUS) was simultaneously performed to assist in localizing the abscess and assessing our depth
of resection to prevent perforation of the prostatic capsule. During
the procedure, thin tissue sweeps were performed using the bipolar
electrocautery resection loop in order to shave down the prostatic
tissue to the level of the abscess (Figure 2A). Once the pseudo capsule
of the abscess was perforated, pressure was applied with the cystoscope
to drain all the purulent fluid from within (Figure 2B). Once drained,
the empty abscess cavity was inspected and the periphery of the
prostate (outer edge of the abscess capsule) was intact (Figure 2C).
The bladder was drained immediately following un roofing of the
abscess in order to collect a specimen to send for bacterial, fungal, and
mycobacterial cultures. An 18Fr 3-way catheter was left in place with
continuous bladder irrigation for 24 hours. Upon catheter removal,
the patient was able to void without difficulty. The prostate abscess
cultures ultimately grew abundant pseudomonas, and the patient was
treated with a 6-week course of oral ciprofloxacin.
Further workup of the pulmonary lesions ruled out an invasive
mycobacterial infection. Two weeks after his TURP, the disseminated
infection improved and the patient was then able to resume
chemotherapy for his AML. He was seen in the urology clinic five
weeks post-operatively, at which time he showed no signs of residual
infection and denied any urinary symptoms. He had a normal digital
rectal exam at that time.
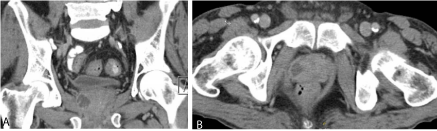
Figure 1
Figure 1
Axial and coronal images of a non-contrast CT scan of the pelvis highlighting the hypoechoic prostatic
abscess.
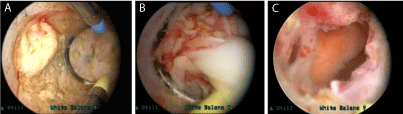
Figure 2
Figure 2
Images from the transurethral resection of the prostatic abscess using bipolar electro-cautery loop. A) After cutting several strips from the prostate, the
abscess tissue can be appreciated bulging into the view. B) Initial unroofing shows release of a large amount of purulent fluid. C) After evacuating the fluid and
debris, the residual empty abscess cavity can be seen.
Discussion
Prostate abscess formation has become a rare condition with the
widespread use of antibiotics; only a handful of case reports or case
series exist over the past several decades [1-7]. Because of the lack
of reliable pathognomonic symptoms, diagnosis of a prostate abscess
can often be delayed. However, it represents a serious infection with
a high mortality rate unless treated properly [1-2]. Therefore, a high
index of suspicion should be held in patients with persistent high
fevers or confirmed systemic infection and any lower urinary tract
symptoms (LUTS), including dysuria, urgency, and urinary frequency.
Risk factors for prostatic abscess include indwelling catheters, recent
urinary tract instrumentation, bladder outlet obstruction, history of
acute or chronic bacterial prostatitis, and an immunocompromised
state. Diagnosis can be confirmed with TRUS, CT, and/or magnetic
resonance imaging (MRI) [1].
The primary treatment for all patients diagnosed with a prostate
abscess is parenteral antibiotics primarily targeting gram-negative
bacteria. E. coli is the most commonly identified bacteria in
prostate infections, representing 65-80% of prostatitis cases. Other gram-negative bacteria such as Pseudomonas aeruginosa, Serratia, Klebsiella, and Enterobacter combine for 10-15% of cases. Grampositive
bacteria such as Staphylocoocus and Enterococcus account for
5-10% of prostate infections; therefore, broad-spectrum antibiotics
should be considered in patients with persistent fevers or severe
infections [2-3].
Our case presents a severely immunocompromised patient with a
known systemic pseudomonas infection and persistent fevers despite
treatment with broad-spectrum antibiotics. He did have urinary
symptoms as well, but this was not elucidated until after the prostate
abscess was discovered on CT imaging.
The decision whether to drain the abscess has traditionally been
based upon the size of the ab-scess, with abscesses >2 cm often being
drained [4]. The efficacy of drainage via transurethral unroofing or
a TRUS-guided needle aspiration is controversial in the literature
and is often based upon abscess location, multifocality, prostate
size, and clinician preference [3,5]. One study of these various
management strategies demonstrated significantly shortened hospital
stays (10 days) with transurethral un roofing when compared with
conservative management (19 days) or needle aspiration (23 days)
[5]. A review of the literature is consistent with this pattern of longer
treatment duration in patients managed conservatively or with needle
aspiration [3-7]. The risks of TURP are perforation of the prostatic
capsule at the time of procedure or delayed complications such as
urethral diverticulum, stricture, or incontinence. Transrectal needle
aspiration carries a higher risk of recurrence in some series, as well as
a risk of rectovesical or rectourethral fistula formation.
Our patient presented with a 2 cm prostatic abscess that was
relatively deep, extending to the prostatic capsule. In addition,
he presented under unique circumstances in that he was undergoing
repeat induction chemotherapy for his refractory AML and
being considered for a stem cell transplant. All treatment had been
halted in the setting of his infection. As such, clearing him of his
pseudomonas infection in the timeliest manner was paramount so
that he could resume his chemotherapy. Therefore, the decision was
made to perform a transurethral un roofing of the abscess. The use of
intra-operative TRUS added significant value in localizing the abscess
and preventing perforation of the prostatic capsule given the depth
of resection that was required. As a result of surgical intervention,
the abscess was maximally drained and the patient’s pseudomonas
infection was cleared in a timely manner, enabling him to resume
chemotherapy within two weeks of his surgery.
Conclusion
This case demonstrates the challenges in diagnosing a prostate abscess as well as the variables that must be considered in choosing how to properly manage the infection such as size, location, and clinical scenario. Here, the patient’s prostate abscess was delaying vital treatment for his refractory AML, and surgical drainage enabled prompt eradication of his infection. Based on our review of the literature, transurethral un roofing of the abscess is highly effective at accomplishing this goal.
References
- Granados EA, Riley G, Salvador J, Vincente J. Prostatic abscess: Diagnosis and treatment. J Urol. 1992; 148: 80-82.
- Ludwig M, Schroeder-Printzen I, Schiefer HG, Weidner W. Diagnosis and therapeutic man-agement of 18 patients with prostatic abscess. Urology. 1999; 53: 340-345.
- Jang K, Lee DH, Lee SH, Chung BH. Treatment of prostatic abscess: case collection and comparison of treatment methods. Korean J Urol. 2012; 53: 860-864.
- Lee DS, Choe H, Kim HY, Kim SW, Bae SR, Yoon BI, et al. Acute bacterial prostatitis and abscess formation. BMC Urology. 2016; 16: 38.
- Elshal AM, Abdelhalim A, Barakat TS, Shaaban AA, Nabeeh A, Ibrahiem E-H. Prostatic ab-scess: Objective assessment of the treatment approach in the absence of guidelines. Arab J Urol. 2014; 12: 262-268.
- Scorey H, Daniel S. Nocardia farcinica bacteraemia presenting as a prostate abscess. ID-Cases. 2016; 5: 24-26.
- Gan E. Transrectal ultrasound-guided needle aspiration for prostatic abscesses: an alternative to transurethral drainage?. Tech Urol. 2000; 6: 178-184.