Case Report
Intestinal Ischemia after the Use of Terlipressin for Variceal Bleeding in a Patient with Primary Biliary Cirrhosis: A Case Report
Parmentier-de-Leon C, Gonzalez-Romero F, Beristain-Hernandez JL*
Department of General Surgery, La Raza National Medical Center, Mexico
*Corresponding author: José-Luis Beristain-Hernandez, Department of General Surgery, Hospital de Especialidades. La Raza National Medical Center. Mexico City, 02990, Mexico
Published: 20 Jun, 2016
Cite this article as: Parmentier-de-Leon C; GonzalezRomero
F, Beristain-Hernandez JL.
Intestinal Ischemia after the Use of
Terlipressin for Variceal Bleeding in a
Patient with Primary Biliary Cirrhosis: A
Case Report. Ann Clin Case Rep. 2016; 1: 1020.
Abstract
Primary biliary cirrhosis is a chronic cholestatic liver disease characterized by destruction of small intrahepatic bile ducts, leading to fibrosis and potential cirrhosis through resulting complications. Approximately half of the patients with cirrhosis have gastroesophageal varices and one-third of all patients with varices will develop acute variceal hemorrhage. Vasopressin is a potent vasoconstrictor of both systemic and splanchnic circulation, one of the only vasoactive compounds, which have been approved by regulatory agencies for the treatment of bleeding esophageal varices. Only 3 cases of intestinal ischemia have been reported, with this paper we report a fourth.
Keywords: Primary biliary cirrhosis; Terlipressin; Intestinal ischeamia; Variceal bleeding; Vasopressin
Core Tip
In this paper we present a case of intestinal ischemia after the use or terlipressin in a patient with variceal bleeding secondary to primary biliary cirrhosis. Only 3 cases have been reported previously in the literature
Introduction
Primary biliary cirrhosis is a chronic cholestatic liver disease characterised by destruction of small
intrahepatic bile ducts, leading to fibrosis and potential cirrhosis through resulting complications.
The serological hallmark of primary biliary cirrhosis is the antimitochondrial antibody, a highly
disease-specific antibody identified in about 95% of patients with primary biliary cirrhosis [1].
Approximately half of the patients with cirrhosis have gastroesophageal varices and one-third
of all patients with varices will develop acute variceal hemorrhage, a complication that still carries a
mortality of up to 15% to 20% [2].
Vasopressin is a potent vasoconstrictor of both systemic and splanchnic circulation [2], one of
the only vasoactive compounds, which have been approved by regulatory agencies for the treatment
of bleeding esophageal varices [3]. Terlipressin is a synthetic analogue of vasopressin, which causes
vasoconstriction of splanchnic vessels and improves impaired renal function. Terlipressin is
associated with a much lower incidence of ischemic complications compared with vasopressin, but
it may still cause such problems [4]. The most common side effect is abdominal pain. The overall
efficacy of terlipressin in controlling acute variceal hemorrhage is 75% to 80% at 48 hours and of
67% at 5 days [2].
In a review by Krag et al. [5] of several clinical trials which included 1079 patients treated with
terlipressin for variceal bleeding (798 patients) or hepatorrenal syndrome (281 patients), there were
only 2 cases of nonfatal myocardial infarction during treatment with terlipressin in patients with
variceal bleeding. Seven patients developed skin reactions. In this review there were only 3 case
reports on intestinal ischemia. However we found another by Kim et al which describes severe
ischemic bowel necrosis caused by terlipressin in a 46 year old man.
Case Report
Patient is a 37-year-old female with a previous history of primary biliary cirrhosis, diagnosed two
years ago (acute upper gastrointestinal bleeding, elevated alkaline phosphatase and antimitochondrial
antibodies, no liver biopsy required). After that first episode of variceal bleeding, she presented
another three episodes, all treated with variceal banding. She was
also treated with beta blocker (propranolol), ursodeoxycholic acid,
spironolactone and folic acid.
She complained of fatigue 48 hours prior to admission, and 24
hours later, she presented melena and hematochezia in multiple
ocasions. She was admitted to our hospital under the care of the
gastroenterology department where treatment with terlipressin (2
mg every 4 hours) was initated. The second day after her arrival,
she presented abdominal pain, inmmediately after her last dose
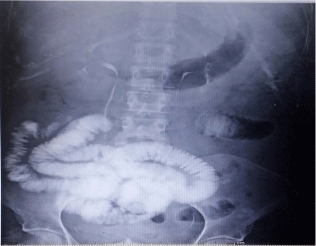
of terlipressin. A consultation to our department was made. Upon
examination, she presented with signs of acute abdomen and
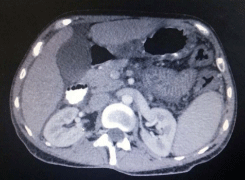
tachycardia, abdominal radiography revealed a stack of coin image
(Figure 1), CT scan revealed bowel loop dilation (Figure 2), and
her hemoglobine levels went from 9.8 mg/dL to 6.1 mg/dL in less
than 24 hours, she also presented hypoalbuminemia (1.7 g/dL) and
hyperbilirubinemia (Total, 3.74 mg/dL; direct 2.57 /dL).
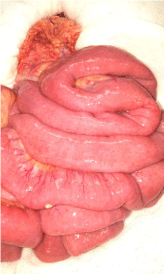
Under the suspicion of acute mesenteric ischemia we decided to
perform an exploratory laparotomy, finding small intestine ischemia,
with mesenteric pulse and peristalsis and no signs of intestinal
necrosis observed (Figure 3). Because of these findings, we decided
to close up the abdomen and perform a second look surgery 48 hours
later. In the meantime the terlipressin was suspended and she was
treated with IV fluids. During those 48 hours endoscopic banding of
varices was performed and treatment with a low molecular weight
heparin was initiated. Second look surgery was performed, observing
a complete remission of intestinal ischemia, she still presented
adecuate mesenteric pulse and peristalsis (Figure 4). No small bowel
resection was necessary.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
In this case report we present a new case of intestinal ischemia
associated with the use of terlipressin, which serves to prove that
although it is the initial drug of choice for variceal bleeding whenever
available, ischemic complications can still present. The most common
ones being skin complications [5] However complications in the
gastrointestinal system can prove to be fatal [4]. Whenever a patient
is treated with this medication close monitoring is necessary and
its use must be suspended immediately if the patient complains of
abdominal pain.
According to a study conducted between 2007 and 2008 which
included 122 patients with variceal bleeding the combination of
variceal banding in the first 12 hours and the use of terlipressin are the
best treatment with better hemodynamic stability, less transfusions
and no difference in mortality at 48 hours and 30 days [6].
References
- Carey EJ, Ali AH, Lindor KD. Primary biliary cirrhosis. Lancet. 2015; 386: 1565-1575.
- Bhutta AQ, Garcia-Tsao G. The Role of Medical Therapy for Variceal Bleeding. Gastrointest Endosc Clin N Am. 2015; 25: 479-490.
- Döhler KD, Meyer M. Vasopressin analogues in the treatment of hepatorenal syndrome and gastrointestinal haemorrhage. Best Pract Res Clin Anaesthesiol. 2008; 22: 335-350.
- Kim HR, Lee YS, Yim HJ, Lee HJ, Ryu JY, Lee HJ, et al. Severe ischemic bowel necrosis caused by terlipressin during treatment of hepatorenal syndrome. Clin Mol Hepatol. 2013; 19: 417-420.
- Krag A, Borup T, Møller S, Bendtsen F. Efficacy and safety of terlipressin in cirrhotic patients with variceal bleeding or hepatorenal syndrome. Adv Ther. 2008; 25: 1105-1140.
- López-Martínez S, Moreno-Portillo M, González-Angulo A, BeristainHernández JL, Fernández-Castro E, Romero-Loera LS, et al. Combined endoscopic variceal banding with Terlipressin in acute variceal bleeding. Endoscopia. 2010; 22: 178–184.