Case Report
Isolated Trochlear Nerve Palsy in Post Traumatic Brain Injury: Incidental Detection Using Vestibular Screening Tests
Tay KWE* and Chua SGK
Department of Rehabilitation Medicine, Tan Tock Seng Hospital Rehabilitation Centre, Singapore
*Corresponding author: Tay KWE, Department of Rehabilitation Medicine, Tan Tock Seng Hospital Rehabilitation Centre, 17 Ang Mo Kio Ave 9, Singapore
Published: 30 Jun, 2018
Cite this article as: Tay KWE, Chua SGK. Isolated
Trochlear Nerve Palsy in Post Traumatic
Brain Injury: Incidental Detection Using
Vestibular Screening Tests. Ann Clin
Case Rep. 2018; 3: 1531.
Abstract
Isolated trochlear Nerve Injury (TNI) following Traumatic Brain Injury (TBI) is uncommon. There
are diagnostic challenges in the early detection of isolated TNI and there is currently no agreed
screening tool for its diagnosis. We report a 30 year-old gentleman with severe TBI, who was detected
to have diplopia during routine screening vestibular tests. He was subsequently diagnosed to have
isolated TNI following a positive Bielschowsky head tilt test. This was managed conservatively and
his symptom of diplopia improved 5 months following head injury.
Keywords: Traumatic brain injury; Trochlear nerve injury; Vestibular screening tests
Introduction
Cranial Nerve (CN) injury is a potential complication of TBI [1]. However, unilateral traumatic
lesion of trochlear nerve is relatively uncommon [2] and its incidence has been reported between
0.23% to 13% [1,3-5]. Previous studies have suggested that CNs I, VII, VIII and in particular the
olfactory nerve; are most frequently injured after TBI [6].
The diagnosis of CN injury after TBI can be challenging. Several TBI patients suffer from
altered consciousness, agitation, cognitive problems like attention and visuospatial deficits. They
also sustain neurological deficits like aphasia and neglect, making it difficult for history taking and
physical examination. The clinician has to differentiate CN neuropathies from vestibular ocular
dysfunction, as both can present with diplopia and dizziness.
Currently, there is no consensus on the diagnosis and treatment of CN injury post TBI [1]. We
report a case of post TBI related TNI in which the diagnosis was provoked on routine vestibular
screening.
Case Report
A 30-year-old Chinese male with no past medical history sustained severe TBI after falling
approximately 3.5 meters from a rooftop glass panel while at work. Glasgow Coma Scale (GCS) score
was 15 on arrival to the emergency department. Initial Computed Tomography (CT) brain revealed
acute subarachnoid haemorrhage along sulci of the left frontal lobe with contusion over the left
temporal lobe. There was no evidence of skull vault fracture or raised intracranial pressure (Figures
1A and1B). His TBI was managed conservatively. His GCS score remained 15 throughout his acute
neurosurgical stay. He also sustained a right clavicular fracture which was managed conservatively.
He was transferred to an inpatient rehabilitation facility after 2 weeks post TBI.
Initial physical examination did not reveal any focal neurological signs and motor power was
full throughout. Using the West mead Post Traumatic Amnesia (PTA) scale [7], daily recordings
showed that his PTA duration was 21 days. Initial PTA score was 3 out of 7.
A few days following admission, he complained of giddiness with diplopia. The diplopia was
described as binocular with a vertical component and was persistent throughout the day but
worsened with downward gaze. It resolved on unilateral occlusion. On further examination, he had
diplopia on downward gaze but there was no obvious loss of in torsion, depression and adduction
of his eyes. Examination of his other CNs, motor power, limb ataxia, gait and balance were normal.
To rule out vestibular-ocular causes for giddiness, vestibular screening was done during a
physiotherapy session. Both Dix-Hallpike and Supine Log Roll tests were negative. However, his diplopia was significantly worse on left head tilt during both tests.
He was subsequently referred to the ophthalmologist and found
to have a positive Bielschowsky head tilt test on left head tilt. He was
diagnosed to have left isolated superior oblique nerve palsy from TNI.
This was managed conservatively.
He was discharged from the rehabilitation centre at 5 weeks post-
TBI requiring supervision in ambulation and basic activities of daily
living. He had some residual deficits in memory and abstract thinking
at time of discharge. There was no noticeable recovery of his left
superior oblique nerve palsy during inpatient stay. During outpatient
follow-up at 5 months post injury, he had persistent left TNI with
a positive Bielschowsky head tilt test but his symptoms of diplopia
improved significantly.
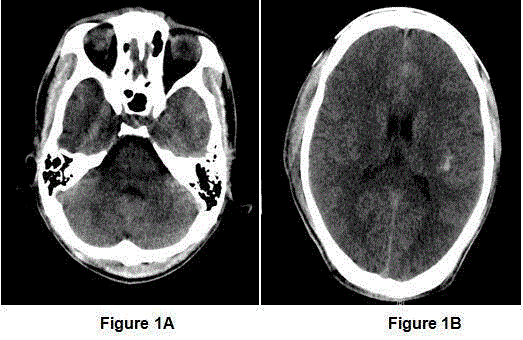
Figure 1
Figure 1
CT brain revealed acute subarachnoid haemorrhage
along sulci of the left frontal lobe with contusion over the left temporal lobe
and bifrontal scalp swelling. There was no evidence of any skull vault fracture
or raised intracranial pressure.
Discussion
Epidemiology and aetiology
The most common acquired cause of TNI is trauma [8]. TBI
accounts for approximately one third of cases with trochlear nerve
palsy [9]. The incidence of TNI in TBI patients ranges from 0.23%
to 13% [1,3-5]. In one study involving retrospective analysis of 31
TBI patients, the incidence of TNI was3.2% [3]. In another study
evaluating 3417 patients after head injury, 0.23% of patients had
isolated TNI [1].
Studies have shown that most patients with TNI have moderate to
severe TBI [9] and this is consistent with TBI in this patient since his
PTA was 21 days, in spite of a normal GCS of 15, indicative of severe
TBI. PTA duration is used as an index of TBI severity. PTA is defined
as inability to lay down memories from one day to the next, and is
assessed subjectively [7]. The duration of PTA is defined as the period
from time of injury until return of continuous memory. However,
there is evidence that traumatic TNI can also occur with mild TBI [2].
Other causes of acquired trochlear nerve palsy include vascular,
neoplastic or inflammatory diseases, which are less common than
traumatic causes [10].
TNI and TBI
The trochlear nucleus is located at the inferior colliculus,
ventrolateral to the cerebral aqueduct [9]. The fibres pass to decussate
in the superior medullary velum [9]. It courses around the midbrain’s
lateral aspect, passes between the posterior cerebral and superior
cerebellar arteries and courses along the tentorium cerebelli [9]. It
subsequently pierces the dura to near the cavernous sinus and enters
the superior orbital fissure 9
The trochlear nerve supplies only the superior oblique muscle.
The muscle’s functions include intorsion, depression and abduction.
The trochlear nerve is susceptible to injury after TBI due to its
long intracranial course (75mm) and thin structure [2,9]. The rigid
tentorium lies next to the trochlear nerve where it can be easily
compressed [2].
Most traumatic TNI are associated with midbrain parenchymal
contusions and hematomas following impact of midbrain against the
tentorium, as well as injury in the cisterns along the nerve’s extraaxial
course [4].
Other mechanisms include orbital fractures or frontal or orbital
impact causing a contusion against the trochlear nerve’s attachment
at the medullary velum [2,9]. This patient had extensive bilateral
frontal scalp swelling which could suggest a significant impact on his
forehead possibly leading to TNI.
This patient also had left frontal lobe injury and diffuse traumatic
subarachnoid haemorrhage which were likely causative mechanisms
for TNI. No midbrain lesions were seen on CT brain.
Clinical presentation and investigation
In subjects with TNI who complain of diplopia, this is often
vertical and torsional; and worse on downward gaze and gaze away
from side of affected muscle. Reading or walking down stairs often
worsens diplopia due to the downward head position [2]. Patients can
have torticollis to the side of the unaffected eye with depressed chin.
This is a compensatory head posture to place the unaffected eye in the
position of least deviation [2].
There is a lack of literature on the diagnosis of TNI after TBI
[9]. TNI can be difficult to assess and are frequently missed because
the patient’s eye position may appear normal with compensatory
measures from other recti muscles [2]. TBI patients suffer from
reduced sensorium, altered consciousness, agitation, cognitive
deficits hence leading to under-reporting of symptoms of diplopia
and delays in the diagnosis and treatment of TNI. This patient had
reduced attention at the beginning of admission.
Hypertropia can occur greatest in adducted depression position
of involved eye, more pronounced in unilateral TNI [9]. Other
examination includes the Bielschowsky head tilt test, where there is
hyperdeviation of the affected eye when the patient’s head is tilted
to the affected eye. This is positive in 90% of TNI patients [9]. Other
clinical tests include the Parks’ three step diagnostic technique
[11] and tests for cyclotropia like the Moaddox double prism and
Lancaster-Hess-Lees tests [9]. Another test is the vertical saccadic
velocity determinations which will reveal slowing down saccades in
the adduction position in TNI patients [9].
In this patient, diplopia was worsened during vestibular
screening tests with Dix-Hallpike and Supine Log Roll Screening
Tests. It is possible that during these tests, the patient’s head position
is manipulated in a manner that mimicked the Bielschowsky head
tilt test, resulting in torsional movements of the eyes, thereby
accentuating his TNI symptoms.
A confirmatory radiological diagnosis for TNI is thus far
challenging as there are only a few cases where a brain stem lesion
was detected [12]. Nevertheless, magnetic resonance imaging brain is
the modality of choice for further investigation when initial CT does
not indicate neurological damage for symptomatic patients with TNI.
Management and prognosis
There is a lack of consensus on management of ocular motor
nerve palsies after TBI [3]. Management of traumatic isolated
trochlear nerve palsy can include measures to overcome diplopia.
These include the use of prisms and eye patch for symptomatic relief
[2]. There is usually a 6 month period post injury where the patient’s
condition is observed for any spontaneous recovery, before surgical
intervention is considered [2]. Steroids use in terms of dosage,
duration and efficacy for traumatic TNI has not been well studied [3].
One study has evaluated the use of galantamine in the treatment of
traumatic oculomotor palsies or TNI in 5 patients [13].
The trochlear nerve has the highest rate of recovery amongst the
ocular motor nerves and at least 50% of patients recover [9]. Recovery
time is an average of 10 weeks and ranges from 1 week to 6 months
[9].
Conclusion
Isolated TNI be easily missed in TBI patients due to its subtle
clinical findings. Early detection of CN palsies may positively impact
patient’s rehabilitation progress, functional independence and quality
of life.
This case illustrates the incidental use of vestibular screening
manoeuvres to provoke diplopia associated with isolated TNI,
which subsequently facilitated an early referral to ophthalmology
for definitive diagnosis. Vestibular screening manoeuvres are easy to
perform, safe and require minimal training. There is a need for further
research with regard to the utility of vestibular test manoeuvres to
screen for isolated TNI post TBI, evaluation of prognostic factors and
specific interventions to improve spontaneous recovery from posttraumatic
TNI.
References
- Jin H, Wang S, Hou L, Pan C, Li B, Wang H, et al. Clinical treatment of traumatic brain injury complicated by cranial nerve injury. Injury. 2010;41(9):918-23.
- Ruediger L, Majetschak M. Traumatic unilateral trochlear nerve palsy. J Trauma. 2007 Jun;62(6):E1-3.
- Guichen L, Xiaobo Z, Xiuhong G, Yang S, Xiangfeng G, Yang Z, et al. Ocular movement nerve palsy after mild head trauma. World Neurosurgery. 2016;94:296-302.
- Ventura RE, Balcer LJ, Galetta SL. The neuro-ophthalmology of head trauma. Lancet Neurol. 2014;13(10):1006-16.
- Coello AF, Canals AG, Gonzalez JM, Martín JJ. Cranial nerve injury after minor head trauma. J Neurosurg. 2010;113(3):547-55.
- Chung SM, Fenton GA, Schmidt JG, Selhorst JB. Trauma to the cranial nerves and brainstem. Neurotrauma. 1996;621-38.
- Shores EA, Marosszeky JE, Sandanam J, Batchelor J. Preliminary validation of a scale for measuring the duration of post-traumatic amnesia. Med J Aust. 1986;144(11):569-72.
- Richards BW, Jones FR, Younge BR. Causes and prognosis in 4,278 cases of paralysis of oculomotor, trochlear and abducens cranial nerves. Am J Ophthalmol. 1992;113(5):489-96.
- Mansour AM, Reinecke RD. Central Trochlear Palsy. Surv Opthalmol. 1986;30(5): 279-97.
- Bixenman WW. Diagnosis of Superior Oblique Palsy. J Clin Neuroophthalmol. 1981;1(3):199-208.
- Parks MM. Isolated cyclovertical muscle palsy. Arch opthalmol. 1958:60(8):1027-35.
- Keane JR. Trochlear nerve pareses with brainstem lesions. J Clin Neuroophthalmol. 1986;6(4):242-6.
- Tokarz-Sawińska E, Lachowicz E, Gosławski W. The use of galantamine in the treatment of post-traumatic oculomotor and trochlear nerve palsy. Klin Oczna. 2013;115(4):275-9.