Case Report
18F FDG PET/CT in Extrapulmonary Sarcoidosis
Gupta Khushboo,* and Jadhav Rahul
*Corresponding author: Gupta Khushboo, Department of Radiology and Nuclear Medicine, Rush university Medical Center, Center, 1653, Congress Pkwy, Chicago, 60612, Illinois, USA
Published: 16 Jun, 2018
Cite this article as: Gupta Khushboo, Department of
Radiology and Nuclear Medicine, Rush
university Medical Center, Center,
1653, Congress Pkwy, Chicago, 60612,
Illinois, USA
Abstract
Sarcoidosis is a chronic granulomatous disease and may present with multisystemic involvement.
Hepatic involvement is one of the most common extra-pulmonary diseases and was described as
11.5% in cohort studied in ACCESS study. In such cases early diagnosis is the key to early installment
of specific therapy. This may not only improve the prognosis but may also salvage the possible system
failure. Routine radiological investigation is generally sufficient to make a diagnosis, however, rare
case presentations may require further evaluation to assess extent of extra-pulmonary disease
involvement. FDG PET/CT demonstrates high grade glucose avidity in active granulomatous lesions
and hence can be used for this purpose. Additionally, it also enables determination of treatment
response. In this case report we describe a relapse case of pulmonary sarcoidosis, diagnosed to have
liver and spleen involvement on FDG PET/CT scan which was confirmed on histopathology.
Keywords: 18F FDG PET/CT; Sarcoidosis; Extrapulmonary; Hepatic; Granulomatous disease
Introduction
Sarcoidosis is a systemic granulomatous disease of unknown etiology. Extra-pulmonary
sarcoidosis is known to occur and may involve multiple organs, such as skin, bone marrow,
liver, spleen, muscles, etc. Hepatic sarcoidosis alone involves about half the cases [1]. FDG PET/
0CT demonstrates high grade glucose avidity in active granulomatous lesions [2] and hence can
be used for diagnosis of extra-pulmonary extent of disease as well as treatment response. In this
case report we describe a relapse case of pulmonary sarcoidosis, demonstrating liver and spleen
involvement on FDG PET/CT scan which was confirmed on histopathology. Case Report: A 51year
old postmenopausal lady presented with fever, weight loss, decreased appetite and generalized
weakness since a month. She had past history of sarcoidosis for which she was treated with steroids.
Her recent Angiotensin Converting Enzyme (ACE) values were high. Contrast enhanced CT scan
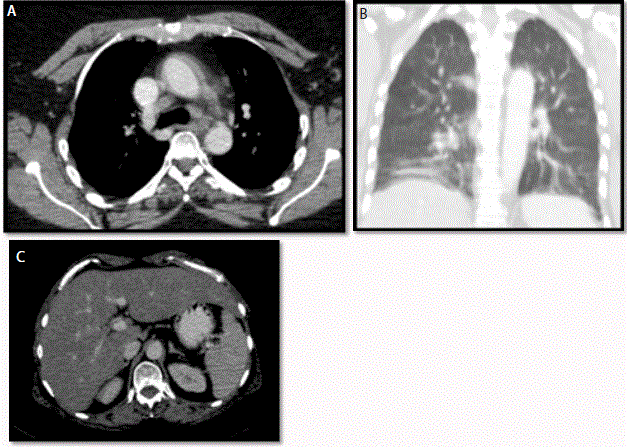
(chest, abdomen and pelvis) was suggestive of discrete sub-centimeter mediastinal and hilar lymph
nodes (Figure 1A), mild interstitial fibrosis in both lungs (Figure 1B) and mild hepatosplenomegaly
with fatty infiltration (Figure 1c).
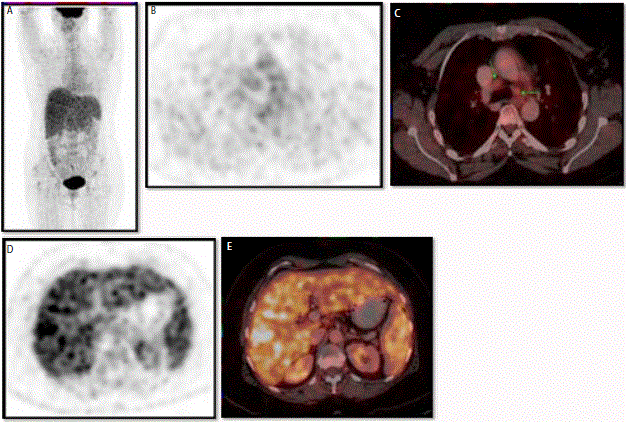
FDG PET-CT whole body scan (Figure 2A) demonstrated moderate increased metabolic activity
in mediastinal lymph nodes (Figure 2B and 2C). There was heterogeneous increased tracer uptake
in entire liver and spleen parenchyma with high grade FDG avidity (Figure 2D and 2E). In clinical
context of raised ACE, findings were concerning for granulomatous disease involvement and liver
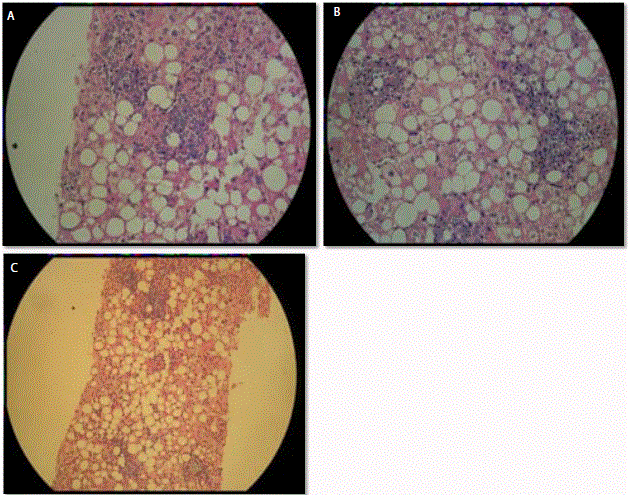
biopsy was suggested. Histopathology revealed distortion of normal lobular and cord pattern of
liver cells, swollen hepatocytes with marked macro vesicular steatosis, composed of epitheloid
histiocytes, neutrophils, few eosinophils and occasional multinucleate giant cells. Fibrin deposition
was also evident within granulomas (Figure 3A-3C); findings suggestive of multiple non-caseating
hepatic micro-granulomas.
Discussion
Extra-pulmonary sarcoidosis is not uncommon, although it is almost always found with
concomitant thoracic involvement [3]. Frequently extra-pulmonary manifestations of the
disease are the major cause of morbidity. Treatment often requires consideration of alternative
immunosuppressive agents and specific consideration towards the organ system involved [4].
Liver and spleen are the most frequently involved viscera, with presence of non-caseating
granulomata noted in 40% to 70% of cases [1]. Patients with liver disease may be asymptomatic
or may progress to chronic cholestases and portal hypertension. In few cases, this may lead to
hepatic failure. When hepatic failure ensues, it is difficult to revert the changes and the patient may
require transplant. Hence, complete systemic evaluation for extra-pulmonary organ involvement is
imperative. Multiple imaging modalities are used, especially CT scan, for non-invasive diagnosis.
However, in most studies (and so in present case study), the liver is
homogeneous in appearance and hypo-attenuating nodules are rarely
seen [1].
FDG PET scans, on the other hand, shows high sensitivity in
localizing granulomatous pathogenesis [2]. The uptake mechanism
depends on number of glucose transporters expressed on cell surface.
In case of infection/inflammation, activated inflammatory cells have
increased expression of glucose transporters. Also, the affinity of
these transporter for deoxyglucose increases by various circulating
cytokines and growth factors [5,6]. This determines localization of
FDG in infective sites. There are other areas demonstrating increase
FDG uptake in setting of infection/ inflammation, such as bone
marrow, spleen and thymus (in children and adolescents). These areas
are integral part of immune system and are involved in production
of inflammatory substances, antibodies and immunoglobulins. FDG
uptakes in these areas are usually low grade and diffuse as compared
to focalized uptake in area of infection. In case of Sarcoidosis, FDG
PET scan helps in determining pulmonary and extra-pulmonary
extent of disease and type of therapy to be instituted [7]. The degree of
FDG uptake also correlates with disease activity and could be used for
treatment monitoring and response purposes [8]. In above presented
case, pattern of high glucose metabolism in liver and spleen on FDG
PET scan in light of raised serum ACE levels largely favored hepatic
sarcoidosis. Such pattern recognition may benefit the clinicians to
establish a better treatment protocol at an early stage.
Figure 1
Figure 1
CECT (chest, abdomen and pelvis): demonstrate discrete sub
centimeter mediastinal and hilar lymph nodes (transaxial image Figure
1A), mild interstitial fibrosis in both lungs (coronal image Figure 1B),
hepatosplenomegaly with fatty infiltration in hepatic parenchyma (transaxial
image Figure 1C).
Figure 2
Figure 2
18F FDG PET/CT Whole body images (MIP Figure 2A) demonstrate
moderate grade activity in mediastinal nodes (dedicated PET scan transaxial
image Figure 2B and fused PET-CT transaxial Figure 2C). High grade
heterogeneous FDG activity in entire liver and spleen (dedicated PET scan
transaxial image Figure 2D and fused PET-CT transaxial Figure 2E).
Figure 3
Figure 3
Microsopy (Figure 3A, 3B and 3C) showed distortion of normal
lobular and cord pattern. Swollen hepatocytes with marked macrovesicular
steatosis and central fat vacuole. These appear composed of epitheloid
histiocytes, neutrophils, few eosinophils and occasional multinucleate giant
cells. Fibrin deposition was evident within granulomas. Portal and peri-portal
fibrosis was present.
Conclusion
Involvement of extra-pulmonary sites in cases of Sarcoidosis often requires aggressive treatment approach. Since this has an influence on prognosis, FDG PET/CT scan can serve as a single step valuable tool in Sarcoidosis evaluation.
Teaching Point
Increased glucose metabolism in liver and spleen, on FDG PET scan, have varied differential diagnosis including diffuse liver disease like cirrhosis, granulomatous disease, metastases and primary malignancy such as lymphoma. Understanding the pattern of uptake may lead to narrow the diagnosis and could be further confirmed on specific laboratory and histopathologic investigation.
References
- Warshauer DM, Lee JK. Imaging manifestations of abdominal sarcoidosis. AJR Am J Roentgenol. 2004;182 (1):15-28.
- Hess S, Hansson SH, Pedersen KT, Basu S, Høilund-Carlsen PF. FDGPET/ CT in Infectious and Inflammatory Diseases. PET Clinics. 2014;9(4): 497-519.
- Design of a case control etiology study of sarcoidosis (ACCESS). J Clin Epidemiol. 1999;52(12):1173-86.
- Judson MA. Sarcoidosis: Clinical presentation, diagnosis, and approach to treatment. Am J Med Sci. 2008;335(1):26-33.
- ZhuangH, Alavi A. 18-fluorodeoxyglucose positron emission tomographic imaging in the detection and monitoring of infection and inflammation. Semin Nucl Med. 2002; 32(1): 47-59.
- PaikJY, Lee KH, Choe YS, Choi Y, Kim BT. Augmented 18F-FDG uptake in activated monocytes occurs during the priming process and involves tyrosine kinases and protein kinase C. J Nucl Med. 2004; 45(1): 124-8.
- Braun jj, Kessler R, Constantinesco A, Imperiale A. 18F-FDG PET/CT in sarcoidos is management: Review and report of 20 cases. Eur J Nucl Med Mol Imaging. 2008;35(8):1537-43.
- Brudin LH, Valind SO, Rhodes CG, Pantin CF, Sweatman M, Jones T, et al. Fluorine-18 deoxyglucose uptake in sarcoidosis measured with positron emission tomography. Eur J Nucl Med. 1994;21(4): 297-305.