Case Report
Diffuse Cutaneous Mastocytosis
Gerda Petersone1*, Sanita Zigure1,2 and Aleksejs Zavorins1
1Department of Dermatology, Riga Stradin’s University, Lativa
2Children’s Clinical University Hospital Riga, Lativa
*Corresponding author: Gerda Petersone, Department of Dermatology, Riga Stradin’s University, Lativa
Published: 25 May, 2018
Cite this article as: Petersone G, Zigure S, Zavorins A.
Diffuse Cutaneous Mastocytosis. Ann
Clin Case Rep. 2018; 3: 1511.
Abstract
Mastocytosis is a group of disorders characterized by abnormal accumulation of mast cells in the skin and other organs. Diffuse cutaneuos mastocytosis is a rare and most severe variant of cutaneous mastocytosis. In this article, we present you a girl with urtical elements on her skin folds, abdomen and axillae since she was 4 month old that progressed into generalized vesiculobullos rash with positive Darrier’s sign. Based on clinical, histological and laboratorial findings the diagnosis of diffuse cutaneous mastocytosis was made at the age of 6 months. Treatment was started at age of 4 months with cetirizine, after the diagnosis was made we increased dose four times, later desloratadine, topical zinc preparations, topical pimecrolimus, montelukast was added but there was no therapeutical effect so at age of 7 months she started therapy with oral glucocorticosteroids. At age of 17 months she started oral cromolyn sodium. This is the first case of DCM in Children’s Clinical University hospital Riga as far as we know.
Introduction
Mastocytosis refers to a heterogeneous group of disorders characterized by the pathologic
accumulation of mast cells in different tissues or organs, predominantly skin, bone marrow, and
visceral organs [1]. Mastocytosis is divided in two main subgroups, Systemic Mastocytosis (SM) and
Cutaneous Mastocytosis (CM) [2]. CM is classified into mastocytoma, maculopapular cutaneous
mastocytosis or urticaria pigmentosa, telangiectatic cutaneous mastocytosis and diffuse mastocytosis
[2-4]. Diffuse Cutaneous Mastocytosis (DCM) is a rare, severe variant of CM, it accounts about 1% to
3% of the cases of CM [2,4]. DCM appears in neonates or in the first month of life and is characterized
by intense symptoms due to increased cutaneous infiltration by mast cells [5]. The first sign may be
blistering and extensive bullae, which may rupture, leaving erosions and crusts. The blisters can be
hemorrhagic. The skin may be leathery and thickened, hyperpigmented. Systemic symptoms, such
as body flushing, pruritus, diarrhea, intestinal bleeding, hypotension, anemia, hypovolemic shock,
can be present due to the large amount of mast cell mediators released locally and absorbed locally
and systemically. Visceral involvement with lymphadenopathy and hepatomegaly may be present.
Rarely, all cutaneous forms of mastocytosis in children can present with acute mast cell activation
events, including anaphylaxis. [4,6]. Mechanical irritation of skin lesions leads to a release of mast
cell mediators (histamine, leukotrienes and prostaglandins) and thus to reddening and urticarial
swelling. This reaction is known as Darier's sign and is pathognomonic for all forms of CM [4,7].
Pruritus and flushing can be triggered by many factors, for example, temperature changes, hot
showers, emotional stress, spicy food, fever, exercise, friction, and certain drugs [4]. Mastocytosis is
also associated with a number of comorbidities such as osteoporosis, gastric and duodenal ulcers,
recurrent anaphylaxis and hematologic disorders such as myeloproliferative or myelodysplastic
disorders and rarely lymphoproliferative disorders [8].
Unfortunately, there is no standardized treatment for mastocytosis and treatment consists
primarily of symptomatic drugs and other treatments that deal with the symptoms experienced by
individual patients [2].
Case Presentation
A 4 month old girl developed urticarial elements on her skin folds, abdomen and axillae. She
was treated by a local dermatologist with cetirizine, nevertheless after a month she developed
generalized vesiculobullous rash. The bullae where flaccid, ruptured easily leaving crusts. When she
was 5 month old, she was admitted to a hospital where she was seen for the first time by the authors
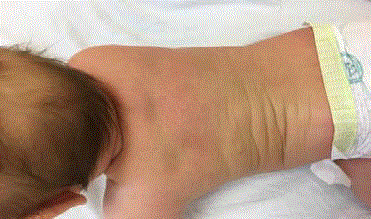
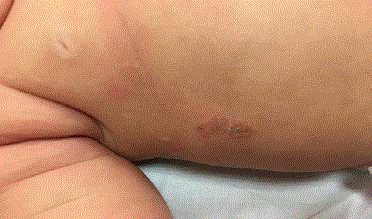
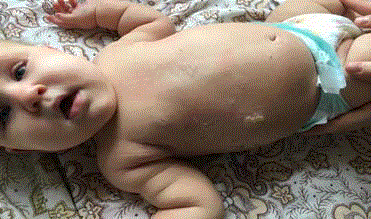
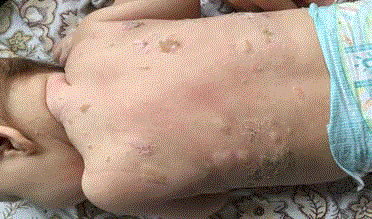
of this article. During physical examination urticarial elements on her back and skin folds were
noted. Yellowish crusts covering erosions secondary to ruptured bullae were observed (Figure 1 and
2). Darrier’s sign was positive: upon stroking the back, the patient developed an urticarial reaction.
Palpation and percussion revealed possible hepatomegaly. Her
parents admitted that the girl seemed to be anxious for the past few
weeks. She woke up several times every night and the skin conditions
worsened when she was stressed.
Laboratory examination revealed thrombocytosis and elevated
serum tryptase level 129 ng/ml. Further investigations were
undertaken to exclude systemic mastocytosis.
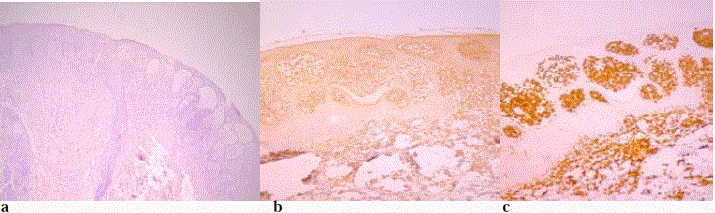
Skin biopsy was performed. The histopathological diagnosis fits
with bullous mastocytosis (Figure 3a-3c). The day after skin biopsy
the patient developed reddish papules, urticarial plaques and new
bullous lesions (Figure 4).
Ultrasound examination of the abdominal cavity confirmed
hepatosplenomegaly. Computer Tomography (CT) of the thorax
demonstrated small, subpleural cysts. Bone marrow biopsy
excluded prominent mast cell infiltration. However there was
massive lymphocytosis without atypia, hyperplasia of neutrophils.
Hematologist recommended periodical observation, no other
intervention was needed.
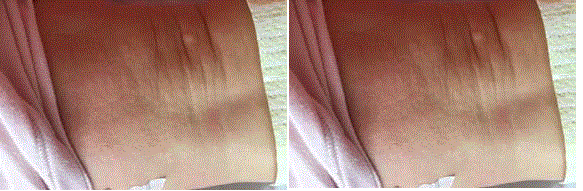
A day after bone marrow biopsy the disease exacerbated.
Generalized vesicobullous rash developed (Figure 5 and 6).
The patient started her therapy with cetirizine at the age
of 4 months. After a month the dosage increased four times.
Afterwards desloratadine, montelukast, topical zinc preparations
and pimecrolimus cream were added. The parents were consulted
about the necessity to avoid disease triggers and given instructions
on the use of the Epinephrin injector. The girl was refractory to the
prescribed therapy. The disease progressed. New bullae developed
almost every day. Therefore, it was decided to initiate systemic
methylprednisolone 1 mg/kg (12 mg) therapy at age of 7 months.
There was good therapeutic response. Bullae formation ceased, even
though the Darrier’s sign remained positive. Abdominal ultrasound monitoring was repeated in a month and no hepatosplenomegaly was
seen. The methylprednisolone was tapered to the minimal effective
dose of 4 mg of methylprednisolone once in three days. Each time
it was tried to tapper or cancel the therapy bullae broke out. At the
age of 17 months oral cromolyn sodium 20 mg/kg was added and
methylprednisolone was canceled. Comely sodium is not widely
available in Latvia, so it was ordered from United Kingdom. At the
moment the patient has been receiving oral therapy with cromolyn
sodium for 3 months. During this period the Darrier’s sign is still
positive and her mother observed development of cutaneous bullae
for 3 times.
Figure 1
Figure 2
Figure 3
Figure 3
Histopathology shows minimal orthokeratosis in epidermis and acanthosis. Monomorphic mast cells with round and oval, hyperchromatic nuclei
and eosinophilic cytoplasm are located in the dermis. Giemsa staining demonstrates multiple small metachromatic granules in the cytoplasm – characteristic
for mast cells. There is also positive antibody staining to CD117 and Mast cell tryptase antigen. Intraepidermal bullae and vesicles filled with fluid containing
eosinophils and mast cells can be seen.
Figure 4
Figure 5
Figure 6
Table 1
Table 2
Discussion
Mastocytosis is diagnosed on the basis of clinical history,
presenting sign and symptoms, histopathology and laboratory
examinations [9]. The World Health Organization (WHO) classifies
mastocytosis into 7 categories (Table 1). WHO has also developed
criteria for systemic mastocytosis (Table 2) [8].
A physical examination with a positive Darier’s sign, serum
tryptase level, blood count and a skin biopsy should be evaluated
initially. In addition to the skin biopsy, bone marrow studies are
recommended if the tryptase is significantly elevated. Severe systemic
symptoms are present, if there is associated organomegaly or if
there is no significant response to initial symptomatic therapy [4].
In children with tryptase < 100 ng/ml the diagnosis of CM may be
decided upon without bone marrow biopsy, unless other signs of SM
are present. Rising tryptase levels or those that exceed 100 ng/ml are
an indication for bone marrow biopsy regardless of age [7]. Tryptase
levels correlate with mast cells numbers in the skin. Elevations of
tryptase is seen in patients with a more severe disease [4].
The approach to treatment of patients with mastocytosis is to
stabilize the release of mast cell mediators and to block their effects
in order to control the symptoms and signs of the disease such as
pruritus, flushing and gastrointestinal cramping [4]. The treatment
includes patient counseling, avoidance of trigger factors of mast
cell degranulation (environmental stimuli, emotional stress, certain
by MC [4,8,9].
The main groups of drugs used in treatment of cutaneuos
mastocytosis are antihistamines, leukotriene antagonists, topical and
oral cromolyn sodium, local therapy with zinc preparations, steroids,
calcineur in inhibitors, NSAID’s, phototherapy and PUVA [2,8]. Only
few case reports describe the use of oral glucocorticoids in treatment
of diffuse cutaneous disease refractory to topical therapy [8].
In our case, the patient did not respond to the common
available treatment options, that is why oral corticosteroids were
added temporarily. Systemic corticosteroids relieved the symptoms.
However, inevitable development of complications prompted search
for an alternative treatment. Unfortunately, oral cromolyn sodium is
not available in our country, therefore it was ordered from abroad. The
treatment proved to be moderately effective with some exacerbations
still observed by the child’s parents.
Cromolyn sodium is a mast cell stabilizer. Its mechanism of action
is unclear. Oral cromolyn sodium has proven to be effective in some
children to control diarrhea, abdominal pain, nausea, and vomiting.
Despite its low absorption in the intestines, cromolyn sodium is said
to be useful in some patients for the treatment of cutaneous symptoms
including pruritus [4]. Currently, cromolyn sodium is one of the
mainstay treatments of mastocytosis [8]. Mastocytosis treatment can
be challenging due to the variability of the cutaneous and systemic
disease. Unfortunately, no universal treatment protocol exists [7].
References
- Vaes M, Benghiat FS, Hermine O. Targeted Treatment Options in Mastocytosis. Front Med (Lausanne). 2017;4:110.
- Edwards AM, Capkova S. Oral and topical sodium cromoglicate in the treatment of diffuse cutaneous mastocytosis in an infant. BMJ Case Reports. 2011.
- Rothe M, Grant-Kels JM, Makkar HS. Mast cell disorders: Kids are not just little people. Clinics in Dermatology. 2016;34(6):760-6.
- Castells M, Metcalfe DD, Escribano L. Guidelines for the Diagnosis and Treatment of Cutaneous Mastocytosis in Children. Am J Clin Dermatol. 2011;12(4):259-70.
- Azana JM, Torrelo A, Matito A. Update on Mastocytosis (Part 2): Categories, Prognosis, and Treatment. Actas Dermosifiliogr. 2016;107(1):15-22.
- Bologna JL, Schaffer JV, Cerroni L. Dermatology. Fourth Edition. Section 18. Neoplasms of the Skin: Tharp, Sofen, Mastocytosis. 2102-2112. 2018. Elsevier Limited.
- Lange M, Nedoszytko B, Gorska A, Anton Żawrocki, Michał Sobjanek, Dariusz Kozlowski. Mastocytosis in children and adults: clinical disease heterogeneity. Arch Med Sci. 2012;8(3):533-41.
- Cardet JC, Akin C, Lee MJ. Mastocytosis: update on pharmacotherapy and future directions. Expert Opin Pharmacother. 2013;14(15): 2033-45.
- Carter MC, Metcalde DD, Komarow HD. Mastocytosis. Immunol Allergy Clin North Am. Author; available in PMC 2015 Feb 1.