Case Report
Bilateral Otomastoiditis in a 8 Month-Old Child with Orofacial Cleft
Charles Maquet, Nicolas Bon-Mardion, Michael Eliezer, Mohamed Hijazi and Jean-Paul Marie*
Service ORL - Chirurgie cervico-faciale, CHU Charles Nicolle Rouen, France
*Corresponding author: Jean-Paul Marie, Service ORL - Chirurgie Cervico-faciale, CHU Charles Nicolle Rouen, 1 rue de Germont, Rouen, 76000, France
Published: 04 May, 2018
Cite this article as: Maquet C, Bon-Mardion N, Eliezer
M, Hijazi M, Marie J-P. Bilateral
Otomastoiditis in a 8 Month-Old Child
with Orofacial Cleft. Ann Clin Case Rep.
2018; 3: 1509.
Introduction
Acute mastoiditis is the most frequent complication of acute media otitis in the pediatric
population. The frequency has decreased with the arrival of antibiotherapy to treat acute media
otitis. The most common germs in cause are Streptococcus pneumoniae, Streptococcus pyogenes,
Pseudomonas aeruginosa, Haemophilus influenzae and Fusobacterium necrophorum [1].
Subperiosteal abscess is a known evolution of acute oto-mastoiditis; it affects more frequently
children under 4 years old (with a mean age of 34 months) and usually affects one side [2].
In most of the cases, patients had a history of acute media otitis with fever, otalgia and mild
transmission hearing loss. Retroauricular abscess is suspected when retroauricular oedema,
auricular proptosis or retroauricular erythema appears. It can even be revealed by predominant
symptoms of complication as meningitis, facial nerve palsy or focal neurologic sign.
Case Report
An 8-month girl with bilateral cleft lip and palate was sent to our department for suspicion of
mastoiditis presenting with bilateral retroauricular erythema and swelling without fever. She had
lip surgery already.
Clinical examination showed bilateral acute media otitis and no fever. Temporal bone CT scan
shows bilateral middle ear effusion without bone complication traducing otomastoiditis (Figure 1).
Axial enhanced CT scan demonstrated bilateral subperiosteal abscess appearing as hypodensities
with peripheral enhancement, larger on the left side. No intracranial complication was found
(Figure 2).
She was treated with bilateral ventilation tube of the tympanic membrane associated with
surgical drainage of the larger abscess (on the left side) and needle aspiration of the contralateral
side. Three days intravenous antibiotherapy was given with amoxicillin and clavulanic acid leading
to a decrease of the symptoms followed by eight days of oral switch therapy. Identified germs were
Staphylococcus epidermidis and Streptococcus intermedius for both sides.
Clinical evolution was fine with no recurrence after a one year follow-up.
Discussion
Orofacial clefts are congenital malformation characterized by incomplete fusion of the hard
palate or superior lip, sometime both. This condition is a well known cause of bilateral recurrent
otitis media.
Unfortunately, despite surgical reparation of the palate cleft, velar insufficiency and tubar
dysfunction remains common, often requiring prophylactic treatment with ventilation tubes and
regular examinations to early diagnose tympanic retraction and emergence of cholesteatoma.
Mastoiditis was the most frequent complication of acute otitis media before the antibiotics era.
It seems important to remind that clinical presentation of subperiosteal abscess is heterogenous, and
does not always include fever or local signs.
Middle ear and brain CT scan with enhancement is the most efficient imaging investigation
to diagnose subperiosteal abscesses with 97% sensitivity even at early stages and detect other
complications [2].
It reveals an opacification of middle ear and mastoid cells, also called otomastoiditis. It detects
brain abscess, lateral sinus thrombosis, subperiosteal abscess and mastoid bone erosion.
Bilateral subperiosteal abscess is an extremely rare presentation,
in 2012, Hathorn reviewed 6 cases of bilateral subperiosteal abscess
and concluded to the efficiency of bilateral cortical mastoidectomy
with fine outcomes (except for atypical germs) all treated with
different antibiotics [3].
To our knowledge, this is the first reported case of bilateral
subperiosteal abscess of very young child with history of orofacial
cleft.
Admitted therapeutic strategy of mastoid subperiosteal abscesses,
with no intracranial complication or suspected Fusobacterium
infection, consists on a conservative treatment associating bilateral
middle ear drainage with ventilation tubes and needle aspiration or
surgical abscess drainage [4].
Even though aggressive, mastoidectomy is the most efficient
treatment in the complicated cases mentioned above.
There are no existing series comparing these two treatment
strategies in bilateral subperiosteal abscesses.
Finally, we can ask ourselves whether bilateral subperiosteal
abscess of mastoid is a complicated entity and therefore should be
treated with primal bilateral mastoidectomy or can it be managed
with the usual combined treatment.
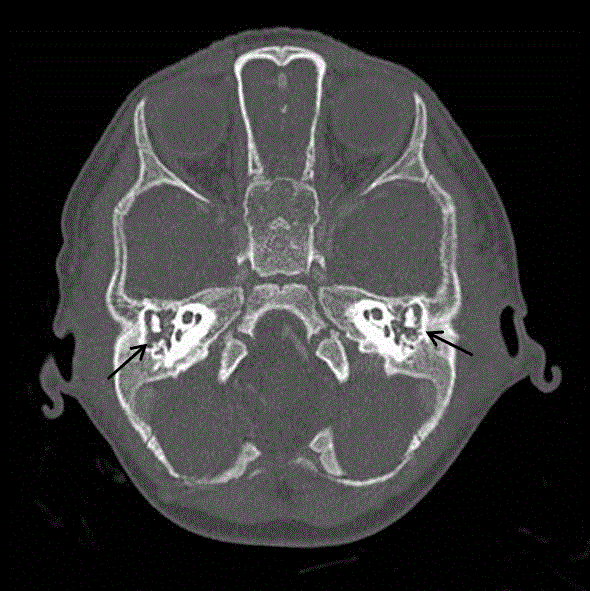
Figure 1
Figure 1
Axial temporal bone CT scan showing bilateral middle ear and
mastoid effusion (Black arrows).
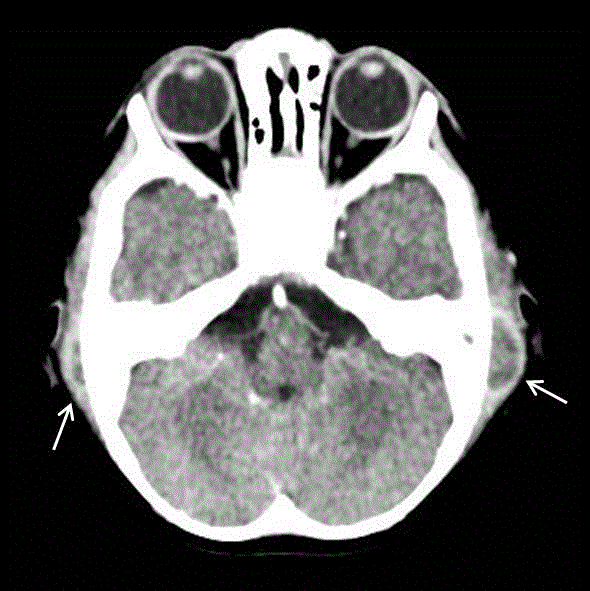
Figure 2
Figure 2
Axial temporal enhanced CT scan showing bilateral mastoid
subperiosteal abscess (White arrows).
References
- P Gorphe, A de Barros, O Choussy, D Dehesdin, JP Marie. Acute mastoiditis in children: 10 years experience in a French tertiary university referral center. Eur Arch Otorhinolaryngol. 2012; 269(2): 455-60.
- Migirov L, Yakirevitch A, Kronenberg J. Mastoid subperiosteal abscess: A review of 51 cases. Int J Pediatr Otorhinolaryngol. 2005;69(11):1529-33.
- Hathorn IF, Hussain SSM. Bilateral acute mastoiditis and subperiosteal abscesses in a child managed by simultaneous bilateral mastoid surgery. J Laryngol Otol. 2012;126(8):825-9.
- Trijolet JP, Bakhos D, Lanotte P, Pondaven S, Lescanne E. Acute mastoiditis in children: can mastoidectomy be avoided?. Ann Otolaryngol Chir Cervicofac. 2009;126(4):169-74.