Case Report
Perinatal Management of Cesarean Scar Dehiscence at 21 Weeks of Gestation
Enengl S*, Brautigam G, Binder H, Oppelt P, Altmann R and Mayer RB
1Division of Cardiology, Department of Internal Medicine, Thomas Jefferson University Hospital, Philadelphia, USA
2Department of Internal Medicine, Thomas Jefferson University Hospital, Philadelphia, USA
*Corresponding author: Sabine Enengl, Department of Gynecology and Obstetrics, Kepler University Hospital, Campus IV Krankenhausstrasse 26-30, 4020 Linz, Austria
Published: 24 Apr, 2017
Cite this article as: Enengl S, Brautigam G, Binder H,
Oppelt P, Altmann R, Mayer RB.
Perinatal Management of Cesarean
Scar Dehiscence at 21 Weeks of
Gestation. Ann Clin Case Rep. 2018;
3: 1492.
Abstract
Uterine rupture following a uterine cesarean scar dehiscence is a potentially life-threatening complication for both mother and fetus. In this report we want to describe the case of a 33-year-old gravida 2 para 1, who was diagnosed with distinct cesarean scar dehiscence at 21 weeks of gestation. Surveillance with weekly repeated sonographic examinations of the lower uterine segment and clinical monitoring allowed continuation of the pregnancy for further six weeks to reach the point of fetal viability. As recent studies have revealed no clear evidence how to handle such sonographic findings, this case report demonstrates a possible way of perinatal management.
Keywords: Cesarean section; Dehiscence; Uterine rupture; Ultrasonography; Lower uterine segment
Introduction
This case report demonstrates the difficulty of predicting the individual risk of uterine rupture if a cesarean scar dehiscence is diagnosed during pregnancy. The individual approach is influenced by the patient’s gestational week. In this case it was possible to continue the pregnancy by assessing the patient’s risk for uterine rupture on the basis of ultrasound findings.
Case Presentation
A 33-year-old woman, gravida 2 para 1, was referred to us because of lower abdominal pain at 15+4 weeks of gestation. Her previous pregnancy 2 years ago resulted in an emergent cesarean section (CS) performed in Hungary due to non-reassuring cardiotocographic findings. Ultrasound postpartum revealed no pathological findings, with the patient showing uneventful postpartum course. At 20+6 weeks, she complained of persistent discomfort on her lower abdomen, which prompted us to perform close ultrasound examination, revealing thin lower segment, the area corresponding to the previous uterine scar: it was 2.5 mm thick with 10 mm width. At 22+1 weeks of gestation the patient was hospitalized because of discomfort and progressive scar dehiscence (2.5 mm thin and 12 mm in width: (Figure 1)): analgesia (Paracetamol Kabi®/Fresenius Kabi Austria, Paracetamol, 1000 mg, intravenous) were administered under bed rest. Fetal measurements, the cervical length and fetal Doppler sonography were within normal range. At 23+5 and 23+6 weeks of gestation, the patient received corticosteroids (Solu-Celestan®/MSD, Betamethason- Disodiumphosphate, 2 mg x 12 mg, intramuscular) for fetal lung maturation, with tocolysis (Tractocile®/Ferring, Atosiban, bolus (6.75 mg), infusion (37.5 mg), intravenous. The degree of dehiscence increased: less than 2 mm thin and 24 mm in width (Figure 2). She was discharged at her own request at Christmas at 25 weeks after extensive counseling on the risks and complications. The patient was again admitted at 25+2 weeks of gestation due to preterm labor contractions. Ultrasound examinations revealed further progression of the dehiscence, measuring 27 mm in width whereas the cervical length remained normal. Tocolysis was continued. At 26+5 weeks of gestation uterine contractions developed. Ultrasound revealed a further progress of the dehiscence (47 mm width) with cervix shortening. We diagnosed this condition as tocolytic failure with imminent uterine rupture, and an emergent CS was performed. Intraoperative findings showed a dehiscence covered by peritoneum (incomplete uterine rupture). The bladder was pulled up so uterotomy (transverse incision) was performed higher, just above the edge of the bladder without any severe hemorrhage. The neonate was delivered without any difficulty and transferred to the neonatal intensive care unit. The postoperative development was uneventful; the patient was discharged five days after surgery. It would have been technically difficult and hazardous to correct the entire uterine defect during emergent CS. Hence, an interval assessment and excision of myometrial defect with reconstruction by laparoscopy or laparotomy has been planned before the patient attempts further pregnancy. Unfortunately the patient did not keep her follow-up appointments; she stated that further appointments in Hungary have been scheduled.
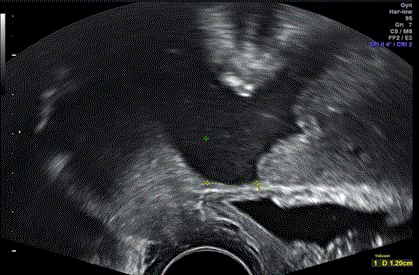
Figure 1
Figure 1
Transvaginal sonography revealed the existence of a uterine scar
dehiscence measuring 12mm in width at 22+1 weeks of gestation.
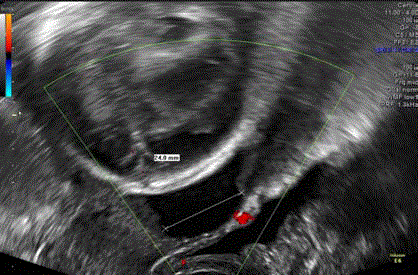
Figure 2
Figure 2
Transvaginal sonography of the progressive dehiscence measuring
24mm in width at 23+6 weeks of gestation.
Discussion
Cesarean scar dehiscence may be found incidentally during
repeat cesarean section. If scar dehiscence is diagnosed during
pregnancy, no reliable method to predict the individual risk of
uterine rupture has been found up to now. In fact, there are several predictive models for uterine rupture using risk factors, but they
have not proven clinically relevant [1]. One recent study showed that
the incision location in the uterus, maternal age, a higher newborn
birth weight and uterine retroflexion might play a role [2]. There are
also attempts to evaluate the risk through sonographic examinations
of the myometrial thickness or the width and length of a defect.
However, the results seem to be only subjective impressions and a
more objective assessment is needed to become reproducible [3].
Some authors consider a thickness of the lower uterine segment of
<2.5 mm predictive of an increased risk of full rupture [4].
The individual approach is influenced by the patient’s stage of
gestation and clinical condition. In case of a suspected dehiscence
near term, a subsequent cesarean delivery before the onset of labor
seems to be the best option to avoid progression to rupture. There are
only a few case reports, so there is no clear recommendation as how
to manage cases with such sonographic findings [5]. If cesarean scar
dehiscence is diagnosed in early pregnancy, there is no clear evidence
for a standardized management, so an individualized approach has
to be chosen. This case report demonstrates how a pregnancy could
be continued by assessing the risk of the patient for uterine rupture
based on sonographic findings.
References
- Landon MB. Predicting uterine rupture in women undergoing trial of labor after prior cesarean delivery. Semin Perinatol. 2010; 34:267-71.
- Pomorski M, Fuchs T, Rosner-Tenerowicz A, Zimmer M. Morphology of the cesarean section scar in the non-pregnant uterus after one elective cesarean section. Ginekol Pol. 2017; 88:174-9.
- Naji O, Abdallah Y, Bij De Vaate AJ, Smith A, Pexsters A, Stalder C, et al. Standardized approach for imaging and measuring Cesarean section scars using ultrasonography. Ultrasound Obstet Gynecol. 2012; 39:252-9.
- Bujold E, Jastrow N, Simoneau J, Brunet S, Gauthier RJ. Prediction of complete uterine rupture by sonographic evaluation of the lower uterine segment. Am J Obstet Gynecol. 2009; 201:320.e1-6.
- Fox NS, Gerber RS, Mourad M, Saltzman DH, Klauser CK, Gupta S, et al. Pregnancy outcomes in patients with prior uterine rupture or dehiscence. Obstet Gynecol. 2014; 123:785-9.