Case Report
Bilateral Anconeus Epitrochliaris Causing Cubital Tunnel Syndrome: A Case Report
Lebur Rohman1*, Yusuf Michla1, Stefan Holden2 and Rebecca Walsh2
1Department of Orthopedics, Sunderland Royal Hospital, United Kingdom
2Medical Student, Newcastle University, United Kingdom
*Corresponding author: Lebur Rohman, ST5 Orthopaedic Registrar, Sunderland Royal Hospital, United Kingdom
Published: 24 Nov, 2017
Cite this article as: Rohman L, Michla Y, Holden S, Walsh
R. Bilateral Anconeus Epitrochliaris
Causing Cubital Tunnel Syndrome: A
Case Report. Ann Clin Case Rep. 2017;
2: 1475.
Abstract
A case report describing the very rare finding of bilateral Anconeus Epitrochliaris. The patient presented with bilateral ulnar nerve symptoms and intraoperative findings identified bilateral Anconeus Epitrochliaris as the cause to the ulnar nerve compression. Ulnar nerve compression can occur at various sites within the cubital tunnel, with the most common sites being the 2 heads of the Flexor Carpi Ulnaris muscle, arcade of struthers and between Osborne’s Ligament and the MCL. Entrapment by the Anconeus Epitrochliaris muscle is a rare finding and is present in approximately 3%-34% of individuals. Furthermore, those found to have this muscle have a 25% chance of having bilateral muscles thus ulnar nerve entrapment is likely in the opposite arm. Careful history and examination is key in diagnosing and treating ulnar nerve entrapment regardless of the cause.
Keywords: Anconeus epitrochliaris; Ulnar nerve; Cubital tunnel syndrome
Introduction
The finding of the muscle Anconeus Epitrochliaris is rare, but when present can cause Cubital Tunnel Syndrome. However, finding bilateral Anconeus Epitrochliaris is even rarer. The literature
on this rare cause of Cubital Tunnel Syndrome is sparse. To our knowledge this is the second report
of bilateral Anconeus Epitrochliaris.
This article will present the case report of the patient along with a concise discussion on ulnar
nerve anatomy, distribution and cubital tunnel syndrome.
Case Presentation
A 49-year-old female, right hand dominant and a business woman presented to an upper limb
clinic, complaining of bilateral hand problems. She gave a one year history of persistent bilateral
little and ring finger numbness, present initially at night time and prolonged elbow flexion positions.
Over the last few month prior to presentation her symptoms were reproduced on minimal elbow
flexion positions and increasing pain in the elbow, thus troubled by her symptoms throughout the
day and every day. She denied any weakness in her hands and no neck pain or trauma.
The patient had no past medical history of note and was not taking any regular medications.
On examination, inspection of the elbow joints and entire upper limbs were unremarkable. There
was reduced sensation to both sides of the little fingers and only the ulnar half of the ring fingers
bilaterally. There was no muscle wasting in the hands and power of (MRC grading) 5/5 in the 1st
dorsal interrossi and Abductor Digiti Minimi muscle bilaterally. There was a positive elbow flexion
test bilaterally, reproducing symptoms within 30 seconds. Furthermore, Tinel’s test over the Cubital
tunnel was strongly positive. A full examination of the radial and median nerve was completely
normal as was neck examination. A clinical diagnosis of bilateral Cubital Tunnel Syndrome was
made, and since the examination and history were strongly positive, nerve conduction studies were
not deemed necessary and plain radiographs were unremarkable.
The patient underwent Cubital Tunnel Decompression on the left side under a general
anaesthetic, with full resolution of symptoms. Subsequent decompression on the right side was done
6 month later, again with full resolution of symptoms. The cause of this patient’s symptoms was
identified intra-operatively, with identification of the Anconeus Epitrochliaris muscle bilaterally,
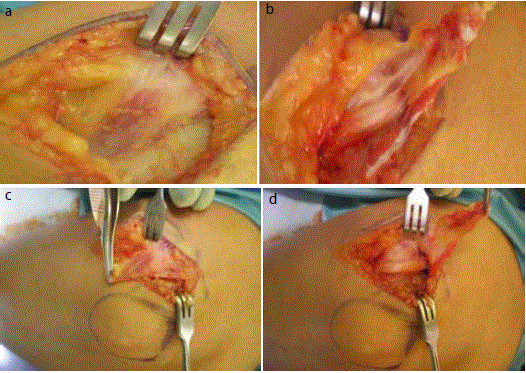
which was clearly causing compression of the nerve macroscopically (Figure 1 a-d) A) right elbow with initial dissection demonstrating a structure resembling muscle. B) Anconeus Epitrochliaris
elevated to expose the right ulnar nerve beneath. C) Left elbow demonstrating a muscle overlying the cubital tunnel. D) Anconeus Epitrochliaris elevated to expose left
ulnar nerve beneath).
Figure 1
Figure 1
A) Right elbow with initial dissection demonstrating a structure
resembling muscle. B) Anconeus Epitrochliaris elevated to expose the right
ulnar nerve beneath. C) Left elbow demonstrating a muscle overlying the
cubital tunnel. D) Anconeus Epitrochliaris elevated to expose left ulnar nerve
beneath).
Figure 2
Figure 3
Discussion
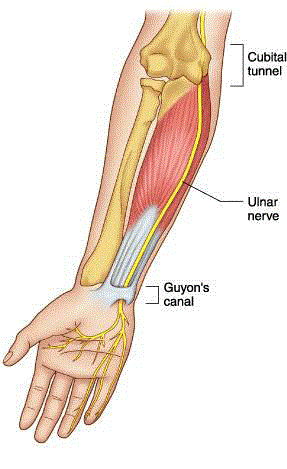
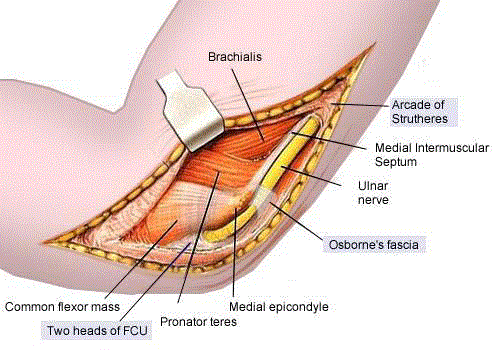
Cubital tunnel syndrome occurs when the ulnar nerve, which is
formed by nerve roots C8 to T1, becomes crushed or irritated within
the cubital tunnel [1-2] and along other points during the course of
the nerve to the terminal digital branches (Figure 2 and 3). In the
most common anatomic pattern, the ulnar nerve passes through the
medial intermuscular septum (MIS) at approximately the midpoint
of the arm, as it approaches the elbow, before entering the posterior
aspect of the arm. Travelling behind MIS, on the medial aspect of the
triceps, the ulnar nerve then enters the post condylar groove lateral to
the medial epicondyle. At the elbow, the ulnar nerve passes through
the cubital tunnel, between the medial epicondyle and the olecranon.
The roof of the cubital tunnel is formed by a thickening aponeurosis,
which becomes the cubital tunnel retinaculum, called Osborne’s
band (or ligament of Osborne) [3]. Extending from the medial
epicondyle to the tip of the olecranon, and approximately 4mm-2cm wide from proximal to distal end, Osborne’s band connects the
tendinous insertions on the humeral and ulnar heads of the Flexor
Carpi Ulnaris muscle (FCU). The distal margin merges with the fascia
covering the humeral and ulnar heads of the FCU. The fibres of the
cubital tunnel retinaculum are arranged transversely, and are pulled
taught during flexion of the elbow. It is functionally discrete from
the FCU aponeurosis [4,5] Osborne’s band is also reported as the
thickened border of the flexor carpi ulnaris aponeurosis [6]. An extra
structure, the Epitrochleoanconeus ligament, has also been reported,
covering the ulnar nerve at this level [7]. The floor of the cubital
tunnel is formed of the medial collateral elbow ligaments and the
joint capsule, with the medial epicondyle and the olecranon forming
the walls. The ulnar nerve branches to the elbow whilst within the
tunnel. After exiting, the ulnar nerve travels into the forearm between
the humeral and ulnar heads of the FCU and then branches to the
FCU. When ulnar nerve entrapment occurs, the most common sites
are at the Arcade of Struthers, the flexor carpi ulnaris aponeurosis,
the medial intramuscular septum and finally the deep flexor pronator
aponeurosis [5].
However, there frequently exist other anatomic patterns, already
described by Cutts et al. [8]. The third most common of these relates
to the presence of the anconeus epitrochlearis muscle. Anconeus
epitrochlearis is an extra muscle that has a prevalence of between 3%
and 34%, according to cadaveric studies [8-12]. Located proximally to
the origin of the two heads of the flexor carpi ulnaris, it arises from the
medial border of the olecranon, and inserts into the medial epicondyle.
It follows the same route as the retinaculum and in the absence of
Osborne’s band lies across the roof of the cubital tunnel. Cubital
tunnel syndrome is a well-recognised ulnar neuropathy resulting
from compression of the ulnar nerve at the elbow [13]. It is the second
most common entrapment neuropathy in the arm, with an incidence
rate of 24.7 per 100,000 [14,15]. More often than not, the cause is
unknown, so it is usually idiopathic. There are however, several space
occupying lesions, as well as the anomalous anconeus epitrochlearis
muscle that have been reported to cause ulnar nerve compression
at the cubital tunnel [16,17,18]. Ulnar neuropathy secondary to the
anconeus epitrochlearis muscle presents differently to idiopathic
cubital tunnel syndrome, for example presenting at a younger age
and progressing more rapidly. The associated symptoms have also
been seen to have a shorter duration [19]. Increased elbow pain that is
more notable than the sensory symptoms is also found [16,18,20]. We
also found this to be the case. It is thought that 25% of the people with
this muscle and who are symptomatic will have bilateral anconeus
epitrochliaris [17]. Despite the presence of this anomalous muscle being reported to be present in 3% to 34% of cadaveric specimens
[8-12] the clinical diagnosis of secondary ulnar neuropathy is rare.
Reports of the anconeus epitrochlearis causing compression [17,19-
23] do not actual manage to show how common the condition is, and
the prevalence of ulnar nerve compression secondary to anconeus
epitrochlearis is unknown [17]. As such it is more often than not an
operative finding, not a preoperative diagnosis [16,17,23]. It is worth
noting, also, that occasionally the anconeus epitrochlearis muscle is
incomplete, with its structure being both muscular and fibrous. As
such, it is suggested that the Epitrochleoanconeus ligament described
may in fact be an anconeus epitrochlearis muscle, with a highly fibrous
structure [24]. The fact that the prevalence of ulnar neuropathy
caused by the anconeus epitrochliaris muscle is uncertain [17,19,23]
makes it difficult to evaluate how frequently any bilateral neuropathy
may occur bilaterally. At the time of writing, the authors had only
found one other case report of a similar bilateral ulnar neuropathy
caused by the anconeus epitrochlearis muscle [26]. We found that
surgical excision of the muscle provided symptomatic relief and a
positive outcome for the patient, and this is consistent with other’s
findings [25,26].
Due to the strength of the diagnosis based on the patient’s history
and examination, nerve conduction studies were not performed in
order to confirm the diagnosis. In other cases, nerve conduction
studies can be used to examine the location of the nerve entrapment,
as well as the severity and precise location [27]. Kern also showed that
nerve conduction studies will most reliably demonstrate slowed ulnar
nerve conduction at the elbow, with conduction speeds less than
45.0 metres/second suggested as appropriately slowed conduction
[23]. It is worth noting, however, that electrodiagnosis of ulnar nerve
entrapment can give false readings and as in our case are not always
necessary in the presence of a compelling history and examination.
It is also worth considering, that it can sometimes be the case that
nerve conduction studies can sometimes be subject to the skill of
the healthcare professional performing the test, and it is suggested
that rather than relying only on the results of the test, the patient’s
experiences and symptoms should also be considered [28-29].
Further, we suggest, owing to the prevalence of the Anconeus
Epitrochliaris muscle in cadaveric specimens [8-12] there may
be benefits to informing any patient who presents with unilateral
neuropathy found as a result of Anconeus Epitrochlearis of the
potential presentation of the same symptoms in the other arm at
a later date. This may in turn help with the prevention of further
complications and reduce the need for future surgery for symptomatic
relief.
Conclusion
In summary, the causes of Cubital Tunnel Syndrome can be wide ranging but most commonly occur due to a few common causes. Despite the cause of the syndrome prompt clinical history and examination is paramount in the diagnosis and surgical treatment is usually necessary. Having an awareness of more unusual causes can aid the clinician to be vigilant in the management of the patient and also aid surgical dissection and exploration. When the anomalous muscle Anconeus Epitrochliaris is present one should suspect the possibility of bilateral presence and counsel/investigate the patient appropriately.
References
- William Feindel, Joseph Stratford. Cubital tunnel compression in tardy ulnar nerve palsy. Can Med Assoc. 1958. 78(5): 351-353.
- LLC ST. Cubital Tunnel Syndrome. 2017.
- GV O. Surgical treatment of tardy ulnar neuritis. J Bone Joint Surg. 1957; 39:782.
- O'Driscoll SW, Horii E, Carmichael SW, Morrey BF. The cubital tunnel and ulnar neuropathy. J Bone Joint Surg Br. 1991; 73(4):613-617.
- James R Doyle, Michael J Botte, Philadelphia PA, Lippincott Williams, Wilkins. Surgical Anatomy of the Hand & Upper Extremity. J Hand Ther. 2004; 17(1): 72-73.
- Rengachary SS. Entrapment neuropathies. In: Wilkins RH, Rengachary SS, editors. Neurosurgery. New York: McGraw-Hill; 1987. p.1-28.
- Brunelli G. Ulnar nerve compression at the elbow. In: Brunelli GA editor. Nerve Lesions of the Upper Limb. Pavia: EDIMES; 2004. p.91-94.
- Cutts S. Cubital tunnel syndrome. Postgrad Med J. 2007; 83(975):28-31.
- Dellon AL. Musculotendinous variations about the medial humeral epicondyle. J Hand Surg Am. 1986 ; 11(2):175-181.
- Masear VR, Hill JJ Jr, Cohen SM. Ulnar compression neuropathy secondary to the anconeus epitrochlearis muscle. J Hand Surg. 1988; 13(5):720-724.
- O'Hara JJ, Stone JH. Ulnar nerve compression caused by a prominent medial head of the triceps and an anconeus epitrochlearis muscle. J Hand Surg. 1996; 21(1): 133-135.
- Husarik DB, Saupe N, Pfirrmann CW, Jost B, Hodler J, Zanetti M. Ligaments and plicae of the elbow: normal MR imaging variability in 60 asymptomatic subjects. Radiology. 2010; 257(1):185-194.
- Vanderpool DW, Chalmers J, Lamb DW, Whiston TB. Peripheral compression lesions of the ulnar nerve. J Bone Joint Surg Br. 1968; 50:792-803.
- Sookur PA, Naraghi AM, Bleakney RR, Jalan R, Chan O, White LM. Accessory Muscles: Anatomy, Symptoms, and Radiologic Evaluation. Radiographics. 2008; 28(2):481-499.
- Folberg CR, Weiss AP, Akelman E. Cubital tunnel syndrome. Part I: Presentation and diagnosis. Orthop Rev. 1994; 23(2):136-144.
- Assmus H, Antoniadis G, Bischoff C. Carpal and cubital tunnel and other, Rarer nerve compression syndromes. Dtsch Arztebl Int. 2015; 112(1-2):14-26.
- Li X, Dines JS, Gorman M, Limpisvasti O, Gambardella R, Yocum L. Anconeus epitrochlearis as a source of medial elbow pain in baseball pitchers. Orthopedics. 2012; 35:e1129-e1132.
- Jeon IH, Fairbairn KJ, Neumann L, Wallace WA. MR imaging of edematous anconeus epitrochlearis: another cause of medial elbow pain? Skeletal Radiol. 2005; 34(2): 103-107.
- Masear VR, Hill JJ Jr, Cohen SM. Ulnar compression neuropathy secondary to the anconeus epitrochlearis muscle. J Hand Surg Am. 1988; 13(5): 720-724.
- Nellans K, Galdi B, Kim HM, Levine WN. Ulnar neuropathy as a result of anconeus epitrochlearis. Orthopedics. 2014; 37(8):e743-e745.
- MD Guidelines. Neuropathy of Ulnar Nerve (Entrapment). 2017.
- Byun SD, Kim CH, Jeon IH. Ulnar neuropathy caused by an anconeus epitrochlearis: clinical and electrophysiological findings. J Hand Surg Am. 2011; 36(7): 607-608.
- Erdem Bagatur A, Yalcin MB, Ozer UE. Anconeus Epitrochlearis Muscle Causing Ulnar Neuropathy at the Elbow: Clinical and Neurophysiological Differential Diagnosis. Orthopedics. 2016; 39(5):e988-e991.
- Cheriyan T, Neuhaus V, Mudgal CS. Velocity drop in anconeus epitrochlearis-associated cubital tunnel syndrome. Am J Orthop (Belle Mead NJ). 2014; 43: 227-229.
- Dekelver I, Van Glabbeek F, Dijs H, Stassijns G. Bilateral ulnar nerve entrapment by the M. anconeus epitrochlearis. A case report and literature review. Clin Rheumatol. 2012; 31(7):1139-1142.
- Gervasio O, Zaccone C. Surgical approach to ulnar nerve compression at the elbow caused by the epitrochleoanconeus muscle and a prominent medial head of the triceps. Neurosurgery. 2008; 62:186-92.
- Kern, RZ. The electrodiagnosis of ulnar nerve entrapment at the elbow. Can J Neurol Sci. 2003: 30(4): 314-319.
- Salerno DF, Werner A, Albers JW, Becker MP, Armstrong J, Franzblau A. Reliability of nerve conduction studies in active workers. Muscle Nerve. 1999; 22(10):1372-1379.
- Deborah Allen. Cubital Tunnel Syndrome. OrthoBullets. 2017.