Case Report
High Degree Atrioventricular Block and Syncope in the Tetralogy of Fallot (TOF)
Delarue A1,2,3*, Houeijeh A2,3 and Godart F2,3
11Department of Medicine, Laboratoire d'anatomie, France
2Department of Medicine, Hospital Cardiologique, France
3Department of Medicine, University Lille, France
*Corresponding author: Delarue A, Department of Medicine, Laboratoire d'anatomie, 1 place de Verdun, 59045, Lille cedex, France
Published: 24 Oct, 2017
Cite this article as: Delarue A, Houeijeh A, Godart F. High
Degree Atrioventricular Block and
Syncope in the Tetralogy of Fallot
(TOF). Ann Clin Case Rep. 2017; 2:
1455.
Abstract
Introduction: TOF is the most frequent congenital cyanogen cardiopathy. Sudden death is the most
frequent adverse event after surgical treatment, mostly due to Serious Ventricular Rhythm Trouble.
High degree atrioventricular block is rare cause of syncope or sudden death especially late after
complete correction.
Case Presentation: We describe here the case of a 49 years old patient suffering of a regular TOF
operated at the age of six followed by a total atrioventricular block during post-operative period,
which quickly and spontaneously self-resoluted, an which presented recently severe syncope. There
is no argument for extra cardiac explanation. EKG found total right bundle-branch block, left axis
and an anterior left bundle-branch half-block. The echocardiography found a TOF corrected with
good results (normal volume of the right cavities and a minor pulmonary leakage). The programmed
ventricular stimulation was negative and electrophysiological study founding a long HV delay
leading to an implantation of pacemaker.
Discussion: The HDAB diagnosis in these situations is not that easy from an epidemiological
point of view and pathophysiology, but it may help avoid the excessive implantation of automatic
implantable defibrillator. A good correction result, trans-annular patch absence and the EKG aspect
should evoke this diagnostic.
Keywords: Syncope; Fallot; Total atrioventricular block; Late; Pacemaker
Introduction
TOF is the most frequent congenital cyanogen cardiopathy. Sudden death is one of most frequent adverse event after surgical treatment, mostly due to Serious Ventricular Rhythm Trouble (SVRT) [1,2]. Nonetheless, High Degree atrioventricular blocks (HDAB) are a rare cause of sudden death within those patients, especially when the times from total surgical treatment increase [3]. SVRT are caused by a dilatation of the right cavities and by myocardic’s scars (trans-annular patch, ventriculotomy) [4]. HDAB are cause by lesions of the conduction tissue. We describe here the case of a patient suffering of a TOF which presented severe syncope due to a HDAB, confirmed by electrophysiological study.
Case Presentation
A 49 years old patient consults at the emergency department following multiple faintness with
syncope during both rest and effort time. The most interesting point of his medical past history
is a regular TOF operated at the age of six followed by a total atrioventricular block during postoperative
time which quickly and spontaneously self-resoluted. There was no case of sudden death
in the relative. The patient wasn’t taking any medication. The clinical examination was normal, no
argument for neurological explanations of that syncope was found. The interrogation of the patient
found several arguments for a cardiogenic explanation.
Paraclinic
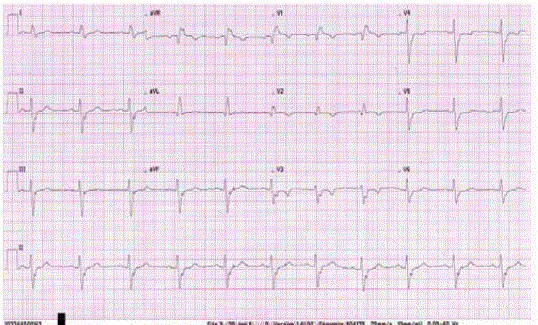
EKG found a sinusal rhythm, normal PR, total right bundle-branch block (160ms), left axis
and an anterior left bundle-branch half-block (Figure 1). An echocardiography was performed
and found a TOF corrected with good results, normal volume of the right cavities and a minor
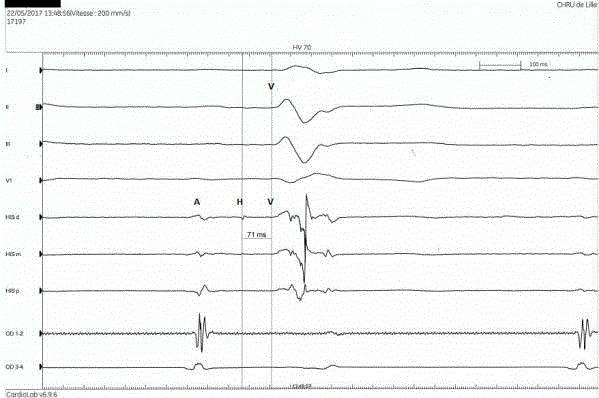
pulmonary leakage. The patient benefited from a multisite programmed ventricular stimulation (PVS), negative and from an electrophysiological study founding a long HV delay of 71 ms (Figure 2). Leading to an implantation of a dual chamber pacemaker (43 years after repair). No recurrence of the
syncope occurred.
Figure 1
Figure 1
EKG with normal PR, right bundle-branch block, left axis, anterior
left bundle-branchhalf- block.
Figure 2
Figure 2
Electrophysiological study founding a long HV delay of 71 ms. A =
atrial wave, H : His wave, V : ventricular wave.
Discussion
By frequency argument, syncope in long-term operated TOF is
caused by SVRT [5], requiring an implantable automatic defibrillator (AID) or radiofrequency ablation. In selected patients, SVRT occur
through a re-entry mechanism around scars [6,7] induced by surgery
and / or dilatation of right cavities.
Making the HDAB hypothesis in these situations is not that
easy from an epidemiological point of view and pathophysiology,
but it may help avoid the excessive implantation of AID. The lack of
expansion of right cavities, trans-annular patch absence and the EKG
aspect should evoke this mechanism on a classic right branch block
associated with a left heart axis while it is generally a right axis in the
TOF, or if it is associated with a first degree atrioventricular block.
References
- Garson A. Ventricular arrhythmias after repair of congenital heart disease: Who needs treatment?. Cardiology in the Young. 1991: 177-181.
- Khairy P, Ionescu-Ittu R, Mackie AS, Abrahamowicz M, Pilote L, Marelli AJ. Changing mortality in congenital heart disease. J Am Coll Cardiol. 2010; 56: 1149-1157.
- Wu MH, Lu CW, Chen HC, Chiu SN, Kao FY, Huang SK. Arrhythmic Burdens in Patients with Tetralogy of Fallot: A National Database Study. Heart Rhythm. 2015: 12; 604-609.
- Gatzoulis MA, Balaji S, Webber SA, Siu SC, Hokanson JS, Poile C, et al. Risk factors for arrhythmia and sudden cardiac death late after repair of tetralogy of Fallot: a multicentre study. Lancet. 2000; 356: 975-981.
- Nollert G, Fischlein T, Bouterwek S, Böhmer C, Dewald O, Kreuzer E, et al. Long-term results of total repair of tetralogy of Fallot in adulthood: 35 years follow-up in 104 patients corrected at the age of 18 or older. Thorac Cardiovasc Surg. 1997; 45: 178-181.
- Maury P, Sacher F, Rollin A, Mondoly P, Duparc A, Zeppenfeld K, et al. Ventricular arrhythmias and sudden death in tetralogy of Fallot. Arch Cardiovasc Dis. 2017; 110: 354-362.
- Kapel GF, Sacher F, Dekkers OM, Watanabe M, Blom NA, Thambo JB, et al. Arrhythmogenic Anatomical Isthmuses Identified by Electroanatomical Mapping Are the Substrate for Ventricular Tachycardia in Repaired Tetralogy of Fallot. Eur Heart J. 2017; 38: 268-276.