Case Report
An Aggressive Malignant form of Fibrous Solitary Tumor of the Pleura: A Case Report and Literature Review
Sani Rabiou1*, Hicham Harmouchi1, Kassim Sidibé2, Marouane Lakranbi1, Yassine Ouadnouni1,3 and Mohamed Smahi1,3
1Department of Thoracic Surgery, CHU Hassan II, Morocco
2Department of Imagery, CHU Hassan II, Morocco
3Departmet of Medicine and Pharmacy, Sidi-Mohamed-Ben-Abdellah University, Morocco
*Corresponding author: Sani Rabiou, Department of Thoracic Surgery, Service de chirurgie thoracique C1, CHU Hassan II, Fès, Morocco
Published: 12 Oct, 2017
Cite this article as: Rabiou S, Harmouchi H, Sidibé K,
Lakranbi M, Ouadnouni Y, Smahi M. An
Aggressive Malignant form of Fibrous
Solitary Tumor of the Pleura: A Case
Report and Literature Review. Ann Clin
Case Rep. 2017; 2: 1443.
Abstract
Background: The solitary malignant fibrous tumor of the pleura is rare histological entity with aggressive potential.
Case Presentation: The authors report the case of a 55 years old male who presented with left chest
pain. The diagnosis of a solitary malignant fibrous tumor of the pleura was evoked on the basis of
CT scan chest and confirmed by histopathological analysis of a tissue biopsy obtained by anterior
mediastinotomy.
Conclusions: If surgery is effective for benign forms, chemotherapy alone or coupled with
radiotherapy remains the only therapeutic option for the malignant forms of these tumors.
Keywords: Tumor of the pleura; Fibrous solitary tumor; Malignant tumor; Chemotherapy
Introduction
The solitary fibrous tumor of the pleura is a rare fibroblastic entity, most often localized and benign, accounting for less than 5% of all pleural tumors. Less than 10% of these tumors are labelled malignant with life-threatening metastasis [1]. Clinical manifestations may be respiratory or extra-thoracic with arthralgia, clubbing of the fingers and hypoglycaemic seizures. We report the observation of a patient with chest pain with dyspnea in whom the diagnosis of solitary malignant fibrous tumor of the pleura was evoked on the CT scan and then confirmed by the pathological examination of a tissue biopsy obtained by mediastinotomy.
Case Presentation
A 55-year-old male with a history of smoking, operated 3 times (in 2005, 2007 and 2009) for recurrent Dermato fibrosarcoma protuberans (Darier-Ferrand sarcoma, DFSP) of the right anterior thoracic wall. He had since 4 months pain in the left chest wall radiating to the left upper limb, dyspnea on exertion and weight loss of 6 kg in 4 months. The symptomatology was aggravated one week before presentation by the accentuation of the dyspnea. On admission, he had a general condition preserved with a blood pressure 150/80 mmHg and tachypnoea at 34 cycles/min associated with edema of the lower limbs. The chest examination was in favour of a consolidating lesion affecting the middle part of the left hemithorax. The chest X-ray showed opacity of the left hemithorax with mediastinal deviation to the right side (Figure 1). On CT chest with contrast, a mass, massively necrotic, occupied the left hemithorax, having close contact with the pericardium and the main pulmonary artery which was encircled by more than 180°. This mass engages the left stem bronchus and the left lower lobar bronchus and was laminated (Figure 2). It was associated with an invasion of the diaphragm with the presence of Para tracheal mediastinal adenopathy. There were no extra-thoracic lesions. The histopathological study of a large biopsy core obtained by anterior mediastinotomy under general anaesthesia was in favour of a solitary malignant fibrous tumor of the pleura (Figures 3 and 4). In fact, the patient was operated before for Darrier-Ferandsarcoma of the right chest wall. Actually we initially thought of a metastasis but after discussion with pathologists and oncologists we concluded a solitary malignant fibrous tumor of the pleura. After a discussion at the multidisciplinary consultation meeting, the decision of a radio-chemotherapy was made. The patient is currently followed in oncology department in 2nd chemotherapy cure.
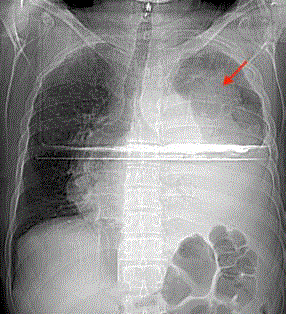
Figure 1
Figure 1
Chest X-ray showing opacity of left thoracic hemi champ with
mediastinal deviation to right side.
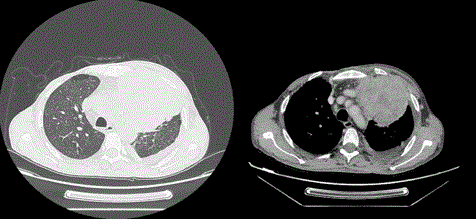
Figure 2
Figure 2
Thoracic tomodensitometry with injection of contrast medium,
which targets a tissue mass, massively necrotic, having contact with the left
ventricle and the pulmonary artery it encompasses.
Figure 3
Figure 3
Malignant solitary fibrous tumor of fusocellular architecture, cells
display cytonuclearatypieslabeled with mitosis figs (x20).
Figure 4
Figure 4
Malignant solitary fibroid tumor. A: Diffuse and intense cytoplasmic
labeling by CD34 (x 20). B: Nuclear labeling of mitotic cells by Ki67 (x 20).
Discussion
The solitary fibrous tumors of the pleura represent a rare
histological entity belonging to the pleural tumor groups of submesothelial
origin with variable clinical expression. This condition
can occur at any age, but predominates in patients over 50 years
with a balanced sex ratio in the majority of reported cases [2].
Clinically, these tumors may manifest as chest pain, associated or not
with dyspnea or cough. In some cases, haemoptysis or obstructive
pneumonia may be in the clinical presentation [3,4]. The intensity
of these symptoms is often correlated with the aggressiveness and
size of the tumor by the compression effect it exerts not only on the
respiratory system but also on the cardiac chambers responsible for
dyspnea at rest as the case of our patient. Some solitary fibrous tumors
may be associated with certain paraneoplastic syndromes such as
clubbing of the fingers, a hypertrophic pneumonic osteoarthropathy
of Pierre Marie, but especially hypoglycaemia in about 5% of cases,
which is secondary to the secretion by the tumor of an insulin- Like
substances [2,5,6].
Chest x-ray is a diagnostic step, usually showing a rounded,
homogeneous and well-defined opacity. The diagnosis of malignancy
can be evoked before a speculated opacity associated mainly with
pleural effusion [4].
The thoracic computed tomography will complement the
assessment by confirming the pleural origin and tissue nature of the
tumor, as well as its localization and its relationship with the pleura
and adjacent organs [7]. The tumor often appears very limited and
homogeneous, but a heterogeneous aspect can be observed. As is
the case in our patient, the malignant nature of a solitary fibrous tumor of the pleura is strongly evoked, whenever there are necrotichaemorrhagic rearrangements on the CT scan [8]. The thoracic
computed tomography allows us to study the loco-regional extension
of the tumor, an essential element of the therapeutic decision.
Some authors have noted the value of magnetic resonance imaging
(MRI), which makes it possible to determine the fibrous nature of
the tumor, especially in the T1 sequence, which distinguishes it from
other mediastinopulmonary, parietal and diaphragmatic structures
[8,9]. At this stage, the histological diagnosis by biopsy of the tumor
mass, with histological analysis should be proposed [10,11].
For our patient, we obtained biopsy by anterior mediastinotomy.
This technique allowed us, under general anaesthesia, to have large
biopsy fragments necessary for a consistent histological analysis
thus avoiding the misdiagnosis. From the histopathological point of
view, malignant and benign solitary fibrous tumors are defined. The
malignant forms, more rare, are defined by numerous mitoses, areas
of necrosis, and a nuclear pleomorphism [10]. Immunohistochemical
analysis, using antibodies (Ac Bcl2, CD99, CD34, vimentin, keratin
...), makes it possible to affirm the positive diagnosis and to eliminate
differential diagnoses such as sarcomas, Mesotheliomas [10].
The reference treatment is a complete surgical resection of
the tumor at its implantation base, which can sometimes extend
to the pulmonary parenchyma or to the chest wall in the event of
invasion [2,12]. In the aggressive forms of solitary fibrous tumors
of the pleura, surgical resection may be followed by chemotherapy
associated or not with radiotherapy, the real interest of which
remains to be demonstrated. In the specific case of our observation,
in view of the invasiveness of the tumor radiologically and the
results of the pathological examination including histology and immunohistochemistry, the decision of a radio-chemotherapy
was retained. Indeed, ifosfamide and adriamycin chemotherapy is
of interest in malignant inoperable forms at the outset, or for the
significant reduction in the size of an operable tumor [13]. This
chemotherapy could be justified in neo-adjuvant, in large tumors or
in postoperative, in case of incomplete resection [13]. Radiotherapy
may also be indicated after surgical resection, in case of histological
signs of malignancy, especially if this resection has been incomplete.
Because of an evolutionary profile that is difficult to evaluate, remote
radio clinic surveillance is recommended by some authors in search
of metastasis [14,15].
Conclusion
The diagnosis of solitary fibrous tumors of the pleura is histological, facilitated by the complement of immunohistochemistry. The management is surgical excision without delay. However, for aggressive and/or metastatic malignancies, chemotherapy alone or in combination with radiotherapy remains the only therapeutic option that can improve prognosis in terms of survival.
References
- Benjelloun H, Yassine N, Bourkadi N Z, Bakhatar A, Alaoui Yazidi A, Bahlaoui A. Tumeurfibreuse solitaire de la plèvre à potentielagressif : à propos d’un cas. Rev Mal Respir 2007; 24: 83.
- Cardillo G, Facciolo F, Cavazzana A, Capece G, Gasparri R, Martelli M. Localized (solitary) fibrous tumors of the pleura: an analysis of 55 patients. Ann ThoracSurg 2000; 70: 1808-1812.
- Robinson LA, Reilly RB. Localized pleural mesothelioma. The clinical spectrum. Chest. 1994; 106: 1611-1615.
- de Perrot M, Fischer S, Bründler MA, Sekine Y, Keshavjee S. Solitary fibrous tumors of the pleura. Ann Thorac Surg. 2002; 74: 285-293.
- Léna H, Desrues B, Caullet-Maugendre S, Le Coz A, Huet H, Delaval P. Le fibrome pleural : apport de l’immunohistochimie. Rev Mal Respir. 1995; 12: 383-385.
- Hamidou M, Bani-Sadr F, Kenzi A, Sagan C, Grolleau JY. [Hypoglycemia associated with pleural fibromas. Study of insulin-like growth factors (IGF) and pathogenic considerations]. Rev Med Interne. 2002; 23: 447-453.
- Ali SZ, Hoon V, Hoda S, Heelan R, Zakowski MF. Solitary fibrous tumor: a cytologic-histologic study with clinica, radiologic andimmunohisto-chemical correlations. Cancer 1997; 81: 116-121.
- Cazaban S, Icard P, Le Rochais JP, Martel B, Galateau F, Evrard C. [Pleural fibromas: a review based on 12 cases]. Ann Chir. 1999; 53: 215-221.
- Raclot A, Muller C, Grivaux M, Beroud P, Blanchon F. [A voluminous mass at the base of the thorax]. Rev Pneumol Clin. 1994; 50: 343-345.
- Le Guen Y, Hureaux J, Valo I, Jousset Y, Bizieux-Thaminy A, T. Urban. Tumeursfibreuses solitaires pleurales. À propos de deux observations Rev Mal Respir. 2004; 21 : 865-872.
- Rabiou S, Belliraj L, Abderrahim El B , Issoufou I , Ammor FZ, Ghalimi J, et al. À propos de la gestionchirurgicale de deuxtumeursfibreuses solitaires géantes. JCTCV. 2016; 20: 1-6.
- Jougon J, Minniti A, Bégueret H, Dromer C, Delcambre F, Mac Bride T, et al. [Solitary fibrous thoracic tumor: a rare tumor with unpredictable course]. Rev Pneumol Clin. 2002; 58: 35-38.
- Chermiti Ben Abdallah F, Bousnina S, Racil H, Ismail L, El Mezni F, Megdiche ML, et al. [Solitary malignant fibrous tumors of the pleura]. Rev Pneumol Clin. 2010; 66: 187-190.
- Kanthan R, Torkian B. Recurrent solitary fibrous tumor of the pleura with malignant transformation. Arch Pathol Lab Med. 2004; 128: 460-462.
- de Perrot M, Kurt AM, Robert JH, Borisch B, Spiliopoulos A. Clinical behavior of solitary fibrous tumors of the pleura. Ann Thorac Surg. 1999; 67: 1456-1459.