Case Report
A Case Report Describing Intraoperative Movement of Toric Intraocular Lens (IOL) In a Patient with Keratoconus and High Astigmatism
Alanna Wood1*, Erin Thornell2 and Smita Agarwal2
1Department of Ophthalmology, Hornsby Ku-ring-gai Hospital, Australia
2Department of Ophthalmology, Wollongong Eye Specialists, Australia
*Corresponding author: Alanna Wood, Hornsby Ku-ring-gai Hospital, Palmerston Road, Hornsby, NSW 2077, Australia
Published: 10 Oct, 2017
Cite this article as: Wood A, Thornell E, Agarwal S. A
Case Report Describing Intraoperative
Movement of Toric Intraocular Lens
(IOL) In a Patient with Keratoconus and
High Astigmatism. Ann Clin Case Rep.
2017; 2: 1441.
Abstract
Background: We present a case of intraoperative rotation of a toric lens during cataract surgery in a patient with high irregular astigmatism as a result of keratoconus. Case Presentation: Despite numerous attempts to stabilise intraoperatively, the intraocular lens (IOL) continued to rotate until a capsular tension ring (CTR) was inserted. Good centration and rotational stability was achieved and remained at follow-up. Conclusions: We propose the possibility of an irregularly shaped capsular bag in some patients with keratoconus and high astigmatism, potentially causing the IOL to rotate to a position that better accommodates the conformation of the capsular bag. Preoperative assessment of the shape of the capsular bag in patients with keratoconus may be beneficial in preventing intraoperative rotation of IOLs.
Keywords: IOL; Rotational instability; Keratoconus; Astigmatism
Introduction
Corneal ectatic disorders such as keratoconus can result in progressive corneal thinning, irregular corneal astigmatism and visually significant cataract at younger ages compared to the general population [1]. Toric IOL implantation during cataract surgery in those with significant astigmatism can provide satisfactory vision, however accurate centration and stable alignment are paramount to achieving this outcome [2]. Rotation has been reported as one of the most common causes of patient dissatisfaction in the immediate postoperative period particularly with highpowered toric lenses, with incidence of rotation being brand and type specific [2,3]. Previous case studies that have reported toric IOL instability have described utilising both single and double CTR implantation to fixate the lens in the correct position [4,5]. Implantation of IOLs in eyes with for me fruste keratoconus without the incidence of rotational instability has also been reported [6]. However, we report a case of intraoperative rotation of a toric IOL in an eye with keratoconus and high astigmatism that required the insertion of a CTR to stabilise the lens.
Case Presentation
Mrs CB, a 53-year-old caucasian female presented complaining of decreased vision bilaterally
which was long-standing in nature, being spectacle-dependent since childhood. Her symptoms
included blurring of vision, glare and difficulty reading at short and long distances. On slit lamp
examination, Mrs CB was found to have bilateral nuclear and cortical cataracts. No features of
pseudo-exfoliation syndrome or capsular fibrosis were identified and she had not had prior ocular
surgery performed. Her best corrected visual acuity (BCVA) preoperatively was 6/12 in the right eye
and 6/9 in the left eye. Refraction in the right eye was +6.0DS/-5.5DC x 15 degrees and in the left
eye +6.25DS/-5.5DC x 150 degrees. Topography demonstrated keratoconus and biometry showed
an axial length of 22.14 mm.
Intraoperatively, phacoemulsification was successfully performed bilaterally and Rayner
T-flexTM hydrophilic Aspheric 573T 12 mm IOLs were implanted and dialled to the required
positions. The right-sided IOL rotated immediately and continued to rotate despite several attempts
to reposition in the desired axis. Options for intraoperative lens stabilisation were CTR insertion or replacement of the lens with a non-toric IOL leaving her with residual
astigmatism. Intraoperatively, the IOL, despite being well centred,
was found to have rotated to 67 degrees from the desired axis of 106
degrees. The lens was repositioned and a CTR was implanted into the
bag, achieving immediate rotational stability. No zonular weakness
was noted intraoperatively. Postoperative follow-up the next day
revealed an IOL that was well centred and aligned at the desired axis,
with BCVA in the right eye of 6/7.5. Stability was maintained at 3 and
6 months postoperatively.
Figure 1
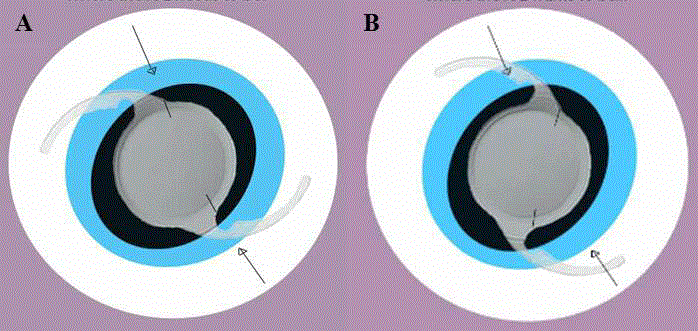
Figure 1
(A) The desired axis of the IOL. (B) The IOL following rotation to an
axis where its conformation fits the capsule most appropriately.
Discussion
The correction of irregular astigmatism in eyes with keratoconus
remains challenging, and for this reason those undergoing IOL
insertion should be carefully assessed preoperatively [6]. Up to a third
of the astigmatic correction is lost if the lens rotates by 10 degrees,
and astigmatism exceeding preoperative values results if rotation
greater than 30 degrees occurs [2,7]. Implant material, haptic design
and IOL size in relation to capsular bag are all features that can affect
spontaneous rotation and need to be considered prior to selecting an
appropriate IOL [2,8]. Over time the capsular bag contracts around
the haptics to enclose and secure the lens, but rotation of the lens
remains a possibility before this contraction occurs [9]. Therefore,
it is important to choose correct IOL size for the bag, as well as
create friction between the IOL haptic and the bag to prevent early
rotation of the lens. Those made from silicone demonstrate higher
postoperative rotation rates and often require surgical realignment
[3]. While the lens used was a hydrophilic lens, hydrophobic lenses
have generally shown greater rotational stability in the post-operative
period perhaps owing to a greater adherence to the capsule [10,11].
In our case, the lens could not be positioned at the desired axis even
intraoperatively. Regarding haptic design, both plate haptics and
open-loop haptics are options, with plate haptics conferring less
postoperative rotation than open-loop [7]. With respect to the IOL
size in relation to the capsular bag, there is a risk of rotation if the IOL
is too small and a risk of the capsular bag stretching and distorting if
too large [8]. To ensure accurate fitting prior to the procedure, the
horizontal corneal diameter and axial length are substituted into
known formulas to calculate the capsular bag diameter [9].
Despite these parameters being carefully assessed preoperatively,
we propose that in some patients with keratoconus and higher
astigmatism, the shape of the capsular bag may also confer a degree
of instability during and after implantation of a toric lens. In the case
presented, the IOL continually rotated intraoperatively, perhaps
owing to a capsular bag that was oval in shape with an apex at 65 degrees, causing the lens to rotate to this position rather than the
desired 106 degree axis (Figure 1). While there are other features as
mentioned that may contribute to rotation of an IOL postoperatively,
we propose that in some patients with keratoconus and with high
astigmatism, the capsular bag may be irregularly shaped, causing
the IOL to rotate to a position that better accommodates the
conformation of the capsular bag. Currently, no preoperative analysis
takes place to predict the shape of the capsular bag in an eye with
keratoconus. Techniques such as optical coherence tomography,
B-scan, ultrasound biomicroscopy or magnetic resonance imaging
could be employed to determine the shape and orientation in this
selected cohort.
Once a lens has rotated intraoperatively, management options
include corneal incisions or laser vision correction, as well as transscleral
suture fixation of the toric IOL. Alternatively, intraoperative
insertion of a CTR into the capsular bag enforces symmetry within
the bag, stretching the equator and flattening the bag in the anterior
and posterior axes, thereby preventing rotation [4]. In this case, a
CTR was used to achieve rotational stability in a patient with irregular
astigmatism secondary to keratoconus, yielding good visual acuity
results that persisted postoperatively. Based on our experience, we are
suggesting that preoperative assessment of the capsular bag, possibly
through a modality such as B-scan,may be beneficial in planning the
surgical outcomes of patients with keratoconus.
References
- Thebpatiphat N, Hammersmith KM, Rapuano CJ, Ayres BD, Cohen EJ. Cataract surgery in keratoconus. Eye Contact Lens. 2007; 33: 244-246.
- Chang DF. Early rotational stability of the longer Staar toric intraocular lens: fifty consecutive cases. J Cataract Refract Surg. 2003; 29: 935-940.
- Buckhurst PJ, Wolffsohn JS, Naroo SA, Davies LN. Rotational and centration stability of an aspheric intraocular lens with a simulated toric design. J Cataract Refract Surg. 2010; 36: 1523-1528.
- Sagiv O, Sachs D. Rotation stability of a toric intraocular lens with a second capsular tension ring. J Cataract Refract Surg. 2015; 41: 1098-1099.
- Safran S. Use of a capsular tension ring to prevent early postoperative rotation of a toric intraocular lens in high axial myopia. J Cataract Refract Surg. 2015; 3: 41-43.
- Nava A, Suarez R. One-year follow-up of toric intraocular lens implantation in forme fruste keratoconus. J Cataract Refract Surg. 2009; 35: 2024-2027.
- Patel CK, Ormonde S, Rosen PH, Bron AJ. Postoperative intraocular lens rotation; a randomized comparison of plate and loop haptic implants. Ophthalmology. 1999; 106: 2190-2195.
- Lim SJ, Kang SJ, Kim HB, Apple DJ. Ideal size of an intraocular lens for capsular bag fixation. J Cataract Refract Surg. 1998; 24: 397-402.
- Tehrani M, Dick HB, Krummenauer F, Pfirrmann G, Boyle T, Stoffelns B. Capsule measuring ring to predict capsular bag diameter and follow its course after foldable intraocular lens implantation. J Cataract Refract Surg. 2003; 29: 2127-2134.
- Lee JY, Kang KM, Shin JP, Kim IT, Kim SY, Park DH. Two-year results of AcrySof toric intraocular lens implantation in patients with combined microincision vitrectomy surgery and phacoemulsification. Br J Ophthalmol. 2013; 97: 444-449.
- Packer M, Rajan M, Ligabue E, Heiner P. Clinical properties of a novel, glistening-free, single-piece, hydrophobic acrylic IOL. Clinical Ophthalmology. 2014; 8: 421-427.