Case Report
Actinomycosis of Gallbladder: A Diagnostic Dilemma
Amine Elmekkaoui1*, Amal Bennani2, Mehdi Soufi3, Mohammed Bouziane3 and Zahi Ismaili1
1Department of Hepato-Gastroenterology, Mohammed I University, Morocco
2Department of Pathology, Mohammed I University, Morocco
3Department of Digestive Surgery, Mohammed I University, Morocco
*Corresponding author: Amine Elmekkaoui, Department of Hepato-Gastroenterology, Mohammed I University, BP 4806 Oujda Université 60049 Oujda, Oujda, Morocco
Published: 21 Aug, 2017
Cite this article as: Elmekkaoui A, Bennani A, Soufi M,
Bouziane M, Ismaili Z. Actinomycosis of
Gallbladder: A Diagnostic Dilemma. Ann
Clin Case Rep. 2017; 2: 1422.
Abstract
We report a rare case of gallbladder actinomycosis in an 88 years old man. The patient presented with a clinical feature of an acute cholecystitis, and a radiological finding mimicking a gallbladder carcinoma. The diagnosis of actinomycosis was made by histopathological examination of the surgical specimen, which is often the case in such infection. The surgery was followed by a longterm antibiotic treatment to prevent recurrence.
Keywords: Actinomycosis; gallbladder; Cholecystectomy; Penicillin
Introduction
Actinomycosis is a chronic suppurative and granulomatous disease characterized by its capacity to invade surrounding tissues, development of multiple abscesses, granulation and dense fibrous tissue [1]. The infection is frequently caused by Actinomyces israelii [2]. Actinomycosis of the gallbladder is an extremely rare disease; less than 50 cases have been reported in the literature [3]. Here we report a new case of actinomycosis of the gallbladder mimicking a gallbladder carcinoma.
Case Presentation
An 88-years-old North African-man presented with fever and nausea and a history of three
months of intermittent right upper quadrant pain which became severe 2 days before his hospital
admission. Past medical history showed hypertension and diabetes. Clinical examination revealed
moderate dehydration, pyrexia (39°C) and tachycardia (118 beats/min), conjunctive jaundice and a
10 cm tender mass in the right upper abdominal quadrant.
Blood tests showed high levels of white cell count (16 000/mm3) and C-reactive protein (56 mg/
dL). Hepatic blood test showed an elevated alkaline phosphatase (480 IU/L) and gamma glutamyl
transpeptidase (570 IU/L). Total and conjugated bilirubin levels were slightly high (2.1 mg/dL and
1.1 mg/dL respectively) and serum albumin was low (17 g/L). For tumor markers, carcinoembryonic
antigen and carbohydrate antigen 19-9 were normal (6.8 ng/mL and 1 U/mL respectively).
Ultrasonography reviewed an acute calculous cholecystitis and a lesion in the gallbladder,
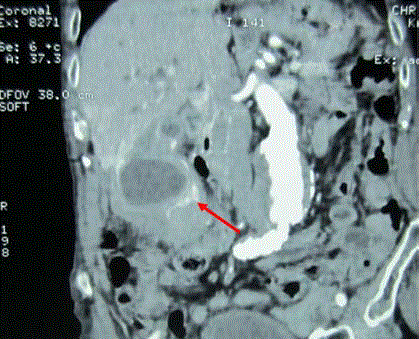
which was isoechoic to surrounding parenchyma. A Computed Tomography (CT scan) of the
abdomen was performed and showed a mass mimicking a gallbladder carcinoma (Figure 1). The
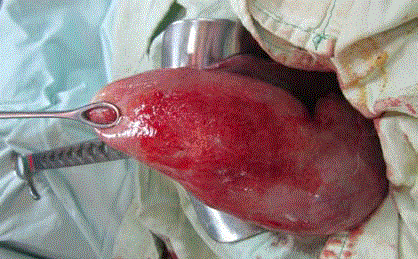
wall of the gallbladder was thickened and stones were found in the main bile duct. Intraoperative
findings suggested gallbladder cancer (Figure 2). The patient underwent a cholecystectomy with choledochotomy and placement of a Kehr drain after extraction of bile duct gallstones. Because
of the emergent context, a cholecystectomy was carried out awaiting the histological results and
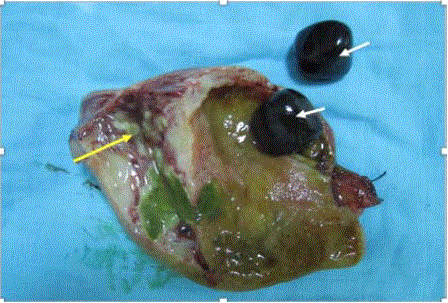
the complementary imaging before deciding the necessity of further resections. Opening of the
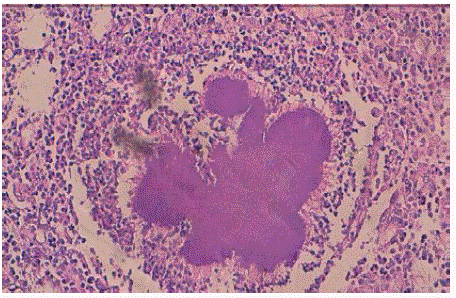
surgical specimen found a parietal thickening with the presence of multiple small abscesses (Figure 3). Histologic examination was consistent with peri-gallbladder necrosis containing numerous
bacterial colonies of Actinomyces species (Figure 4). A diagnosis of gallbladder actinomycosis was made. The patient made an uneventful recovery and was started on a 6-months cure of penicillin.
Ona year after surgery, no recurrence has been observed.
Figure 1
Figure 2
Figure 3
Figure 4
Figure 4
Chronic inflamed granulation tissue with many characteristic
'sulphur granules' of Actinomycosis, composed of basophilic radiating
filaments (hematoxilin eosin safran X10).
Discussion
Actinomycosis is an infection caused by a gram-positive anaerobic bacterium: Actimyces species
[1,3]. There are no less than 30 species of actinomyces, the most common is Actimyces Israelii.
Other species can produce infection in humans such A. Viscosus A. naeslundii, A. odontolyticus,
gerencseriae and A. meyeri [1]. The bacterium is common commensal in the mucous membrane of oral cavity, intestinal tract and female genitalia. Actinomyces were
once considered fungi because of their branching filaments [4]. Latter,
taxonomic studies confirmed that Actinomyces are bacteria rather
than fungi by virtue of their lack of nuclear membrane or cell wall
chitin, reproduction by fission, insensitivity to amphotericin B and
sensitivity to penicillin [5,6]. But the question is still debated; recently
Rothschild and al. evaluated actinomyces spp and, surprisingly, found
that it showed great similarities to fungal infections, bringing into
question its current classification as a bacterium [3,7].
Actinomyces are microorganisms of low pathogenicity and require
mucosal barrier disruption caused by trauma, surgery (e.g. perforated
acute diverticulitis or appendicitis), foreign body ingestion (e.g.
fish or chicken bone), irradiation, or local inflammatory to produce
disease [2]. Other risk factors are described, like immunosuppression
condition, neoplastic disease, diabetes and intrauterine contraceptive
devices (IUDs) [2]. Furthermore, actinomycosis is generally a
polymicrobial infection, associated with other bacteria in 65% of
cases [8]. Copathogenes may assist in the spread of infection by
inhibiting host defenses and reducing local oxygen tension. Once
infection is established a subacute-to-chronic disease is produced and
spread to surrounding tissues without regard for anatomic barriers.
The end result is a chronic, indurated, suppurative infection or a
granulomatous inflammation and frequent development of multiple
abscesses; especially in abdominal site. The fibrotic walls of the mass
before suppuration may be confused with a neoplasm [2].
The most common localization of this infection is the cervicofacial.
Ten to 20% occur in abdomino-pelvic region, which is the most
indolent and non-specific presentation [3]. The infection involves usually the ileocecal region mimicking Crohn disease or tuberculosis.
Actinomycosis of the gallbladder is a very rare condition; about 50
cases are reported in the medical literature [3,8]. In the gallbladder,
appendicitis is considered the primary source of actinomycosis, but
infection may follow a perforated intestinal ulcer or even a blunt
trauma. Retrograde spread of actinomycetes from the duodenum
through the common bile duct or hematogenous spread have been
considered as a possible route of infection [4].
There are no specific clinical or radiological signs of the infection.
A preoperative diagnosis is difficult; less than 10 % of cases are
detected preoperatively [1]. In the case of gallbladder, no reported
case of actinomycosis of the gallbladder has been diagnosed prior
to laparotomy [1]. Moreover, gallbladder actinomycosis can be
presented as a chronic cholecystitis but more frequently as an acute
disease [3]. Ultrasonography and CT scan usually reveal a tumourlike,
infiltrative mass that enhances with contrast, mimicking a
gallbladder adenocarcinoma [8]. There is no specific, valid serological
test for diagnosis. A direct cyto-bacteriological examination of the
bile collected intra-operatively, carried out by an informed biologist,
or at best an anaerobic culture could show the organism in 50% of
cases; but in the latter case it can take several weeks which is not very
useful for such cases [9]. The presence, in microbiological study, of a
non–acid-fast, a gram-positive organism with filamentous branching
is suggestive of the diagnosis [2]. It is very common for the diagnosis
to be made only after the pathological examination of the surgical
specimen.
After a cholecystectomy, prolonged antimicrobial therapy (6 to
12 months) is recommended for patients with all clinical forms of actinomycosis to prevent disease recrudescence. However, adequate
drainage is indicated if abscesses are present [2]. The treatment of
choice is high dose intravenous penicillin followed by oral penicillin
alone (i.e., amoxicillin, piperacillin) or combined with β-lactamase
inhibitor (i.e., clavulanate, tazobactam) to cover others aerobic and
anaerobic co-pathogens [2,9].
Conclusion
Gallbladder actinomycosis is a very rare condition that mimics a wide variety of intra-abdominal complains such as malignant disease. The diagnosis is difficult and usually post-operative, made by the histological examination of the cholecystectomy specimen. The treatment needs long term antibiotics to avoid recurrence.