Case Report
Avoiding General Anesthesia for a Patient with Severe Pulmonary Compromise
Priyesh R Patel*, Heather D McFarland, Nicholas L Pesa and Nicole D Snyder
Department of Anesthesiology and Perioperative Medicine, University Hospitals Case Medical Center, Case
Western Reserve University School of Medicine, USA
*Corresponding author: Priyesh R Patel, Department of Anesthesiology and Perioperative Medicine, University Hospitals Case Medical Center, Case Western Reserve University School of Medicine, 11100 Euclid Avenue, Cleveland, Ohio 44106, USA
Published: 18 Aug, 2017
Cite this article as: Patel PR, McFarland HD, Pesa
NL, Snyder ND. Avoiding General
Anesthesia for a Patient with Severe
Pulmonary Compromise. Ann Clin Case
Rep. 2017; 2: 1420.
Abstract
Patients with severe pulmonary disease are sometimes denied necessary surgical procedures given the foreseen perioperative complications of general anesthesia, including respiratory failure, atelectasis, and pneumonia.Little data has been reported on the use of neuraxial anesthesia in attempt to avoid general anesthesia and the associated use of muscle relaxants and endotracheal intubation in this patient population. Our case report demonstrates the use of epidural anesthesia with the complete avoidance of general anesthesia in a patient with severe pulmonary disease, undergoing a hemicolectomy and end ileostomy for a high-grade adenocarcinoma of the colon.
Introduction
All patients undergoing general anesthesia are at risk for perioperative pulmonary complications in the form of respiratory failure, pneumonia, and atelectasis. Furthermore, major abdominal surgery in the setting of underlying Chronic Obstructive Pulmonary Disease (COPD) places patients at a significantly increased risk of such complications, especially in the postoperative period. Sources have suggested that the avoidance of general anesthesia may mitigate some degree of the above mentioned pulmonary decline [1]. Other benefits that have been appreciated by this approach include superior hemodynamic stability [1,2]. Our case demonstrates a technique to avoid general anesthesia with the primary goal of avoiding additional insultin a patient with preexisting severe respiratory disease.
Case Presentation
A 72-year-old male presented with a colonic mass at the hepatic flexure requiring surgical intervention. His past medical history was most notable for severe COPD and Coronary Artery Disease (CAD). Recent pulmonary function testing showed that both the Forced Expiratory Volume in 1 second (FEV1) and Forced Vital Capacity (FVC) were 0.75 liters (L) and 1.7 L, respectively. The FEV1/FVC ratio was 43%. The patient was compliant with his pulmonary medications, which included albuterol, ipratropium, tiotropium, and prednisone. He was previously denied surgical intervention at another institution citing a high risk of perioperative pulmonary complications. After evaluating the patient, our team elected to offer surgery with Neuraxial Anesthesia (NA) as the primary anesthetic. We discussed our concerns and the consideration for NA with both the surgeon and patient. All parties were cooperative and understanding of the benefits and limitations. We took the patient to the operating room and provided supplemental oxygen via facemask. Standard monitors were placed. An epidural catheter was placed in the lumbar area, at the L1-L2 interspace, to minimize thoracic compromise, cardiac accelerations, and extensive sympathectomy in the setting of CAD. Twenty-five milligrams of bupivacaine 0.25% were injected via the epidural catheter. This provided anesthesia to the T6 dermatomal distribution at 15 minutes. Midazolam sedation was provided. A dose of fentanyl 100 micrograms was provided via the epidural catheter for intraoperative analgesia at the commencement of the procedure. An open right hemicolectomy and end ileostomy was completed in 60 minutes by the surgeon without complication. The epidural catheter was kept in place for post-operative analgesia. No perioperative pulmonary decline was noted. The epidural was removed on post-operative day three and his respiratory status remained stable throughout his hospital stay.
Figure 1
Figure 1
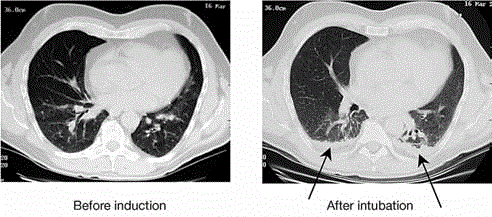
Computer topography scan of a healthy patient before (left) and
after (right) general anesthesia with intubation. The level is 1 cm below the
right diaphragm. Arrows indicate the immediate collapse of lung fields.
Discussion
Many patients with severe pulmonary compromise are denied surgery, as they are prone to
further functional decline in the postoperative period. GA induction and intubation results in the immediate dependence of mechanical ventilation. GA also places the
patient at risk for bronchospasm, V/Q mismatch, pneumothorax, and
respiratory depression from residual anesthetic and muscle relaxant.
In comparison, although not completely benign, NA can mitigate
some of these risks. For example, the decrease in functional residual
capacity brought by abdominal surgery is less profound under NA in
that diaphragmatic function and chest wall compliance are improved.
Conversely, NA can negatively influence FEV1 secondary to
diminished abdominal muscle tone. This may result in the reduction
of coughing and also the clearance of pulmonary secretions. However,
aggressive pulmonary toilet in the perioperative time period can help
overcome these issues [3,4].
In a review by Groeben, the physiological effects of neuraxial
anesthesia are outlined. With a sensory blockade between the T1-T5
dermatomes provided by a thoracic epidural, there was a decrease
in vital capacity (VC) of 5.6% and a decrease in FEV1 of 4.9%
from baseline. Furthermore, a wider blockade between the C4-T7
dermatomes resulted in a decrease in VC of 25% and decrease of FEV1
of 13%. Though the epidural anesthesia did change these parameters
significantly, the decreases were not detrimental in the clinical setting
[5]. In comparison, with patients undergoing cholecystectomy with
GA alone, there was a decrease in FEV1 by 55% [6]. FEV1 is reflective
of the ability to cough, which is an important postoperative measure of
lung function and in the clearance of secretions. During the recovery
period from GA, FEV1 is further compromised by residual muscle
relaxant, which decreases the patient’s ability to cough. Conversely,
when employing NA as the sole anesthetic, muscle relaxant is avoided
and thus eliminates the dramatic negative impact on FEV1.
Even when NA is employed in the setting of GA, patients were
able to perform VC and FEV1 tests one hour after extubation, while
patients with GA alone could not [5]. This is significant in that it
suggests the earlier return of baseline pulmonary function.
After abdominal surgery, there is a reduction in VC by at least
60%. Using thoracic epidural anesthesia has shown improvements
of Functional Residual Capacity (FRC) from 21.7 % to 15.9% and
reduced the diminished VC from 63% to 45%. The mechanism
behind this include superior pain control and the minimization of
opioid pain medication, as well as improved diaphragmatic function
secondary to the blockade of reflexes that inhibit diaphragm function
after an abdominal surgery [7]. In turn, patients are able to take deeper
breaths, cough, and participate is physiotherapies, such as incentive
spirometry [7]. Pulmonary gas exchange is also impaired when using
GA due to intrapulmonary shunting secondary to atelectasis and V/Q
mismatch. This is shown on computerized tomography as collapsing
of lung fields that occurs immediately after GA and intubation (Figure 1). Theoretically, regional atelectasis may result when employing
neuraxial techniques. This is secondary to both decreased muscle
tone and diaphragm movement. However, there is evidence that
GA with the addition of NA had no increase of V/Q mismatch or
gas exchange impairment [6]. Additionally, even when high thoracic
epidural anesthesia is used, there is no difference in arterial–alveolar
gradient or in the measure of direct shunt [5].
Patients with severe COPD already have a diminished FEV1.
There is concern that NA decreases VC and further depressesFEV1.
Nonetheless, the data suggests that the reduction in FEV1 in patients
with COPD compared to those free of pulmonary disease (8-10%) is
much less [5].
More recently, Guay published an article comparing the effects
of NA and GA on perioperative and postoperative morbidity and
mortality, including death, chest infections, myocardial infarction
and serious adverse event outcomes. All Cochrane Reviews that were
included in this study spanned from the use of NA with or without GA
to GA alone in adult patients with intermediate or high cardiac risk.
Notable was the reduction in 0 to 30 day mortality in the setting of NA
in comparison with GA and a decreased risk of pneumonia with NA
compared to GA [3]. Another advantage of epidural anesthesia is that
it blunts the stress response, during and after surgery, and decreases
the resulting inflammatory and coagulation pathways associated
with it. In turn, there is a reduction in the likelihood accompanying
sequelae, such as thromboembolic complications, myocardial
ischemia and infarction, impaired pulmonary function, ileus, fatigue,
postoperative infection and postoperative confusion [7].
Determining the appropriate patient population to direct NA
as the primary anesthetic is significant. It appears from our review
that given the pulmonary benefits, patients with severe lung disease
may benefit from this strategy. Thus, determining the chances
of a postoperative pulmonary complication would be of help.
Canet performed a prospective, multicenter, observational study
with intents of developing a predictive index for postoperative
pulmonary complications. Seven statistically significant independent
predictors including low preoperative arterial oxygen saturation,
acute respiratory infection in the previous month, age, preoperative
anemia, upper abdominal or intrathoracic surgery, surgical duration
of two or more hours, and emergent surgery [8]. This gave rise to the
ARISCAT risk index, which developed a point system using the seven
independent risk factors determined by the study. The incidences of
pulmonary complications correlate as 1.6% in low scoring patients,
13.3% in intermediate scores and 42.2% in high scores. Utilizing this
assessment may be useful in deciding the patients that can benefit
from NA as opposed to GA [8].
Ultimately, the literature analyzing the use of NA with the
complete avoidance of GA is greatly limited. In our search, two other
cases were reported where GA was avoided and regional or combined
lumbar spinal-thoracic epidural anesthesia was used with successful
outcomes and no adverse pulmonary events; yet, neither utilized a
neuraxial technique as the primary anesthetic [2,9]. Much of the
research in this area includes a population which has undergone
epidural anesthesia in combination with general anesthesia. In
addition, many of the studies are small in sample size and outdated
[10]. Large randomized multicenter studies are needed to determine
if there is a true benefit in using NA to avoid pulmonary compromise
in patients with severe COPD.
Conclusion
References
- Van Lier F, van der Geest PJ, Hoeks SE, van Gestel YR, Hol JW, Sin DD, et al. Epidural analgesia is associated with improved health outcomes of surgical patients with chronic obstructive pulmonary disease. Anesthesiology. 2011; 115: 315-321.
- Oriana Ng, Sze Ying Thong, Claramae Shulyn Chia, Melissa Ching Ching Teo. Revision of loop colostomy under regional anaesthesia and sedation. Singapore Med J. 2015; 56: e89-e91.
- Guay J, Choi PT, Suresh S, Albert N, Kopp S, Pace NL. Neuraxial anesthesia for the prevention of postoperative mortality and major morbidity: An overview of cochrane systematic reviews. Anesth Analg. 2014; 119: 716-725.
- Savas JF, Litwack R, Davis K, Miller TA. Regional anesthesia as an alternative to general anesthesia for abdominal surgery in patients with severe pulmonary impairment. Am J Surg. 2004; 188: 603-605.
- Groeben H. Epidural anesthesia and pulmonary function. J Anesth. 2006; 20: 290-299.
- Clemente A, Carli F. The physiological effects of thoracic epidural anesthesia and analgesia on the cardiovascular, respiratory and gastrointestinal systems. Minerva Anestesiol. 2008; 74: 549-563.
- Nimmo S. Benefit and outcome after epidural analgesia. BJA. 2004; 4: 44-47.
- Canet J1, Gallart L, Gomar C, Paluzie G, Vallès J, Castillo J, et al. Prediction of postoperative pulmonary complications in a population-based surgical cohort. Anesthesiology. 2010; 113: 1338-1350.
- Kapala M, Meterissian S, Schricker T. Neuraxial anesthesia and intraoperative bilevel positive airway pressure in a patient with severe chronic obstructive pulmonary disease and obstructive sleep apnea undergoing elective sigmoid resection. Reg Anesth; 34: 69-71.
- Kettner SC, Willschke H, Marhofer P. Does regional anaesthesia really improve outcome?. BJA. 2011; 107: i90-i95.