Case Report
Benefits of Physical Therapy Interventions for a Patient with End-Stage Pulmonary Disease who developed Right-Sided Heart Failure Requiring ECMO Support Bridging to Lung Transplantation
Samantha Mancuso#, Kirby Mayer*# and Anil Gonipath
Rehabilitation Sciences Doctoral Program, University of Kentucky, USA
#Both the authors contributed equally
*Corresponding author: Kirby Mayer, Samantha Mancuso, Rehabilitation Sciences Doctoral Program, College Health Sciences, University of Kentucky, 900 S. Limestone, CTW Lexington, KY 40536- 0200, USA
Published: 17 Jul, 2017
Cite this article as: Mancuso S, Mayer K, Gonipath
A. Benefits of Physical Therapy
Interventions for a Patient with End-
Stage Pulmonary Disease who
developed Right-Sided Heart Failure
Requiring ECMO Support Bridging to
Lung Transplantation. Ann Clin Case
Rep. 2017; 2: 1402.
Abstract
Background: Extracorporeal Membrane Oxygenation Support (ECMO) is the highest level
of life support. The purpose of this case report is to establish the multi-disciplinary approach
to rehabilitation in a novel patient case. The report establishes the safety and importance of
rehabilitation interventions during two phases of the patient’s critically complex medical course.
Case Presentation: A 50-year-old male diagnosed with advanced idiopathic pulmonary fibrosis
that required ECMO support as a bridge to lung transplantation. During the pre-transplantation
phase, the patient suffered significant decline leading to the development of right-sided heart failure
and acute kidney injury. The severity of his medical condition required multiple re-configurations
of the ECMO circuit to maximize cardio-respiratory support. Rehabilitation interventions were
implemented during both pre- and post-transplant stages with emphasis placed on a multidisciplinary
approach to delivery of interventions.
Outcomes: On day 50, the patient underwent successful bilateral lung transplantation. During
both phases, there were no adverse events during any rehabilitation session. In addition, the patient
progressed from fully dependent in the initial stages to a modified independence state at hospital
discharge. The complicated and novel case (IPF developing right sided heart failure requiring
multiple cannulation strategies) demonstrates the feasibility and importance of physical therapy to
improve pre-transplantation status as well as maximize outcomes following surgery.
Discussion: There is limited evidence describing rehabilitation interventions for critically ill
patients requiring ECMO support. This case report confirms that physical therapy can be safely
implemented in the most complex cases. The case report also attempts to show the importance of
implementing physical therapy to best prepare the patient for transplantation surgery.
Introduction
Extracorporeal Membrane Oxygenation Support (ECMO) is a therapeutic intervention utilized
for patients suffering from cardio-respiratory failure. ECMO, the highest level of life support, allows
for different perfusion strategies to temporarily support patients as they recover or to facilitate as
a bridge to transplantation (heart or lung) [1,2]. ECMO provides cardiorespiratory support by facilitating gas exchange and perfusion through a device outside the body. Cannulas placed in
large caliber veins direct deoxygenated blood to the membrane oxygenator outside the body. The
oxygenator replenishes oxygen and removes carbon dioxide through the juxtaposition of airflow
and blood across a semipermeable membrane. The blood is then returned through a different
channel (either in the same cannula – double lumen cannulation, or in a different cannula – two
single lumen cannulae). A pump (commonly, a centrifugal pump in adults) assists the flow through
the circuit and may also, in Veno-arterial (VA) ECMO contribute directly to the generation of an
arterial pressure gradient; this promotes adequate systemic perfusion. VenoVenous (VV) ECMO
(drainage from and return to the venous system) is used primarily for respiratory support in acute
respiratory failure to manage refractory hypoxia, hypercapnia and respiratory acidosis or both [1]. Comparatively, VA ECMO is used for hemodynamic support in patients with decompensated heart
failure who may also have respiratory compromise [1,2].
ECMO interventions are high-risk, invasive procedures
undertaken in critically-ill patients. A multi-center randomized
controlled trial (CESAR) in the UK compared ECMO with
conventional mechanical ventilation for severe Acute Respiratory
Distress Syndrome (ARDS). The CESAR study suggested that ECMO
was associated with an improved rate of survival [3]. The collaboration
of the multidisciplinary team is essential to maximizing the benefits
of ECMO therapy. However, ECMO is not without its complications.
The nature of the device presents multiple risks including hemorrhage,
extremity ischemia, thrombosis, infection, and pump/oxygenator
failure [4]. Complications also arise from the complexity of treating a
critically-ill patient including prolonged immobility, use of sedation,
and long term mechanical ventilation [5-7]. To address these issues,
early mobilization has been identified as a key intervention. Recent
research has established that early mobilization has many benefits
including improved survival rates, prevention of multi-organ system
failure, prevention of pressures ulcers and reduction in long-term,
critical illness related to neuromuscular dysfunction [5,6,8,-12].
Rehder et al. [13] found that “awake ECMO” patients had improved
survival rates, reduced wait-times to transplant surgery and notably
shorter post-transplant length of hospital stay. Furthermore, it has
been suggested that pre-transplant conditioning is an important
predictor of morbidity and mortality in patients who undergo ECMO
therapy [13].
Early mobilization in patients requiring ECMO is possible
through improvements in technology. The introduction of the
Avalon double lumen cannulas, improved portability, and enhanced
membrane oxygenator design has allowed patients to mobilize easier
and with reduced risks. The use of ECMO has allowed facilitated a
reduction in the need for mechanical ventilation and sedation in
patients with ARDS, allowing them to engage in Activities of Daily
Living (ADL) as well as rehabilitation exercises.
Rehabilitation in the form of physical therapy may improve
physical functioning and conditioning; this is likely to better prepare
critically ill patients for either organ transplant or return to baseline
functioning prior to critical illness. The complexity of cannulation
strategies, disease types and patient demographics present a challenge
in terms of validating physical therapy interventions in patients
receiving ECMO therapy. Furthermore, evidence supporting physical
therapy interventions with patients on ECMO is limited. Case reports,
however, can provide insight and confirm the need for early physical
therapy interventions with this select population.
The purpose of this case report is to describe safe and effective
physical therapy interventions utilized to treat a patient with endstage
pulmonary disease as he awaited transplantation (on ECMO) and in the post-transplant recovery phase. The patient case is a novel case due to the complexity of the patient’s pre-transplant medical
condition requiring multiple re-configurations of the ECMO circuit
due to his deteriorating medical condition including onset of rightsided
heart failure. The physical therapy plan of care required ongoing
modifications as cannulation strategies were adjusted to provide
continued support in the face of progressive cardiopulmonary disease.
Clinical Findings and Hospital Stay
A 50-year-old male with significant past medical history of
COPD and histoplasmosis was hospitalized in February 2014 for
pneumonia and then transferred to the University of Kentucky on
April 5, 2014. Initially, he required high-flow supplemental oxygen
to maintain oxygen saturation; however, in spite of significant
support, he continued to become progressively more hypoxemic. An
extensive workup including clinical assessment, radiographic picture,
and bronchoscopy results were consistent with a new diagnosis
of advanced idiopathic pulmonary fibrosis. Due to the patient’s
clinically deteriorating lung function and likely candidacy for lung
transplantation, the patient was brought to the Cardiothoracic
Intensive Care Unit to initiate Veno-Venous (VV) ECMO. This was
performed with a size 27 French Avalon cannula inserted through
the right internal jugular vein with a goal of bridging the patient to
lung transplantation. After cannulation, the patient developed an
Acute Kidney Injury (AKI) with etiology of acute tubular necrosis
likely a combination of low flow (flow of approximately 4.2 Liters)
and high vancomycin levels; he eventually required continuous
renal replacement therapy and intermittent hemodialysis which
complicated mobility as well. He underwent a tracheostomy on day 5
to help with ambulation on ECMO and his kidney function continued
to worsen. On day 12, due to concerns for right heart failure (Table 1) and continued less than optimal oxygenation, he was transitioned
to venoarterial-venous (VAV) ECMO with cannulation in the left
femoral artery with a 17 French cannula to provide enhanced systemic
perfusion and support; this ultimately provided an additional two
liters of flow. On day 15, he was transitioned to venovenous-arterial
(VVA) ECMO with de-cannulation of the left femoral arterial
cannula and placement of a right axillary arterial 22 French cannula.
This promoted enhanced mobility with few limitations to walking
except use of the right shoulder.
On day 55, he underwent bilateral orthotropic lung transplantation
which was complicated by bleeding of the left hemithorax
necessitating re-exploration of the surgical site and administration of
favor VII. Due to this complication, the patient was left with an open
sternotomy which was closed on post-operative day 3. This limited
the patient to passive range of motion only during that time. Also, during that time, there was concern for subclinical seizures (clinically, a change in mental status with abnormal EEG findings of generalized
slowing and intermittent bifrontal and right fronto-temporal sharp
waves). On day 58, he returned to OR for pleural washout, closure of
the sternum, and therapeutic bronchoscopy. During recovery phase
of transplantation, he required frequent therapeutic bronchosc opic
procedures to clear secretions daily initially and moving out to every
other day. On day 106, his tracheostomy was removed and he was
discharged from the hospital the next day.
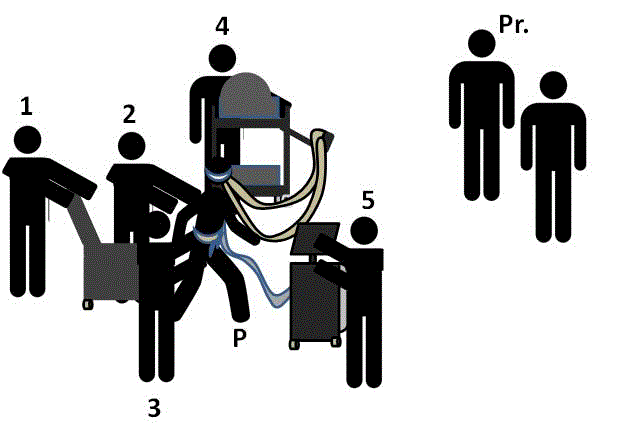
Figure 1
Figure 1
ECMO Mobility Interdisciplinary Team.
The multidisciplinary team is essential to the safety of ambulatory ECMO programs and the success of therapy interventions aimed at preventing deconditioning prior to transplant so that post-transplant outcomes may be optimized.
Key: 1: Nursing Care Technician or Physical Therapy Technician; 2: Physical Therapist; 3: Occupational Therapist; 4: Perfusionist or Nurse; 5: Respiratory Therapist; Pr.: Physician, Advanced Practice Provider, or Nurse; P: Patient on ECMO.
The Incorporation of Physical and Occupational Therapy Interventions to Promote Mobility
This patient required ECMO for irreversible end-stage respiratory
failure as a means of bridging to lung transplantation. Physical
therapy interventions are vital to prepare for a successful surgery
and promote recovery following surgery to minimize deconditioning
and optimize functional status. Physical therapy in the postoperative
period is equally as important to the success of the patient with
emphasis placed on restoring independence and functional mobility.
In the bridge to transplant and recovery stages, the goal of physical
therapy interventions is to optimize physical functioning in order to
maximize medical outcomes and quality of life following discharge
from the hospital. The severity of this patient’s illness presented
multiple barriers to rehabilitation. First, safety is a primary concern
in all phases of hospitalization. This is further emphasized when a
patient is receiving ECMO therapy. Ensuring safety of the ECMO
patient requires a well-coordinated multidisciplinary approach
with the assistance of many care providers (Figure 1). Effective
communication with all involved parties is essential to ensure safe
and effective therapy. Collaboration to ensure the ECMO circuit is
constantly monitored to decrease risk of an adverse event is essential.
Potential risks include dislodgement of a thrombus during physical
activity, mal-positioning of cannulas resulting in decreased flow,
and the accidental disengagement of cannula connections that could
result in massive hemorrhage and distributive shock. These risks
can result in fear or uncertainty of the multidisciplinary team; thus,
extensive training and troubleshooting of problems is required of all
professional working with patients on ECMO. Figure 1 describes how
the Mechanical Circulatory Support (MCS) team organized ECMO mobility.
Additionally, early mobility is further restricted by placement of
certain arterial cannulations. For example, this patient had a femoral
arterial cannulation present initially which limited hip flexion; hip
flexion can occlude the cannula preventing blood flow to the distal
extremity and the body overall. This occurred in this case study and
was one reason for fewer PT interventions prior to transplantation.
In most cases supine interventions can still be conducted but are
not preferred to exercises that involve standing and walking because
upright exercise engage all of the muscles, promote trunk control and
improve strength.
Furthermore, the placement of arterial cannulations in areas such
as the axillary artery can limit ROM of the upper extremities, resulting
in decreased strength and deconditioning that affects independent
activities of daily living. This cannulation limited occupational therapy
treatments to the fullest extent for this particular patient. Thus, the
rehabilitation plan of care must be fulfilled in a way that addresses
cannulation sites to promote safety and optimizing treatment.
Physical Therapy Examination
The initial physical therapy evaluation was conducted on
day 6 (two days after initiation of ECMO support). In addition to
the physical therapist, a perfusionist, nurse, and a nursing care
technician were present for initial examination to monitor the patient
and ECMO circuit. The patient was able to follow commands, but
required constant verbal and tactile cues to maintain alertness; he was
repeatedly distracted by fatigue and inability to keep his eyes open.
He communicated with hand and facial gestures as he was unable
to vocalize due to tracheostomy placement. The patient required
dependent assistance to perform rolling in bed as well as moving from
supine to sitting at the edge of the bed. Once in the sitting position,
he had difficulty maintaining control of his trunk and head without
support from the therapist. The patient remained sitting for twelve
minutes with vital signs stable, but had severe difficulty maintaining
arousal, requiring repeated stimulation. The physical therapist
determined that the patient could not safely attempt standing due to
severe weakness, fatigability, and difficulty maintaining arousal. In
addition, muscle manual testing was difficult to fully assess; he had
significant weakness throughout. This signifies the weakness and
deconditioning from reduced mobility from initial hospitalization in February as well as one week of full immobility.
The initial assessment revealed that his functional mobility was
severely impaired due to severely decreased activity tolerance from
poor cardiopulmonary function. Prolonged immobility (~37 days
immobility: 6 days in our hospital plus 31 days at transferring facility)
resulted in significant weakness and reduced physical functioning.
Based on his initial physical therapy evaluation combined with
evolving medical condition, the patient was a poor candidate for lung
transplantation. An intensive physical therapy plan was developed
and implemented to improve his candidacy in preparation for lung
transplantation. An updated plan was established following surgical
interventions to focus on interventions to maximize independence
and functional mobility.
Table 1
Table 1
Physical therapist initial systems review.
Abbrevations: BUE: Bilateral Upper Extremities; BLE: Bilateral Lower Extremities; RUE: Right Upper Extremity; LUE: Left Upper Extremity; PROM: Passive Range Of Motion; WFL: With Functional Limitations
Therapeutic Interventions
Pre-transplantation interventions (Bridge phase)
During the pre-transplantation phase or bridge phase physical
therapy interventions focused on tolerance to activity to improve
overall physicality. Initially the patient engaged in bed mobility tasks
and sitting upright at the edge of the bed with assistance. Progression
to standing interventions were delayed as the patient presented with
severe weakness, deconditioning, and a femoral arterial cannula
which prevented this. The physical therapist gradually progressed
interventions by reducing the assistance level with tasks in bed and
during sitting upright, thus maximizing patient work load. The
therapist continued this progression until the patient demonstrated
improved core and trunk strength in the sitting then standing
positions. The first standing interventions lasted only a few seconds
and the patient required substantial assistance to achieve and
maintain erect, upright position.
In addition to sitting and standing interventions in the bridge
phase, the therapist emphasized therapeutic exercises to increase
tolerance to activity and improve strength. The therapist encouraged
the family to assist the patient with performance of these exercises
three times per day, providing written instruction and verbal
feedback. These exercises focused on gross movements of the arms
and legs to improve global strength and cardiovascular function.
Exercises were crucial on days when the physical therapist was not available to incorporate mobility into the daily plan of care. In the bridge phase, mobility other than rolling in bed was deferred multiple
days due to evolving medical condition including development of
right-sided heart failure with patient requiring changes in location
of cannulation, femoral cannulas, femoral central lines, decreases
in alertness, worsening of kidney function and hemodynamic
instability. His right-sided heart failure included severe dilatation of
the right ventricle and pulmonary artery resulting in an estimated
right ventricular systolic pressure of 50 mm Hg to 60 mm Hg. The
patient also had peripheral signs including peripheral edema, hepatic
steatosis, and borderline splenomegaly. See Table 2 for a summary of
interventions.
Post-transplantation interventions (Recovery phase)
Following surgery, the patient was severely debilitated with
significant weakness. During the immediate postoperative period,
the patient was critically ill requiring extensive medical interventions
including vasopressor support to maintain adequate blood pressure
and subsequent perfusion. After sternal closure and washout, the
patient’s clinical condition began to improve each day, allowing for
increased participation in daily physical therapy interventions. The
patient engaged in a variety of rehabilitation interventions including
bed mobility training, transfer training, gait training, therapeutic
exercises, balance training and activity tolerance training. Given
the duration and complexity of his critical illness, the patient had
to re-learn how to perform many ADLs such as bathing, dressing,
toileting, hygiene, eating and transferring. The physical therapist
utilized a variety of strategies for learning including the cognitive and
psychomotor domains. Strategies included verbal and tactile cues as
well as demonstration of activities with teach back methods. Learning
was evaluated using return demonstration of psychomotor skills
and limiting feedback as time progressed to allow the patient time
to reflect on importance of skills learned; this utilized the affective
learning domain.
During the recovery phase, the patient followed a gradual
progression pattern that was positive in nature. Each therapy
session, the patient demonstrated improved strength and tolerance
translating to less assistance. For example, after transplantation, the
patient required max assistance of two people to perform one sit to stand transfer. Two weeks after surgery, the patient could stand
with moderate assist of one person. Once the difficulty of standing
decreased, the therapist initiated bed to chair transfer training. This
intervention expanded upon sit to stand transfer with the addition of
pivoting to a chair. This eventually evolved to side to side and forward
steps from the bed to the chair. This was a significant milestone as this
allowed him to sit upright in a chair for extended periods, but also
marked the beginning of gait training. This has great implications for
his respiratory status postoperatively as it allowed him to properly
expand the lungs and participate in pulmonary hygiene with physical
exercise.
As time progressed, walking became an important component of
the patient’s physical therapy. Ambulation demands global strength,
tolerance to activity, coordination, and balance. Once the patient
demonstrated the strength to participate in ambulation, the therapist
shifted focus from tasks in the sitting position to maximizing his ability
to walk. The patient, once again, gradually improved his ambulation
distance as the days passed. Initially, he required support of a thoracic
walker with multiple rest periods to travel a total of fifty feet. Goals
for ambulation were communicated to the multidisciplinary team to
promote recovery for the patient including the use of nursing and ancillary staff. At discharge, the patient successful performed 1000 feet of ambulation using a rolling walker and only contact guard assist
for safety. See Table 3 for the patient’s physical and occupational
therapy milestones.
Post transplantation, therapeutic exercises were used in adjunct
to the patient’s daily session of therapy that included ambulation.
A detailed, progressive exercise program was established including
upper and lower extremities exercises performed at least three times
a day. These exercises focused on isolated muscle strengthening due
to severe weakness in the patient’s hips, shoulders, and core. The
therapist also initiated and coordinated care to include exercises
against manual resistance or a resistive exercise band. Patient
confidence and motivation to perform the home-exercise plan was
crucial to his adherence to his therapy regimen during the recovery
phase. As the patient’s functional mobility improved, the therapist
initiated higher-level exercises such as standing dynamic balance
exercises.ancillary staff. At discharge, the patient successful performed 1000
feet of ambulation using a rolling walker and only contact guard assist
for safety. See Table 3 for the patient’s physical and occupational
therapy milestones.
Post transplantation, therapeutic exercises were used in adjunct
to the patient’s daily session of therapy that included ambulation.
A detailed, progressive exercise program was established including
upper and lower extremities exercises performed at least three times
a day. These exercises focused on isolated muscle strengthening due
to severe weakness in the patient’s hips, shoulders, and core. The
therapist also initiated and coordinated care to include exercises
against manual resistance or a resistive exercise band. Patient
confidence and motivation to perform the home-exercise plan was
crucial to his adherence to his therapy regimen during the recovery
phase. As the patient’s functional mobility improved, the therapist
initiated higher-level exercises such as standing dynamic balance
exercises.
Table 2
Discussion
The patient had very little cardiopulmonary reserve and reduced
muscular endurance both pre and post-bilateral lung transplantation.
Activity tolerance training was implemented into every session not
separately as it is in some circumstances. The patient participated
in physical therapy interventions at minimum five times per week
as well as daily activity and exercises driven by nursing and family
during both stages pre- and post-transplantation. Nursing and
family provided interventions were directed by the therapists. In
addition to physical therapy, the patient received interventions
focused on strength and activity from an occupational therapist.
After discharge, the patient repeatedly stated his thankfulness for the
ability to perform simple task such as brushing his teeth or washing
his hair with the occupational and physical therapist. The use of the
multidisciplinary team as well as role identification for the patient’s
family seemed to optimize the patient’s experience and allow him to
grow both physically and mentally. Particularly, nursing staff and the
family focused on mental well-being; they served as a major source of
psychosocial support for the patient in his journey to recovery. Close
communication and education delivered by the physical therapist
positively influenced the patient’s strength and tolerance both pre
and post-transplant. Task completion improved as the need for rest
breaks slowly dissipated. As the patient grew more tolerant of activity,
his confidence increased. The patient seemed to gain more selfefficacy
as well which also greatly improved his tolerance to activity
because he believed he could achieve the goals set forth before him.
In regards to functionality, the patient improved his score on
the Kansas Functional Outcome Measure from a 1/28 on initial
PT evaluation to a 24/28 at discharge. In addition, the patient
was performing bed mobility, transfers, and ADLs with modified
independence; this was a significant improvement from dependency
at initial evaluation. During his final PT intervention, the patient
performed 1,000 feet of gait with an assistive device, on room air with
no rest breaks and no assistance.
It is important to note that during the patient’s physical
therapy program, no adverse events occurred during any activity.
Both phases of rehabilitation were performed in a safe, controlled
environment with a strong emphasis on communication between the
multidisciplinary team. Additionally, physical therapy interventions
did not result in the worsening or acute changes of the patient’s
medical condition at any point in time. As the patient progressed,
the therapist increased the difficulty of intervention to appropriately
challenge the patient’s functional status and mobility. As the patient
progressed, the proper number of staff and care providers was
available. This often included a one to one ratio of the primary nurse
to the patient in addition to physical rehabilitation technicians,
nursing care technicians, therapists (both physical and occupational),
perfusionists, and respiratory therapists. The multidisciplinary
involvement of this patient was essential to his success in therapy
while on ECMO as well as post transplantation.
Table 3
Conclusion
This case reports demonstrates how a fifty-year-old patient with
idiopathic pulmonary fibrosis was able to safely ambulate while on
ECMO and how that therapy improved his functional status posttransplant.
Although his medical course was complicated by rightsided
heat failure, physical therapy interventions proved effective
and did not result in any adverse events or negative unintended
consequences in regards to his medical condition. This case shows
how a well-integrated physical rehabilitation program contributed to
the patient’s improved physicality, activity tolerance, and self-efficacy
in regards to physical activity.
The methodology used in this case is based on evidence that
suggests physical rehabilitation can be successful in patients who
require ECMO support suffering from advanced lung disease [14].
Furthermore, clinicians have noted that therapy can be safe and
effective for patients awaiting lung transplantation; however, there
is limited research in this population [15]. As the use of ECMO
increases, more evidence is needed to support mechanical circulatory
support (MCS) programs in their development of ambulatory ECMO
teams. Identification of how therapy is initiated, communicated to
the interdisciplinary team, and implemented with the assistance
of multiple disciplines can set a foundation for the development
of such programs. The determination of valid and reliable tools to
track physical progress in this population would also be beneficial.
Therefore, it is important to identify trials, tribulations, and lessons
learned so that the care of patient’s on ECMO therapy may be improved.
References
- Shekar K, Mullany DV, Thomson B, Ziegenfuss M, Platts DG, Fraser JF. Extracorporeal life support devices and strategies for management of acute cardiorespiratory failure in adult patients: a comprehensive review. Crit Care. 2014; 18: 219.
- Fraser JF, Shekar K, Diab S, Dunster K, Foley SR, McDonald CI, et al. ECMO – the clinician’s view. ISBT Science Series. 2012; 7: 82-88.
- Thalanany MM, Mugford M, Hibbert C, Cooper NJ, Truesdale A, Robinson S, et al. Methods of data collection and analysis for the economic evaluation alongside a national, multi-centre trial in the UK: conventional ventilation or ECMO for Severe Adult Respiratory Failure (CESAR). BMC Health Serv Res. 2008; 8: 94.
- Tramm R, Ilic D, Davies AR, Pellegrino VA, Romero L, Hodgson C. Extracorporeal membrane oxygenation for critically ill adults. Cochrane Database Syst Rev. 2015; 1: CD010381.
- De Jonghe B, Sharshar T, Lefaucheur J, Authier FJ, Durand-Zaleski I, Boussarsar M, et al. Paresis acquired in the intensive care unit: A prospective multicenter study. JAMA. 2002; 288: 2859-2867.
- Needham DM. Mobilizing patients in the intensive care unit: Improving neuromuscular weakness and physical function. JAMA. 2008; 300: 1685-1690.
- Desai SV, Law TJ, Needham DM. Long-term complications of critical care. Crit Care Med. 2011; 39: 371-379.
- Thomsen GE, Snow GL, Rodriguez L, Hopkins RO. Patients with respiratory failure increase ambulation after transfer to an intensive care unit where early activity is a priority. Crit Care Med. 2008; 36: 1119-1124.
- Bailey P, Thomsen GE, Spuhler VJ, Blair R, Jewkes J, Bezdjian L, et al. Early activity is feasible and safe in respiratory failure patients. Crit Care Med. 2007; 35: 139-145.
- Morris PE, Goad A, Thompson C, Taylor K, Harry B, Passmore L, et al. Early intensive care unit mobility therapy in the treatment of acute respiratory failure. Crit Care Med. 2008; 36: 2238-2243.
- Burtin C, Clerckx B, Robbeets C, Ferdinande P, Langer D, Troosters T, et al. Early exercise in critically ill patients enhances short-term functional recovery. Crit Care Med. 2009; 37: 2499-2505.
- Needham DM, Korupolu R, Zanni JM, Pradhan P, Colantuoni E, Palmer JB, et al. Early Physical Medicine and Rehabilitation for Patients with Acute Respiratory Failure: A Quality Improvement Project. Arch Phys Med Rehabil. 2010; 91: 536-542.
- Rehder KJ, Turner DA, Hartwig MG, Williford WL, Bonadonna D, Walczak RJ Jr, et al. Active rehabilitation during extracorporeal membrane oxygenation as a bridge to lung transplantation. Respir Care. 2013; 58: 1291-1298.
- Rahimi RA, Skrzat J, Reddy DR, Zanni JM, Fan E, Stephens RS, et al. Physical rehabilitation of patients in the intensive care unit requiring extracorporeal membrane oxygenation: a small case series. Phys Ther. 2013; 93: 248-255.
- Turner DA, Cheifetz IM, Rehder KJ, Williford WL, Bonadonna D, Banuelos SJ, et al. Active rehabilitation and physical therapy during extracorporeal membrane oxygenation while awaiting lung transplantation: a practical approach. Crit Care Med. 2011; 39: 2593-2598.