Case Report
Cutaneous Aspergillosis in a Child with Acute Lymphoblastic Leukaemia
V Naga Raja Adusumilli*, Suneel C Mundkur, Shrikiran A Hebbar and Shravan K
Department of Paediatrics, Manipal University, India
*Corresponding author: Suneel C Mundkur, Department of Paediatrics, Kasturba Medical College, Madhav Nagar, Near Tiger Circle, Manipal, Karnataka 576104, India
Published: 12 Jul, 2017
Cite this article as: Adusumilli VNR, Mundkur SC, Hebbar
SA, Shravan K. Cutaneous Aspergillosis
in a Child with Acute Lymphoblastic
Leukaemia. Ann Clin Case Rep. 2017;
2: 1398.
Abstract
Primary cutaneous aspergillosis is a rare cutaneous disease that usually affects the immunocompromised patients. The most common associated disorders in children are leukemias and lymphomas although it can also occur in the neonates and preterms due to their immunological immaturity. Here we report a case of a 8-year-old boy diagnosed with B cell acute lymphoblastic leukemia during chemotherapy, developed multiple vesicular erythematous cutaneous lesions in the venepuncture area of the left forearm, and histopathology was suggestive of Aspergillosis.
Introduction
Fungi of the genus Aspergillus are ubiquitous and grow mainly in the soil, water, and the decomposing vegetation. They are opportunistic pathogens usually found in the immunocompromised individuals & are the second most common fungal infections after Candida They rarely affect the immunocompetent persons. The most frequently involved fungi are Aspergillus fumigatus and Aspergillus flavus. Primary cutaneous aspergillosis is a rare cutaneous disease that usually affects the immunocompromised patients. We present a case of cutaneous aspergillosis without systemic involvement in aB cell ALL child who responded favourably to topical treatment.
Case Presentation
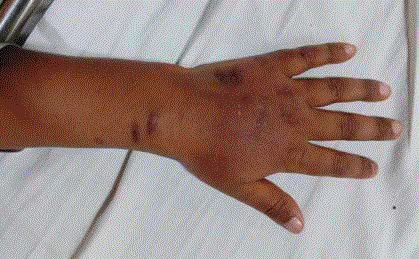
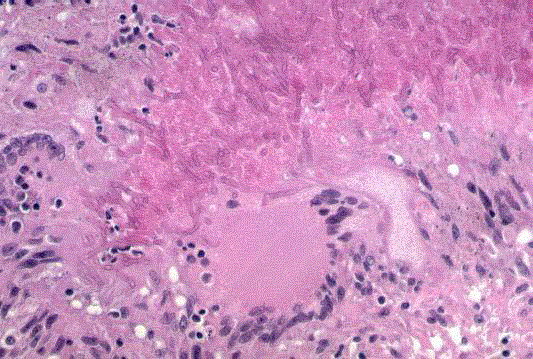
An 8 year old boy had multiple vesicular inflammatory cutaneous lesions at venepuncture area on the left hand and wrist (Figure1 and 2). The child was a diagnosed case of B cell acute lymphoblastic leukemia and was on treatment with BerlinFrankfurt-Münster 1995 protocol for acute lymphoblastic leukaemia. On day 45 the patient developed a lesion on the left forearm that consisted of a vesicular erythematous rash, near venepuncture area. There was no evidence of systemic infection, blood culture was sterile. CBC showed Leucopenia with Neutropenia. A cutaneous biopsy performed showed an inflammatory reaction and in which abundant septate fungal hyphae were observed branching at sharp angles suggestive of Aspergillosis. After a few days, the lesion had healed with scarring with topical antifungal medications.
Figure 1
Figure 2
Discussion
Cutaneous Aspergillosis may occur as primary or secondary infection. The former requires direct inoculation of the fungus into the skin, generally associated with a local injury. Secondary cutaneous Aspergillosis develops through the haematogenous dissemination to the skin from the distant focus. It is estimated that 4% to 11% of patients with systemic Aspergillosis develop secondary involvement of the skin. Contagious spread of Aspergillosis from paranasal/maxillary sinuses to skin or mucosa is also reported. In general, 0.27% of leukemia patients develop cutaneous Aspergillosis in some form. Primary cutaneous Aspergillosis (PCA) is a rare form of presentation. Aspergillus infection is associated with prolonged neutropenia, immunosuppressive & corticosteroid therapy, broadspectrum antibiotics, underlying malignancy, premature infants, AIDS, and patients with intravenous catheters. In children, primary cutaneous Aspergillosis (PCA) may be observed in three situations. 1. In Immunocompromised, skin lesions are most often caused by Aspergillus flavus and A. fumigatus at the site of catheterization or point of contact with dressing or gauge. 2. Aspergillus fumigatus & A. flavus are also most often implicated in new-borns& premature infants due to their defective skin barrier & immature immune system. 3. Aspergillus terrus & A. fumigatus cause lesion at catheter insertion/trauma site in immunocompetent children. In our case it was Primary cutaneous Aspergellosis with no evidence of systemic infection in a immunocompromised host who responded well to the topical medication [1-3].
References
- Walsh T J. Primary Cutaneous Aspergillosis-an emerging infection among immunocompromised patients. Clin Infect Dis. 2008; 27: 453-457.
- Nucci M, Marr KA. Emerging fungal diseases. Clin Infect Dis. 2005; 41: 521-526.
- Munn S, Keane F, Child F. Primary Cutaneous Aspergillosis. Br J Dermatol.1999; 141: 378-380.