Case Report
Axillary Apocrine Carcinoma with Bone Metastasis: First Report with Bone Scan Image
Sun Yu1, Gui Jicong1, Lu Yiping2, Xing-Dang Liu1*, Zhu Xiaoli3, Cheng Jingyi4 and Geng Daoying2
1Department of Nuclear Medicine, Fudan University, China
2Department of Radiology, Fudan University, China
3Department of Pathology, Fudan University Shanghai Cancer Center, China
4Department of Nuclear Medicine, Fudan University Cancer Hospital, China
*Corresponding author: Xing-Dang Liu, Department of Nuclear Medicine, Huashan Hospital, Fudan University, 12 Wulumuqi Zhong Rd, Shanghai 200040, PR China
Published: 06 Jul, 2017
Cite this article as: Yu S, Jicong G, Yiping L, Liu X-D, Xiaoli
Z, Jingyi C, et al. Axillary Apocrine
Carcinoma with Bone Metastasis: First
Report with Bone Scan Image. Ann Clin
Case Rep. 2017; 2: 1392.
Abstract
Apocrine carcinoma is a rare malignant neoplasm with differentiation towards apocrine glands. Rare cases of apocrine carcinoma are reported to have bone metastasis, and their bone scan images have never been showed in the literature. We report a case of a 59-year-old man with a painless tumor of the left axilla and first showed his image of 99mTc-MDP SPECT-CT bone scan. The patient underwent excision of the left axilla with left axillary lymphnode resection twice. Eight years later after his carcinoma was diagnosed, the patient noted intermittent pain in his back, and 99mTc-MDP SPECT-CT bone scan showed increased radioactivity in his bones. We discuss apocrine carcinoma with bone metastasis and review pertinent literature. We find osteogenic metastasis is a main style of the bone metastasis of apocrine carcinoma and should not be only limited in axial skeleton. The whole-body bone scan exam must be recommended for patients with apocrine carcinoma, even when they have lived more than 5 years after the surgery.
Keywords: Apocrine carcinoma; SPECT-CT; Bone scan
Introduction
Since the advent of the PET/CT, SPECT/CT seems increasingly outdated for patients with cancer. But it still has indications, such as for ill-defined bone pain, especially for tumor patients. 99mTc-MDP SPECT-CT bone scan was known sensitive for cancer patients with skeletal metastases, such as breast, lung, prostate and gastrointestinal cancer. In fact, SPECT-CT bone scan should be recommended for all kinds of cancer patients with skeletal metastases. Apocrine carcinoma is a rare cutaneous malignant neoplasm which histopathologically manifests itself as ductal carcinoma. The tumor occurs more frequently in the axilla, perineum, eyelids and external auditory canals, where apocrine glands are abundant. Rare cases of apocrine carcinoma are reported to have metastases. However, in this report of apocrine carcinoma, we show the skeletal metastases in axial bones with the 99mTc-MDP SPECT-CT bone scan.
Case Presentation
In this study, we report a 59-year-old Chinese man with a long history of apocrine carcinoma,
and 8 years after the diagnosis, 99mTc-MDP SPECT-CT bone scan showed increased radioactivity in
his axial bones.
This patient used to be an employee who worked in Japan. When being 51 years old, he had
found a movable mass without tenderness in his left axilla which had been 2-3cm in diameter. He
had attributed this to his busy working; however, the mass progressed gradually. He visited a local
hospital and experienced tumor excision in the year of 2006. After surgery, he didn’t get further
treatment until his return to China in 2011. He visited an oncologist in Shanghai and found swelling
lymph nodules in his left axilla by ultrasound. He was then admitted to have removal of axillary
lymph nodes. The histology documented surgery`s involvement of subclavicular lymph nodes and
pectoralis minor with infiltration of carcinoma cells. On gross pathologic review, the mass measured
3.5 cm × 2 cm and appeared granular and pale white to gray-tan in color. Microscopic evaluation
(hematoxylin-eosin) revealed low differentiated adenocarcinoma with inclination of apocrine
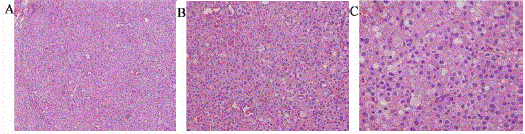
carcinoma showed in Figure 1A, B and C with different magnification. The patient then received an adjuvant local radiotherapy at 50 Gy in left mammary and clavicular
regions. In November 2014 he presented at our department with the
chief complaint of intermittent pain in his back which could persist
for 2-3 days before remission.
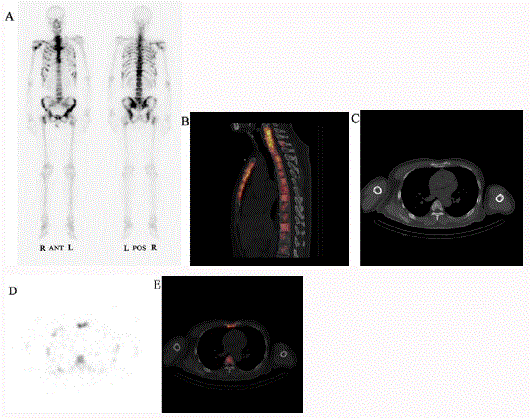
A SPECT-CT Whole-body bone scan was performed 4 hours
after injection of 25 mCi (925MBq) 99mTc-MDP. The whole-body
SPECT image revealed extensive metastatic disease both in his axial
skeletons included bilateral rips, sternum and vertebral, and the
appendicular skeletons included right clavicle, right scapula, right
humerus head, hip bones and bilateral femurs of the patient (Figure
2A). The SPECT-CT image in the sagittal plane and the axial plane
showed that high density shadow in the skeleton in the CT image was
found where the high radioactivity concentrate in the SPECT image
(Figure 2B, C, D and E).
Figure 1
Figure 1
Primary axillary apocrine carcinoma histology. Cells are relatively small with moderately pleomorphic, hyperchromatic nuclei and pale cytoplasm.
Intracytoplasmic vacuoles are present (*A, B, C are 100/200/400 magnification respectively).
Figure 2
Figure 2
Anterior and posterior whole-body bone scans with 99mTc methylene diphosphonate of the patient showed high concentration of drugs in both axial
skeletons and appendicular skeletons. And in the CT image high density shadow in the skeleton was found where the high radioactivity concentrate in the SPECT
image. A is the whole-body scan; B is in sagittal plane; C, D and E are CT, SPECT, SPECT/CT images in axial planes respectively.
Discussion
Apocrine carcinoma was first reported by Gates et al. in series with 5 cases being discovered [1]. In the following years, there are a
few reports worldwide to describe the disease in series [2,3]. To our
knowledge, there are few reports about the metastasis of apocrine
carcinoma. The total amount of metastatic cases worldwide is about
20 [3-7]. Apocrine carcinoma mainly spread through the lymphatic,
but hematogenous spread also occurred in 3 cases including liver and
brain [6,7]. In our case the patient was found recurrence 5 years after
onset and metastasis 3 years afterwards. His metastasis was found in
axial skeleton which was aligned with one case reported before, but
without more detailed imaging resources [8]. This is the first report
with SPECT and CT bone image.
Actually, apocrine carcinoma with bone metastasis is not reported
the first time [9,10]. But no author has described and analyzed the
bone scan image from the patients with apocrine carcinoma. In
this case, the multiple metastatic foci in the skeletons are almost
osteogenic metastasis, with the high concentration of radioactivity.
The same character was mentioned in two case reports in China
[8,11], without bone scan image, however. Therefore, we have reason
to guess osteogenic metastasis is a main style of the bone metastasis
of apocrine carcinoma. In addition, in our case, the bone metastasis
not only occurred in axial skeletons but also in the appendicular
skeletons. The distribution of the bone metastasis is the same as a case
report [11], but bone metastasis is also found in long bones in another
case [8]. Therefore, the bone metastasis of apocrine carcinoma should
not be only limited in axial skeleton.
Generally, patients with apocrine carcinomas are usually more
than 50 years of age, with a mean age of 57-61 years [3]. No clear
gender, racial or ethnic predilection is observed in the latest research
[3]. Clinically, typical lesions of apocrine carcinoma are slow-growing,
painless, palpable cystic or solid nodules with normal appearance [4].
Our case was just a movable mass without any skin lesions which
made it hard to have any clinical differential diagnosis. Because of its
rarity, apocrine carcinoma remains a diagnosis of exclusion. Biopsy is
still the gold-standard for diagnosis and several pathological features
can help in this process [12].
The treatment of apocrine carcinoma mainly includes surgery,
chemotherapy and radiotherapy. Initial surgical treatment is proved
to be important; if complete resection is possible, long-term survival
can be expected [4,13]. Patients with apocrine carcinoma show
different diagnosis which seems no relation with treatment method
or clinical course but correlate with degree of tumor differentiation.
Those patients with well-differentiated tumor cells did extremely well
and could achieve long-term remission with surgery alone. However,
patients with moderately or poorly differentiated tumor cells had
higher local recurrence rates after resection and were far more likely
to have metastasis, just like our case [4,13]. After 8 years later he was
firstly diagnosed with apocrine carcinoma, he performed bone scan
because of intermittent pain in his back and found bone metastasis.
But actually he had already had bone metastasis for some time and
there are no bone symptoms. For some patients who had lived more
than 5 years, they may have bone metastasis. The whole-body bone
scan exams could find bone metastasis earlier and provide guidance
for further treatment, and maybe extend the patients’ survival time.
Therefore, the whole-body bone scan exam must be recommended
for patients with apocrine carcinoma, especially with moderately or
poorly differentiated apocrine carcinoma, just like what we do for
patients with other cancers.
References
- Gates O, Warren S, Warvi WN. Tumors of sweat glands. Am J Pathology. 1943; 19: 591-631.
- Urso C, Bondi R, Paglierani M, Salvadori A, Anichini C, Giannini A. Carcinomas of Sweat Glands: Report of 60 cases. Arch Pathol Lab Med. 2001; 125: 498-505.
- Robson A, Lazar AJ, Ben Nagi J, Hanby A, Grayson W, Feinmesser M, et al. Primary cutaneous apocrine carcinoma: a clinico-pathologic analysis of 24 cases. Am J Surg Pathol. 2008; 32: 682-690.
- Chamberlain RS, Huber K, White JC, Travaglino-Parda R. Apocrine Gland Carcinoma of the Axilla Review of the Literature and Recommendations for Treatment. Am J Clin Oncol. 1999; 22: 131-135.
- Ivan D, Nash JW, Prieto VG, Calonje E, Lyle S, Diwan AH, et al. Use of p63 expression in distinguishing primary and metastatic cutaneous adnexal neoplasms from metastatic adenocarcinoma to skin. J Cutan Pathol. 2007; 34: 474-480.
- Gallerani E, Ciriolo M, Rossini C, Cavalli F. Axillary apocrine carcinoma with brain metastases. J Clin Oncol. 2007; 25: 5655-5656.
- Bagwan IN, Taylor A, Dina R. Metastatic apocrine carcinoma of female genital tract. J Clin Pathol. 2009; 62: 287-288.
- Liu Y, Zhang WC. A case report: Axillary Apocrine Carcinoma with Bone Metastasis. Chin J Oncol. 2015; 37: 640-641.
- Ishida M, Hotta M, Kushima R, Okabe H. A case of porocarcinoma arising in pigmented hidroacanthoma simplex with multiple lymph node, liver and bone metastases. J Cutan Pathol. 2011; 38: 227-231.
- Kiyohara T, Kumakiri MKawami KKouraba STakeuchi ASawai T, et al. Apocrine carcinoma of the vulva in a band-like arrangement with inflammatory and telangiectatic metastasis via local lymphatic channels. Int J Derm. 2003; 42: 71-74.
- Liu PJ. A case report: Axillary Apocrine Carcinoma with Bone Metastasis. Chinese J Cancer Prevention and Treatment. 2006; 2: 152.
- L Requena, H Kutzner, MA Hurt. Malignant tumors with apocrine and eccrine differentiation, in World Health Organization classification of tumors. Pathology and genetics of skin tumors, IARC Press: Lyon. 2006; 135-138.
- Ogata D, Kiyohara Y, Yoshikawa S, Kasami M. Treatment strategy for cutaneous apocrine carcinoma. Int J Clin Oncol. 2014; 19: 712-715.