Case Report
Anti-CTLA-4 Monoclonal Antibodies Induced Hypophysitis: Case Report and Literature Review
Jaafar Jaafar* and Jacques Philippe
Division of Endocrinology and Diabetology, Geneva University Hospitals and Faculty of Medicine, Switzerland
*Corresponding author: Jaafar Jaafar, Division of Endocrinology and Diabetology, Geneva University Hospitals and Faculty of Medicine, Gabrielle-Perret-Gentil 4, Geneva, 1211, Switzerland
Published: 20 Jun, 2017
Cite this article as: Jaafar J, Philippe J. Anti-CTLA-4
Monoclonal Antibodies Induced
Hypophysitis: Case Report and
Literature Review. Ann Clin Case Rep.
2017; 2: 1382.
Abstract
Treatment with Anti-CTLA-4 Monoclonal Antibodies (mAb) has become a common choice in advanced melanoma and is under evaluation for many other types of cancer. These antibodies inhibit the interaction between CTLA-4 (Cytotoxic T Lymphocyte-Associated Antigen 4) receptors on the T cell surface and the antigen presenting cell surface molecules B7, leading to the activation or enhancement of T cell immune responses. The oncologic beneficial effects of Anti-CTLA-4 mAb are marred by many immune related adverse effects, including Ipilimumab-Induced Hypophysitis (IIH). We, herein, report an illustrative case with a literature review. Based on this research, the incidence of IIH was between 1.75% and 13%. Presenting symptoms were predominantly headache and fatigue. Pituitary enlargement was the main radiologic sign on MRI. The thyrotrophic and adrenocorticotropic axes were the most commonly affected followed by gonadotropic, somatotropic and lactotropic axes, respectively. Time to hypophysitis onset varied between 5 and 40 weeks after starting ipilimumab and treatment withdrawal due to hypophysitis was largely variable. Finally, thyrotropin and gonadotropin axes recovered more frequently than other anterior pituitary axes.
Introduction
The emergence of new antitumor drugs called Immune Check-Points Inhibitors (ICIs) in the management of melanoma, Non-Small Cell Lung Cancers (NSCLC) and other cancers led to the development of new forms of adverse effects called Immune Related Adverse Effects (irAEs), as compared to conventional chemotherapy. These new multisystem adverse effects include dermatologic, gastrointestinal, pulmonary, and endocrine effects. Endocrinologists are increasingly facing the diagnosis and management of the endocrine irAEs on the thyroid, pituitary, adrenal glands and pancreas, which was, up until recently, not indexed in endocrine diseases. The nowadays admitted and used ICI are essentially anti-cytotoxic T lymphocyte antigen 4 (CTLA-4) antibodies, anti-programmed cell death-1 (PD-1) antibodies and anti-Programmed death-ligand 1 (PD-L- 1) with other check-point inhibitors currently under investigation. Ipilimumab (Ipi-) is un anti- CTLA-4 antibody which showed a beneficial effect in advanced melanoma, but these beneficial effects are tainted by several undesirable effects including hypophysitis. Here we report a case of ipilimumab induced hypophysitis with a literature review of the incidence, diagnosis, treatment and follow-up of this condition.
Case Presentation
A 62-year-old Caucasian male patient diagnosed 6 years ago with non-metastatic right thigh melanoma was treated by tumour excision with inguinal lymph node dissection. His past medical history includes an ischemic stroke due to dissection of the left vertebral artery. Two years ago, he presented a metastatic relapse with a subcutaneous nodule on the anteromedial face of the right thigh with hepatic metastasis rapidly progressive within 2 months, bone metastasis and left adrenal metastasis, without adrenal insufficiency. The patient was started on intravenous (i.v) ipilimumab (Ipi-) 3mg/kg every 21 days. The patient underwent a pre-treatment thyroid assessment which was normal and subsequently serial TSH measurements before every Ipi- injection. Twenty days after the forth injection of Ipi- he presented a mild headache and fatigue. Biological tests showed central hypothyroidism with TSH at 0.1mU/l and free T4 at 11.7 pmol/l (N: 12-22pmol/l), low testosterone 1.27μg/l (N: 2.73-8.16μg/l) with low LH, a surprisingly high level of IGF-1 at 244 μg/l and a normal cosyntropin stimulation test. However, two months later, the cortisol level was reduced to 2μmol/l (Figure 1). A 18F-FDG PET scan showed a high pituitary uptake compared with a previous PET scan (Figure 2), and a Gadolinium-injected pituitary MRI done 10 days later showed hypertrophic and heterogenic pituitary with diminished spontaneous posterior pituitary intensity (Figure 3). The patient was started on levothyroxine and high-dose prednisone with subsequent progressively decreasing doses, as well as replacement treatment with testosterone. The clinical course was rapidly favourable whereas biologically, he recovered the thyrotrophic axis within 52 weeks but till today, the patient needs corticosteroid and testosterone replacement therapy. Ipi- was stopped at the diagnosis of hypophysitis but the patient had already received 4 doses. A new treatment with pembrolizumab 2mg/kg i.v every 21 days was started 5 weeks after the last dose of Ipi- (2 weeks after the hypophysitis diagnosis) because of disease progression in the liver, internal and external right iliac lymph nodes along with a global increase in almost all known bone and left adrenal metastases.
Figure 1
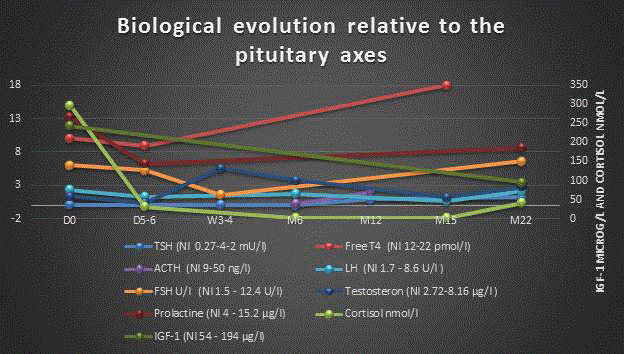
Figure 1
This chart shows the course of different pituitary axes from the
moment of hypophysitis diagnosis to the last available laboratory results.
Levothyroxine and steroids were started on day 0, while testosterone was
started on D7. Levothyroxine was discontinued after 52 weeks of treatment.
D: day; W: week; M: month; Nl: normal range.
Figure 2
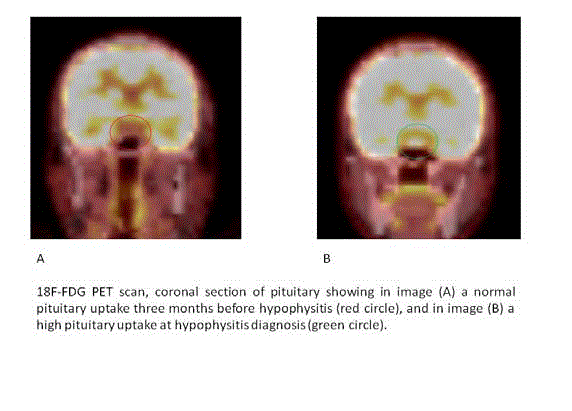
Figure 2
Coronal view of the pituitary by reconstruction after fusion of PET
scan with 18F-FDG and CT scan. Image (A) shows no pituitary uptake before
hypophysitis, and image (B) shows a high pituitary uptake at the diagnosis
of hypophysitis.
Figure 3
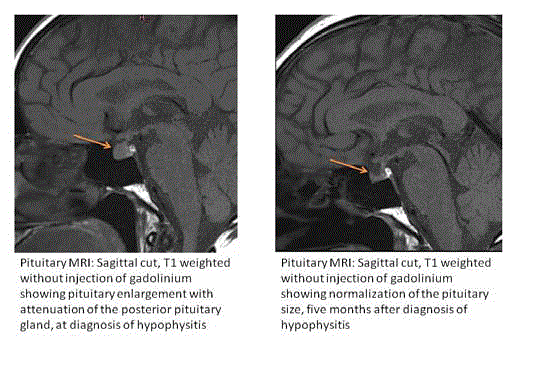
Figure 3
Pituitary MRI, Sagittal cut, T1 weighted without injection of
gadolinium showing pituitary enlargement with attenuation of the posterior
pituitary gland, at diagnosis of hypophysitis (left image) and normalization
of the pituitary gland size five months after diagnosis of hypophysitis (right
image).
Discussion
CTLA-4 immune check-point inhibition
The role of CTLA-4 was clearly evoked by Linsley et al. [1] in 1991
and 1992, who showed a suppression of T cell-dependent antibody
responses to sheep erythrocytes or keyhole limpet hemocyanin, by
CTLA4 Immunoglobulin (Ig) treatment in vivo. Simultaneously,
Lenschow described a long-term survival of xenogenetic pancreas islet
grafts using CTLA-4Ig, thus emphasizing the immunosuppressive
role of this cell surface protein [2]. Chambers described in 2001 the
CTLA-4-mediated inhibition in regulation of T cell responses [3].
Lymphocyte T cell activation require recognition and binding of T Cell Receptor (TCR) to antigen-bound Major Histocompatibility
Complex (MHC) present on the Antigen-Presenting Cell (APC) with
simultaneous co-stimulatory interaction between CD28 on the T
cell and members of the B7 family on the APC [4]. This is followed
by activation of pro-survival signals as well as the production of
cytokines production and stimulation of cell expansion. CTLA-4, is
a homologue of CD28 and functions as an inhibitory receptor for
B7 co stimulatory molecules expressed on APCs with 20-fold higher
affinity binding to B7 molecules than to CD28 [1]. T cell activation
up regulates CTLA-4 which will compete with CD28 for binding to
B7, thereby transmitting a suppressive signal for T cell activation
[1,5]. In 1994, Walunas et al. [6] showed that the blockade of CTLA-
4 interaction with B7 enhances T cell activation in vitro, whereas
antibodies that engage CTLA-4 signalling attenuate T cell activation.
In 1995, Krummel et al. [7] showed that cross-linking of CTLA-4
together with the TCR and CD28 strongly inhibits proliferation and
IL-2 secretion by T cells, and that CD28 and CTLA-4 deliver opposing
signals that appear to be used by the T cell to determine the response
to activation. Given the inhibitory effect of CTLA-4 in the T cell
response, it was proposed that blockade of CTLA-4 might overcome
the CTLA-4-mediated suppression and enhance pre-existing or
induced immune responses to cancer. This finding was clinically
proven in two phase III studies [8-10]. This allowed Ipilimumab
(Ipi-), which is a fully human IgG1 Monoclonal Antibody (mAb),
to be approved by the Food and Drug Administration (FDA) and
by the European Medicine Agency (EMA) in 2011 as the first anti-
CTLA-4 mAb for the treatment of advanced malignant melanoma.
Ipilimumab is currently being assessed by several trials in lung,
renal, prostate, pancreas, liver and ovarian cancer, in addition to
lymphoma, leukaemia, and other haematological disorders and solid
tumours [11].
Despite its clinical benefits, treatment with anti-CTLA-4
mAb is associated with multiple organs irAEs, which are different
from conventional chemotherapy. These adverse effects include
dermatological toxicities, colitis, diarrhoea, hepatotoxicity, as well
as endocrine, ocular, renal and neurologic immune Adverse Events
(AEs) [12]. Endocrine AEs (eAEs) were essentially hypophysitis or
hypopituitarism, thyroiditis with hyper and hypothyroidism and
adrenalitis. In general, eAEs occur in the first 6 months of treatment,
especially during the induction period. In a phase III follow-up study of ipilimumab (with or without gp100) pre-treated patients with stage
IV melanoma who progressed under treatment, retreatment with
anti-CTLA-4 mAb (ipilimumab) did not confer new types of toxicity
and most events were mild to moderate [13]. Table 1 shows the result
of a data research that we did in October 2016 of phase I, II, III and
IV human trials, available in full English text, with CTLA-4 blockade.
We found 139 studies. All abstracts were reviewed and studies with
≤20 patients were excluded. IIH incidence was between 2.76% [14]
and 17% [15]. This incidence was greater when Ipilimumab was
associated with anti-PD-1 antibodies compared with ipilimumab
alone [16,17].
CTLA-4-mAb induced hypophysitis
Hypophysitis is an inflammation of the pituitary gland
characterized pathologically by mainly lymphocytic infiltration and
destruction of endocrine cells. It could be primary (idiopathic) or
secondary with clearly a traceable triggering cause. Since the arrival
of anti-CTLA-4 mAb, hypophysitis had emerged as one of the
numerous irAEs. One of the first cases was described in 2003 by Phan
in a patient with advanced melanoma treated with ipilimumab [18].
Blansfield then reported 8 cases of hypophysitis out of 163 patients
with advanced melanoma or renal cell cancer treated by anti-CTLA-4
mAb with an incidence of hypophysitis of 4.9% [19].
The incidence of Ipilimumab Induced Hypophysitis (IIH) was
reported by recent studies to be between 0.5% and 17.2% when used
alone in advanced melanoma, with a higher incidence when using
high compared to low doses [14,20-22]. Time to onset varies between
3.6 and 40 weeks [20,22-24], and when hypophysitis occurs, Ipidiscontinuation
is 24-35% [25]. Ipi-discontinuation did not appear
to affect the outcome of hypophysitis [26]. The main symptoms were
fatigue and headache [25]. In a phase II study comparing ipilimumab
to placebo in add-on therapy to Paclitaxel and carboplatin in 204
patients with stage III/IV NSCLC, the incidence of hypophysitis and
hypopituitarism in the active arm was 2.76 % [14]. The association of ipilimumab with other ICIs like anti PD-1 was associated with 2%-12% of all hypophysitis grades in advanced stage melanoma patients
[25]. The relation between dose and immune toxicity of Anti–
CTLA-4-mAb in patients with metastatic melanoma was clearly
demonstrated, with increasing grade III/IV irAEs incidence (35%)
after a dose escalating of ipilimumab form 3 or 5 mg/kg to 9 mg/kg
every 3 weeks [21] compared with an incidence of 25% in patients
who received 3 mg/kg of antibody plus a peptide vaccine [27].
In a retrospective study of 154 adult patients with metastatic
melanoma treated by ipilimumab, male gender and older age were
risk factors for IIH, and pituitary enlargement on MRI was a sensitive
and a specific sign for IIH, which can precede the clinical diagnosis
and resolves rapidly under high steroid dose treatment. In this
study, anterior pituitary function recovery was uncommon and the
incidence of hypophysitis was positively correlated with improved
survival (median survival 19.4 months with and 8.8 months without
IIH) [20]. Male gender and older age were found by another team as
predictors of hypophysitis in this setting [22]. Nevertheless they were
not retained as predisposing factors for IIH in a recent retrospective
study [23]. Hypophysitis with panhypopituitarism was described also
for the first time in 2009 in two patients with prostate cancer treated
with ipilimumab. In one patient, the onset of hypopituitarism was 4
weeks after initiation of Ipilimumab (10 mg weekly) with recovery
of the Hypothalamic-Pituitary-Thyroid (HPT) axis after 9 months.
The other patients presented hypopituitarism with Diabetes Insipidus
(DI), with recovery after 3 days of high dose corticosteroids [11]. It
is noteworthy that DI did not occur in large retrospective studies of
IIH in patients with melanoma [19,20,24]. Hypophysitis induced by
anti-CTLA-4-mAb could affect one, two or more pituitary axes, with
typically gonadotrophic and thyrotrophic axes involvement first [28].
Table 2 summarizes several longitudinal studies (mainly
retrospective in nature), that investigate the incidence, the clinical,
biological and radiological presentation, and follow up of IIH.
According to these studies the incidence of IIH was between 1.75%
and 13%. Presenting symptoms were essentially headache, fatigue,
personality changes and nausea. When pituitary MRI was done,
pituitary enlargement was the main radiologic sign but was not
consistently present. No case of DI was reported in all these studies
(englobing 1636 patients).The thyrotrophic and adrenocorticotropic
axes were the most commonly affected (probably because they were
systemically assessed), followed by gonadotropic, somatotropic
and lactotropic axes, respectively. Treatment withdrawal because
of hypophysitis was largely variable from 0 to 100% [19,27]. Time
to hypophysitis onset after starting Ipi- also varied between 5 and
40 weeks. Thyrotropin and gonadotropin axes recovered more
frequently, as compared to other anterior pituitary axes, with also a
low rate of adrenocorticotropic recovery (Table 2).
Mechanism of anti-CTLA-4 mAb induced hypophysitis
To respond to the question why do anti-CTLA-4 mAb,
especially ipi-, provokehypophysitis, Iwama et al. [29] developed
a murine hypophysitis model by repeated injections of a CTLA-
4 blocking antibody, leading to pituitary lymphocytic infiltration
with development of circulating anti-pituitary antibodies. They
then followed 20 patients with advanced melanoma or prostate
cancer treated with ipi- and found that the 7 patients who developed hypophysitis had all novel anti-pituitary antibodies whereas the
13 patients who did not develop hypophysitis did not have these
antibodies. These antibodies mainly recognized thyrotropin-, folliclestimulating
hormone–, and corticotropin-secreting cells. CTLA-
4 was expressed at both RNA and protein levels in the pituitary
gland, particularly in prolactin- and thyrotropin-secreting cells. It
is then hypothesized that the injected anti-CTLA-4 antibody could
cause pituitary toxicity if bound to CTLA-4 antigen expressed
“ectopically” on pituitary endocrine cells. These cells became the
site of complement activation, with deposition of C3d and C4d
components leading to an inflammatory cascade similar to that seen
in type II hypersensitivity. Conversely, in a recent retrospective study,
pituitary antibodies were not found in all 9 patients who developed
hypophysitis out of 273 patients with metastatic melanoma who
were treated with Ipilimumab [23]. Nevertheless, it remains unclear
why some patients but not others develop these antibodies. In one
autopsy study of 6 patients treated with ipilimumab for melanoma
the expression of CTLA-4 was present in all patients’ pituitary glands
but at different levels, with the highest expression level in the patient
who had severe hypophysitis. This study included one patient who
had clinical and biological hypophysitis and a second with pituitary
lymphocytic infiltration without clinical hypophysitis, and four other
patients with normal pituitary function and structure. This elevated
CTLA-4 expression was associated with high T-cell infiltration
and IgG dependent complement fixation and phagocytosis. These
findings suggest that a high level of CTLA-4 expression predisposes
to hypophysitis through type IV (T-cell dependent) and type II
(IgG dependent) immune mechanisms. This may possibly explain
why only some patients develop hypophysitis when treated by anti-
CTLA-4 mAb.
Diagnosis of anti-CTLA-4 mAb induced hypophysitis
Treating patients with ICIs require a good knowledge about their
irAEs, and a low threshold of suspicion to evocate these AEs. In patients
who are treated with anti-CTLA-4-mAb, especially ipilimumab,
hypophysitis should be suspected in case of new onset headache,
fatigue, hypotension, nausea, confusion and other symptoms and
signs which are summarized in Table 3 [18-20,23,24,27,30]. Diabetes
insipidus is very rare and was described in one patient with prostate
cancer treated by Ipi [11]. Clinically, it might be associated with
supine or orthostatic hypotension. Hyponatremia is present in some
patients but not all.
When possible, before starting treatment, a morning evaluation
of pituitary function should be performed, including corticotropic,
thyrotrophic, and gonadotropic axes, by measuring Thyroid Stimulating Hormone (TSH), Free Thyroxine (fT4) and Free Tri-
Iodothyronine (fT3), Adrenocorticotropic Hormone (ACTH)
and cortisol, testosterone (in male patients) or estradiol (in female
patients) with Luteinizing Hormone (LH) and Follicular Stimulating
Hormone (FSH). A normal Cosyntropin Stimulation Test (CST)
does not exclude an abnormal corticotroph axis due to a still normal
adrenal response in a recently damaged pituitary gland. If doubt
persists, a Corticotropin-Releasing Hormone (CRH) stimulation
test could be done. On the other hand, a normal or high ACTH
with a low cortisol or abnormal response to CST indicates primary
adrenal damage, which is another possible complication of anti-
CTLA-4-mAb. Similarly, a pituitary cause of hypothyroidism will
be associated with both low or normal low TSH and low peripheral
thyroid hormones (fT4 and fT3), while primary hypothyroidism will
show a high TSH with low fT3 and fT4. Pituitary antibodies are not a
part of the diagnostic workup.
MRI is not crucial for hypophysitis diagnosis and is sometimes
normal even when there is clinical and biological evidence of
hypophysitis, but when abnormal it confirms this diagnosis and
allows exclusion of alternative diagnoses, mainly brain metastasis.
Gadolinium injected cerebral MRI focusing on the pituitary gland
is the test of choice and in case of hypophysitis it shows a pituitary
gland and stalk enlargement and/or heterogeneity with loss of normal
posterior pituitary signal intensity on the pre contrast images [31]
(Figure 3). Follow up pituitary MRI may show evolution to empty
sella [23].
Management of anti-CTLA-4 mAb induced hypophysitis
High-dose corticosteroids to treat hypophysitis was suggested
by some studies [11,20,25] but others did not find a clear benefit
on the outcome of frequency and time to resolution. Hormone
replacement should be introduced in the case of deficiencies
[22,23,26]. One study proposes to use high-dose corticosteroids only
in severe and persistent mass-effect symptoms [23].When high-dose
corticosteroids are prescribed for treatment of acute hypophysitis,
the suggested treatment is intravenous prednisone dose (1mg/kg)
followed by the same oral daily dose with a gradual tapering over 4
weeks [28,32]. Thereafter, corticotropic substitution can be achieved
using hydrocortisone 10 to 20 mg in the morning and 5 to10 mg
in the beginning of the afternoon or by a single dose of prednisone
5 mg to 7.5 mg in the morning with a thyroid substitution dose of
levothyroxine 1.2 to 1.8 mg/kg. There are no recommendations for
sex hormone replacement in immune induced hypophysitis. A caseby-
case assessment should therefore be done. In our practice, when
a patient is hemodynamically stable without symptoms suggestive of
local compression, we use replacement doses for deficient hormones,
starting by corticosteroids then levothyroxine and eventually
testosterone replacement. GH analogues are contraindicated in
oncological circumstances.
Follow-up and reversibility of anti-CTLA-4 mAb induced
hypophysitis
Endocrinological long term follow-up after hypophysitis due to
anti-CTLA-4 mAb is not standardised and is often dictated by the
oncologic course. This generates a clinical practice disparity which
is appreciated when we observe the heterogenic results of both
prospective and retrospective studies reported here. Generally, the
pituitary size normalises on follow-up, but pituitary axes recover
variably. Based on long term retrospective studies, the corticoadrenal
axis recovery rate varies between 0 and 18.7% [26,33]. However, these
values are probably underestimated due to the negative feedback of
exogenous corticosteroids which are usually maintained over long
periods of time without systematically evaluating the possibility of
weaning. The pituitary-thyroid axis recovers between 0 and 100%
[23,33] and the gonadotropic axis recovers between 0 and 83.3%
[24,27]. Finally, time to recovery varies from days to over two years.
Table 1
Table 2
Table 3
Conclusion
Ipilimumab-induced hypophysitis has become a frequent immune check-point inhibitors complication, especially when Ipi- is used with other ICIs. Its recognition is based on acknowledgement and familiarity with adverse effects of this treatment and on having a low suspicion threshold. The main clinical presentation is headaches associated with fatigue. The workup includes anterior pituitary axes assessment along with pituitary imaging, preferably MRI. The use of high steroid doses as a treatment of acute phase of hypophysitis remains controversial. Deficient pituitary axes should be replaced and periodic evaluation of eventual pituitary hormone recovery should be done. Some studies suggested that the occurrence of hypophysitis might predict a better response to Ipi-. Finally, the mechanisms of the adverse effects must be better understood to look for preventive measures.
References
- Linsley PS, Brady W, Urnes M, Grosmaire LS, Damle NK, Ledbetter JA. CTLA-4 is a second receptor for the B cell activation antigen B7. J Exp Med. 1991; 174: 561-569.
- Lenschow DJ, Zeng Y, Thistlethwaite JR, Montag A, Brady W, Gibson MG, et al. Long-term survival of xenogeneic pancreatic islet grafts induced by CTLA4lg. Science. 1992; 257: 789–792.
- Chambers CA, Kuhns MS, Egen JG, Allison JP. CTLA-4-mediated inhibition in regulation of T cell responses: mechanisms and manipulation in tumor immunotherapy. Annu Rev Immunol. 2001; 19: 565-594.
- Fife BT, Bluestone JA. Control of peripheral T-cell tolerance and autoimmunity via the CTLA-4 and PD-1 pathways. Immunol Rev. 2008; 224: 166-182.
- Linsley PS, Greene JL, Brady W, Bajorath J, Ledbetter JA, Peach R. Human B7-1 (CD80) and B7-2 (CD86) bind with similar avidities but distinct kinetics to CD28 and CTLA-4 receptors. Immunity. 1994; 1: 793–801.
- Walunas TL, Lenschow DJ, Bakker CY, Linsley PS, Freeman GJ, Green JM, et al. Pillars article: CTLA-4 can function as a negative regulator of T cell activation. Immunity. 1994. 1: 405-413. J Immunol. 2011; 187: 3466–3474.
- Krummel MF, Allison JP. CD28 and CTLA-4 have opposing effects on the response of T cells to stimulation. J Exp Med. 1995; 182: 459–465.
- Hodi FS, O'Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010; 363: 711-723.
- Robert C, Thomas L, Bondarenko I, O’Day S, Weber J, Garbe C, et al. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med. 2011;364(26):2517–26.
- Peggs KS, Quezada SA. Ipilimumab: attenuation of an inhibitory immune checkpoint improves survival in metastatic melanoma. Expert Rev Anticancer Ther. 2010; 10: 1697–1701.
- Dillard T, Yedinak CG, Alumkal J, Fleseriu M. Anti-CTLA-4 antibody therapy associated autoimmune hypophysitis: serious immune related adverse events across a spectrum of cancer subtypes. Pituitary. 2010; 13: 29–38.
- Quirk SK, Shure AK, Agrawal DK. Immune-mediated adverse events of anticytotoxic T lymphocyte-associated antigen 4 antibody therapy in metastatic melanoma. Transl Res. 2015; 166: 412–424.
- Robert C, Schadendorf D, Messina M, Hodi FS, O’Day S. Efficacy and safety of retreatment with ipilimumab in patients with pretreated advanced melanoma who progressed after initially achieving disease control. Clin Cancer Res. 2013; 19: 2232–2239.
- Lynch TJ, Bondarenko I, Luft A, Serwatowski P, Barlesi F, Chacko R, et al. Ipilimumab in combination with paclitaxel and carboplatin as first-line treatment in stage IIIB/IV non-small-cell lung cancer: results from a randomized, double-blind, multicenter phase II study. J Clin Oncol. 2012; 30: 2046–2054.
- Maker AV, Phan GQ, Attia P, Yang JC, Sherry RM, Topalian SL, et al. Tumor regression and autoimmunity in patients treated with cytotoxic T lymphocyte-associated antigen 4 blockade and interleukin 2: a phase I/II study. Ann Surg Oncol. 2005; 12: 1005–1016.
- Postow MA, Chesney J, Pavlick AC, Robert C, Grossmann K, McDermott D, et al. Nivolumab and ipilimumab versus ipilimumab in untreated melanoma. N Engl J Med. 2015; 372: 2006-2017.
- Larkin J, Chiarion-Sileni V, Gonzalez R, Grob JJ, Cowey CL, Lao CD, et al. Combined Nivolumab and Ipilimumab or Monotherapy in Untreated Melanoma. N Engl J Med. 2015; 373: 23-34.
- Phan GQ, Yang JC, Sherry RM, Hwu P, Topalian SL, Schwartzentruber DJ, et al. Cancer regression and autoimmunity induced by cytotoxic T lymphocyte-associated antigen 4 blockade in patients with metastatic melanoma. Proc Natl Acad Sci U S A. 2003; 100: 8372–8277.
- Blansfield JA, Beck KE, Tran K, Yang JC, Hughes MS, Kammula US, et al. Cytotoxic T-lymphocyte-associated antigen-4 blockage can induce autoimmune hypophysitis in patients with metastatic melanoma and renal cancer. J Immunother. 2005; 28: 593–598.
- Faje AT, Sullivan R, Lawrence D, Tritos NA, Fadden R, Klibanski A, et al. Ipilimumab-induced hypophysitis: a detailed longitudinal analysis in a large cohort of patients with metastatic melanoma. J Clin Endocrinol Metab. 2014; 99: 4078–4085.
- Maker AV, Yang JC, Sherry RM, Topalian SL, Kammula US, Royal RE, et al. Intrapatient dose escalation of anti-CTLA-4 antibody in patients with metastatic melanoma. J Immunother. 2006; 29: 455-463.
- Lam T, Chan MM, Sweeting AN. Ipilimumab-induced hypophysitis in melanoma patients: an Australian case series. Intern Med J. 2015; 45:1066-1073.
- Brilli L, Danielli R, Ciuoli C, Calabrò L, Di Giacomo AM, Cerase A, et al. Prevalence of hypophysitis in a cohort of patients with metastatic melanoma and prostate cancer treated with ipilimumab. Endocrine. 2017.
- Albarel F, Gaudy C, Castinetti F, Carré T, Morange I, Conte-Devolx B, et al. Long-term follow-up of ipilimumab-induced hypophysitis, a common adverse event of the anti-CTLA-4 antibody in melanoma. Eur J Endocrinol. 2015; 172: 195-204.
- Torino F, Corsello SM, Salvatori R. Endocrinological side-effects of immune checkpoint inhibitors. Curr Opin Oncol. 2016; 28: 278-287.
- Min L, Hodi FS, Giobbie-Hurder A, Ott PA, Luke JJ, Donahue H, et al. Systemic high-dose corticosteroid treatment does not improve the outcome of ipilimumab-related hypophysitis: a retrospective cohort study. Clin Cancer Res. 2015; 21: 749-755.
- Attia P, Phan GQ, Maker AV, Robinson MR, Quezado MM, Yang JC, et al. Autoimmunity Correlates With Tumor Regression in Patients With Metastatic Melanoma Treated With Anti–Cytotoxic T-Lymphocyte Antigen-4. J Clin Oncol. 2005; 23: 6043–6053.
- Weber JS, Kähler KC, Hauschild A. Management of immune-related adverse events and kinetics of response with ipilimumab. J Clin Oncol. 2012; 30: 2691-2697.
- Iwama S, De Remigis A, Callahan MK, Slovin SF, Wolchok JD, Caturegli P. Pituitary expression of CTLA-4 mediates hypophysitis secondary to administration of CTLA-4 blocking antibody. Sci Transl Med. 2014; 6.
- Downey SG, Klapper JA, Smith FO, Yang JC, Sherry RM, Royal RE, et al. Prognostic factors related to clinical response in patients with metastatic melanoma treated by CTL-associated antigen-4 blockade. Clin Cancer Res. 2007; 13: 6681–6688.
- Carpenter KJ, Murtagh RD, Lilienfeld H, Weber J, Murtagh FR. Ipilimumab-induced hypophysitis: MR imaging findings. AJNR Am J Neuroradiol. 2009; 30: 1751-1753.
- Postow MA. Managing immune checkpoint-blocking antibody side effects. Am Soc Clin Oncol Educ Book. 2015.
- Ryder M, Callahan M, Postow MA, Wolchok J, Fagin JA. Endocrine-related adverse events following ipilimumab in patients with advanced melanoma: a comprehensive retrospective review from a single institution. Endocr Relat Cancer. 2014; 21: 371-381.