Case Report
Collet Sicard Syndrome
L Mayer1, M Spiegel2, C Boehme1, T Toell1, A Grams3, S Kiechl1, J Willeit1 and M Knoflach1*
1Department of Neurology, Medical University Innsbruck, Austria
2Department of Neurology, Sanatorium Kettenbruecke, Austria
3Department of Neuroradiology, Medical University Innsbruck, Austria
*Corresponding author: Michael Knoflach, Department of Neurology, Medical University Innsbruck, Anichstr, 35, A-6020 Innsbruck, Austria
Published: 17 Jun, 2017
Cite this article as: L Mayer, M Spiegel, C Boehme, T Toell,
A Grams, S Kiechl, et al. Collet Sicard
Syndrome. Ann Clin Case Rep. 2017;
2: 1379.
Abstract
We report two patients with Collet Sicard Syndrome due to internal carotid artery dissection. Manifestation of cranial nerve palsies IX to XII was preceded by neck pain and minor trauma in one patient. Compression of the cranial nerves by the expanding vessel diameter close to the base of the skull was documented by MRI. Both patients did not suffer stroke and the local symptoms recovered completely within several months.
Case Presentation
Case 1
A 60-year-old man presented with a 3-week history of right-sided neck pain, ipsilateral headache,
problems with swallowing and tongue movements, dysarthria and hoarseness. The medical history
was uneventful otherwise without episodes of cerebral or retinal ischaemia, neoplastic illness,
recent infection or trauma. In the local hospital right-sided paresis of the hypoglossal and recurrent
laryngeal nerves was diagnosed. Ultrasound of the extracranial carotid and vertebral arteries was
normal except for small atherosclerotic plaques at the carotid bifurcations and the cerebral MRI
was unremarkable. CT of the neck, however, showed a suspicious contrast-enhancing lesion in the
right tonsillar region extending towards the hypoglossal and vagus nerves. To rule out malignancy,
cautious surgical exploration and tonsillectomy were performed. Histological work-up was
consistent with tonsillitis. The patient was treated with antibiotics and discharged home.
Two weeks later the patient deteriorated. Swallowing and elevation of the right arm was
not possible and therefore the subject was admitted to the university hospital of Innsbruck. On
admission the neurological examination showed right-sided glossopharyngeal and spinal accessory
nerve lesions (moderate paresis of the upper portion of the trapezius and the sternocleidomastoid
muscles) in addition to the pre-existing hypoglossal and recurrent laryngeal nerve palsies (cranial
nerves IX, X, XI, and XII) (Figure 1). Lumbar puncture delivered normal cerebrospinal fluid
while MRI with T1 fat saturation and MR-angiography revealed a dissection of the right internal
carotid artery in its very distal extracranial section close to the base of the skull with prominent
subadventitial wall haematoma and expansion of the vessel diameter but without relevant narrowing
of the lumen (Figure 2). There was a prominent coiling of the internal carotid artery at the dissection site. No ischemic lesions were detected and because the vessel did not show significant stenosis the
patient was treated with antiplatelet agents (aspirin 100 mg daily). During hospital stay possible risk
factors for cervical artery dissection (i.e. connective tissue disease, primary vessel disease) could be
excluded but untreated hypertension and hypercholesterolemia were found. On routine 3-month
follow-up, the patient’s symptoms had significantly improved and no post-dissecting aneurysm had
emerged. When last seen, clinical examination showed complete remission and the vessel status had
normalized on MRI.
Case 2
A 55-year-old man complained about left-sided neck pain followed by dysphagia and hoarseness
two weeks after a minor head trauma. The patient’s general practitioner supposed the diagnosis of
laryngitis. Symptoms worsened progressively and the patient was admitted to the emergency room
of our clinics. Neurological examination unravelled left-sided lower cranial nerve palsies IX, X, XI,
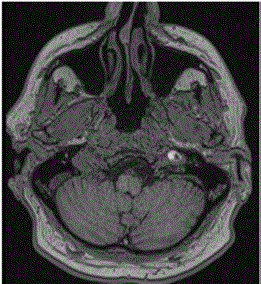
and XII causing symptoms identical to Case 1 except for left-sidedness. MRI was performed and
showed subadventitial internal carotid artery dissection loco typico with a substantial increase in
vessel diameter and normal lumen size (Figure 3). The patient was initially treated with intravenous heparin and switched to antiplatelet therapy after one week (aspirin 100 mg daily). Again, no connective tissue disease and this time additionally no cardiovascular risk factors were evident. Three months later he had recovered completely.
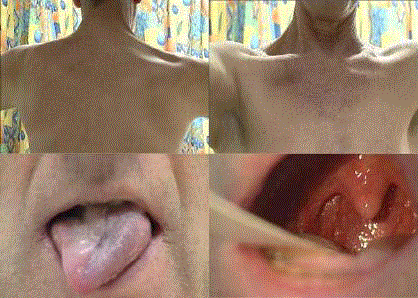
Figure 1
Figure 1
Clinical examination patient 1 showing atrophy of the upper portion
of the right trapezius muscle, right-sided hypoglossal and glossopharyngeal
(i.e. asymmetric deviation of the uvula to the left and absent gag reflex) nerve
palsies.
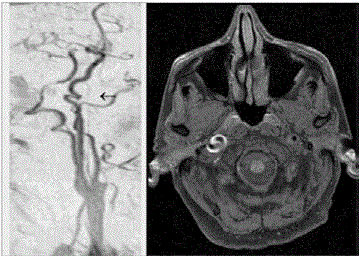
Figure 2
Figure 2
T1 fat saturated MRI imaging of patient 1 showing dissections of
the right ICA and coiling at the area of dissection.
Figure 3
Discussion
Collet Sicard Syndrome represents the combination of lower
cranial nerve palsies IX to XII [1,2]. The aetiology of Collet Sicard
Syndrome is heterogeneous, ranging from immunological (e.g.
idiopathic cranial polyneuritis) and infectious diseases (e.g. Lyme’s
disease and herpes zoster) to local expansive lesions in the retrostyloid
region caused by neoplasms of the epipharynx or metastases at the
skull base [3]. In most of these patients neoplastic illness is already
known when cranial nerve palsies develop and the correct diagnosis is easily established.
Our two case reports suggest internal carotid artery dissection as
another more challenging and probably under-recognised pathology
underlying Collet Sicard Syndrome. In the retrostyloid region the
internal carotid artery is in close touch with the glossopharyngeal,
vagus and spinal accessory nerves which all pass through the jugular
foramen, and the hypoglossal nerve which exits from the hypoglossal
canal. The carotid artery segment 2-3 cm past the bifurcation is the
predilection site for spontaneous dissection that tends to propagate to
the base of the skull (own unpublished data) where dissection with a
subadventitial hematoma can lead to expansion of the vessel diameter
and subsequent compression of the nerves [4]. It was also proposed
that dissection may cause interruption of the blood supply to the
nerves. This mechanism, however, is less plausible because the lower
cranial nerves in their extracranial course are usually nourished from
the ascending pharyngeal artery - a branch of the external carotid
artery.
The cause for the distal segment of the internal carotid artery
being most commonly affected is essentially unknown. Likely
hypotheses include local factors like styloid process length, styloid
process to internal carotid artery distance [5] or increased mechanical
wall stress during head movement in this vessel area [6].
Distal carotid artery dissection can present with ischemic stroke
or recurrent transient ischemic attacks, yet recently diagnosis of
clinically asymptomatic (i.e. local symptoms only) dissections has
become more frequent, possibly due to the increased availability
of advanced imaging modalities. Typically local pain (head, neck)
is present in almost all cases, with Horner's syndrome or pulsatile
tinnitus [7] also being very frequent. Lower cranial nerve palsies
occur in up to 10 % of patients with internal carotid artery dissection
either as the leading clinical symptom or in combination with one or
more of the aforementioned local symptoms.
Single cases of Collet Sicard syndrome and internal carotid
artery dissection have previously been published [4,8-14]. In line
with our two cases the spontaneous course seems to be benign with
(near) complete resolution of the nerve palsies [4,14]. Still early
establishment of a correct diagnosis and treatment is mandatory
because of the risk of stroke in the case of a subintimal propagation
of the mural hematoma. We want to increase awareness of the fact
that Collet Sicard Syndrome or isolated lower cranial nerve palsies
may be caused by internal carotid artery dissection. If noticed, the
diagnosis is easily established by MRI with T1 fat saturation and MR
angiography.
Author’s Contributions
Lukas Mayer: Writing of the manuscript and literature research.
Michael Spiegel: Patient care and Critical revision of the
manuscript for important intellectual content.
Christian Boehme: Critical revision of the manuscript for
important intellectual content.
Thomas Toell: Critical revision of the manuscript for important
intellectual content.
Astrid Grams: Patient care and critical revision of the manuscript
for important intellectual content.
Johann Willeit: Patient care and critical revision of the manuscript
for important intellectual content.
Stefan Kiechl: Patient care, critical revision of the manuscript for
important intellectual content.
Michael Knoflach: Senior author and critical revision of the
manuscript for important intellectual content.
References
- Collet FJ. Sur un nouveau syndrome paralytique pharyngo-larynge par blessure de guerre (hemiplegie glosso-laryngo-scapulo-pharyngee). Lyon Medical. 1915; 124: 121-129.
- Sicard JA. Syndrome du carrefour condylodechire posterieur (type pur de paralysie des quatre derniers nerfs craniers). Marseille Medical. 1917; 53: 385-397.
- Prashant R, Franks A. Collet-Sicard syndrome-a report and review. Lancet Oncol. 2003; 4: 376–377.
- Waespe W, Niesper J, Imhof HG, Valavanis A. Lower cranial nerve palsies due to internal carotid dissection. Stroke. 1988; 19: 1561-1564.
- Smoot TW, Taha A, Tarlov N, Riebe B. Eagle syndrome: A case report of stylocarotid syndrome with internal carotid artery dissection. Interv Neuroradiol J Peritherapeutic Neuroradiol Surg Proced Relat Neurosci. 2017; 1591019917706050.
- Callaghan FM, Luechinger R, Kurtcuoglu V, Sarikaya H, Poulikakos D, Baumgartner RW. Wall stress of the cervical carotid artery in patients with carotid dissection: a case-control study. Am J Physiol Heart Circ Physiol. 2011; 300: H1451-H1458.
- Lanczik O, Szabo K, Gass A, Hennerici MG. Tinnitus after cycling. Lancet Lond Engl. 2003; 362: 292.
- Rees JH, Valentine AR, Llewelyn JG. Spontaneous bilateral carotid and vertebral artery dissection presenting as a Collet-Sicard syndrome. Br J Radiol. 1997; 70: 856–858.
- Schmidt F, Dihné M, Steinbach J, Bühring U, Küker W. [Raeder- and Collet-Siccard-Syndrome. Acute pareses of cranial nerves symptomatic of a dissection of internal carotid artery]. Nervenarzt. 2000; 71: 502–505.
- Heckmann JG, Tomandl B, Duhm C, Stefan H, Neundörfer B. Collet-Sicard syndrome due to coiling and dissection of the internal carotid artery. Cerebrovasc Dis Basel Switz. 2000; 10: 487–488.
- Walker S, McCarron MO, Flynn PA, Watt M. Left internal carotid artery dissection presenting with headache, Collet-Sicard syndrome and sustained hypertension. Eur J Neurol. 2003; 10: 731–732.
- Mohr A, Ebert S, Knauth M. [Spontaneous dissection of the internal carotid artery with ipsilateral Collet-Sicard syndrome]. ROFO Fortschr Geb Rontgenstr Nuklearmed. 2006; 178: 444–6.
- Battaglia F, Martini L, Tannier C. [Collet-Sicard syndrome after carotid artery dissection]. Rev Neurol (Paris). 2009; 165: 588–590.
- Smith R, Tassone P, Saada J. Collet-Sicard syndrome as a result of unilateral carotid artery dissection. BMJ Case Rep. 2013; 2013.