Case Report
Dystrophic Epidermolysis Bullosa with Laryngotracheal Involvement: Abscess on the Vocal Cords
Oya Yucel*
Department of Pediatrics, Baskent University, Turkey
*Corresponding author: Oya Yucel, Department of Pediatrics, Baskent University, Istanbul Education and Research Hospital, Kosuyolu. Veysı Pasa Sok. 100.yıl sitesi. H-Blok. No:22, Uskudar /Istanbul, Turkey
Published: 05 Jun, 2017
Cite this article as: Yucel O. Dystrophic Epidermolysis Bullosa with Laryngotracheal Involvement: Abscess on the Vocal Cords. Ann Clin Case Rep. 2017; 2: 1368.
Abstract
Background: Dystrophic Epidermolysis Bullosa (DEB) is a rare genodermatosis characterized by blister formation as a result of separation of the skin from underlying tissue. The mucous membranes
can be involved in DEB. Laryngotracheal involvement is rare.
Case Report: A 4-year old girl with episodes of respiratory problems over a long period of time was
admitted to hospital. She had severe asthmatic attacks without complete recovery while using an
inhaled bronchodilator together with inhaled steroid continuously. Her family was living in Iraq.
Vital signs were stable. The patient had blisters with erosion and scar formation on the skin, especially
at the pressure sites on the patient's extremities. Her toenails and fingernails were thickened and
dystrophic. The patient had no respiratory distress on examination, however, inspiratory stridor
was determined instead of expiratory wheezing. Laryngoscopic examination was performed in
surgery and an inflammatory abscess was detected on the vocal cords.
Conclusion: A patient with an abscess on the vocal cords because of infected blisters due to DEB is
presented.
Keywords: Children; Childhood; Dystropic epidermolysis bullosa
Introduction
Epidermolysis Bullosa (EB) is a rare hereditary disease characterized by widespread blistering of
the skin and mucous membranes. In patients suffering from EB, trauma or friction causes separation of
the skin from underlying tissue resulting in consecutive painful blisters, scarifications, contractures,
and pseudosyndactyly. The prevalence of EB is reported as 11.07 cases in United States, 54 cases in
Norway, 7.8 cases in Japan, 15.4 cases in Italy, 10.3 cases in Australia and 9.6 cases in Croatia per one
million live births [1]. EB of the skin results from genetic defects in molecules related to adhesion with loss of adhesion resulting in blister formation. These may occur anywhere on the body but most
commonly appear at friction and minor trauma sites such as the feet and hands. In some subtypes,
blisters may also occur on internal organs, such as the esophagus and respiratory tract. The mode
of inheritance may be autosomal dominant or recessive but all forms of dystrophic EB (DEB) result
from mutations in the gene encoding type VII collagen, COL7A1 [2]. EB can be described as a
genodermatosis. There are three major types of EB based on the site of blister formation within the
skin: EB Simplex (EBS), Junctional EB (JEB) and DEB. EBS results from mutations within either the
keratin 5 or keratin 14 gene. JEB-Herlitz (JEB-H) is caused by severe mutations within any of the
three genes which encode for laminin-332. A minority of non-Herlitz JEB (JEB-nH) have mutations
within the gene encoding for type XVII collagen. However, in DEB, there are no mutations hotspots
within the COL7A1 gene. Every family with DEB has its own unique type of mutation. If there is
a mutations known in the family, It would facilitate in DNA mutational analysis, especially for
prenatal diagnoses using specimens obtained from chorionic villi [3]. The site of blister formation within skin in DEB is the lamina densa and upper dermis. Mild pseudosyndactyly or flexion
contractures of the fingers are present in 6% of those with autosomal dominant DEB. The frequency
of Dominant DEB (DDEB) was 68%, with 19% of uncertain inheritance and 13% of recessive
DEB (RDEB) [4]. The prognosis depends on the subtype of the disease. Infants and children with inherited EB, particularly those with JEB, are at significant risk of death as a result of complications
[5]. Cases with EBS and DDEB have normal life expectancies with significant morbidity. Diagnostic tests are biopsy of a blister on the skin or mucous membranes which involves İmmunofluorescence
Antigen Mapping (IFM) and/or Transmission Electron Microscopy (TEM) [3,6]. The diagnosis
of EB is most obvious for physicians experienced in dermatology. However, some cases will need
differential diagnosis. Any blistering disorder in the newborn period may mimic EB. These include Herpes simplex virus, epidermolytic ichthyosis, bullous impetigo and
incontinentia pigmenti. Acquired disorders for differential diagnosis
are immunobullous disorders, EB acquisita, Linear IgA dermatosis,
bullous pemphigoid, cicatricial pemphigoid, pemphigus, infectious
diseases, Herpes simplex, staphylococcal scalded skin syndrome and
bullous impetigo [3].
Currently, there is no cure for EB. The most important issues
in basic care are prevention of blistering and secondary infection
of blisters Band-aids, bandages, or tape should not be used on the
skin. Skin fragility is characteristically worsened in warm weather.
Patients should avoid exposure to heat and humidity. If possible,
air conditioned environments should be recommended. Hand
deformities can be prevented by meticulous nightly wrapping of
the digits. If not performed, surgical procedures will be necessary.
There are some experimental approaches; Ex Vivo replacement for
autosomal recessive EB, transplantation of allogeneic fibroblasts for
RDEB, transplantation of bone marrow-derived stem cells or infusion
of recombinant protein (i.e., type VII collagen for RDEB) [3]. The
mucous membranes can also be involved in DEB. The highest risk of
upper airway strictures and obstruction occurs in JEB-H. Recurrent
esophageal blistering and erosions can lead to stricture formation
[3,7,8]. However, laryngotracheal involvement is rare in DEB. This
case report presents involvement of the vocal cords in DEB in a 4-year
old girl complaining about recurrent respiratory distress.
Case Presentation
The patient had been experiencing episodes of respiratory
problems for a long time and occasionally had severe asthmatic attacks
without complete recovery. She was using an inhaled bronchodilator together with inhaled steroid continuously. In her family history,
her maternal uncle had the same findings since birth. She was the
fourth children of the same parents and other children in the family
did not have any problems. Her family was living in Iraq and she was
admitted to a different hospital for respiratory distress which never
completely resolved. The patient was 4-years old when admitted to
the pediatric clinic in Baskent University Hospital, Istanbul (Turkey).
An examination revealed stable vital signs. The recurrent respiratory
distress, skin fragility and nail abnormalities were major complaints.
On examination, her weight was 15,500g and height was 101 cm.
Failure to thrive and growth retardation were not determined. On
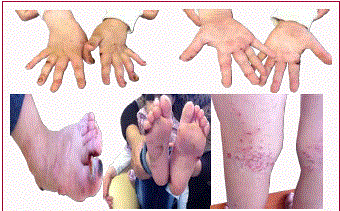
inspection, the patient had blisters with erosion and scar formation on
the skin, especially on the pressure sites of her extremities (Figure 1).
In the case presented here, blister scars were commonly observed on
the feet and hands at pressure sites of friction and minor trauma. She
had significant dental decay in the mouth. Her toenails and fingernails
were thickened and dystrophic. Milia were not present. The patient
had no respiratory distress on examination; however, inspiratory
stridor was determined instead of expiratory wheezing. She had
used inhaled bronchodilator and inhaled steroids continuously for
a long time. She may have complained of long-standing stridor,
but not asthmatic attacks. She had minor lymphadenopathies. On
auscultation, cardiac pansystolic murmur was determined. An atrial
septal defect was diagnosed by a cardiologist. Chest radiography was
completed, blood tests including CBC, BUN, creatinine, AST, ALT
and urinalysis were evaluated as normal. She did not have anemia.
She was admitted to our hospital for laryngoscopic examination
with anesthesia. The mucous membrane in the mouth and
oropharynx were normal. Laryngoscopic examination was performed
by an otolaryngologist in surgery in order to check the supraglottic
structures, vocal cords or trachea in terms of separation of the mucous
membranes from underlying tissue with minor trauma. The fragility
of mucous membranes can make laryngoscopic examination risky
because shedding by the blisters might be expected to produce upper
airway obstruction or strictures of upper airways. The clinicians were
aware of the risks. Similar lesions to those on the skin were observed
in the larynx and an inflammatory abscess was identified on the vocal
cords. Infected materials and tissue in the blister were aspirated and
sent to the pathology department. Two hours later, severe respiratory
distress suddenly occured because of upper airway obstruction due
to shedding of blisters. She was administered oxygen therapy for
two hours, recovered with coughing attacks, was monitored for one
whole day and then discharged. She was monitored for one week
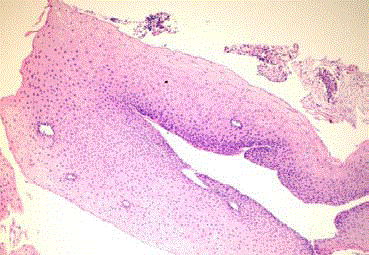
before returning to her country. Pathologic evaluation revealed
blister cleavage below the basal lamina and subepithelial separation
(Figure 2). Supportive therapies, future risks and genetic basis of this
disease were explained to her parents. Genetic analysis could not be
performed.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
DEB is a rare hereditary disease involving the skin. However,
certain types of EB can also affect the respiratory system. Involvement
of the oropharynx is more common than laryngotracheal
involvement. Even if mucous membrane involvement is extensive,
airway obstruction does not contribute to mortality in these patients.
Recurrent respiratory distress has been wrongly interpreted as
asthmatic attacks in some children with EB. A child suffering from
inspiratory stridor was diagnosed with a blister abscess on the vocal
cords in EB and is presented as a rare case in our paper.
Collagen VII anchoring fibrils are a component of the airway
basal membrane. They are an integral part of the supracellular
anchoring network that attaches the epithelium to the extracellular
matrix. Reduction of collagen VII in EB is associated with sloughing
of epithelium [9]. This means that respiratory tract involvement
can be found in certain types of EB. Lesions can be detected on the
mucosa of the respiratory tract from the oral cavity to the bronchi.
The oral cavity and oropharynx are involved more frequently than
the hypopharynx, larynx and trachea. Involvement of laryngeal and
tracheal mucosa is generally associated with increased morbidity and
mortality, complications and therapeutic difficulties [10]. These are
more common in JEB and DEB than in EBS [5]. JEB may involve
the upper airway, especially in JEB-H. Granulation tissue which is
a pathognomonic finding in JEB-H was not present in our patient.
In DDEB, blistering is often mild and limited to hands, feet, knees,
and elbows, but nonetheless heals with scarring. Dystrophic nails
are common and may be the only manifestation of DDEB [11]. In
our case, toenails and fingernails were thickened and dystrophic.
Failure to thrive, growth retardation and severe anemia which are
characteristic features of RDEB and JEB-H were not determined
in our patient [3]. The patient was diagnosed as having dominant
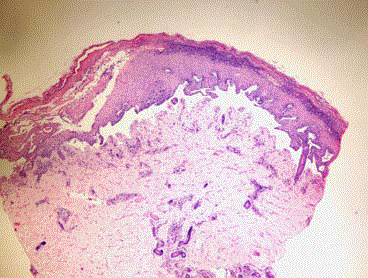
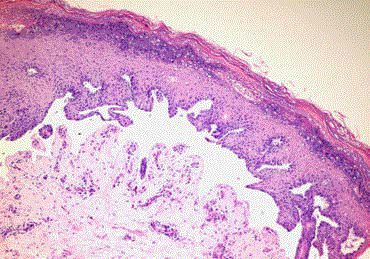
DEB on the basis of clinical, familial and histological findings). The
diagnosis was supported by biopsy (Figure 3 and 4).
Laryngotracheal involvement should be considered for EB in
any child presenting with symptoms of respiratory distress and
laryngoscopic examination should be considered and performed
in the operating room by an otolaryngologist. However, clinicians
should be aware of the risks of shedding by the blisters due to the
endoscopy.
Acknowledgement
Verbal permission was obtained from the family to publish pictures of their child.
References
- Fine JD. Epidemiology of Inherited Epidermolysis Bullosa Based on Incidence and Prevalence Estimates From the National Epidermolysis Bullosa Registry. JAMA Dermatol. 2016; 152: 1231-1238.
- Mallipeddi R, Bleck O, Mellerio JE, Ashton GH, Eady RA, McGrath JA. Dilemmas in distinguishing between dominant and recessive forms of dystrophic epidermolysis bullosa. Br J Dermatol. 2003; 149: 810-818.
- Fine JD. Inherited epidermolysis bullosa. Orphanet Journal of Rare Diseases. 2010; 5: 12.
- Horn HM, Tidman MJ. The clinical spectrum of dystrophic epidermolysis bullosa. Br J Dermatol. 2002; 146: 267-274.
- Babić I, Karaman-Ilić M, Pustisek N, Susić S, Skarić I, Kljenak A, et al. Respiratory tract involvement in a child with epidermolysis bullosa simplex with plectin deficiency: a case report. J Pediatr Otorhinolaryngol. 2010; 74: 302-305.
- Fine JD, Eady RA, Bauer EA, Bauer JW, Bruckner-Tuderman L, Heagerty A, et al. The classification of inherited epidermolysis bullosa (EB): Report of the Third International Consensus Meeting on Diagnosis and Classification of EB. J Am Acad Dermatol. 2008; 58: 931-950.
- Fine JD, Johnson LB, Weiner M, Suchindran C. Tracheolaryngeal complications of inherited epidermolysis bullosa. Laryngoscope. 2007; 117: 1652-1660.
- Fine JD, Johnson LB, Weiner M, Suchindran C. Gastrointestinal complications of inherited epidermolysis bullosa: cumulative experience of the National EB Registry. J Pediatr Gastroenterol Nutr. 2008; 46: 147- 158.
- Villone D, Fritsch A, Koch M, Bruckner-Tuderman L, Hansen U, Bruckner P. Supramolecular interactions in the dermo-epidermal junction zone: anchoring fibril-collagen VII tightly binds to banded collagen fibrils. J Biol Chem. 2008; 283: 24506–24513.
- Thompson JW, Ahmed AR, Dudley JP. Epidermolysis bullosa dystrophica of the larynx and trachea. Acute airway obstruction. Ann Otol Rhinol Laryngol. 1980; 89: 428-429.
- Pfendner EG, Lucky AW. Dystrophic Epidermolysis Bullosa. Gene Reviews. 1993-2017. 2006.