Case Report
Pseudoaneurysm of the Facial Artery Following Bilateral Temporomandibular Joint Replacement: A Case Report
Lanit Anand*
Department of Oral Health, Middlemore Hospital, Auckland, New Zealand
*Corresponding author: Lanit Anand, Department of Oral Health, Middlemore Hospital, 11/3 Burton Street, Grafton, Auckland 1010, New Zealand
Published: 08 May, 2017
Cite this article as: Anand L. Pseudoaneurysm of the Facial Artery Following Bilateral Temporomandibular Joint Replacement: A Case Report. Ann Clin Case Rep. 2017; 2: 1356.
Abstract
Introduction: Pseudoaneurysm of the facial artery is a rare event. Rupture of the arterial wall leads
to extravasation of blood into the surrounding tissue, followed by tamponade and clot formation.
Left untreated this has the potential to cause catastrophic haemorrhage.
Case Report: A 59-year-old male presented to our department with bony ankylosis of his
temporomandibular joints bilaterally as a result of previous osteomyelitis. He underwent bilateral
temperomandibular joint replacements in a two-stage procedure. Following his discharge he
presented to the emergency department six weeks later in haemorrhagic shock, having lost significant
blood volume from a pulsatile lesion over his right mandible. Computed tomography angiography
revealed a pseudoaneurysm of the right facial artery. He proceeded to emergent embolisation with
resolution of the pseudoaneurysm.
Introduction
Aneurysms are defined as abnormal and local dilatations of blood vessel walls. They can be
classified as either true or false. In a true aneurysm all three layers of the affected blood vessel are
involved: intima, media and adventitia [1]. A false aneurysm, or pseudoaneurysm, is a collection of blood leaking completely out of an artery, but confined next to the vessel by the surrounding tissue [2].
Pseudoaneurysms are caused by the partial rupture of an artery, followed by the extravasation
of blood into the surrounding tissue. This leads to haematoma formation that tamponades the
arterial flow. The structure of the haematoma begins to organise and an endothelial lining forms
around the periphery [3]. Following liquefaction of the haematoma, the aneurysmal sac and artery communicate, forming a pulsatile mass. This mass may gradually expand and is at risk of rupture,
which can lead to life threatening haemorrhage [2,4]. Pseudoaneurysms usually show a delayed occurrence, presenting weeks or months after the precipitating event [3,5,6].
We present a case of a pseudoaneurysm of the right facial artery that occurred in the weeks
following bilateral temperomandibular joint (TMJ) replacement surgery. To the author’s knowledge
this has not been reported in the literature to date.
Case Presentation
A 59 year old male was referred to the Oral and Maxillofacial Surgery (OMFS) Department
for evaluation and management of his complete trismus. He had immigrated to New Zealand
six months prior from Africa. Approximately 10 years ago he suffered widespread mandibular
osteomyelitis, which was treated with intra-venous penicillin over many months. Prior to this, his
mouth opening was normal.
On examination, the patient was micrognathic, with a retruded chin and atrophied masseter
muscles. He had tethering of the skin over the body of the mandible bilaterally. Computed
Tomography (CT) showed bony fusion of both the left and right mandibular condyles to their
respective glenoid fossa.
Following biopsy of his condyles to ensure the osteomyelitis had completely resolved, he
underwent two-stage bilateral TMJ replacement surgery. After initial resection of the bony
ankylosis and placement of temporary spacers, he proceeded to placement of bilateral artificial
temporomandibular (TM) joints.
Following TMJ replacement surgery, the patient recovered well without complication and was discharged home. He was reviewed two weeks following the surgery
where he was noted to have developed a haematoma over his right
submandibular wound (site of surgical access). There was no sign of
infection, but was causing the patient discomfort. At the time, under
local anaesthetic, this haematoma was partially evacuated. Upon
review the following week, this area was much more comfortable, and
at further review at two weeks it continued to improve, but had not
resolved completely.
Approximately two weeks after his last review (six weeks since the
initial surgery) he presented to the Emergency Department (ED) in
hemorrhagic shock. He had sustained a severe bleed from a pulsatile
lesion in the right suubmandibular region. Intra oral examination
was unremarkable. His haemoglobin on arrival was 59 g/L and
blood pressure 90/51 mmHg. Blood tests showed prothrombin time
(PT) and activated partial thromboplastin time (APTT) were within
normal limits.
Following resuscitation with normal saline and two units of red
blood cells he was stabilized and direct pressure over the lesion had
stopped the bleed. A computed tomography arteriogram (CTA) was
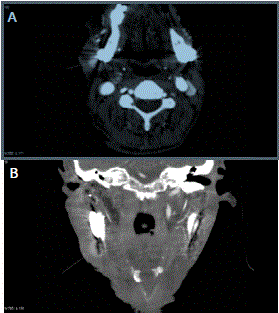
arranged urgently. This showed a large pseudoaneurysm of the right
facial artery, lying superficial to the right TMJ replacement, with the arterial defect lying posterior to the point of attachment at the ramus of the mandible (Figure 1 A and B ).
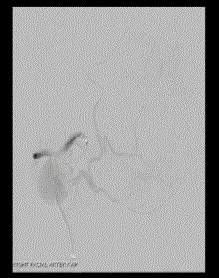
Endovascular embolisation was arranged and a microcatheter
was passed through the base of the aneurysm to the exit point of the
facial artery from the aneurysm. (Figure 2) A tissue adhesive (75%
histocryl/lipiodol/tantalum) was injected, closing the facial artery
both proximal and distal to the aneurysm, and closing the defect in the
artery without filling the bulk of the aneurysm (Figure 3). Follow up
CTA was performed that showed resolution of the pseudoaneurysm
(Figure 4 A and B). The patient made a successful recovery, and has
had no recurrence or complications from the treatment after one year
of follow up.
Figure 1
Figure 2
Figure 3
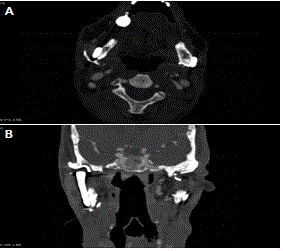
Figure 4
Figure 4
A) Postoperative follow up CTA (axial view) shows resolution of the
pseudoaneurysm. B) Coronal View.
Discussion
Pseudoaneurysms of the branches of the external carotid artery are
extremely rare [2,6]. The soft tissues and bones of the face protect these
branches, but in regions where they surface and cross bone structures,
they become vulnerable to damage [5]. Pseudoaneurysm of the facial
artery has been noted to occur following maxillofacial trauma [2,5],
orthognathic surgery [3,6,7], surgical removal of molar teeth [8], and odontogenic infection [9]. The most dangerous complication
of a pseudoaneurysm in this region is catastrophic haemorrhage
following rupture. Other complications include compression of
adjacent neurovascular structures, and release of embolic thrombi. In
this case pseudoaneurysm of the facial artery presented clinically as a painless, pulsatile lesion in the right submandibular region. Clinical findings such as pulsations or a bruit suggest a vascular aetiology
[10,11]. CTA is the investigation of choice in these situations, as it
can assess the patency and position of the branches of the ECA, as
well as delineating the anatomic details of the Pseudoaneurysm [2,4].
The consensus amongst the literature is that emoblisation through
interventional radiology of the aneurysm is safest and most effective
treatment method [3,7]. Treatment is essentially mandatory, given the
unstable nature of pseudoaneurysms, and the potentially devastating
consequences of rupture.
This case highlights the importance of prompt evaluation and
treatment of pseudoaneurysms of the facial artery. It is important to
ensure adequate postoperative follow up after surgery to the region as
pseudoaneuryms have a delayed presentation.
References
- Kumar P, Clark M, eds. Kumar & Clarke’s Clinical Medicine. 7th edn. Edinburgh: Elsevier Saunders, 2010.
- Ribeiro-Ribeiro AL, de Melo Alves Junior S, de Jesus Viana Pinheiro J. Traumatic pseudoaneurysm of the facial artery: late complication and effects on local blood flow. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112(1):e4–9.
- Lanigan DT, Hey JH, West RA. Major vascular complications of orthognathic surgery: false aneurysms and arteriovenous fistulas following orthognathic surgery. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons. 1991;49(6):571–7.
- Cooperband BR, Friedel W, Bhatt GM, Eisig S. False aneurysm of the facial artery. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons. 1989;47(12):1327–9.
- Madani M, Veznedaroglu E, Pazoki A, Danesh J, Matson SL. Pseudoaneurysm of the facial artery as a late complication of bilateral sagittal split osteotomy and facial trauma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod.. 2010;110(5):579–84.
- Jo HW, Kim YS, Kang DH, Lee SH, Kwon TG. Pseudoaneurysm of the facial artery occurred after mandibular sagittal split ramus osteotomy. Oral Maxillofac Surg. 2013;17(2):151–4.
- Rayati F, Parsa H, Abed P, Karagah T. Facial Artery Pseudoaneurysm Following Surgical Removal of a Mandibular Molar. Journal of Oral and Maxillofacial Surgery. 2010;68(7):1683–5.
- Lopes Oliveira M, Semedo C, Quintela M, Fragata I, Coelho C, Valejo Coelho P. Pseudoaneurysm of the facial artery territory in an odontogenic infection setting. Oral Radiol. 2015;32(2):119–125.
- Cohen MA. False (traumatic) aneurysm of the facial artery caused by a foreign body. Int J Oral Maxillofac Surg. 1986;15(3):336-8.
- Dediol E, Manojlovic S, Biocic J, Franceski D, Ivanac G. Facial artery pseudoaneurysm without evidence of trauma. Int J Oral Maxillofac Surg. 2011;40(9):988-90.
- Bradley JP, Elahi M, Kawamoto HK. Delayed presentation of pseudoaneurysm after Le Fort I osteotomy. J Craniofac Surg. 2002;13(6):746-50.